Hear that sound?
It’s silence. The silence of sound sleep.
Linda Cole, 65, a retired school physical therapist assistant from Zeeland, Michigan, had struggled with sleep issues for years.
Until recently, her sleep hadn’t been sound for a long time. Nor silent.
“That I had sleep apnea was actually an accidental find,” Cole said. “I had a bad case of flu, made worse by asthma, and I was having a bronchoscopy done when my doctor noted that I appear to have sleep apnea. During a sleep study, I was having as many as 31 events per hour during sleep.”
By events, Cole was referring to long moments during her sleep when she would stop breathing, only to recover with a gasp, sometimes coughing and spluttering for air.
No wonder she often felt drowsy during the day.
“I was officially diagnosed with sleep apnea in 2018,” she said. “My doctor also found that my oxygenation level—how much oxygen there was in my blood—was too low.”
Sleep apnea is a sleep disorder in which breathing is constantly interrupted. These pauses can last a few seconds to minutes.
If oxygen flow doesn’t reach the heart and brain regularly during sleep—which can happen with sleep apnea—it can potentially lead to serious health issues such as stroke, high blood pressure, Type 2 diabetes, heart problems and other conditions.
Symptoms of sleep apnea can include snoring and gasping during sleep, morning headaches, dry mouth upon waking, irritability, difficulty concentrating during the day and daytime fatigue.
Troubled sleep
On her doctor’s recommendation, Cole tried continuous positive airway pressure, or CPAP.
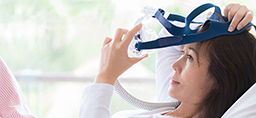
It’s a machine that comes with a mask worn during the night. The mask is placed over the nose or nose and mouth, depending on how you breathe. A hose connects to a machine that uses mild air pressure to keep the airways open.
The mild air pressure keeps the airways from collapsing during sleep, so you can sleep without interruption.
“I tried different kinds of CPAP masks,” Cole said. “The first one had these tubes, like plugs, that fit into my nose. And it was too painful.
“The second kind was a mask that sat under my nose and left my mouth free—but that, too, was uncomfortable. It gave me a dry throat and filled up my stomach with air, so I would wake up feeling bloated and have acid reflux.”
Cole tried the CPAP for a year, but largely gave up on it, even when her doctor told her that her oxygenation rates had improved.
“I hated the CPAP, so my doctor told me about another option,” Cole said.
That option: a device called Inspire.
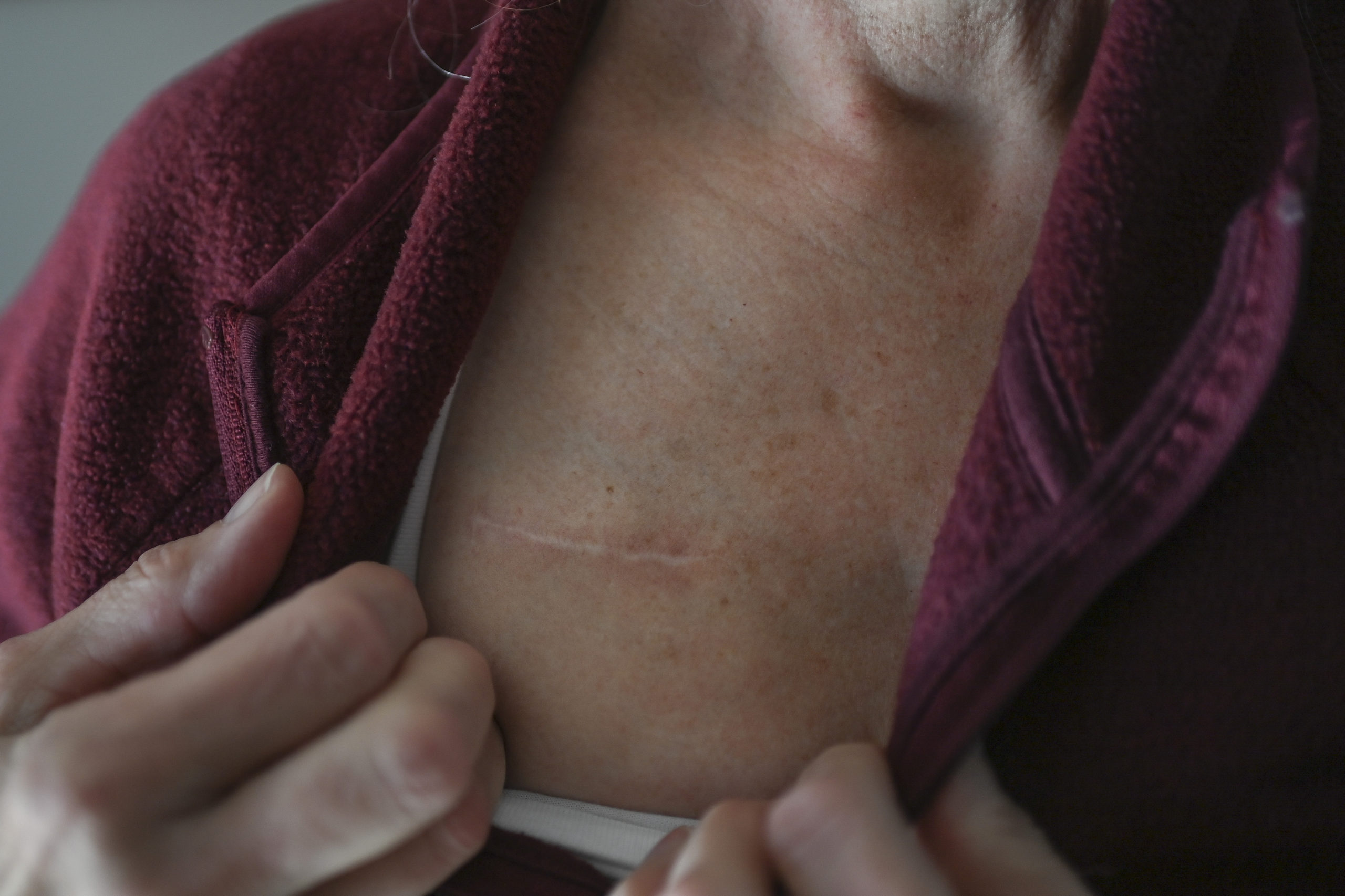
It’s a small surgical implant placed under the skin of the chest.
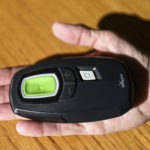
It’s operated by a handheld remote, communicating wirelessly with the implant. When the device is turned on, it stimulates the nerve controlling the tongue muscles to move and open the airway. It keeps the airway open and helps the sleeper inhale evenly.
“I was tested for Inspire during fall 2019,” Cole said. “Doctors put a tiny camera down my throat to see how the tissues in my throat opened and closed, front to back. I was thrilled to learn that I was a good candidate for Inspire.”
Sweet dreams
Doctors scheduled the procedure for June 1, 2020, at Corewell Health Butterworth Hospital.
Kelly Waters, MD, a physician in sleep medicine and neurology, is the program lead for Inspire implantations at Corewell Health.
The main types of sleep apnea are obstructive sleep apnea, central sleep apnea and complex sleep apnea syndrome, Dr. Waters said.
“Inspire can treat obstructive sleep apnea,” Dr. Waters said. “It is the most common type of apnea, when throat muscles relax during sleep.
“When the throat muscles relax, they narrow or close the airway as you breathe in. The brain senses this and wakes you just long enough to get muscle tone back and open the airway to breathe again. This is probably so short a moment that you don’t remember it when awake.”
Central sleep apnea, less common, happens when the respiratory drive of breathing is ineffective and can still wake the brain. Both can result in fluctuating oxygen levels.
Central sleep apnea is primarily treated with specialized BiPAP machines to support that missing respiratory effort. Complex sleep apnea syndrome is a combination of both obstructive and central sleep apnea.
“Inspire won’t help these,” Dr. Waters said. “But Linda had obstructive sleep apnea, so Inspire worked well for her.”
While CPAP is considered the first line of treatment for obstructive sleep apnea, Dr. Waters agreed it didn’t work well for Cole.
Cole’s care team implanted the Inspire device and two lead wires to her chest and under the jaw.
“It’s an outpatient procedure that takes between two and three hours,” Dr. Waters said. “And the device has a battery similar to a pacemaker. We have implanted close to 100 of these devices here, so our experts can sometimes do the procedure in as little as an hour.”
Before the device is activated, the patient must wait five to six weeks for recovery.
The team activated Cole’s device in July 2020. She was the first to receive the Inspire device at Corewell Health.
“It took a few adjustments in the doctor’s office to find that sweet spot of voltage to move my tongue forward to open my airway, but not too much,” Cole said. “And then, that first night, I slept a full six hours. I hadn’t done that in years. It was the best sleep I could remember.”
Cole can now sleep six to eight hours per night, without interruption.
“I have more energy, my brain feels less foggy, and I am less irritable,” she said.
Her husband, Mark Cole, is happy, too.
“I have my beautiful wife back,” he said.
The new device is quiet and effective.
“With Inspire, there’s just a little beep and she sleeps all night,” he said. “The snoring has almost entirely stopped. This miraculous device has made both our lives better.”
Dr. Waters nodded in agreement.
“Most of the referrals we get for Inspire come from spouses,” she said, smiling.





 /a>
/a>
 /a>
/a>
 /a>
/a>
Linda is my good friend. She was after me for almost a year to get Inspire because I had a hate relationship with my cpap machine. I couldnt stand wearing it.
I was afraid that my body would reject the Inspire implant. I finally agreed because I wasn’t using my cpap at all. Let me tell you, it was the best decision I ever made!!
When they asked how long I want my Inspire set for( sleeping hours) I told them “If I could get 6 hrs sleep, I would be thrilled!”About 2-3 wks later I called and told them I needed it set for 8.
I looked forward to going to sleep, instead of dreading it. I love my Inspire!!!!