At one point, Xuan-Mai Roush’s problem had gotten so bad that she struggled just to walk around the house.
She’d find herself sitting frequently to catch her breath. She couldn’t go anywhere, couldn’t do much of anything. Even when she did get out, she had to walk stooped over.
Now, Roush is standing tall and enjoying life again. She’s finding pleasure in the simple things—cleaning her house, playing with her dog and making plans for a garden this summer.
They can go out and do what they love to do. It’s like they have a new lease on life.
“I have joy and I have peace now,” said Roush, 68, of Hastings, Michigan. “I feel normal. It’s just wonderful. It’s a miracle.”
That miracle: a cutting-edge procedure that corrected her long-running coronary artery blockage.
Her specific ailment is known as chronic total occlusion, a condition in which a coronary artery has been completely blocked for a period of at least three months.
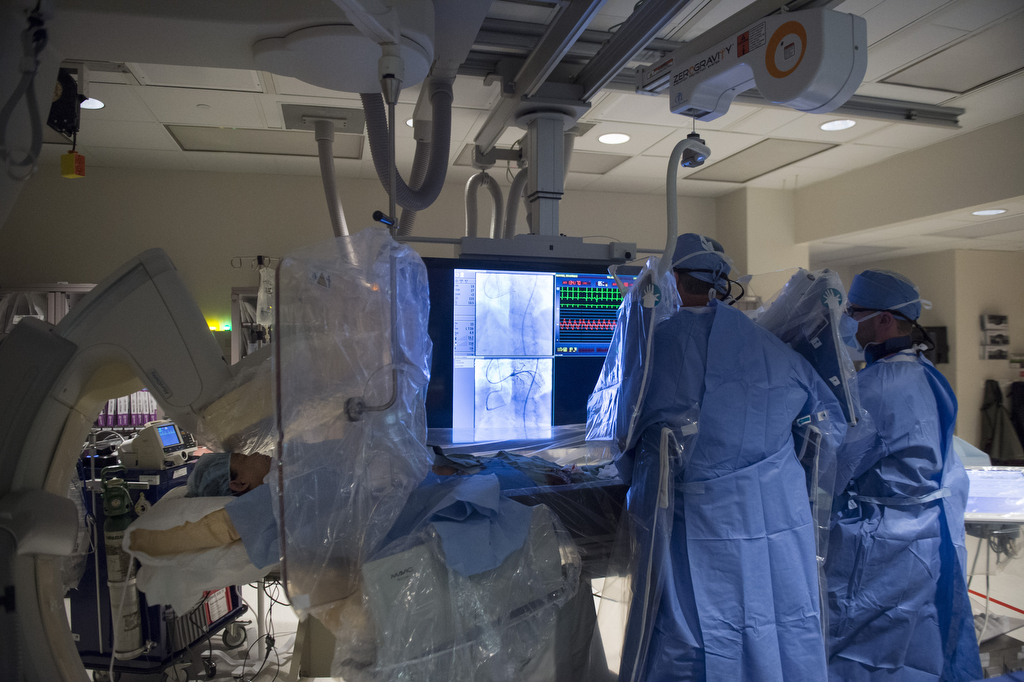
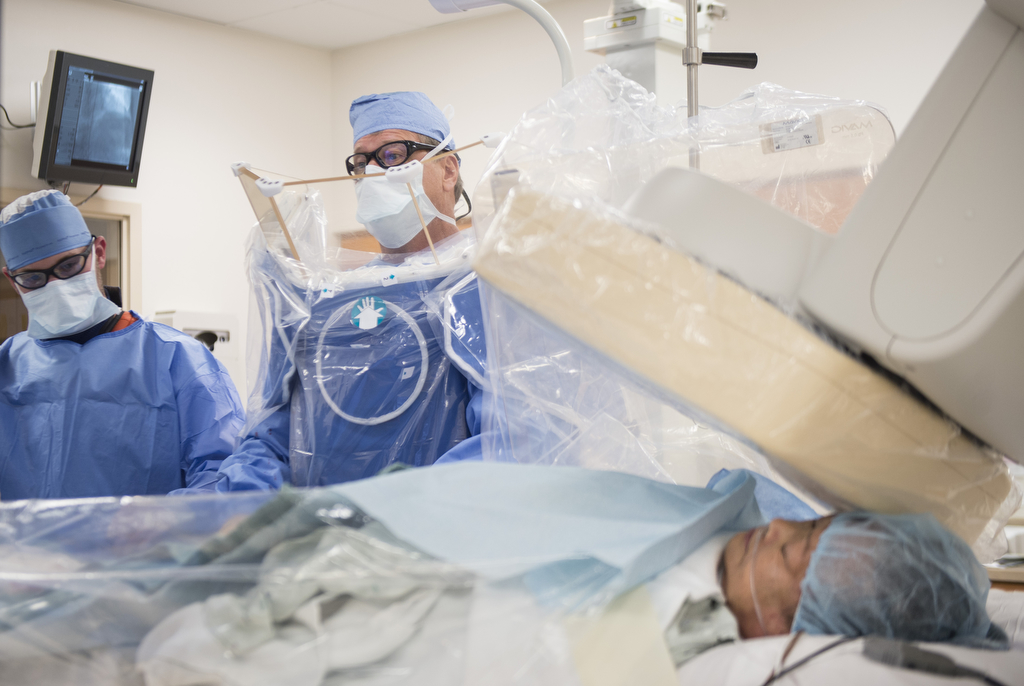
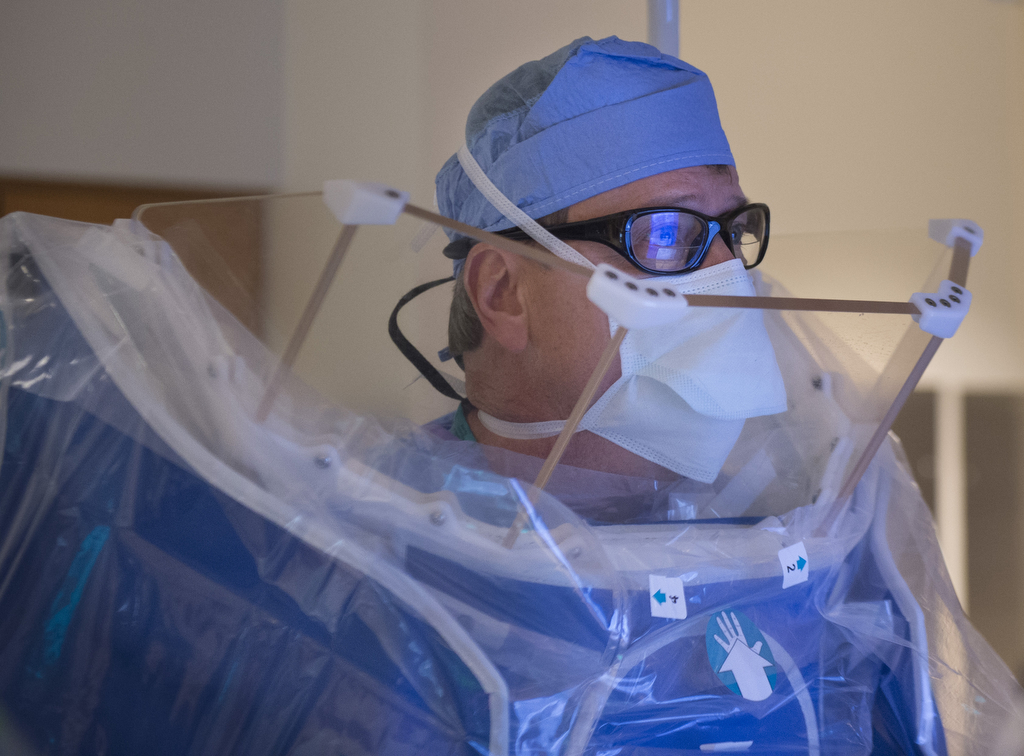
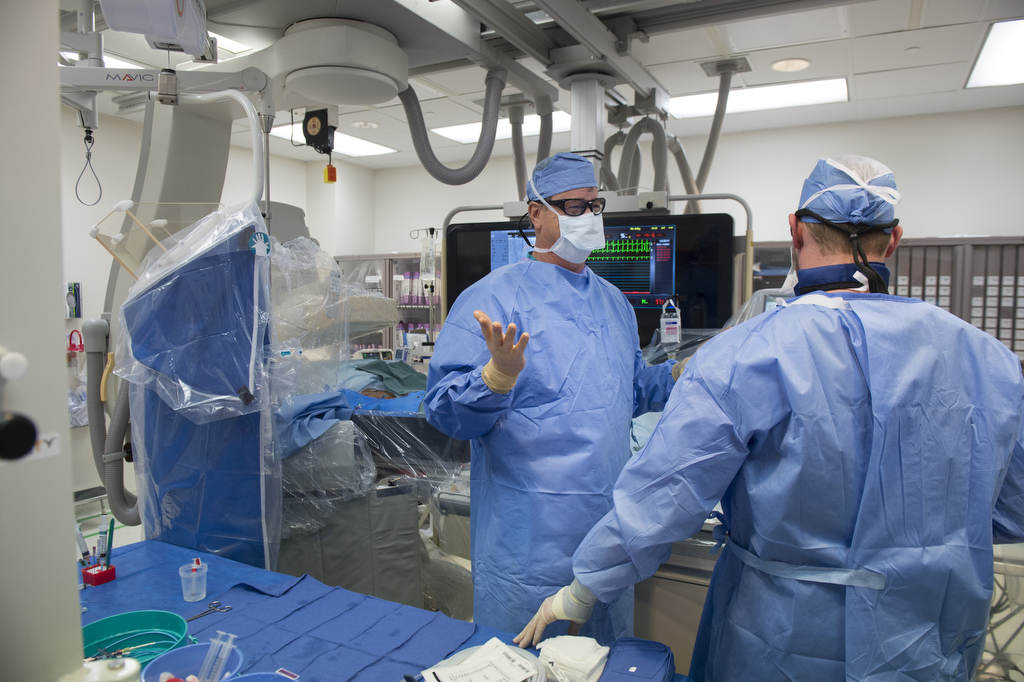
Treatment options for chronic total occlusion had typically been limited, until two Spectrum Health cardiologists—Kevin Wolschleger, MD, and David Wohns, MD—became specially trained to treat this condition through a minimally invasive procedure in Spectrum Health’s cath lab.
When Spectrum Health began offering the procedure in October 2013, it became one of the first hospitals in Michigan to do so. Drs. Wolschleger and Wohns have since performed it about 200 times, including earlier this year on Roush.
And, in Roush’s case as with many others, the results have been astounding.
“I am so grateful that they saved my life,” Roush said.
New lease
John Mulder, PA-C, a Spectrum Health physician’s assistant who helps inpatient cardiology patients, works with Drs. Wohns and Wolschleger to screen patients who are possible candidates for the total occlusion procedure.
For those who qualify, he walks them through the whole process beginning to end.
“The most exciting thing is what happens to the patients after they’re fixed,” Mulder said.
He enthusiastically recalls the patient who could finally play golf with his son after decades of weakness. The patient who went back to hunting after a 10-year hiatus. And the patient so excited to ride his motorcycle after years of health restrictions, he took it out in the middle of winter.
Dr. Wolschleger also finds gratification in the success stories.
“They can go out and do what they love to do,” he said. “It’s like they have a new lease on life.”
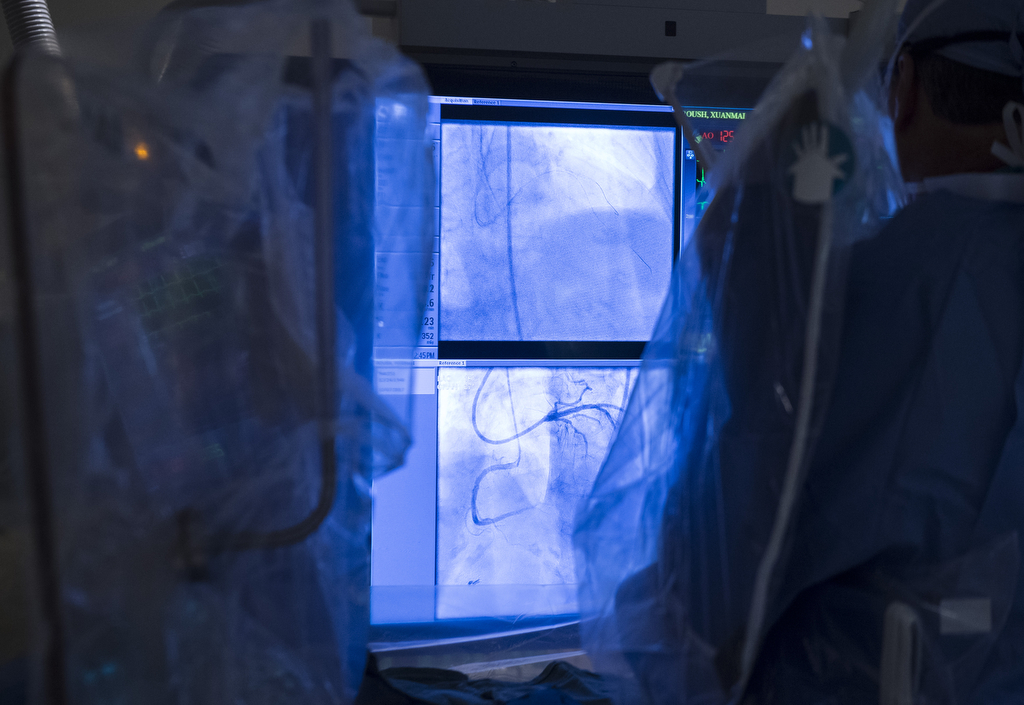
Patients with chronic total occlusion have a coronary artery that has been 100 percent blocked for months or years. The blockage is caused by a heavy buildup of atherosclerotic plaque in the artery.
If a blood vessel isn’t completely blocked, it can be successfully opened with angioplasty or stents. But when it’s completely blocked, those options aren’t as successful.
Unlike a sudden blockage, which causes a heart attack, these blockages can build for months or years, giving the body time to create natural channels around them. But in some cases, the result is disabling. Symptoms for some patients include angina (chest pain or pressure), shortness of breath, dizziness and fatigue.
In the past, chronic total occlusion had been treated with medications, or sometimes bypass surgery. But in many cases, patients were untreatable.
Dr. Wolschleger said cardiologists considered chronic total occlusion the last frontier in interventional cardiology.
And now they’ve conquered it.
Specialized training and new tools and techniques have led to great success in opening these blocked arteries.
In standard stent procedures and in angioplasty, the surgeon navigates the artery with a wire, but it’s difficult to get through the very hard and complete blockage seen in chronic total occlusion.
So instead—in a typically much more complicated and long procedure to treat the chronic total occlusion—they can use stiffer wires, or they might go into the wall of the blood vessel, around the blockage, and then back in to recreate an opening to restore blood flow.
“It’s very challenging,” Dr. Wolschleger said. “Some of these procedures take four to five hours.”
He and Dr. Wohns collaborate to determine the best steps as they work on each case.
New life
Roush found herself in the operating room on Jan. 7.
Just weeks earlier—exactly 10 days before Christmas—she had suffered a heart attack. Doctors had discovered three blockages: two at 85 percent and one at 100 percent.
They corrected the two lesser blockages with stents during her hospital stay, then sent her home to await her Jan. 7 procedure to correct the chronic total occlusion.
They didn’t want to perform heart bypass surgery on her because of the poor condition of her lungs, said her husband, William.
Roush came to the United States in 1972 with William, who had been in the Army. They met in Vietnam, where Roush’s father worked as a carpenter for William’s Army company.
They now have three grown children.
And they plan to live a good, long life together.
William said he took great comfort in hearing doctors explain how they gathered a panel of doctors to discuss his wife’s case so they could determine the best plan. And they explained the plan to Roush and her husband beforehand.
The end result, of course, proved successful.
“She’s not chasing me around the house, but she has a lot more air in her lungs,” William said. “She’s walking upright now. Before, she couldn’t go 10 feet across the room and she was stooped over like an old lady.”
In September, Roush and her husband will celebrate their 50th wedding anniversary.
Stories like these make it all more gratifying for health care providers like Mulder.
“A lot of these people have gotten their lives back,” he said.











 /a>
/a>
 /a>
/a>
 /a>
/a>
Fascinating…and effective! What is the name of the procedure?
I am so happy you are doing so well !!