Bob Verburg had adjusted to living with a mechanical heart pump. He felt grateful for it. The technology had, after all, saved his life.
But that didn’t mean he always liked it.
The system’s external components—two battery packs hanging from his shoulders and a controller strapped to his waist—were bulky to wear. And with the controller wired through his abdomen to a pump attached to his heart, he couldn’t be around water.
No showers, no swimming and no time on his boat.
“It was 24/7 with that baby,” said Bob, a resident of Grandville, Michigan. “We got really acquainted.”
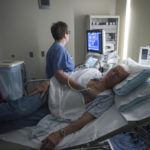
Doctors surgically implanted Bob’s heart pump, known as a left ventricular assist device, or LVAD, at Spectrum Health Fred and Lena Meijer Heart Center shortly after Christmas 2015.
Signs of advanced heart disease, especially shortness of breath, had popped up rather suddenly for the retired industrial engineer and Navy reservist, who at age 77 still worked part time for a funeral home.
Serious breathing trouble landed him in the hospital one December morning. Soon Bob and his wife, Carol, learned he had a faulty aortic valve that had led to a weak, enlarged heart.
Two-part surgery
The medical team decided to do a double surgery—part one to replace his heart valve and part two to insert the LVAD. His heart had grown too weak to pump blood through a new valve on its own, so he needed help with pumping. But having an LVAD alone wouldn’t have worked either, given the extent of the damage to the valve.
Without this twofold solution, he probably would have had six months to live on medication, Carol said.
The operation was successful. Because it had been a major surgery, however, Bob needed time to bounce back.
He spent winter and spring 2016 in rehab—first at Spectrum Health Blodgett Hospital, where he received physical, occupational and speech therapy, and later at home, where he continued therapy with the help of Spectrum Health At Home Visiting Nurse Association.
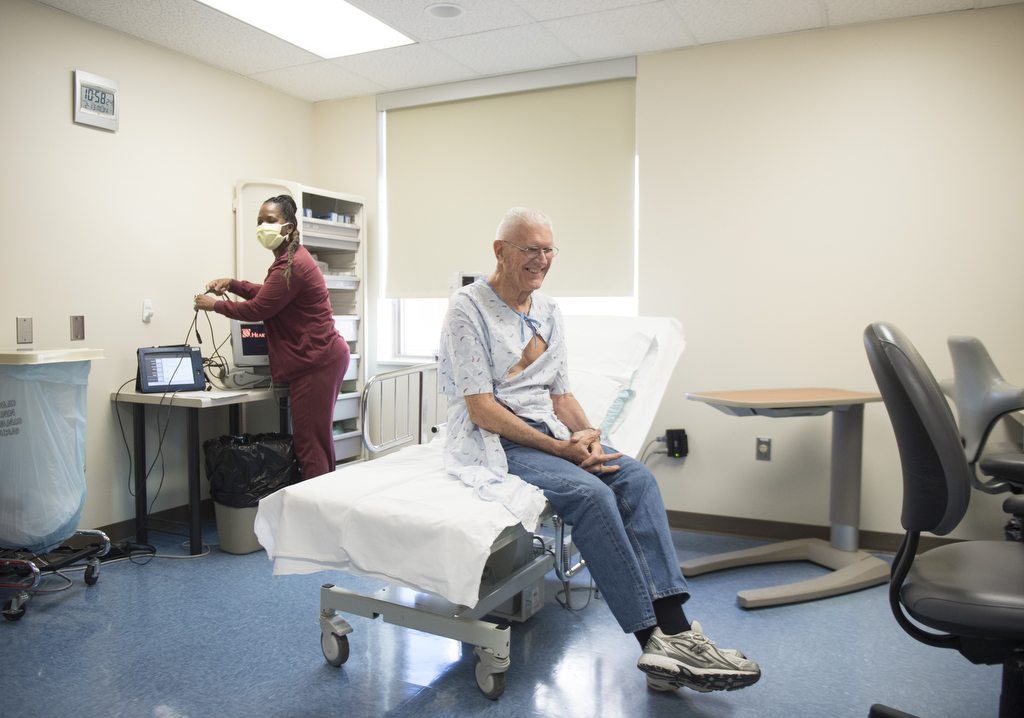
By summertime he and Carol, his trained LVAD caregiver, had settled into the new daily routines that came with having a heart pump—keeping the portable batteries charged, changing the dressing around the driveline site in his abdomen and plugging into a wall power unit at night.
They knew they were in it for the long term because Bob’s age made him too old for a heart transplant.
But then something unexpected happened.
His heart started recovering.
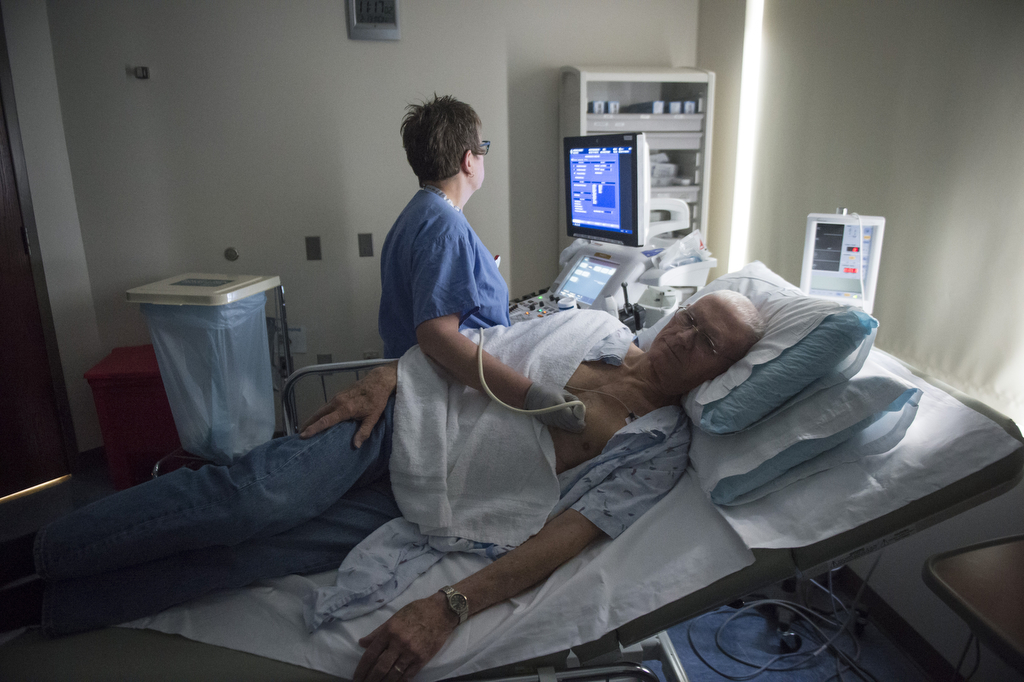
The first signs showed up in routine heart tests, and his cardiology team grew cautiously optimistic.
Then a “low flow” alarm began sounding on Bob’s LVAD controller. The device wouldn’t take in enough blood because his heart was stealing some of the blood.
“The beeping started in May or June, and it kept getting worse,” Carol said. “We never knew where it was going to happen—during the night, at church, or at the symphony or wherever. … He could push it off and it would come right back on. It was very nerve-wracking.”
Pump removal
Later that summer the doctors raised the possibility of removing the LVAD, a surprising development for both the Verburgs and the medical team.
“We were not expecting Bob’s heart to recover,” said Asghar Khaghani, MD, FRCS, a cardiothoracic surgeon with the Spectrum Health Richard DeVos Heart and Lung Transplant Program. “But … he recovered completely, to the extent that his own heart was competing with the device.
“That’s unusual, especially at that age,” Dr. Khaghani said.
Unusual, but not unheard of.
Dr. Khaghani, known internationally for his LVAD surgery expertise, has performed about 35 LVAD removals in his career, including six at Spectrum Health.
Bob stands out as the oldest, said Dr. Khaghani, who removed his LVAD the day after Thanksgiving, 11 months after it had been implanted.
The LVAD had kept him alive long enough for his heart to heal.
“His aortic valve disease made his heart weak, and after the aortic valve replacement there was an opportunity for his heart to recover, even though it was very dilated,” Dr. Khaghani said.
Patients like Bob “need a period of rest for the heart to shrink, because without the device it won’t shrink, it will remain distended,” the doctor explained. “You have to give them a period of survival without heart failure, and with the medical treatment continuing.”
It doesn’t always work, Dr. Khaghani said, adding that using LVAD as a bridge to recovery remains an area of research.
“We still don’t know why some patients recover (on the device) and some don’t,” the doctor said. “We still don’t know what triggers the recovery at the molecular level.”
Newfound freedom
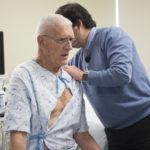
Today Bob’s heart is functioning normally. His ejection fraction, which at its weakest stood at about 10 percent, is close to 60 percent, which is normal, Dr. Khaghani said. He will continue to see his cardiologists, Milena Jani, MD and Michael Dickinson, MD, in the Advanced Heart Failure Program over the long term.
“I think that his prospect is very good. I would expect him to have normal life expectancy,” Dr. Khaghani said.
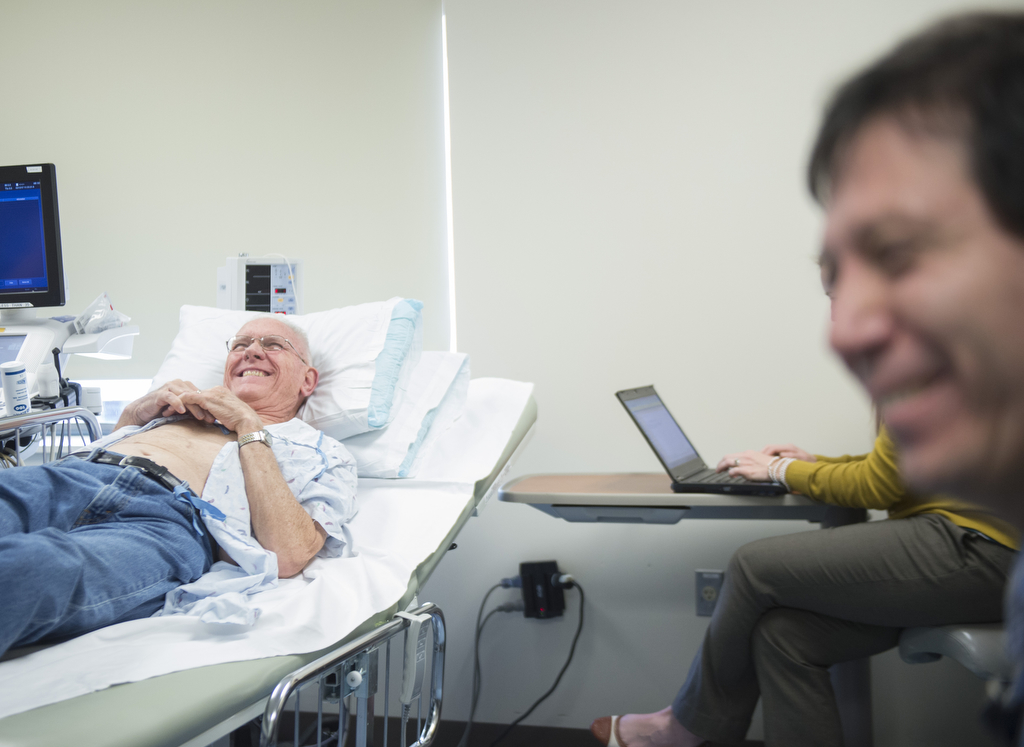
The Verburgs are delighted with Bob’s new independence and the added time they’ve been given together.
“It’s unbelievable,” Carol said. “But you know what? We credit a lot of it to all of the prayers that were offered for us through all of this. We never would have made it this far otherwise.”
Bob still struggles with some lingering short-term memory loss, which Dr. Khaghani said is common after cardiac surgery.
But he is back behind the wheel and he has joined a community choir. And he’s packing his bags for a month in Florida.
“I’m not idle. I’m always on the move,” he said. “It feels good.”














 /a>
/a>
 /a>
/a>
 /a>
/a>
Praise God! He answered prayers. Praise God for the gifts He gives to the medical community and their love for their professions.
Bob, so happy to hear of the amazing recovery. Praise God from whom all blessings flow. Prayers were answered.
Bob, so happy to hear of the amazing recovery. Praise God from whom all blessings flow. Prayers were answered.
Bob and Carol are very special people who are loved by many. Prayers were said daily by for Bob’s recovery and also for Carol who was always there. The doctors and staff who diligently took care of Bob were also upheld in prayer. God’s richest blessing to all who participated in Bob’s miraculous recovery. God is Great.
God is so gooc!! Bless u, your wife & family!! God can do anything but fail!!! I Have a difribulator implanted in my chest!! It went off 6 times back to back
I received my LVAD May 2015. I am experiencing short alarms. I work out 5 days a week, and have reached 300 pounds on my bench press. I have backed down some, but am doing very well for a 69 year old. I go in next week at UNC to see about pump replacement. We will see whether I go that route.
Best wishes to you, Alan.