In January 2019, David Bell noticed his health begin to change. He felt fatigued and short of breath.
But he didn’t have time to be sick.
His elderly father, facing daunting medical troubles, had a series of upcoming appointments with doctors. Bell needed to be there for his dad.
But it didn’t come easy. Things had gotten busier at work and Bell already had to make a 200-mile daily commute from rural Shaftsburg, Michigan—a tiny dot on the map near Lansing—to his job in Portage.
So he did what any loving son and hard worker will do.
He pushed through as best he could and chalked up his fatigue to a lack of sleep and too many worries about his dad.
One Tuesday evening in January, however, the day before a worrisome medical appointment for his dad, Bell began to feel particularly run down.
By Wednesday, “I kept noticing I was out of breath and even had to sleep propped up on pillows that night,” he said.
He quietly promised himself he’d get it checked out. Still, he didn’t want anything to interfere with his dad’s appointment.
“We knew that was going to be the time he heard, ‘You have prostate cancer,'” Bell said. “And I so wanted to be there for him.”
The following day, he managed to get his father to the doctor’s office.
All the while, Bell’s breathing grew labored. “It felt like knives were stabbing into my back,” he said.
After his father’s appointment, Bell asked his wife, Michelle, to drive him to the hospital in Grand Rapids, about 100 miles away.
They soon arrived at the Spectrum Health Butterworth Hospital emergency department, where doctors quickly found an infarction in the lower third of Bell’s right lung.
The good news? His heart appeared healthy.
The bad news? A massive bilateral pulmonary embolism threatened his life.
Thanks to blood thinners, pain medication, oxygen and four days in the hospital, he recovered quickly. And besides being grateful about his lungs’ ability to regenerate, he promised himself to be more mindful of symptoms.
He continues to feel grateful to the ER staff. “The doctors worked so quickly to diagnose me, and the nursing staff took such exceptional care of me during my stay,” he said. “Because of their care and many prayers on my behalf, I’m here to tell about it.”
A dire diagnosis
Bell has venous thromboembolism, an umbrella term that includes blood clots called deep vein thrombi, which often develop in deep leg veins. It also includes pulmonary embolisms like Bell’s, which occur when clots break off from vein walls and travel through the heart to the pulmonary arteries.
Statistically, Bell is incredibly lucky.
According to The Centers for Disease Control and Prevention, about 1 million people suffer from deep vein thrombi—and about 100,000 of them die each year. In as many as 25% of cases, sudden death is the first symptom.
Bell had a history of superficial blood clots in his legs, so he knew he had some issues with his veins.
More than two years later, he’s still shaking his head at the way he delayed seeking treatment.
“Waiting a few days to get it checked out? That was not the smartest thing I’ve ever done,” he said.
Recently, he had another clot, which he had treated at the Spectrum Health Vein Center. Because this was on the surface, doctors didn’t remove it. But he received injections known as sclerotherapy, which causes the vein to scar. That forces the blood to find healthier veins to travel through.
“By closing down these veins, we prevent future events,” said Jennifer Watson, MD, the Spectrum Health vascular surgeon who performed the procedure.
In the past, doctors often treated deep vein thrombi with a technique called vein stripping. “Now we just treat them from the inside,” Dr. Watson said. “And the body gradually absorbs the shut-down veins.”
While the precise cause of deep vein thrombosis is still something of a mystery, experts know that in about 90% of cases, the clots that form pulmonary embolisms come from the legs, Dr. Watson said.
The legs have many veins. While it’s easy to think of arteries as carrying blood throughout the body and veins returning it, “veins are also sort of a holding system,” she said. “When your blood volume is up a little, you need space to put that blood in the veins. So there’s lots of blood volume there.”
One theory: Clots form because veins in the leg are very long, with long columns of valves.
“If you have any difficulty in those valves, that is a more likely place to form clots,” Dr. Watson said. “And there’s a lot of the blood in the legs at any given time.”
Warning signs include swelling and calf-cramping, particularly if it’s in one leg.
“Often, people will say something like, ‘It feels like I’ve pulled a muscle, but I wasn’t doing anything strenuous,'” Dr. Watson said.
Chest pain and shortness of breath are also signs of trouble.
“That’s our worst-case scenario—when the clot breaks off and travels to the lungs,” she said. “That can cause significant chest pain and shortness of breath.”
Once someone has an embolism, they continue to be at risk for future events.
It’s important to know the warning signs, and it’s critical to make sure vascular issues are adequately reflected in medical records, she said. You should always tell health care providers about your vascular history.
“Any type of surgery, trauma or prolonged travel has some risks,” she said. In some cases, doctors recommend compression socks, especially while traveling.
Making health a priority
Bell, now 60, said his intense experience has given him a new lease on life. He’s savoring time with his family, which includes four children and two grandkids.
He’s also managing his health by staying active, with plenty of cycling alongside Michelle on Michigan’s beautiful back roads.
During his long commute for work, he now takes breaks at rest stops. He’s mindful of his legs when on his feet for long periods of time.
He now takes a blood-thinning medication that drastically reduces the likelihood of a recurrence.
But most of all, he looks to his dad as his favorite role model.
His dad is still going strong, even after a diagnosis of prostate cancer.
“He’s 91 going on 71,” Bell said. “After 65 years, he still works part-time as a pastor. When my wife called to tell him my diagnosis that day, even though he had just learned he had cancer, he said, ‘Tell Dave I’ll be praying for him.'”
That generosity, Bell said, is just the kind of inspiration he needs to keep life—and health—in perspective.




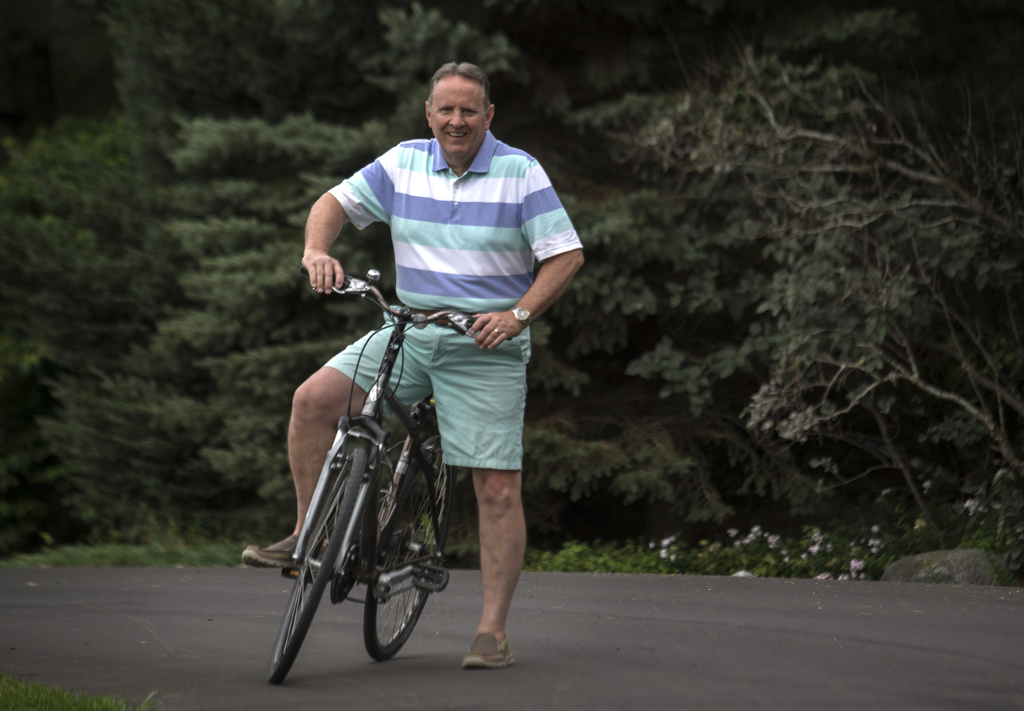

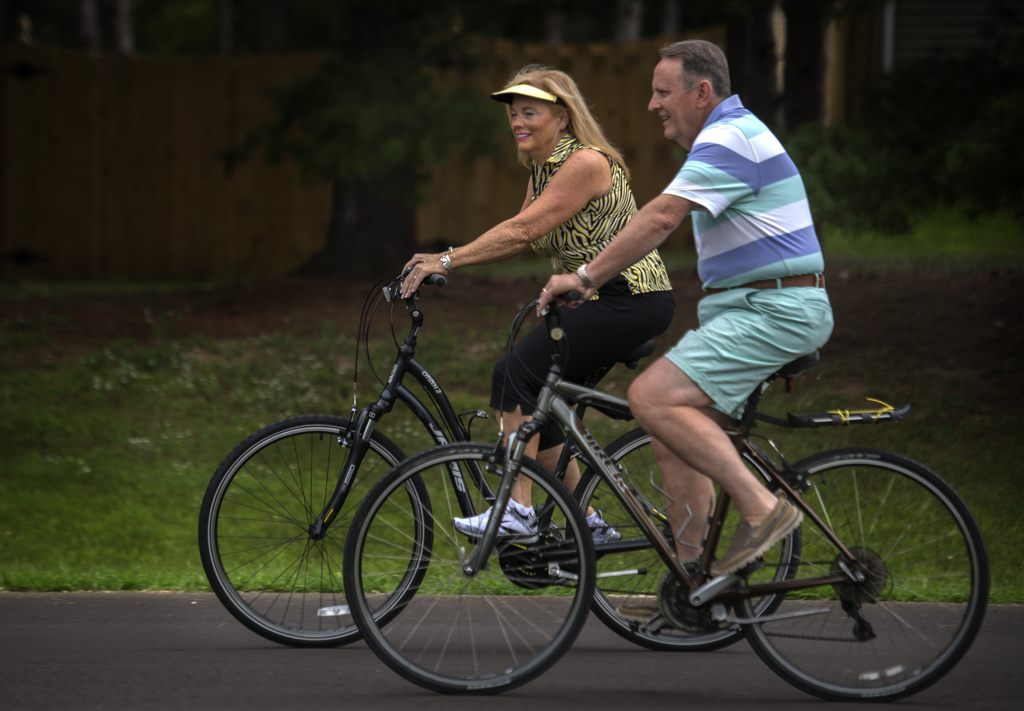









 /a>
/a>
 /a>
/a>
 /a>
/a>
Dave and Michelle are my across the street neighbors. You could not ask for any nicer or more caring people to live close to. He is always there to help if you need it. During the initial stages of his illness he did spend more time in the rest mode and riding his bike everywhere. We tried to return all his help with little things. Dave is back to his “old” self 🙂 Learning what he did go through makes me think that we all need to react to our bodies more and get help before something serious happens. I just was in the hospital with a stroke and I believe I have some vein problems in the back of my neck. I need to call Spectrum Health Heart/Vein Center and make an appointment. Thanks Dave! So glad you’re doing so well.