After tucking their toddler and preschooler in for the night, Alexa Kleinjans and her husband, Brad, climbed into bed, ready for some peace and quiet after a busy August day.
Minutes later, Alexa, 29, felt a sudden, piercing cramp on her left side that escalated to full-on, nausea-inducing pain.
“I got out of bed and vomited all over our bathroom just from the pain,” said Alexa, 22 weeks pregnant at the time.
“I thought I was contracting.”
Sitting in a warm shower eased her discomfort for a time, but the pain ramped up an hour later, making it hard for her to breathe.
Fearing his wife’s pregnancy could be in jeopardy, Brad called his dad to come and stay with the sleeping children.
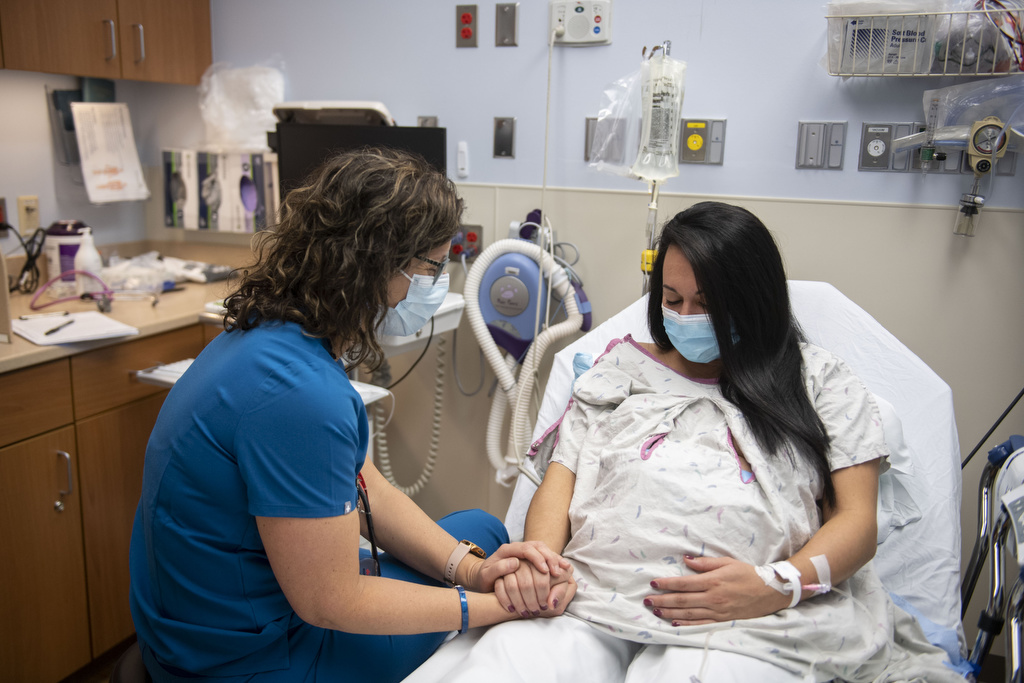
The couple made a hurried post-midnight trip to Spectrum Health Zeeland Community Hospital. There, the emergency department team admitted Alexa and sent her straight to the labor and delivery area, where doctors could evaluate her situation and monitor the baby.
After getting her settled and giving her IV medication for the pain, doctors ordered an ultrasound to identify the source of the trouble.
The images showed a large cyst—more than 5 inches across—near her left ovary. The obstetrician on duty, Darla Olson, MD, called Alexa’s OB-GYN, Dawn DeWitt, MD, to discuss her treatment.
It seemed clear Alexa would need surgery to remove the cyst, but what would be the best route—make a large open incision or perform the procedure laparoscopically, with a few tiny incisions?
Laparoscopy
As the doctors discussed minimally invasive approaches, they called in their colleague Todd Van Heest, MD, an OB-GYN with expertise in advanced laparoscopic techniques. He reviewed the case and helped consider the options.
“These are tough calls to discern sometimes,” Dr. Van Heest said.
A major factor, he said, involved how well he’d be able to maneuver his surgical scopes, given Alexa’s pregnancy.
At 22 weeks, there’s not much room in the abdomen and “you’re operating literally next door to the pregnant uterus,” he said. “You’re at considerable risk for preterm labor.”
On the other hand, if they performed a traditional surgery, Alexa would be left with a long abdominal incision that would have to heal as her uterus continued to grow—another “less than desirable” situation, Dr. Van Heest said.
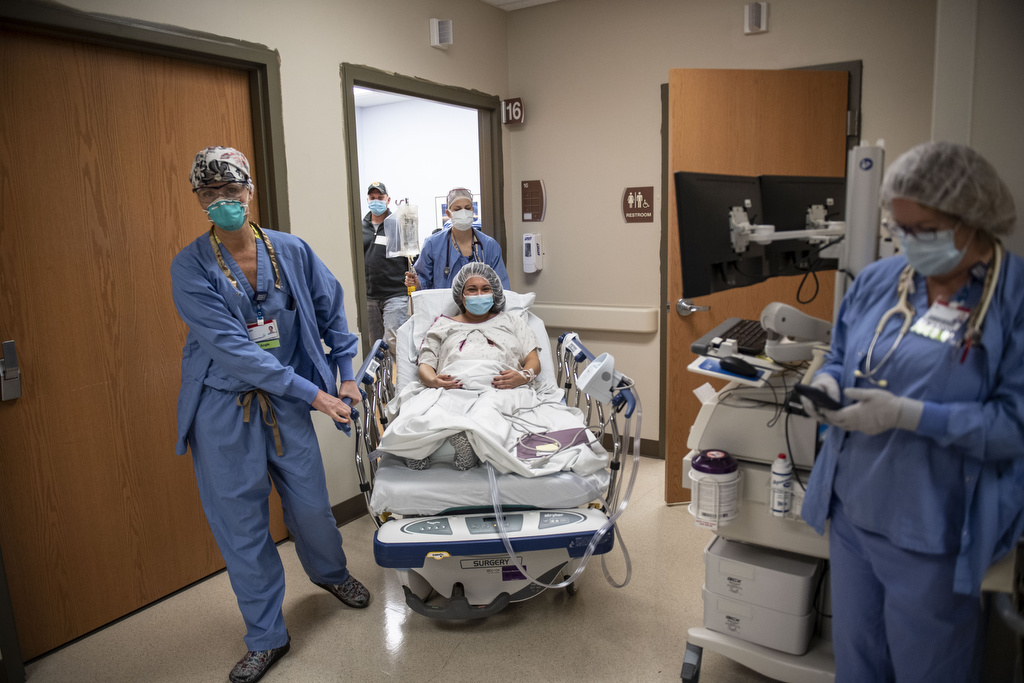
The team decided it made the most sense to do it laparoscopically, placing the ports in locations that would avoid interference with the uterus.
After praying about the doctors’ recommendation, Alexa and her husband felt good about the decision.
“My doctors were just like, ‘We know this is going to be super hard and scary, but … we have to remove this so the rest of the pregnancy is OK,’” Alexa said.
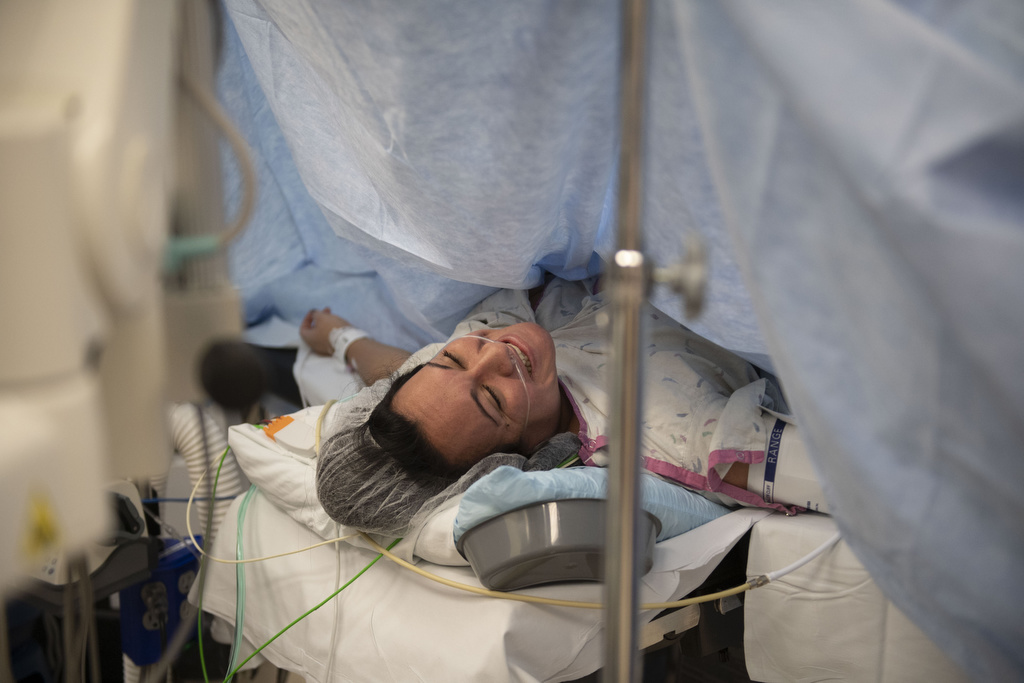
“When they went into surgery, everyone—the anesthesiologist, Dr. Van Heest, Dr. Olson—it was so nice to have that mindset that they all knew what they were doing, and they were so confident and so kind.”
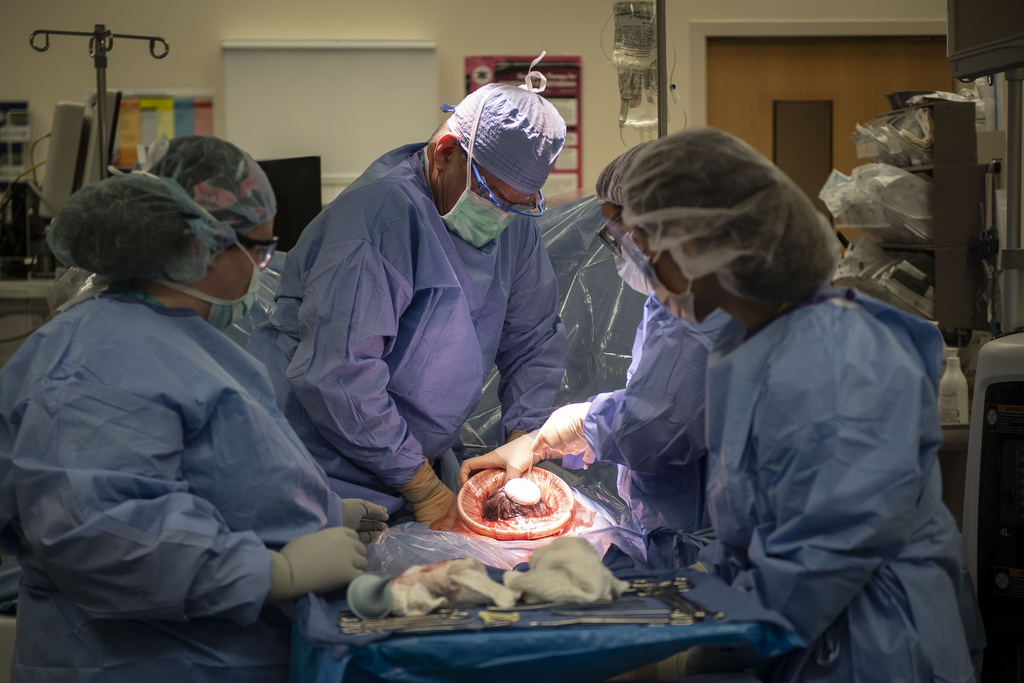
When he got the scopes in, Dr. Van Heest found it difficult to get a clear view of the cyst.
“The whole bottom part of the abdomen is occupied by the uterus,” he said. “And then you’ve got this big cyst that’s competing for space, and it was really just very awkward to try to sort out what was what.”
To make room to move around inside, he had to decompress the cyst, which appeared to be filled with a clear fluid.
After draining some of the fluid—capturing it so it could be tested for the presence of cancerous or precancerous cells—he could see the cyst originated not from the ovary but from the left fallopian tube.
Because of its weight and size, the cyst had twisted and turned on its axis, cutting off the blood supply to the left ovary.
This strangulation of the supply line—the source of Alexa’s pain—had caused discoloration of the ovary.
Alexa’s left fallopian tube would have to come out.
As Drs. Van Heest and Olson worked to remove the tube and a portion of the cyst through the laparoscopic ports, they kept an eye on the ovary to see whether its coloration would improve.
“You don’t want to leave a dead organ in the body. But on the other hand, you don’t want to take out an ovary and push the patient that much closer to possible menopausal changes,” Dr. Van Heest said.
As he watched, he could see the ovary improving, “not looking as dusky as it did at first,” so he felt comfortable leaving it in place.
Throughout the surgery, Alexa experienced no preterm labor. As her nurse told her when she woke up, the baby’s heartbeat remained steady throughout the procedure.
“Baby did not even know that anything was happening,” Alexa said.
‘It looked amazing’
With a successful procedure behind her, Alexa returned home to her family two days later.
Tests on the cystic fluid came back clean, and she had a routine pregnancy until her scheduled cesarean section.
Dr. Van Heest, having brought Alexa through her laparoscopy, agreed to assist Dr. DeWitt with the C-section. He looked forward to seeing how the surgical site would look 17 weeks down the road.
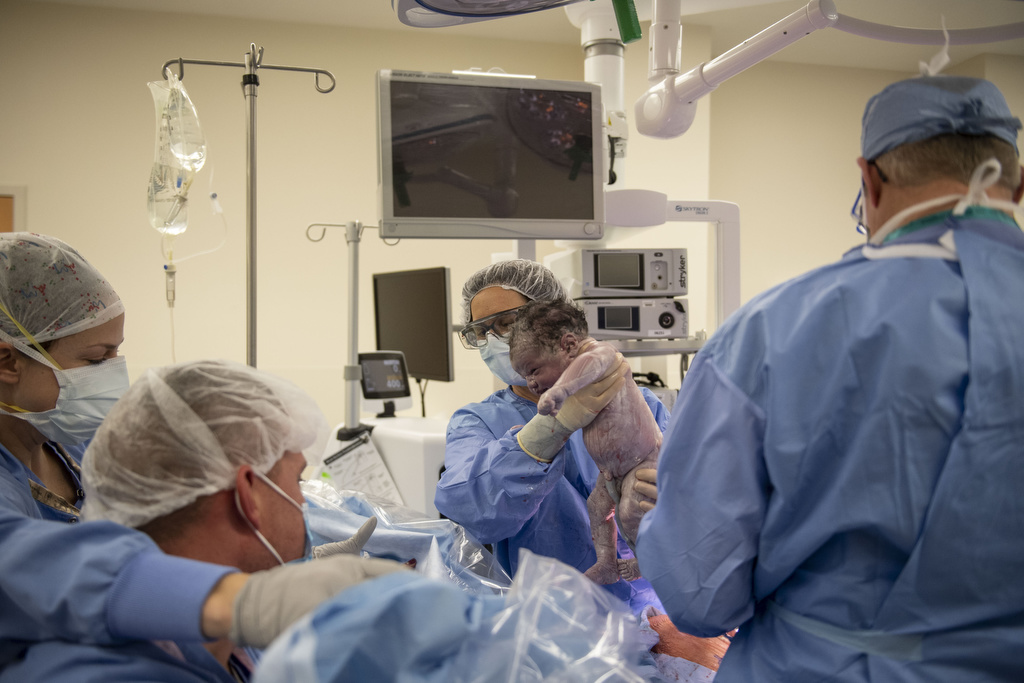
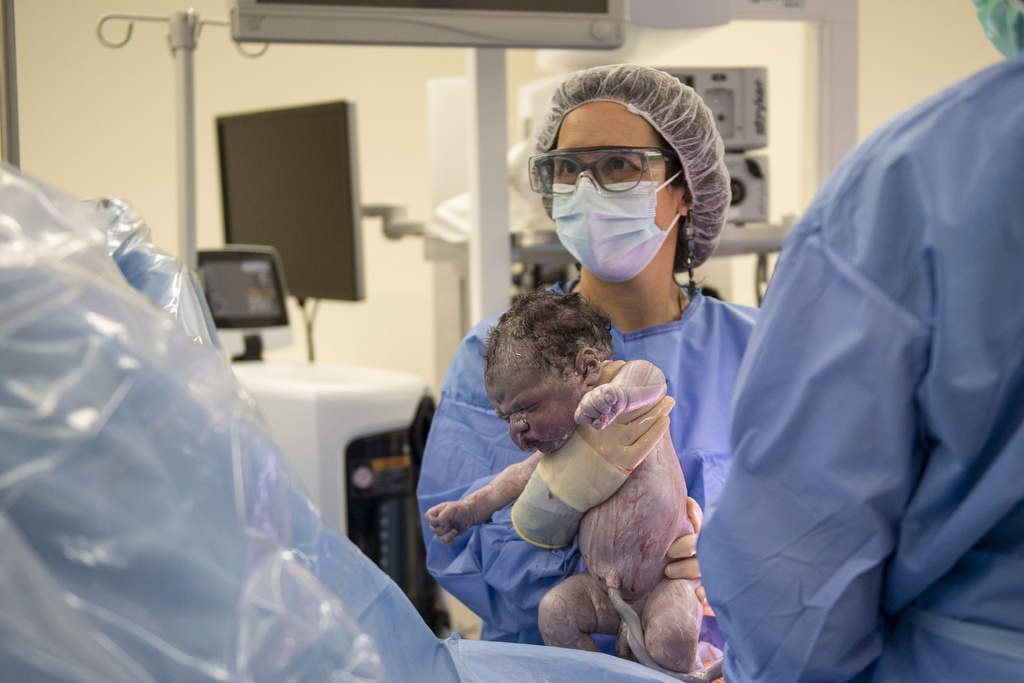
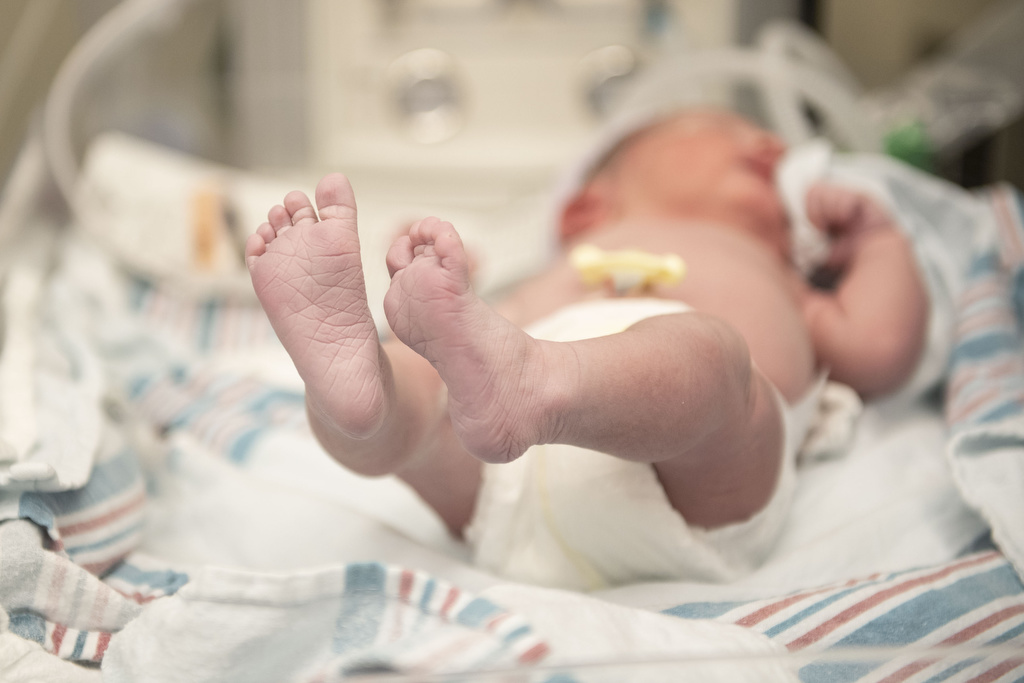
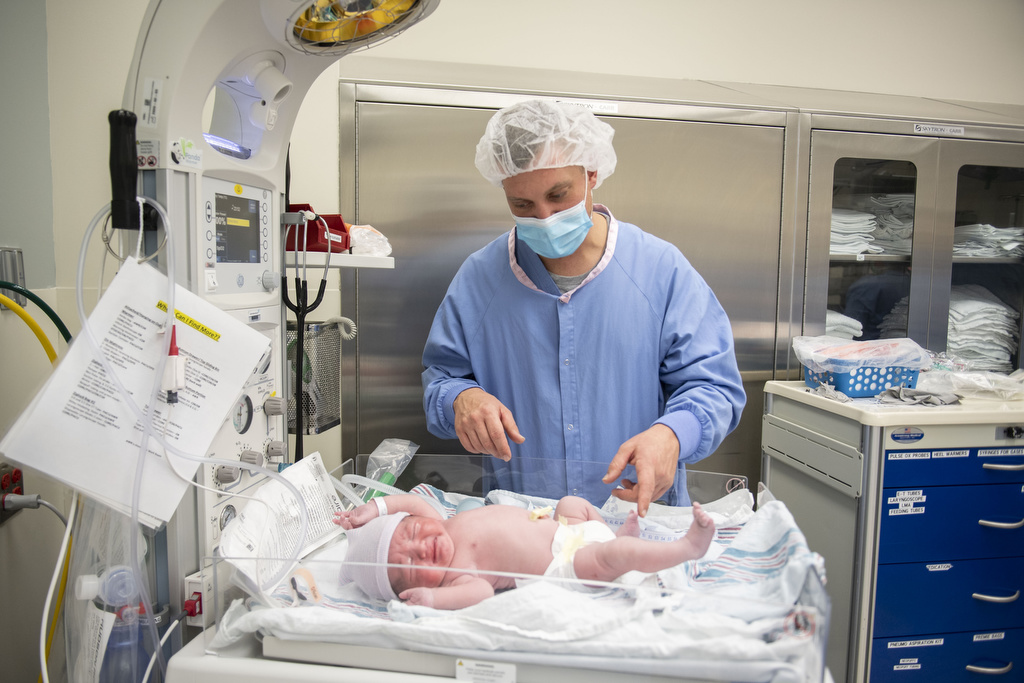
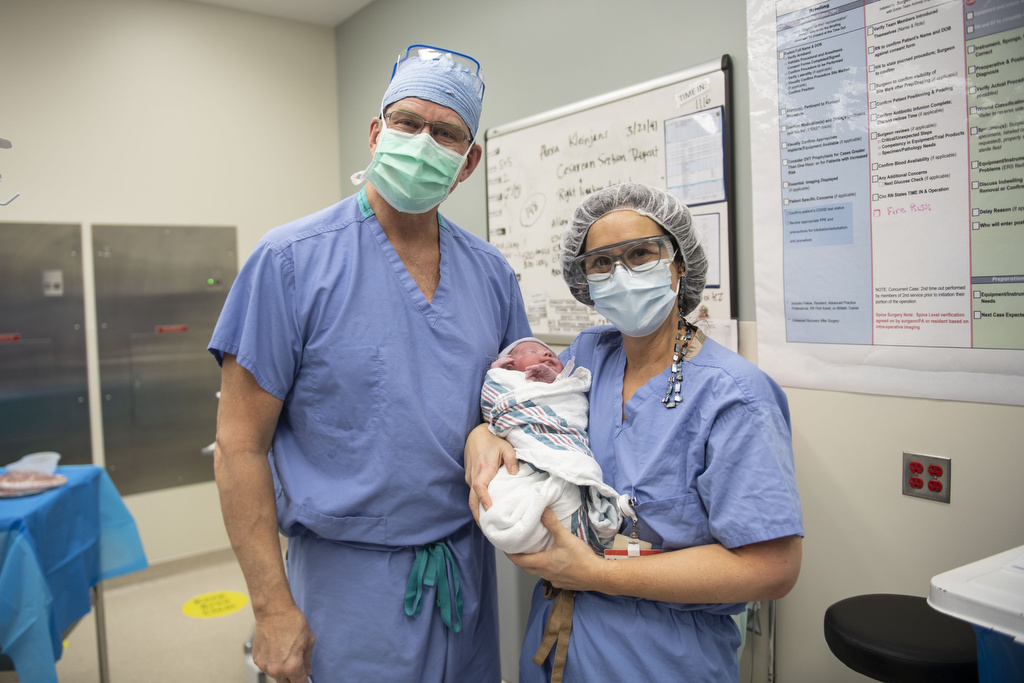
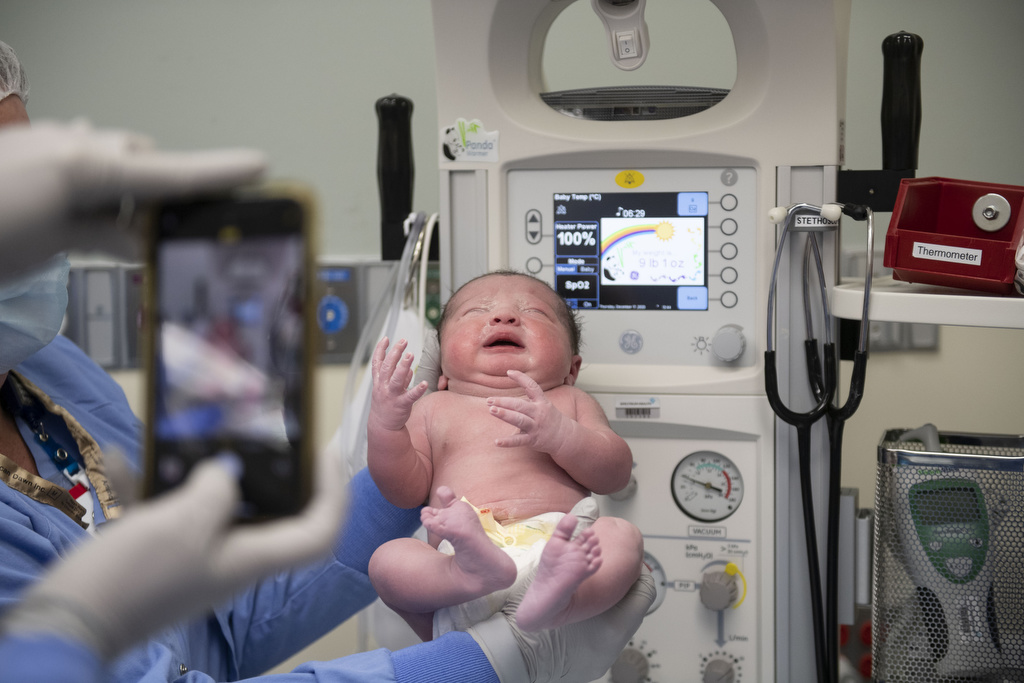
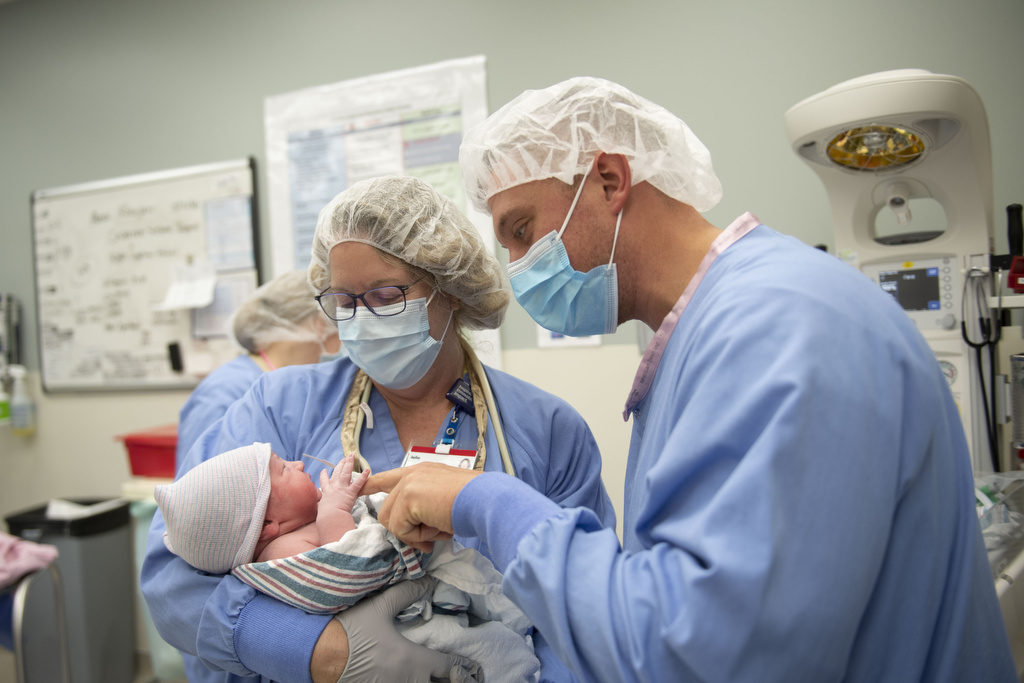
Just past 11 a.m. on Dec. 17, baby Abel Curtis Kleinjans arrived—a beautiful 9-pound bundle, just like his two older siblings.
Once they had delivered the baby and closed up the uterus, Drs. Van Heest and DeWitt got a close-up look at the previous surgery site.
“I couldn’t wait to take a look on that side where the cyst was—and it looked amazing,” Dr. Van Heest said.
“That whole area from which we resected the tube had healed up real nice and just looked fantastic. … It’s always nice to see the end result looking as good as you hoped for.”
From a mom’s perspective, Alexa would say the same thing.
She admits to being nervous before the delivery, but with Abel home and healthy, she feels nothing but gratitude for the Zeeland Community Hospital team.
“Honestly, I would never want to go anywhere else,” she said.
“We’re so thankful. I can’t help but just know that God had this all in control.”
At home with his sister and brother, Abel is alert and easygoing, ready to soak up all the love and attention he can.
“He such a good baby. So chill,” Alexa said. “We are so in love.”





























 /a>
/a>
 /a>
/a>
 /a>
/a>