What a difference a year makes.
In July 2020, the first time Katie Rushlow met the two Blain brothers, they were squirming in their mother’s arms.
A year later, Rushlow laughs when she sees Daxton, 2, squat down and peek into the room where he gets his weekly infusion.
The little blonde boy grins and pops in with a giggle, ready to sing along with Katie Rushlow.
Rushlow is the Gen. John and Maureen Nowak music therapist with the Edward and June Prein Family Pediatric Music Therapy Program and part of the Child Life team at Spectrum Health Helen DeVos Children’s Hospital.
Daxton has the same birthday as his brother Sawyer, 4.
They were born exactly two years and 10 minutes apart.
The brothers have a rare genetic disease called Hunter syndrome, also known as MPS II, referring to a metabolic disorder called mucopolysaccharidoses.
It’s caused by a missing or malfunctioning enzyme that normally breaks down toxic molecules in the body.
When the enzyme is absent, the molecules accumulate and cause permanent and progressive damage that affects appearance, cognitive development, organ function and various physical abilities.
Symptoms usually begin to show at about ages 2 to 4. It affects mostly boys.
Although there is no cure, weekly infusions of an enzyme replacement therapy slow the process of physical decline.
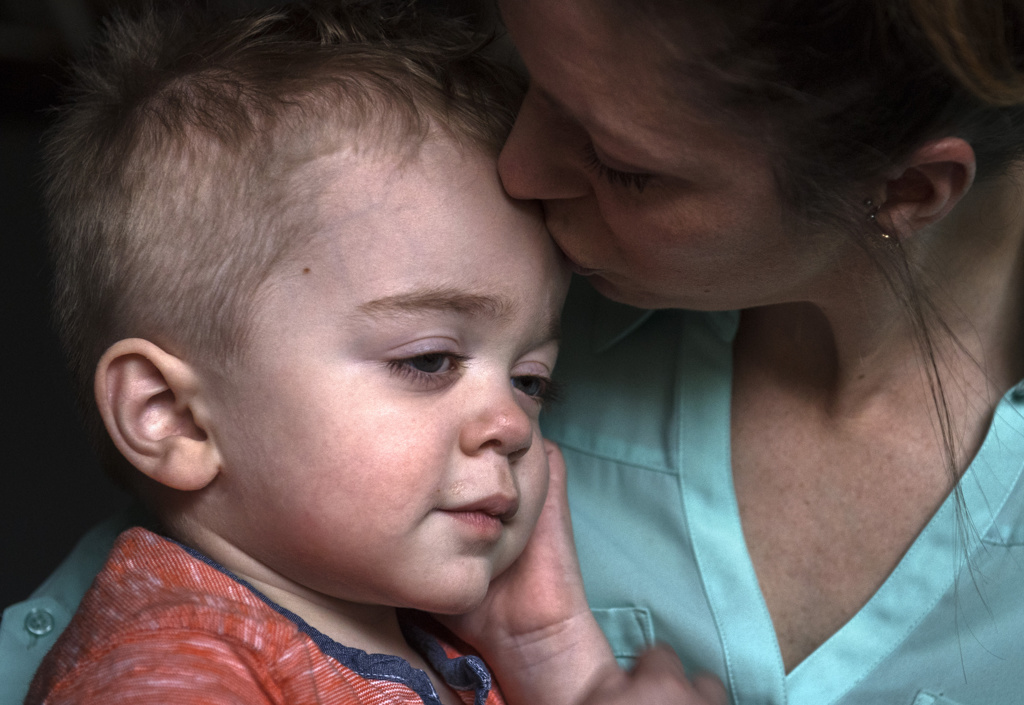
“The boys have come so far in this past year,” Rushlow said. “At the beginning, they were so stressed that Daxton especially would forget to breathe and the boys would need to be reminded to take a breath.
“But we do all we can to distract them during the process and reduce anxiety for them and the whole family,” she said.
“Sometimes if the boys were having a hard day, keeping mom and nurses calm was our main goal. It truly is a group effort. Our interactions with the boys are a perfect example of working as a team to treat the whole patient. The Child Life team works together using different techniques, tools, and diverse education to ultimately help these boys cope, reduce their anxiety and make sure they feel safe and heard.
“And now it’s become a part of their lives—not pleasant, but a routine to which they have become accustomed.”
Early clues
Both boys were healthy at birth, said their mom, Cory Blain.
“In utero, during an ultrasound, the doctor noted enlarged kidneys with Sawyer, but follow-ups showed that that diminished,” Cory said.
Cory, of Saranac, Michigan, has worked in the health care field.
She has an eye for things that seem amiss.
“During his first year, when I was giving Sawyer a bath and his hair was wet against his head, I felt like his head was maybe an odd shape, maybe a little too large,” Cory said. “I asked the pediatrician and she said yes, a bit large, but she was not concerned.”
At about the time Sawyer reached age 3, Cory noticed something unusual. As he was in bed to be tucked in for the night, she ran her fingers through his hair.
“And I noticed an odd ridge down the center of his forehead,” Cory said.
Back to the pediatrician. This time, a new one.
The doctor spoke of something called storage disorder, indicating an abnormal accumulation of a substance in the boy’s body.
“At first I didn’t see it, but I do now,” Cory said. “The doctor spoke about coarse facial features. His eyes were a little more set apart, his lips a little plumper, his nose a little flatter and wider and his hair was coarse.”
The pediatrician recommended a genetic test.
Finding answers
Cory took her son to Helen DeVos Children’s Hospital for a genetic test. The results came back within four to six weeks.
“We found out that Sawyer had a rare genetic disease called Hunter syndrome,” she said.
Cory began researching to learn more. Until then, she didn’t even know this disease existed.
She connected with the National MPS Society to learn about current research.
Doctors referred Sawyer to various specialists to check him over, head to toe.
“Because this disease, I found out, can affect everything,” Cory said. “The specialists wanted to get a baseline for Sawyer for hearing, heart, lungs, joints, bones—everything.”
And there was more.
By this point, Sawyer had a little brother, Daxton.
Could it be that Daxton, too, had inherited this genetic disease?
“The odds were 50/50,” Cory said. “We prayed so hard that Daxton might be spared.”
Two weeks later, test results showed Daxton, too, had Hunter syndrome.
Doctors checked him head to toe.
“Daxton has hip dysplasia,” Cory said. “He now sleeps in a brace for that.
“Both boys also had sedated hearing tests that showed hearing loss,” she said. “And I learned that was common with MPS II. So they will both be fitted soon for hearing aids.”
Time for fun
As the routine for weekly infusions began at Helen DeVos Children’s Hospital, the family came under the care of the hospital’s Child Life team—specialists in child psychology, development, education and therapeutic recreation.
Child Life specialist Erica Tooker had first met the brothers in January 2020.
“Our team used various distraction techniques to ease anxiety,” Tooker said. “We provide psychosocial support to normalize the environment for them, such as exploring the medical instruments that will be used together.”
The boys received their infusions together, a five-hour procedure.
Mom would hold one boy while their Grandpa Tim, called Papa by the boys, would sit with the other brother.
“Over time, we settled into that routine,” Cory said. “Their grandpa would come along to occupy one while I took care of the other brother.”
Tooker showed the boys some of the medical instruments and explained the procedures in a way the brothers could grasp.
As blood pressure cuffs squeezed and needles went into arms, team members engaged the boys with talk, song and play.
The distractions helped reduce the stress.
Rushlow’s music therapy worked its magic.
“Sometimes I would put what was happening into a song,” Rushlow said. “‘And now we get a hug on the arm—Ee-aye, ee-aye, oh!’”
Rushlow would play her guitar and, occasionally, everyone in the room—members of the health team, the boys, their family—would break into song.
“Routine can be calming,” Rushlow said.
It’s especially true when medical procedures can seem overwhelming for little ones. Instead of focusing on the discomfort or fear, kids see members of the Child Life team and feel reassured.
And that’s certainly been the case with Daxton and Sawyer.
Over the past year, they’ve progressed tremendously.
“The boys see us now and they smile,” Rushlow said. “They don’t even flinch anymore when the needle goes in. They have become a part of our family.”
For Rushlow, it’s one of the great rewards to the work.
“It’s been such an awesome gift for all of us,” she said.
Brotherly love
Daxton and Sawyer were recently enrolled in a six-month clinical trial in Chicago, Cory said.
Every Tuesday night they leave Michigan and head to the Windy City for infusions on Wednesday. Then it’s back to Michigan.
“The trial is for a new drug that will cross the blood barrier in a way the old one didn’t,” Cory said. “The enzyme replacement therapy they’ve been getting slows down physical decline, but this new infusion should help the cognitive aspect, too.”
The brothers won’t see the Child Life team at Spectrum Health for about another six months. After the clinical trial is over, however, they’ll resume their infusions in Grand Rapids.
The infusions will continue all their lives.
And the brothers will continue playing just as all little boys do—hugging one moment, scuffling the next.
One recent afternoon, they had just such an episode.
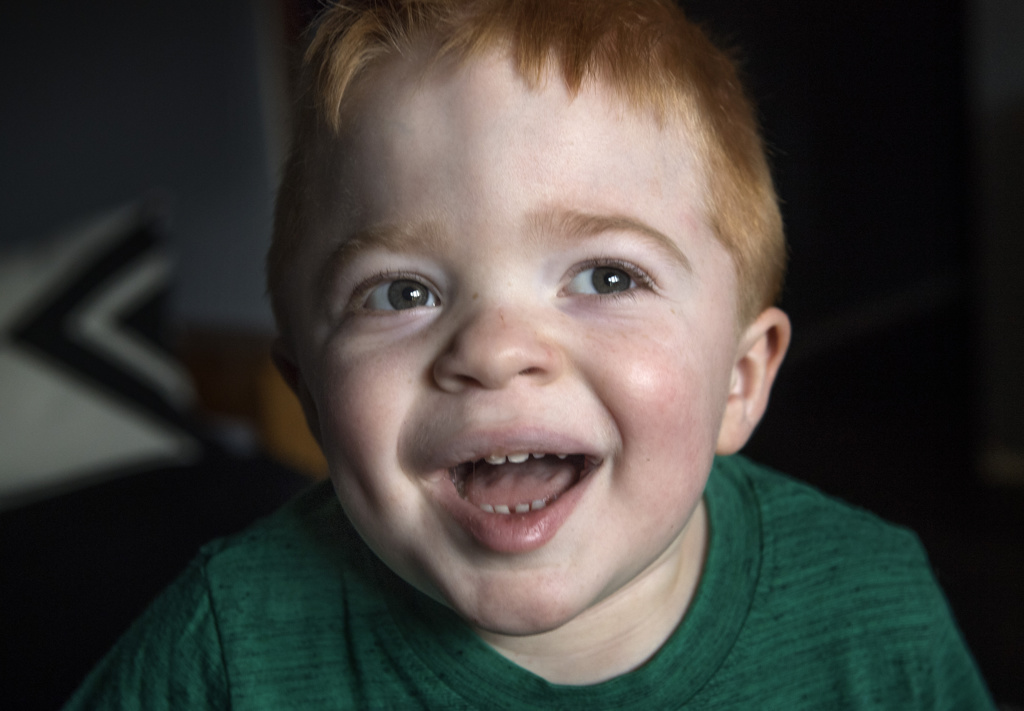
Sawyer’s bright red hair flashed as he wrestled his brother for a favorite toy. A moment of tears emerged, but then disappeared just as quickly when Daxton smiled.
A bright, childlike smile that seemed to say all is right with the world, once again.
Cory finds reassurance in that.
“Sure, there are good days and bad days,” Cory mused. “There’s no time to just sit and think. And that’s probably a good thing. But sometimes it hits hard.
“I’ve learned to soak in all the moments with the boys,” she said. “And I’m grateful that they are able to go through this journey together. They help each other.”



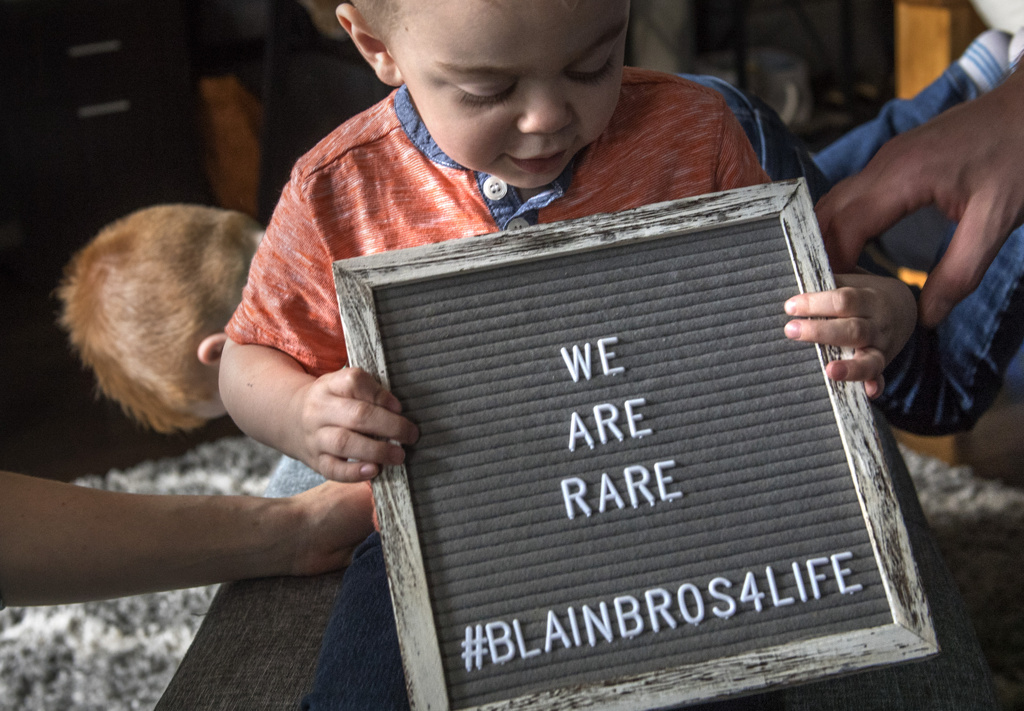






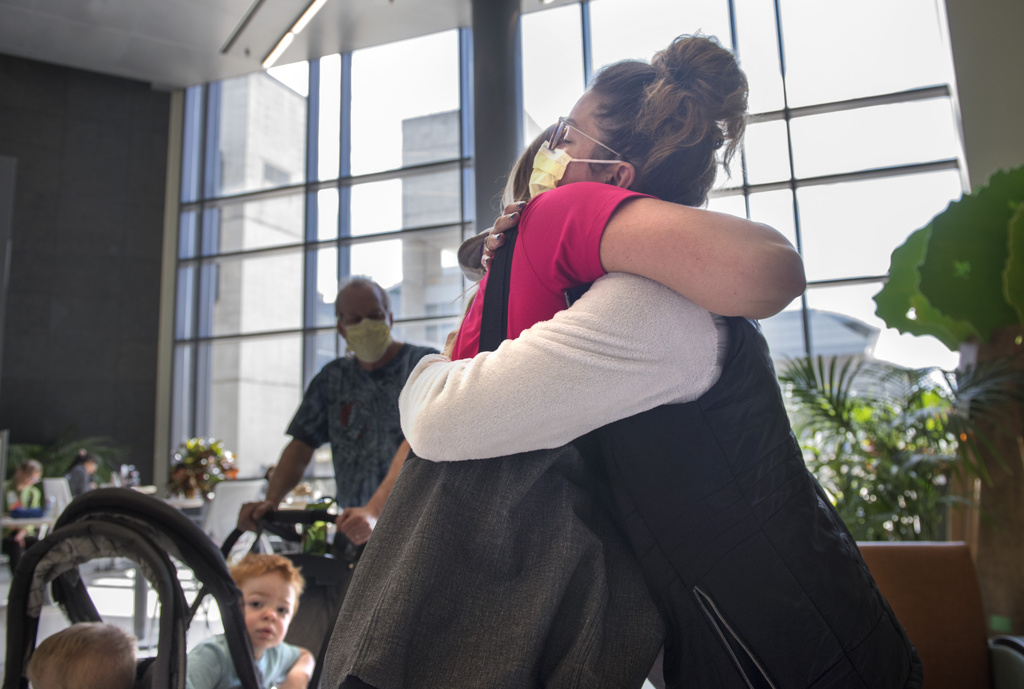


















 /a>
/a>
 /a>
/a>
 /a>
/a>