It’s mostly the stuff of legend, but it’s fascinating nonetheless.
Some folks say Old World cartographers would scribble a haunting phrase onto their maps to mark uncharted territories, places where men had yet to explore.
Hic sunt dracones.
It means, “Here be dragons,” and whether it really ate up any real estate on ancient maps is almost irrelevant, because it’s just a handy admonition for those who dare wander into mysterious, unmapped places.
And anymore, just one place of this sort remains.
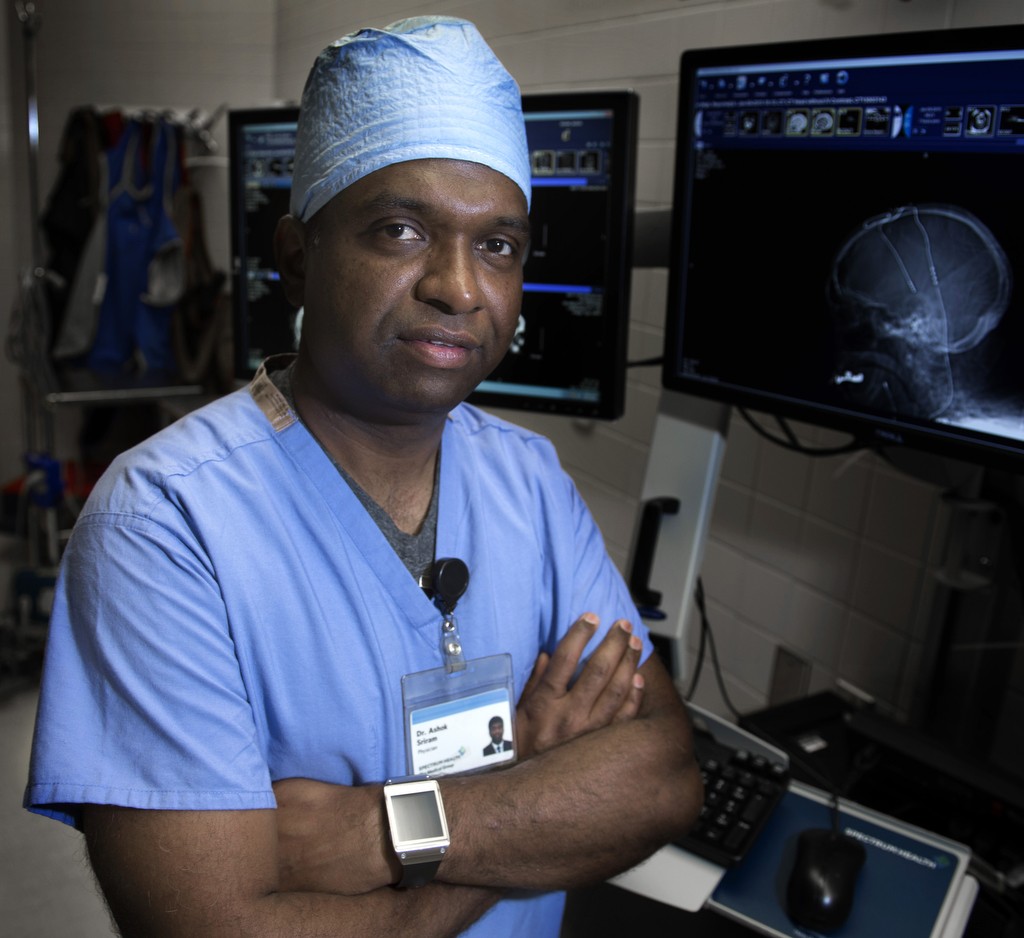
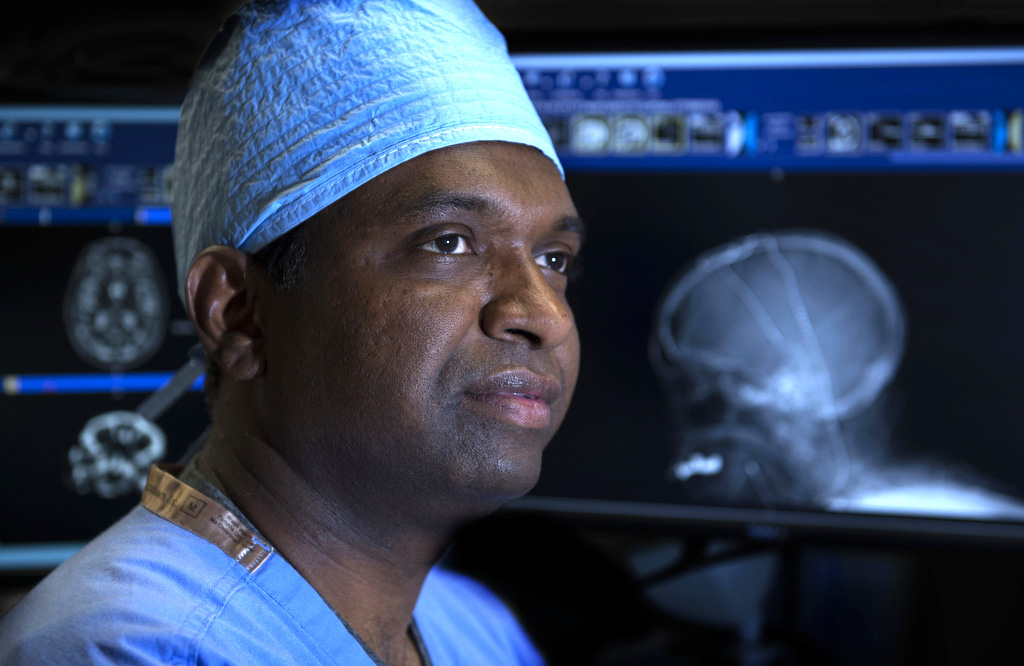
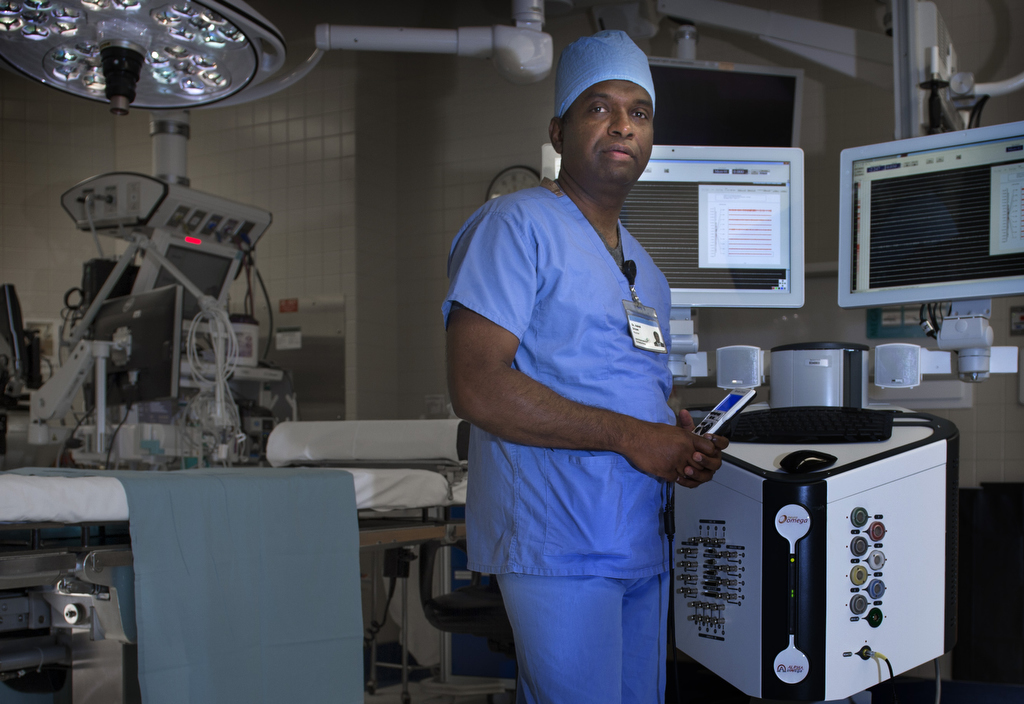
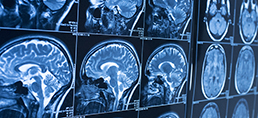
“It’s the ultimate project: mapping the human brain,” said Ashok Sriram, MD, MS, a neurologist with Spectrum Health Medical Group who is fellowship trained in the treatment of movement disorders. “The brain is going to be the last frontier to understand how everything works.”
As he talks about aspects of his craft, Dr. Sriram sounds less like a neurologist and more like a ship captain who would dare venture across waters vaguely familiar, but always full of mystery and mystique.
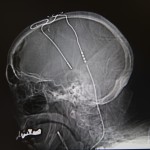
In describing deep brain stimulation, a procedure wherein tiny electrodes are inserted with impossible precision deep inside the brain of a Parkinson’s patient, he says: “We develop a navigational system based on coordinates, just pretty much like a GPS, and we come up with the coordinates based on imaging.”
He adds, “But still, it’s a blind procedure—you can’t be sure you’re where you’re supposed to be.”
As you’d expect with brain surgery, the work is impossibly delicate.
“We move about 30 millimeters using a microelectrode, 0.1 millimeter or 0.2 millimeter at a time, to map out key structures in the brain,” Dr. Sriram said. “All these structures are so close. A millimeter, in these kinds of deep brain stimulation surgeries, makes all the difference.”
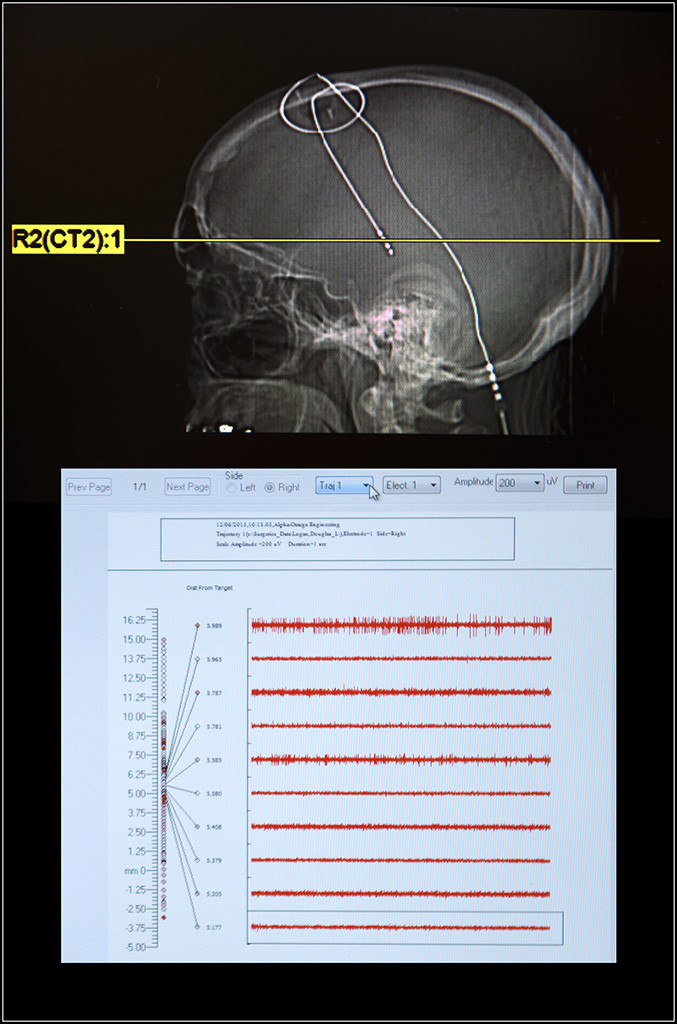
Off by a millimeter in this business, he said, and “you think you’re in Florida (when) you’re actually up in California.”
In Dr. Sriram’s realm, Parkinson’s disease is the creature dwelling in the far-flung regions of the map. It’s the elusive dragon, lurking in the mountainous folds of the brain, a sort of enigma even to modern science as it wreaks slow, steady havoc on mind and body.
But never have the conditions been so good for fighting dragons.
“We know more about Parkinson’s disease now than ever before,” Dr. Sriram said. “You don’t ever want to have Parkinson’s, but if you have to have it, there’s no better time than now, compared to just 20 years ago.”
Growing knowledge
Parkinson’s is a chronic and progressive neurodegenerative disease. There is no cure and the symptoms worsen with time.
So, there’s no slaying this dragon—there’s just holding it at bay with a powerful trident of therapy, medicine and surgery.
The root concepts of these approaches haven’t changed a whole lot over the years—in surgery, for instance, the premise of deep brain stimulation is the same today as it was 20 years ago—but the tools have been finely honed.
It’s the result of better technology and an ever-growing breadth of knowledge, Dr. Sriram said. Even our fundamental understanding of the disease continues to evolve.
Doctors have long known that, in the Parkinson’s brain, cells in a certain region begin to die off, Dr. Sriram said. Fewer cells mean fewer dopamine neurotransmitters, which triggers tremors, slowness and stiffness.
“That’s (always been) our basic understanding,” Dr. Sriram said.
And while neuroscientists have known Parkinson’s motor symptoms—the tremors, stiffness and slowness—are the result of this dopamine deficiency, there is now universal understanding that the onset of the disease, at a molecular level, occurs many years before a person experiences the hallmark signs.
A study published in the journal Neurology this past month found that depression may be the earliest symptom of the disease.
“People with Parkinson’s have anxiety, mood issues and depression even before they’ve had their first motor symptoms, like a tremor,” Dr. Sriram said. “They have constipation, drooling, cognitive impairments and dementia—and many of these symptoms have nothing to do with dopamine neurotransmitters. There’s a lot more involved than just less dopamine in the brain.
“We know that Parkinson’s starts at least 10 to 15 years before you’ve had your first symptoms,” he said. “And by the time a patient has their first symptoms, they’ve already lost approximately 70 percent of the neurons in that part of the brain.”
The belated diagnosis is a factor in the inability thus far to erase the disease.
“I think that’s why we’ve not been successful in finding a cure,” Dr. Sriram said. “By the first time they’re actually diagnosed, it’s a little late.”
A cure would likely come on the heels of scientists finding more reliable ways to obtain an objective diagnosis of the disease—identifying, for instance, specific genetic markers or proteins.
Teaming up on therapy
As neuroscientists and health professionals continue growing their knowledge of Parkinson’s, they steer the direction of treatment.
Top health care institutions now recognize Parkinson’s patients should be engaged in a multidisciplinary approach, given the host of symptoms accompanying the disease.
“We don’t focus just on the tremors,” Dr. Sriram said. “We focus on both the motor and the non-motor aspects of the disease.”
Three years ago, the National Parkinson’s Foundation released findings from its ongoing Parkinson’s Outcomes Project, which showed the disease’s non-motor symptoms have the most significant impact on a person’s quality of life.
“When you combine the non-motor aspects of Parkinson’s—take that mood anxiety and depression and put it all together—all these combined impact the quality of life more than tremor or slowness or stiffness,” Dr. Sriram said. “We’ve started to treat these non-motor symptoms better.”
Spectrum Health’s Movement Disorders Program achieves this through “patient-centered, multidisciplinary care,” Dr. Sriram said.
“Just one person, a neurologist, is not able to help a Parkinson’s patient,” he said. “We use teamwork: a physical therapist; an occupational therapist; speech therapist; a neuropsychologist and psychiatrist to help with cognitive impairments, depression, mania and anxiety; and a neurologist.”
If a patient is treated for tremors but not sleep issues, anxiety, constipation or other non-motor symptoms, “you’re not doing that Parkinson’s patient any justice at all,” Dr. Sriram said.
Surgery and medicine
In surgery and medicine, the fundamental approach to Parkinson’s treatment has been relatively consistent for years.
But with technology exponentially improved, Dr. Sriram said—in the delivery systems for medication and in the precision of equipment used for deep brain stimulation—it’s an entirely different environment for treatment.
“The technology is old, but how we do it, how we target it, we’ve gotten better,” Dr. Sriram said.
The FDA earlier this year approved two such medications—Rytary and the DUOPA Pump. They’re based on existing medication, carbidopa and levodopa.
“We’ve had this medication for decades, but these are new delivery systems,” Dr. Sriram said. “With oral medications, what happens is the medicine goes in the stomach, then the blood, and it swings up quickly. Then as the level comes down, there’s a fluctuation.”
These new systems aim to remedy that. Rytary contains an immediate release of the medicine, but also an extended release component; the DUOPA pump is an infusion pump that delivers a constant dose of the medicine directly into the small intestine, eliminating the fluctuating blood levels of the medicine.
For Parkinson’s patients who need more than medication, however, deep brain stimulation remains the standard of care, Dr. Sriram said.
It is a breathtakingly meticulous procedure.
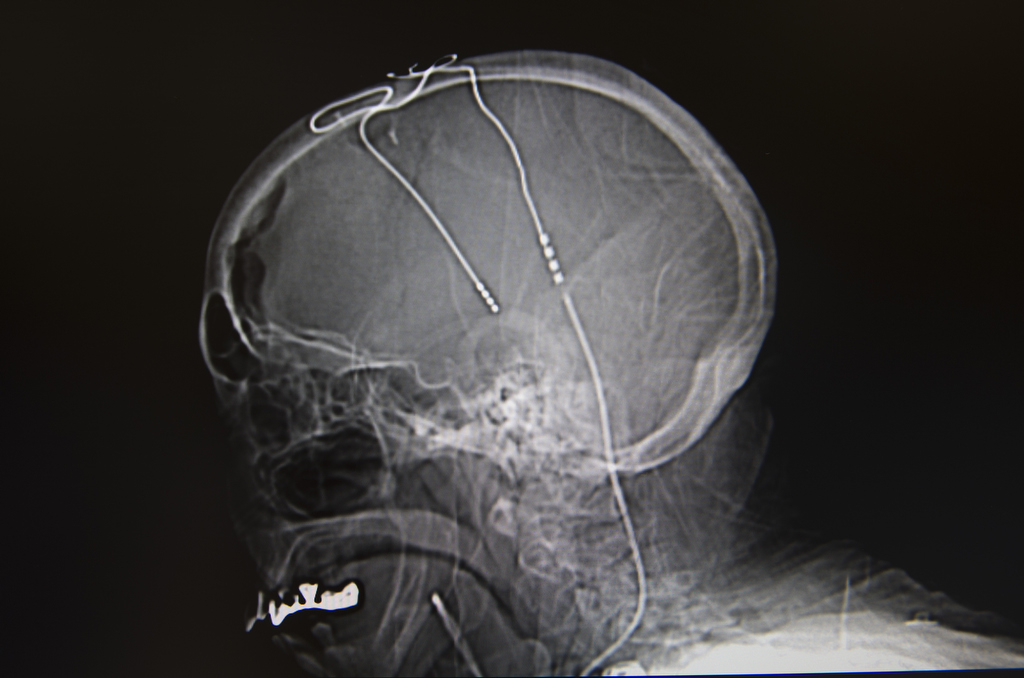
The neurologist is effectively hunting for key brain structures that produce the abnormal patterns inside the Parkinson’s patient’s brain. The procedure introduces microelectrodes that deliver electrical pulses, which regulate the abnormalities.
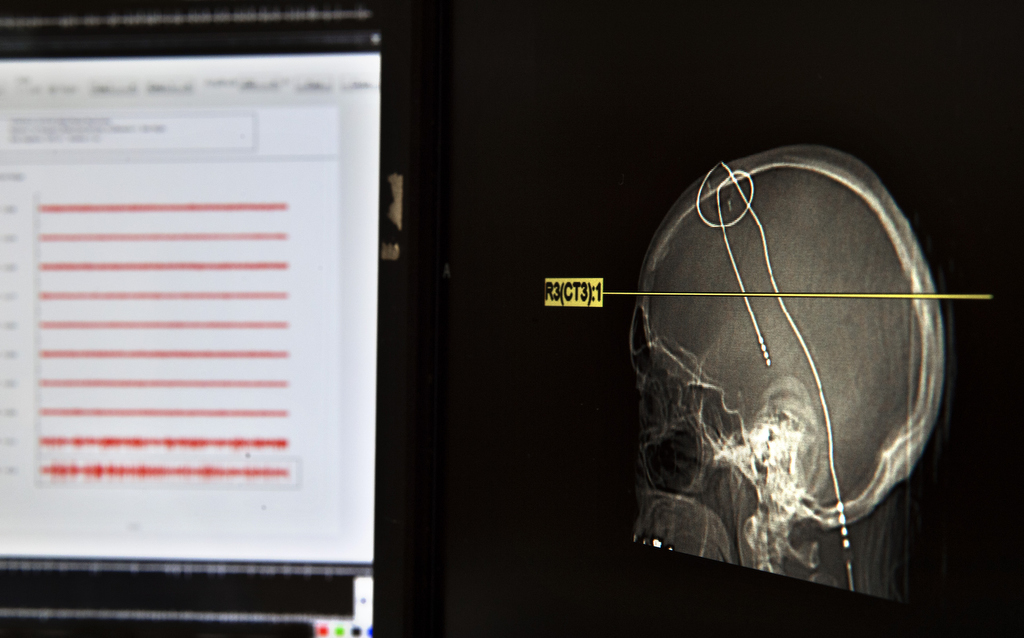
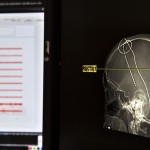
Medical staff obtain an MRI of the patient’s brain beforehand, then in surgery merge this with a frame to create a sort of map of the brain. The patient is lightly sedated but awake, allowing the neurologist to gauge the patient’s speech and movements throughout the procedure, Dr. Sriram said.
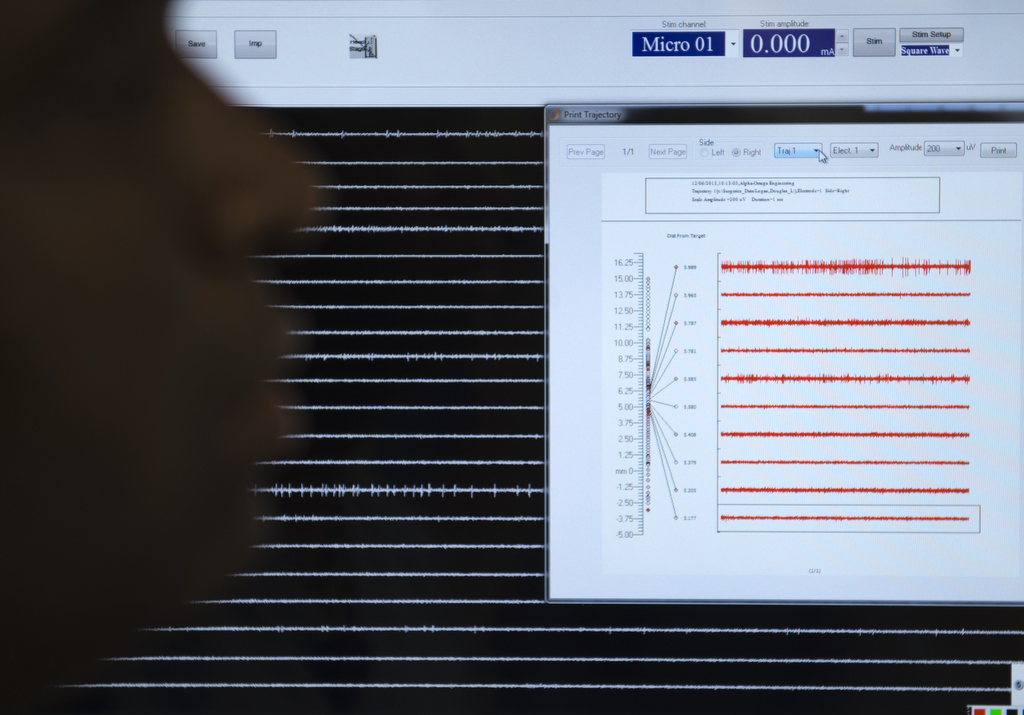
The neurologist inserts the microelectrodes deep into the brain, about 15 centimeters below the surface. He then moves the electrodes about 30 millimeters—0.1 millimeter at a time—as he seeks to identify the offending structures.
“Based on the pattern of activity we see, we know where we are,” Dr. Sriram explained. “The good example we give is it’s like navigating through Europe: We go through different parts of Europe and we pick up where we are based on what language the people speak. If they’re speaking Italian, then we know we’re in Italy.”
This is where technology has improved outcomes. Twenty years ago, when deep brain stimulation was introduced, doctors would use electrodes that could cause side effects.
“Imagine the tip of a wire,” Dr. Sriram said. “The current would go in a circular fashion, and sometimes you’d stimulate a structure you didn’t want to stimulate.”
Manufacturers have produced better tools, giving doctors greater control of the devices and their lasting effects. Instead of delivering an electrical signal that radiates outward, the new electrodes can deliver a laser-focused directional signal.
“We have to be very precise,” Dr. Sriram said, “but we’ve learned how to control this current … specifically to shut off some aspects of the electrode completely, so that we avoid unwanted side effects.
“The electrodes are better, we’re getting a better signal-to-noise ratio, the targeting equipment is better,” he said. “Twenty years ago it was rudimentary. The process now is very refined.”
At some point, the tools and techniques may give way to a vaccine, or perhaps new medicines to slow the progression of the disease in each patient. As it stands now, modern medicine can only alleviate the symptoms of the disease.
“The ultimate question is, can we cure this disease?” Dr. Sriram said. “We’re not there yet.
“We have a lot of treatments available, but nothing to cure Parkinson’s. The research has brought us to where we are—and there’s still a lot of promising research going on.”
One of these days soon, someone in neuroscience may re-draw that brain map.
And in that dark part where Parkinson’s lurked, they’ll write this: “Here were dragons.”

 /a>
/a>
 /a>
/a>
 /a>
/a>
Very informative and well written.
Thank you for this information. My father died from the effects of Parkinson’s and wish there had been a cure to stop his suffering.
You’re welcome, Therese. I wish there was a cure for Parkinson’s. I, also, have a family member suffering from it. I’m glad to see there are advancements being made. Best, Cheryl
Parkinson’s disease is such a mystery in its complexity and understanding how it behaves in different individuals. Still hoping for a cure.
I have had M G for 20 years. Now recently diagnosed with CORTICALBASIL SYNDROME. Helpful article: relationship?