Over the summer, Brenda Tuttle was having trouble catching her breath. Any time she’d exert herself a bit, she’d feel winded. Puzzled, the active 50-year-old started looking for answers.
Her systematic month-long search took her to the gym, three doctors’ offices and an urgent care center before she got to the bottom of it in late July—in the ER.
The quest
The symptoms came on gradually, so she wasn’t alarmed in the beginning.
“First I thought it was just me being out of shape,” said Tuttle, of Grandville, Michigan.
She was already doing weight training with a personal trainer, so she tried upping her cardio workouts. Then she turned to yoga, thinking, “I can’t breathe right—I’ve got to learn how to breathe or something.”
When that didn’t help, Tuttle wondered whether stress or anxiety was the culprit. Though she knew her clinical depression was well managed, she paid a visit to her psychiatrist. The doctor prescribed a new medication, but also advised her to see her primary care physician as her blood pressure was unusually high.
Not having a primary care doctor, she called her OB-GYN’s office and explained her situation. The doctor, who had prescribed birth control pills three months earlier to help regulate Tuttle’s cycle, advised her to do two things: stop taking the hormone pills and visit an urgent care center if her symptoms didn’t improve over the weekend.
Over the next two days, things got worse.
When to watch for a pulmonary embolism
- After a major surgery or a broken leg or hip
- During or after a long flight or car ride
- After starting a new hormone treatment
Signs of a pulmonary embolism
- Leg swelling
- Chest pain
- Shortness of breath
“Any time I’d walk any kind of distance, I’d be like, ‘I have to sit down and catch my breath,’” she said. By now, her husband noticed it too.
That Monday, Tuttle visited her local urgent care facility, where she had a chest X-ray and an EKG. Other than an elevated heart rate, her vital signs and oxygen levels were normal, so she went home to await the results.
As she soon learned, the X-ray revealed a shadow on her lung. The urgent care staff found her a primary care doctor, Carlos Merritt, MD, and got her an appointment for the following day.
That night she couldn’t sleep. Her skin felt hot and clammy. Washing her face, she looked in the mirror and thought her lips looked blue. She sat on the bathroom floor and tried to catch her breath.
In retrospect, Tuttle said, this is when she should have awakened her husband and headed to the ER.
“There were enough things that were concerning me, I should have just gone and gotten the answer sooner,” she said. But it was easy to find other explanations.
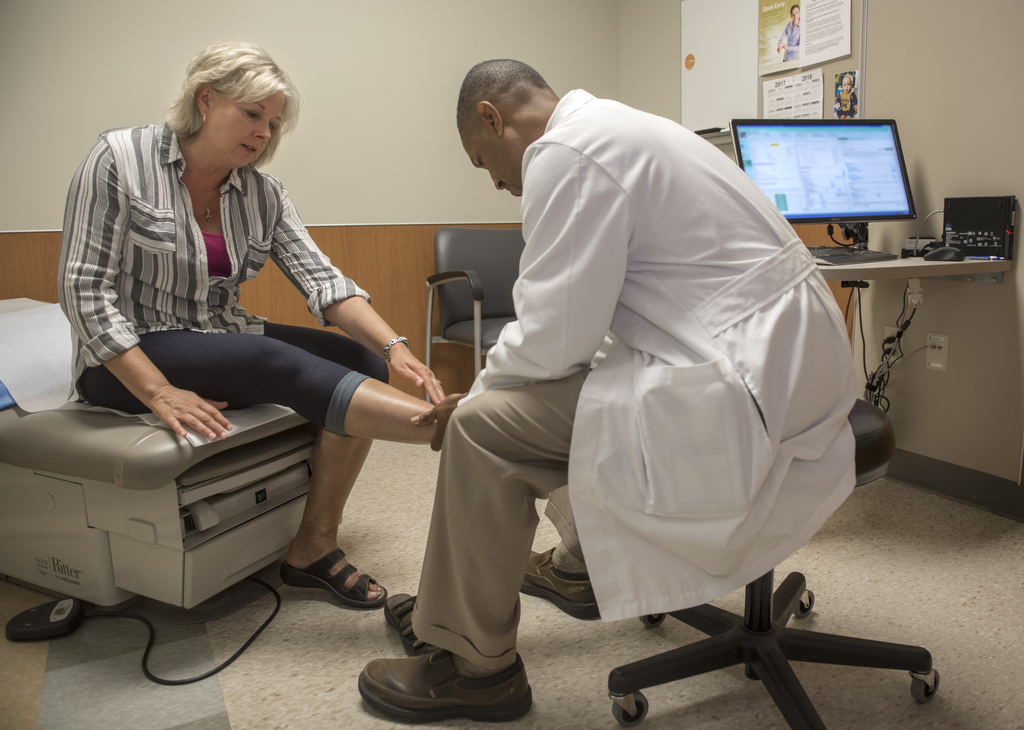
Things came to a head at Dr. Merritt’s office the next day, when both her lips and her feet looked purple. It was clearly time for a CT scan. No more waiting.
Mystery solved
The doctor’s staff called ahead to Spectrum Health Butterworth Hospital’s emergency department, where Tuttle’s husband dropped her off at the entrance.
“I walked myself into all of these places, not realizing what was going on,” she said.
The answer to the mystery was soon revealed: She had a large bilateral pulmonary embolism.
“And we were like, ‘What even is that?’” she said.
As the Tuttles would soon learn, a pulmonary embolism is a blood clot that’s blocking an artery of the lungs. It typically happens when a clot in the leg, a deep vein thrombosis, breaks loose and travels through the bloodstream to the lungs.
It’s a serious condition that can damage the heart, lungs and other organs, and sometimes results in sudden death.
In Tuttle’s case, multiple clots had lodged themselves in both her left and right pulmonary arteries, according to Megan Sanchez, MD, a hospitalist at Butterworth Hospital and the Spectrum Health Fred and Lena Meijer Heart Center. Over time, this put a strain on the right side of her heart.
“It’s sort of like if you had a hose and you put your thumb over it—it would start going really, really hard and fast because most of it’s blocked,” Dr. Sanchez said.
“So the right heart is pumping really hard to try to overcome that blockage in the pulmonary artery. If it can’t overcome that, it fails.”
Though the blockage was indeed hurting Tuttle’s heart, she didn’t need oxygen, as pulmonary embolism patients often do. That was likely because she had such healthy lungs from exercising and not smoking, Dr. Sanchez said.
The question was how to treat her. The ER doctors had put her on an IV drip of heparin, a blood thinner, to stop the clots from growing and to prevent new clots from forming.
Now the medical team could either wait for her body to naturally dissolve the clots or intervene to break up the clots and restore normal blood flow.
Dr. Sanchez asked her colleagues from interventional radiology to make a recommendation. Because of the burden on Tuttle’s heart, Manish Varma, MD, an interventional radiology specialist, advised using thrombolytic therapy to dissolve the clots. Despite the risk of internal bleeding from the blood-thinning drugs, Tuttle agreed to the treatment.
By then, she felt much worse.
“I was so short of breath. My heart would race and I just felt like I was going to die,” she said. “It was very scary.”
Her husband, three daughters and two grandsons occupied her thoughts. She knew they weren’t ready to lose her.
The interventional radiology procedure required Dr. Varma to insert a catheter into a vein in Tuttle’s upper leg and steer it to the pulmonary artery using live X-ray images. Once the catheter was in place, he began delivering clot-busting medication directly to the clots. The medication dripped in overnight, as Tuttle lay in the ICU.
By the next day, Tuttle felt the difference.
“I could tell that it was so much better—I could finally breathe. So it pretty quickly did what it was supposed to do,” she said. And she had no side effects from the procedure.
Three days after arriving at the ER, Tuttle went home. When she went for a follow-up echocardiogram a week later, her heart was pumping normally and the right-sided pressure had decreased.
“So essentially, no real harm done, which is good—really good,” Dr. Sanchez said. “She came in early enough.”
Looking back, the oral contraceptives were the likely cause of Tuttle’s blood clots, Dr. Sanchez said: “That was probably her biggest provoking factor.”
Dr. Sanchez discharged Tuttle with a prescription anticoagulant, Xarelto. After taking that pill for a few months, she should be back to normal, the doctor said.
A second chance
Now that the scare is behind her, Tuttle is rebuilding her strength and coming to terms with the gravity of her experience—especially knowing that her father-in-law died of a blood clot.
“I try not to be dramatic, but it was serious, and I think that’s made me just try to make the most of my second chance,” she said. “I don’t understand why this happened, but I do know that God saved me for a purpose.”
She sees telling her story as one way of giving back. “If I can help somebody else, then I’m willing to share,” she said.
Tuttle and Dr. Sanchez both agree that persistence played a big role in her positive outcome.
“She took enough initiative to keep kind of ‘pressing the bell’ when she wasn’t getting better,” Dr. Sanchez said. “Because she kept pushing, she got the answers she needed.”
Tuttle’s message for others: Don’t doubt yourself if you’re not feeling well.
“If there’s something going on with your breathing and you’re not sure, go get it checked out.”

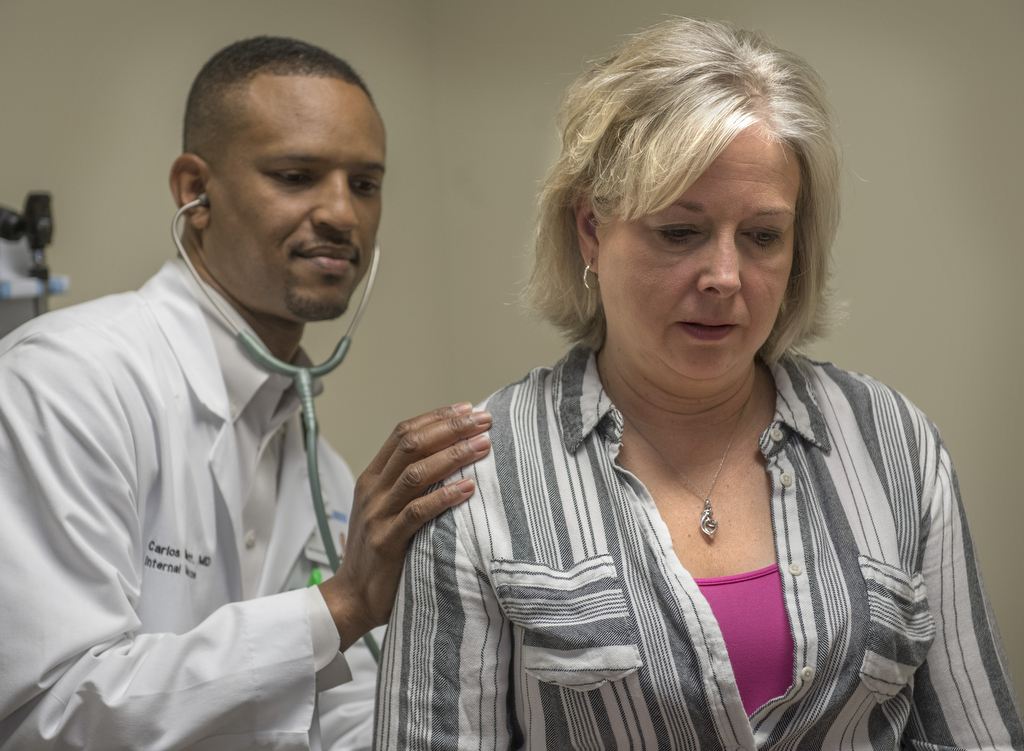














 /a>
/a>
 /a>
/a>
 /a>
/a>
Praise God & Great Drs🙏🤗💕💕💕Thanking God for our Daughter!!!
What a miracle! Praise God from whom all blessings flow!🙏🏻💙☺️
God is good! So thankful he was holding and Carring for one of his precious daughters! Love you sis!!
Brenda ….so glad for a happy ending ….you are really Blessed to have a fresh start after the scare your whole family has experienced . Great job going after an answer your perseverance is why your here today! Gods the man with the plan❤️
Keep sharing your story. You are blessed to be a blessing! God is good all the. time and His Grace is custom made. Counting all the blessings big and small