Homecomings rarely get more powerful than this, because Alexia Kose, almost 4 months old, has never been home.
But Saturday, after living her entire life at Spectrum Health Helen DeVos Children’s Hospital, the little feisty one settled into the comfort of her family’s Traverse City home, swaddled in a gray, white and yellow nursery, decorated with giraffes.
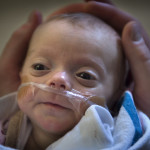
Born at only 25 weeks, her journey is a miracle in some ways, a real-life trudge through a series of trials and tribulations.
Alexia’s successes may seem small, but they are remarkable for one so tiny: adapting to an outside world when her body was gestationally programmed to still be surrounded by the womb’s warmth and security.
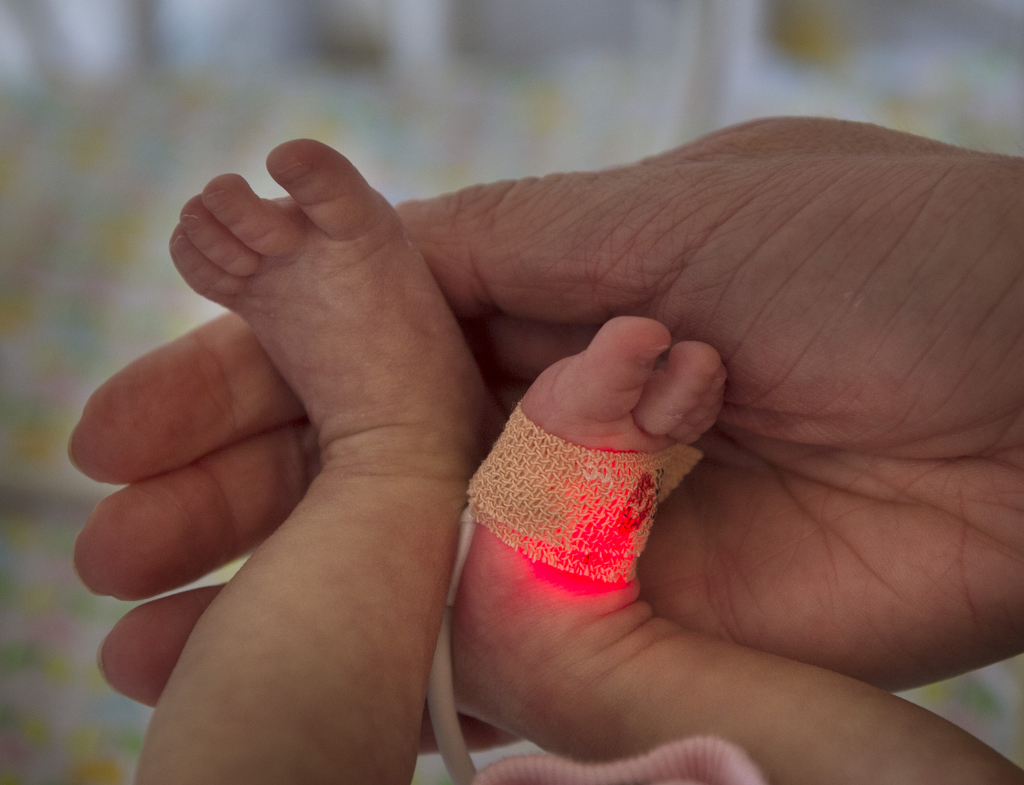
Her parents expected their first child to arrive Nov. 23. Instead, she made her appearance on Aug. 10, weighing only 1 pound 11 ounces, the equivalent of two cans of soda.
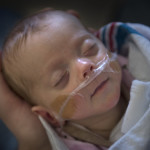
After months of diligent feedings and care in the Helen DeVos Children’s Hospital Small Baby Unit, Alexia has grown to just over 5 pounds.
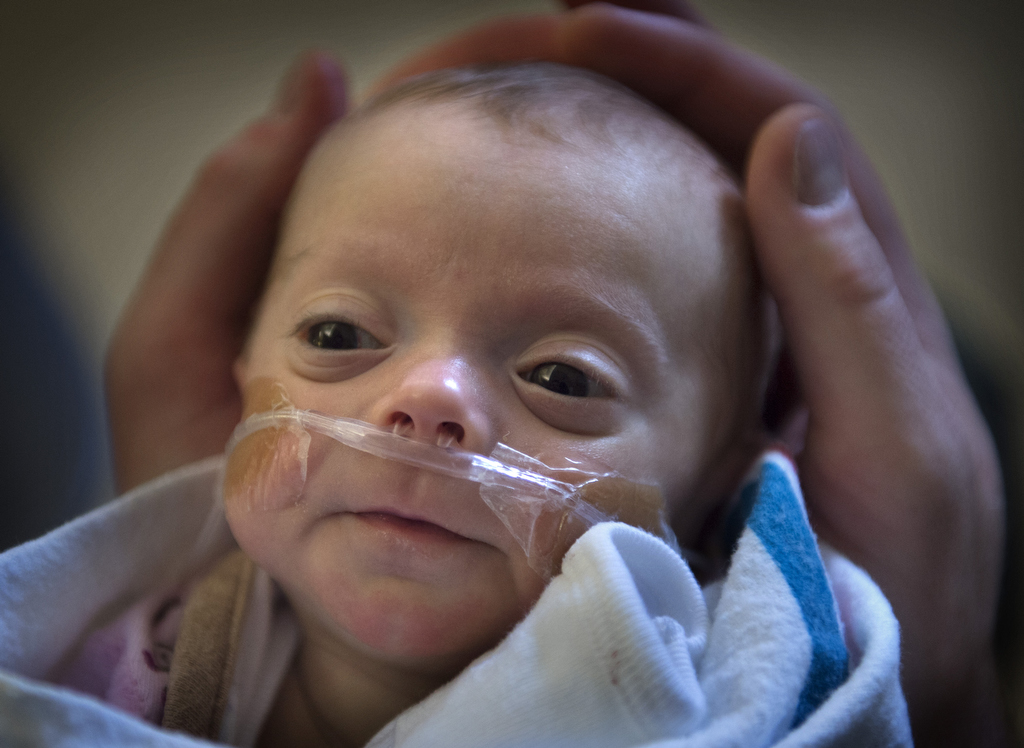
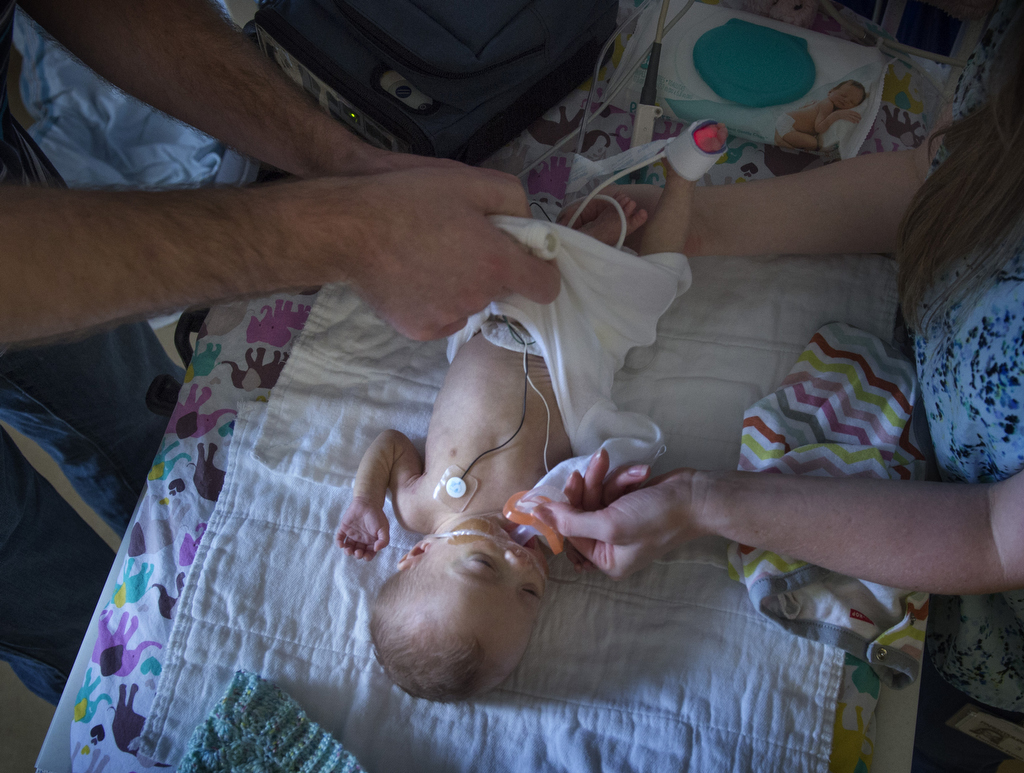
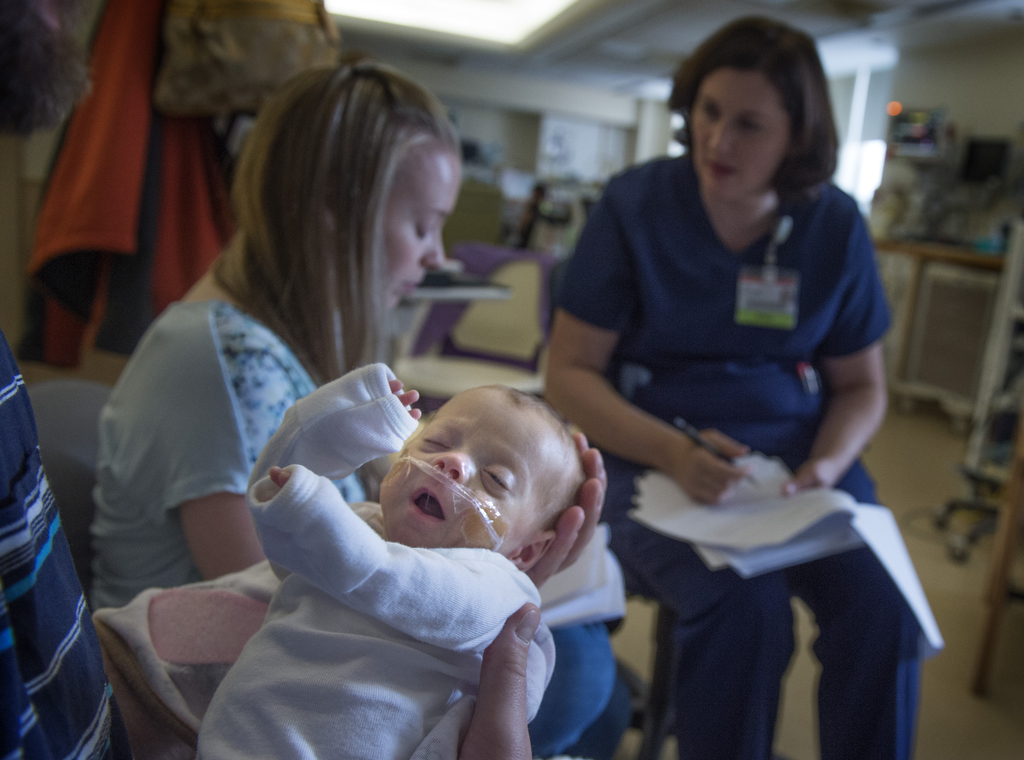
On Friday, the day before her departure, neonatologist Krista Haines, MD, unbuttoned Alexia’s pink and blue monkey PJs and placed a stethoscope on her chest. The baby’s heart and lungs sounded good.
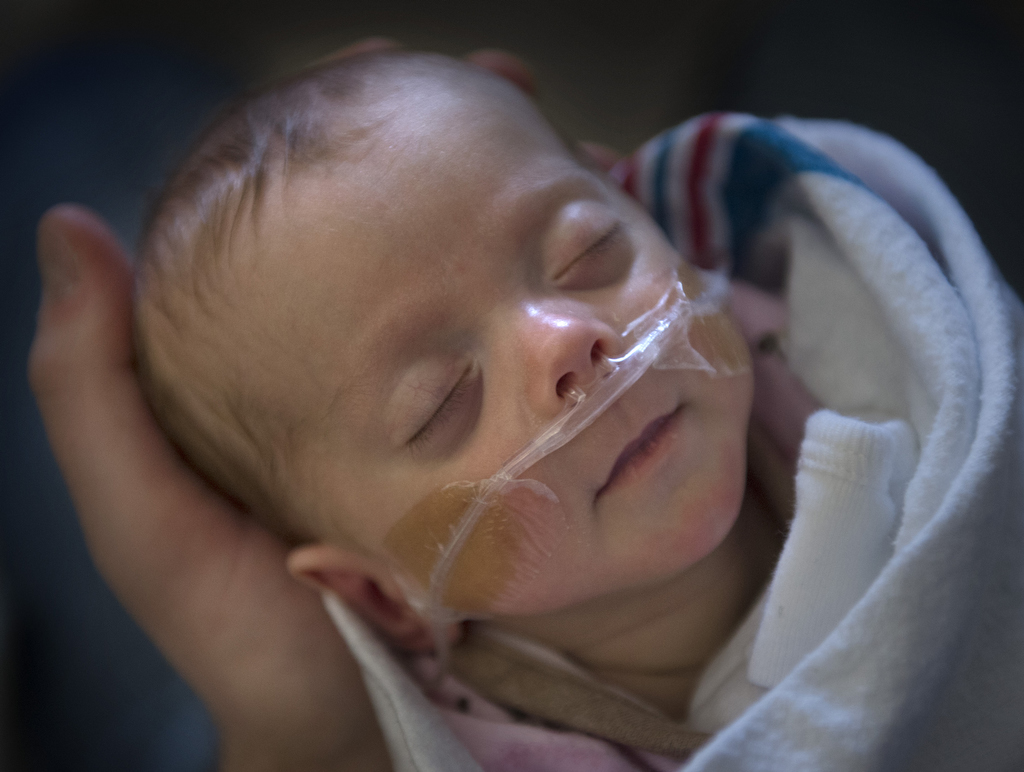
Alexia’s eyelids fluttered and a little smile appeared. She turned her face toward her pacifier, trying to reach it.
“Here’s your paci,” Haleigh Hieftje, RN, softly said.
“She’s a spunky, bright-eyed little girl,” said Hieftje, one of the primary nurses who provided Alexia’s care in the specialized unit within the NICU. “I will be sad to see her go.”
But she’s also glad Alexia’s mom and dad could finally take her home and put her to bed in her own crib.
“I know Danielle and John are wonderful parents,” she added. “It will be exciting to keep up with them in the years to come.”
Heading home
On the counter near Alexia’s crib lay a book created by the NICU staff charting her many milestones since the day she arrived–her first bottle, the day her breathing tube came out, her Nov. 23 due date and the first time she opened her eyes.
There are many more achievements to come, and parents Danielle and John Kose are thrilled to take the first steps.
After an 11 a.m. feeding Saturday, Danielle and John packed up multiple bags—their last four months of living—and prepared to head home.
“You never knew someone so small needed so many things,” Danielle said, laughing.
Dressed in a pink ballet shoe-themed sleeper, Alexia snuggled into her gray car seat.
“I can’t believe she’s actually in the car with us,” said Danielle, sitting in the back seat of the family’s gray 2014 Dodge Durango, next to the beautiful life who was finally en route home.
“It’s very exciting,” Danielle said. “We look forward to raising her. …We’ll just see where life takes us.”
Mallory Vander Kolk, RN, another of Alexia’s primary nurses, praised the little one’s progress.
“She is a little peanut, but she’s strong,” Vander Kolk said. “It’s hard to see her go, but I could not be happier. They are going to be so great together at home.”
They all look back on the days—117 emotional, prayerful days—since Alexia’s premature delivery. And smile. She made it. They made it.
Bound for the Small Baby Unit
That early arrival was quite unexpected, they remember. Danielle had coasted along in her pregnancy until Aug. 10.
“She just decided now was the time,” Danielle said.
Danielle awoke about 4:30 in the morning with what she thought might be contractions. But given the due date, she couldn’t be sure. Several hours later, she was at Munson Medical Center in Traverse City.
“When I got there I was dilated to 6 and she was on her way,” said Danielle, who herself was born two months early in 1984. “I was trying to remain calm and do what the doctors and nurses asked of me.”
Alexia exited the comfort of the womb at 9:15 p.m. Nurses swooped her up to attend to the tiny newborn, who weighed in at 1 pound 11 ounces.
Doctors intubated the newborn and placed her on a ventilator because her tiny lungs were premature and not fully developed.
At about 3 a.m., the specialized neonatal transport team brought Alexia to Helen DeVos Children’s Hospital, where she became a 10-week resident of the Small Baby Unit at the Gerber Foundation Neonatal Center. Designed for “micro-preemies” born before 27 weeks, the Small Baby Unit is one of only a few in the country.
Less than half a percent of babies born at Spectrum Health arrive before 27 weeks gestation.
“We care for approximately 50-60 babies every year that are born less than 27 weeks gestation,” Dr. Haines said.
Most are born at Spectrum Health Butterworth Hospital; some at community hospitals.
Having dedicated “small baby” space on the neonatal unit allows for highly specialized neurological care that promotes healthy brain development in the fragile micro-preemie population and helps parents facing similar circumstances form close connections and sometimes lifetime bonds.
The environment in the Small Baby Unit is dark and quiet. Special precautions are made to minimize stimuli that could cause stress to critically ill neonates like Alexia.
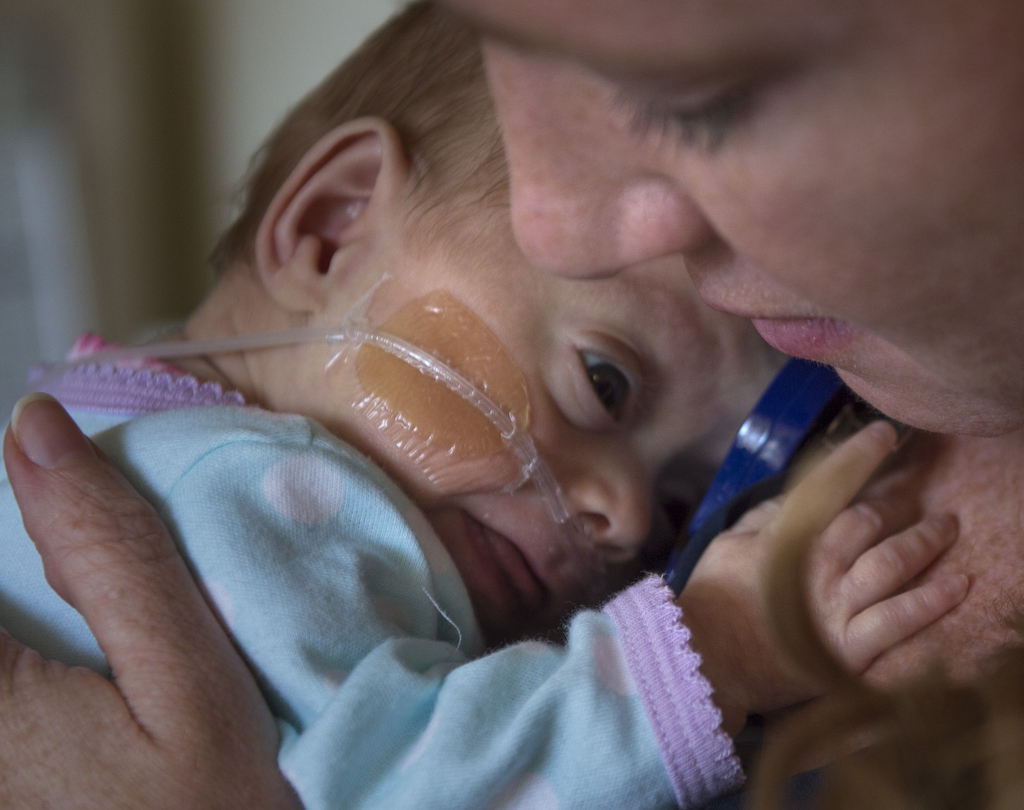
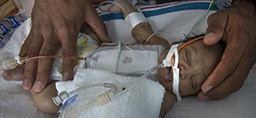
Despite how tiny these babies are, parents are encouraged to not only touch and talk to their baby, but also provide skin-to-skin care as often as possible, even if the baby is on a ventilator. Studies show skin-to-skin contact promotes healthy neurological development, weight gain, growth and bonding.
Emergency surgery
For the first three weeks, Danielle and John spent almost 24/7 next to their child.
“The first couple of days, it seemed like she was doing just fine,” Danielle said. “Her eyes were fused shut and we had to wait for them to open on their own. It seemed like we were doing OK until Aug. 14, four days after she was born.”
Alexia’s belly kept increasing in size, and grew firm.
“They called us at 6:45 in the morning and said, ‘Your daughter needs surgery on her intestines,’” Danielle recalled. “There were several perforations in her intestines.”
The emergency surgery resulted in an ostomy. In November, doctors performed another surgery to reattach Alexia’s bowels.
Danielle said much of her comfort came from being with other families in the small baby unit who faced struggles similar to their own.
“It was kind of special,” Danielle said. “Being our first child and going through this experience, it helped to have a specific type of room dedicated to the situation we were in. It’s helpful knowing other families in the room are going through the same fears and anxieties that go along with having such a small baby.”
Danielle and John practically lived in the dark and quiet environment with their daughter. Alexia provided the light.
“They tried to keep it as quiet as possible even through the constant flow of doctors and nurses coming in,” Danielle said. “For the babies, they cover their eyes with a felt piece of material to keep it as dark as possible to simulate being in the womb.”
The days were difficult. Babies are made to hold, and cuddle.
‘You can do it’
“We would just talk to her, encouraging things like, ‘You’re going to be just fine, you can do it,’” Danielle said. “We spoke very encouraging words to keep her going and to keep ourselves going. Deep down, I was telling myself everything was going to be OK, but we definitely had some scary times.”
Like the phone call when their baby needed bowel surgery, then surgery to close her patent ductus arteriosus, a blood vessel near her tiny heart. There were also lung issues and high blood pressure problems.
“Every day had a new challenge,” she said. “You never knew what you were going to face. Or what would be coming.”
But their little one showed spunk, and fight.
“She kicks her legs constantly,” Danielle said. “There’s just a spunk to her. She’s got a lot of energy and she’s very expressive with her face.”
After 10 weeks in the small baby unit, Alexia and her family graduated to Room 12, a transitional nursery. The lights came up, and so did the volume level as she assimilated to life outside her pseudo-womb environment. She is still on nasal cannula oxygen, and her progress is a breath of fresh air for her parents.
Dr. Haines said she expects a positive future for her tiny patient.
“Alexia has progressed well during her NICU course,” Dr. Haines said. “I expect her to do very well. She’ll have close follow-up in our Neurodevelopmental Pediatrics Clinic. It’s important to track development and figure out different resources she may or may not need.”
Danielle and John also received a lot of education on her care, including developmental exercises they can do at home.
“She’s very appropriate and right on track,” Dr. Haines said. “They’re armed with the tools and the best resources to optimize Alexia’s best outcome.”
Dr. Haines has watched Alexia come full circle.
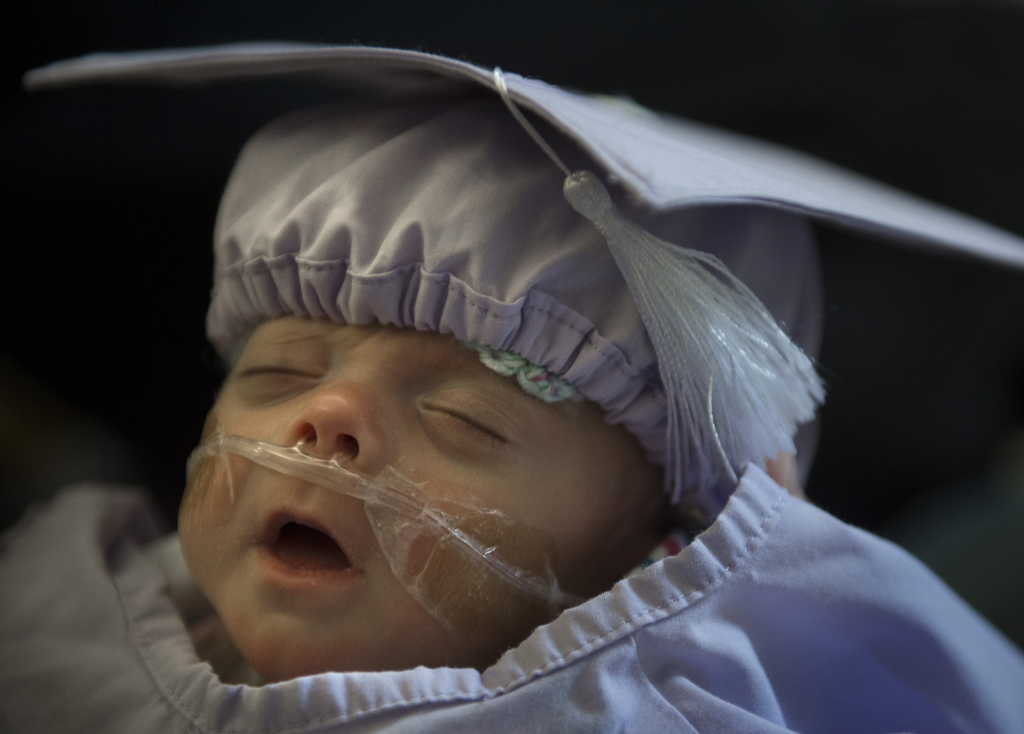
“Going home is a pretty momentous occasion for her and her family,” Dr. Haines said. “It’s really a celebration, a graduation for them. I was on call the night she arrived so it’s exciting and rewarding to be the neonatologist to discharge her home.”
Alexia is eating well, growing and Danielle is beginning to work on breastfeeding.
“We found a groove for her that she was able to gain weight,” Danielle said. Crossing that hurdle made the next goal obtainable—bringing their baby home by Christmastime.
It’s hard to imagine any gift they receive on Dec. 25 will be more meaningful than the one they received Saturday—a baby, in swaddling clothing, coming home.




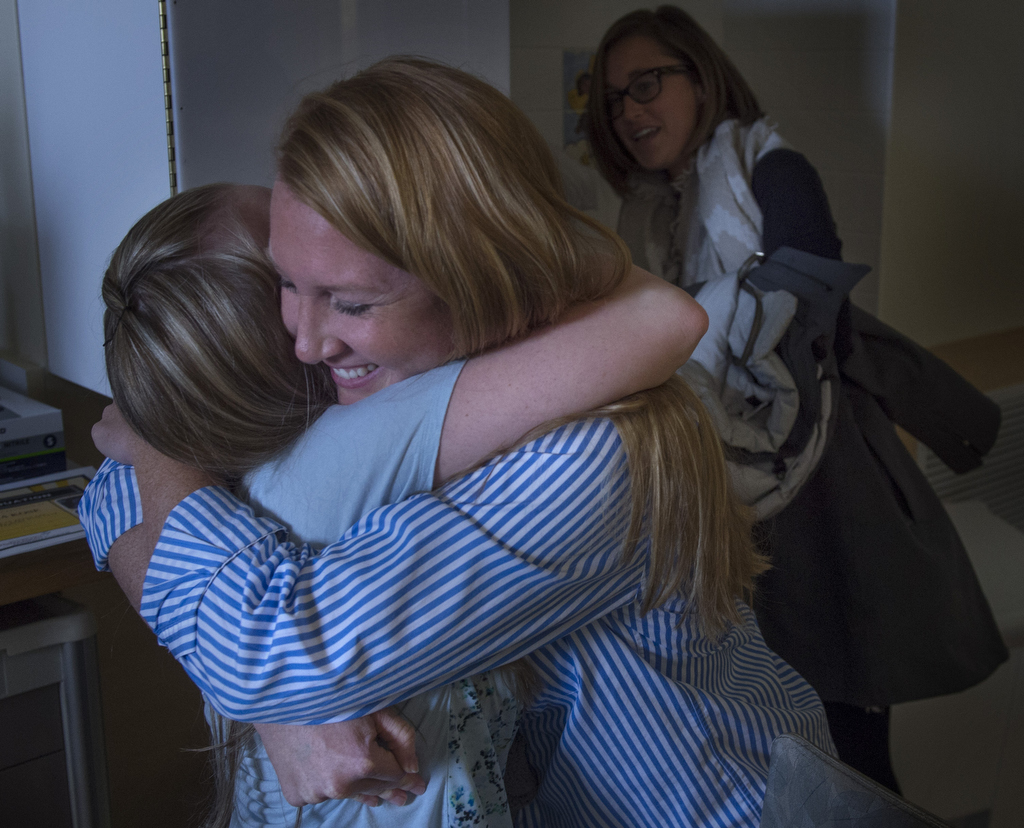




























 /a>
/a>
 /a>
/a>
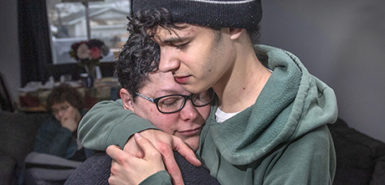 /a>
/a>
This story really hit home my daughter was born at Butterworth waiging at 1pound and 9 ounces and was 12 ” long. We couldn’t hold her for for 2 months. But when we could it was heaven. My baby girls name is Anna Nichole ferrill and she is such a fighter. She is 19 now and the only thing you can tell the the something from her birth was her height. She is done growing at 5′ 9″. But she is ok with that. She is a very loving and kind hearted person and would do anything for anyone. She gets a kick out of me telling her about how she was born and her seeing how small she was. I had to have a coaction. And I loved all the drs and nurses there !!!!! They was so helpful with everything.
I had a premi and he is now a top leading engineer in the race car division at Honda. His beginning wasn’t normal & at first we thought that he was blind. It took 9 months before he could focus. He had a horrible time walking and fell up until he was six. This little one has a wonderful chance. Never give up. Physical therapy daily is a must. God bless
John and Danielle, not many people get to experience miracles as profound as this miracle of life in your little baby. Her miracle story will always be a miracle and that will bring many people back to God. For God’s not dead he is alive and in the life of this little baby we see that. May she growi n holiness as she sees how God loves her so personally. We will continue to pray for you all as you begin your new life as a family.