By late 2012, Jacqueline Morlan’s quality of life had plummeted.
After three surgeries, mobility in her left wrist had all but vanished. She had given up cherished hobbies like golf and bowling. She was in “bring-me-to-tears pain” on a daily basis.
“I was eating anywhere from 10 to 12 ibuprofen day,” Morlan, 47, said. “I just kept living with it, honestly. … I was kind of frightened to have surgery because the last one had been so utterly painful and didn’t help.”
Unsurprisingly, the ibuprofen didn’t work. She ended up in the hospital with multiple ulcers. Her wrist and forearm pain only worsened.
She looked online and found the orthopedic hand and upper extremity surgical team at Spectrum Health Medical Group.
The surgeons there gave her two options to deal with the arthritis and instability in her wrist.
The first used cadaver tendons to replace her failing tendons, but there’d be no guarantee those would last beyond a couple years.
The second option involved an incredibly rare surgery: total distal radioulnar joint replacement. Only 3,000 replacements have ever been done worldwide—and only one other in Western Michigan, which this team performed earlier in 2017.
“I just felt like, at that point, I didn’t have anything else to lose,” Morlan said of choosing the joint replacement. “I wasn’t going to be any worse. The only thing I could do was get better. So I chose the second option.”
In June, Levi Hinkelman, MD, a hand, upper extremity and microvascular surgeon, performed the joint replacement.
Six months later, Morlan is pain-free for the first time in nearly a decade. She has almost full mobility in her wrist. She’s doing daily in-home therapy to rebuild strength after years of atrophy from not using those muscles.
And she’s excited to play golf in the spring for the first time in five years.
“I have these new clubs and bag that have just been sitting in my closet for years,” Morlan said. “I’m looking forward to breaking them out.”
‘Crunching potato chips’
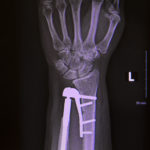
So what is total distal radioulnar joint replacement?
The radioulnar joint is a joint between the two bones of the forearm: the radius and ulna.
“Those are the bones that normally let you rotate your forearm,” Dr. Hinkelman said. “But when you get arthritis or instability in those bones, you can lose the ability to rotate and it can be very painful. … Up until recently, we didn’t have any good solutions.”
One common remedy, Dr. Hinkelman said, was to fuse the two bones together into one bone, eliminating the painful bone-on-bone contact. But that left patients with the inability to rotate their forearms and turn their palms upward.
“It cured the pain, but that procedure was really very debilitating for people, because it was a profound loss of function,” Dr. Hinkelman said.
Other options included soft-tissue stabilization procedures, taking out the head of ulnar bone, replacing the ulnar bone and using cadaver joints, among other treatments.
Morlan tried a few of those. Her problems, she had been told, stemmed from having too long of an ulnar bone, which “ground down” her radioulnar joint.
In 2010 she underwent ulnar bone replacement surgery at a hospital in central Michigan. She expected immediate relief after the surgery, but instead the pain worsened.
She next went to a university hospital in Michigan, followed by an Ohio hospital. She still experienced numbness from nerve decompression.
And strangely, her wrist began to make noises—“like crunching potato chips,” she said.
Doctors at the Ohio hospital told Morlan her implant was catching on the tendon and “tearing it up,” causing that sound and her pain. They performed two surgeries: a nerve decompression first, and later they added tissue under her tendon to raise it up and help avoid contact with the implant.
The crunching sound went away, but the pain persisted. Fearing more surgeries, she turned to ibuprofen and “tried to suck it up.”
‘A game-changer’
Dr. Hinkelman described total distal radioulnar joint replacement as a “last gasp … and end-of-the-line procedure.”

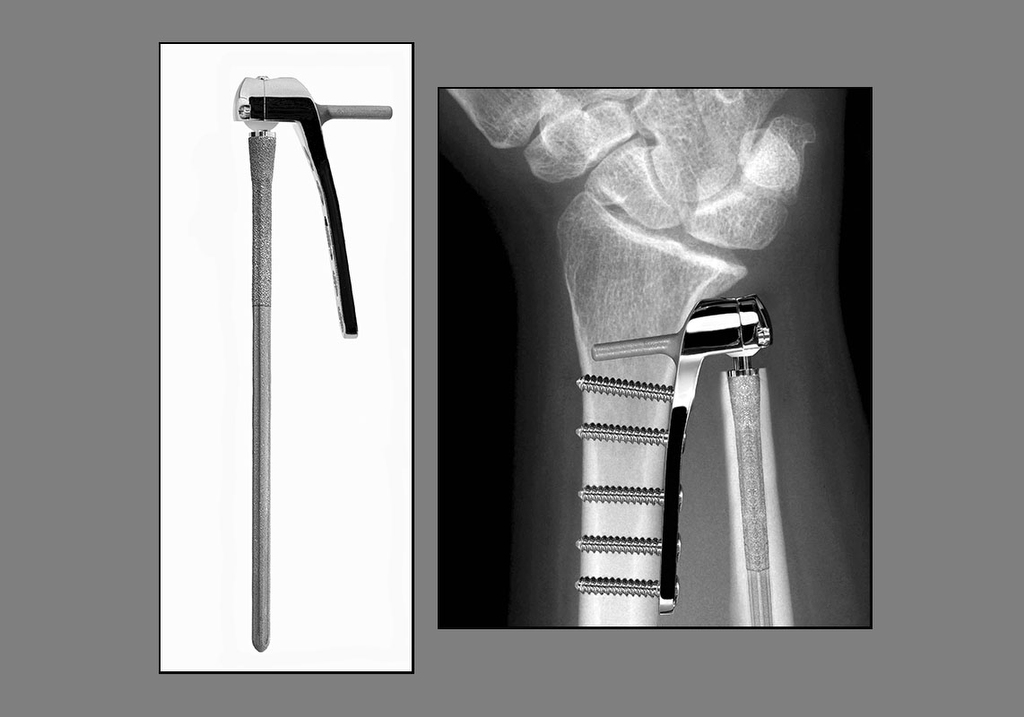
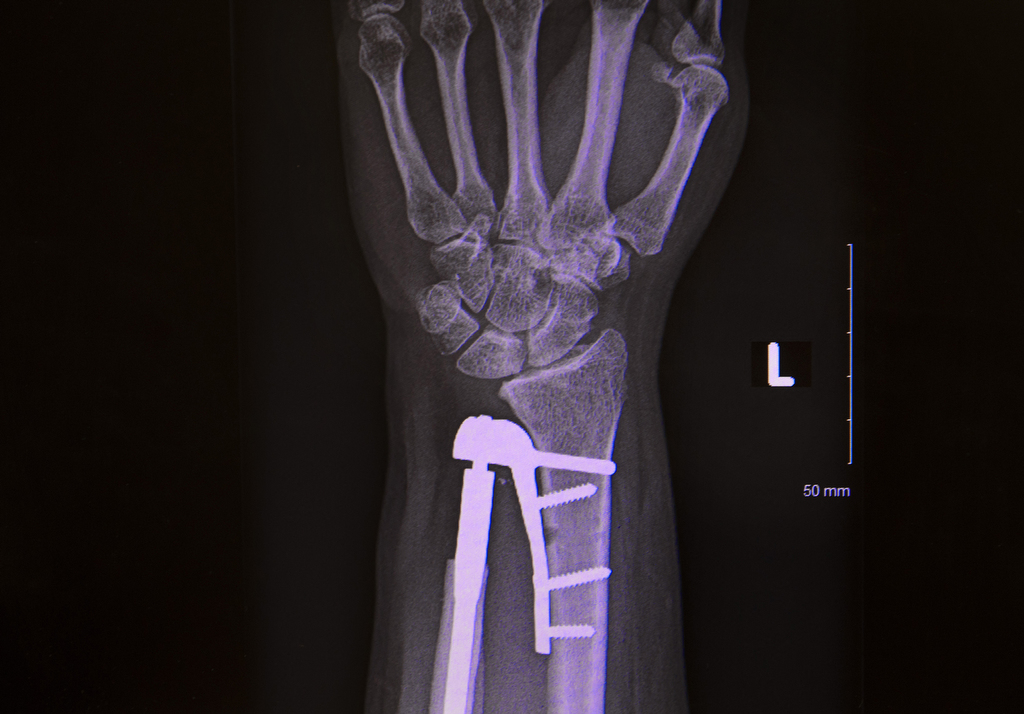
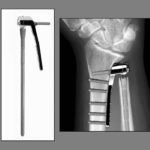
The implant, called an Aptis implant, is a metal-plastic interface that provides flexibility and the cushioning between bones that a healthy human joint provides.
“It restores functionality while also eliminating pain,” Dr. Hinkelman said. “It’s kind of a game-changer for people with those two problems.”
Because few patients have ever received the implant—it’s only been widely available for about a decade—doctors don’t know the long-term effects.
“We don’t have a lot of data,” Dr. Hinkelman said. “Will this implant fail over time? If so, how long will it last? We don’t have a lot of answers. With more time and data, hopefully it could be a lifelong fix. But we just don’t have data like, for example, hip replacements, which have been around 40 years.”
That lack of data, the procedure’s invasive nature and the fact that it’s the best option for a difficult-to-fix injury means doctors prefer to try other options first, which is why it’s been so infrequently used, Dr. Hinkelman said.
“I think that whenever you’re doing a surgery that you know that this is the good solution for that problem and not another good solution after that one, that’s where the nervousness comes from,” he said. “It comes from our desire to have it go perfectly, that the patient won’t have any complications and problems afterward, because there’s no good fix if it doesn’t go well.”
For her part, Morlan has been ecstatic with the results.
Post-surgery, she could feel the top of her left hand for the first time in years. She could bend her wrist back and forth and rotate her forearm, all abilities she’d lost over time.
“They gave me back things in my life that I hadn’t had in a long time,” she said.
Morlan is the prototypical candidate for this type of procedure, Dr. Hinkelman said. He has another patient who is a candidate for the procedure, possibly as early as this winter. And if patients like Morlan continue to see the benefits of the implant over time, he expects he will do the surgery much more often.
“It’s been very successful for her so far,” Dr. Hinkelman said of Morlan. “She is the classic example of a patient who had multiple surgeries that didn’t work, with persistent pain in her forearm that never went away, but she’s noticed a dramatic improvement since having the procedure done.
“I do think that, in the future, if the implant demonstrates good longevity, it will become more commonplace early on,” he said. “It will become more of a primary procedure instead of a salvage procedure.”



 /a>
/a>
 /a>
/a>
 /a>
/a>
Is there any option like this for an elbow that has no cartilage left? My husband has this and it is painful I think much of the time.
Hi Gail, So sorry to hear your husband is in so much pain. Please do reach out to an orthopedic specialist to get a consultation for your husband. You can schedule an appointment with Spectrum Health Medical Group Orthopedics by calling 616.267.8860. They should be able to share what options your husband might have that would improve his quality of life. Best wishes to you both!
I myself had 2 surgeries so far and still have constant pain and limited use of left hand. Weight limit was set ar 3lbs. Finally a doctor suggested having this surgery (5/03/2019) . So started surfing the web. Glad came across this testimony, feel a lot better about going through with the procedure. Know not all outcomes are the same but I’m hopeful. Was a active person before worked all the time. If this implant can restore at least part of that with little to none pain I will be so happy.
Regina, I’m so glad you found this article and that it makes you feel more comfortable and hopeful. To learn more about hand and upper extremity surgery that could help with your situation, I’d recommend scheduling an appointment with Spectrum Health Medical Group Orthopedics by calling 616.267.8860. Best wishes to you! Cheers, Cheryl
How did it go? How long was recovery? How is the mobility post surgery and now months later?
My Doctor talked to me today about this procedure. I have had two surgeries within the last 8 months, including a ulna shortening. The pain is almost worse now and my range of motion has decreased. What is the recovery tiime?
Hi. Could you eventually bowl again after a total wrist replacement?