
It was past midnight on a Tuesday, the second week of December.
Amid the hypnotic whir of medical machines and early morning chatter in Spectrum Health Helen DeVos Children’s Hospital, new mom Amanda Miles got to thinking about how things had turned out in the past few months.
Her son, Jackson, was just shy of 2 months old.
Amanda, 27, and her husband Jeff, 27, saw their 6-pound 13-ounce baby boy as nothing short of a miracle, even if they knew straight away the little guy’s introduction to life was destined for struggle.
Before he was born, doctors had detected a defect in Jackson’s tiny heart.
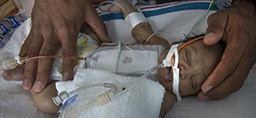
When Oct. 15 came, staffers were ready and waiting in the delivery room at Spectrum Health Butterworth Hospital. They were joined by employees from the children’s hospital Neonatal Intensive Care Unit (NICU), along with a small army of specialists.
“They were prepared,” Amanda said. “He would go from the delivery room to the NICU. We knew he would have to have surgery five days later.”
He arrived with a congenital heart defect, but there was more.
He had a cleft palate, lung disease and a horseshoe kidney, a disorder in which his kidneys fused to create a single “horseshoe” shape. He spent the first five days in the third-floor NICU before staff moved him to the pediatric intensive care unit (PICU) on the eighth floor, to meet his pre- and post-surgery needs.
Day 5 of Jackson’s life began with open-heart surgery from the Helen DeVos Children’s Hospital Congenital Heart Center team, which is led by cardiothoracic surgeon, Marcus Haw, MS, FRCS, and interventional cardiologist Joseph Vettukattil, MD. Surgeons repaired the total anomalous pulmonary venous return and the coarctation of the aorta, and they used a pulmonary artery band to reduce pulmonary blood flow.

Jackson was then taken back to surgery the following day, Amanda said, with surgeons tightening the pulmonary artery band. Shortly thereafter he underwent a cardiac catheterization, followed by another surgery.
His challenges persisted.
“They tried closing his chest,” Amanda said. “He didn’t tolerate it. They had to open him back up, then close him back up about a day and a half later.”
There was dialysis, too, and later doctors took steps to help him breathe on his own. That lasted about 14 hours before they had to re-intubate him. Finally, they had to perform a tracheotomy so he could grow and develop and come off sedation.
“He’ll still need more surgery,” Amanda said.
‘Thank you for loving me’
Past midnight on that Tuesday in December, about eight weeks after Jackson was born, Amanda was understandably weighted in thought. To lighten the load, she sat down at a computer in the children’s hospital and began to type.
The seventh-grade language arts teacher didn’t have trouble finding the words. She recounted the events of recent weeks—the gestures of kindness, the encouraging words, the trials and troubles—and she thought about all the people who were instrumental in Jackson’s survival.
She wrote messages from Jackson and his new parents to the doctors, nurses and caregivers who made a difference. She even thanked the snack cart workers who delivered smiles with her favorite fare, Rice Krispies treats and Pepsi:
• Thank you for loving me and making sure I am clean. Also, thank you for caring about my mom and making sure my parents hold me!
• Thank you for taking such good care of me and giving me cute blankets!
• You took care of me during the first few weeks and prayed with us. Thank you!
•We are thankful for your skilled hands that have helped our son so far. Most of all, you have amazed us in the way you show compassion for our son, Jackson, and us. We truly feel blessed to know you. Best Wishes always, The Miles Family.
• Thank you for your smiles, greetings, and nourishment throughout the day. It is nice to see friendly faces each day when you’re in a place you hope no one ever needs. However, we are blessed to be here because Jackson needs it. You make every day a little bit brighter.
By the time she was done, Amanda had written more than a dozen messages.
At 3 a.m., she pushed the send button.
‘A unique group’
Health care professionals in pediatrics, particularly those in intensive and emergency care units, are a special breed. On the one hand, the world demands of them a soft countenance so the children in their care feel safe and the parents feel reassured. On the other hand, they have to be constantly on the mark, almost machine-like in their accuracy and speed, and ever cognizant of the seriousness of their work.
The job demands 50 parts compassion, 50 parts competence.
“They’re really a unique group of people,” said Wendy Winger, BSN, CNML, manager of pediatric critical care unit at Helen DeVos Children’s Hospital. “They have to be smart, very intelligent, able to catch on to many things.”
“Pediatric intensive care unit nursing is one of the most unique areas of nursing,” Winger said. “We deal with patients who are a day old, up to 18 years old. You have this whole broad range, and typically the kids are critically ill.”
Winger offers a salient point about treating seriously ill children: The parents are, quite literally, entrusting you with everything they hold dear in life. The standard for care could not be any greater.
“Likely, this is the parent’s most precious being,” Winger said.
It is no small feat, then, to hear grateful words from the mother of an infant who has endured multiple heart surgeries and weeks of procedures.
Amy Neumann, RN, a nurse and a mainstay for the Miles family during Jackson’s time in the PICU, remembers the family’s messages. They came via the children’s hospital website, through the Care Pages system.
“While Amanda’s child was still here and still sick, she thanks us all,” Neumann said. “She’s an amazing person.”
Jackson, Neumann said, required a great deal of care.
“Have we seen a child exactly like him? Absolutely not,” she said. “Will we again someday? Maybe. But he was unique for sure.”
His mother was memorable, too.
“She is the most patient, loving, accepting person that I’ve met,” Neumann said. “We have a lot of great families here. With Amanda, it just seems like trial after trial, she took it all in stride.”
‘They were family’
There’s a curious chemistry afoot when patients and their families end up in the hospital for an extended stay. All those faces that were once unfamiliar when they arrived—the doctors, the nurses, the attendants—become familiar, until one day they become friends, and by the time they leave, they become family.
“We had so many nurses we liked,” Amanda said. “They weren’t really our family, I know that, but they became family because they were there when people gave us the worst news of our lives. You can’t explain those moments—they create a bond unlike anything else.”
It’s natural for patients and families to build close relationships with caregivers, Winger said, although she adds this: Helen DeVos Children’s Hospital has a knack for finding workers who meet great expectations.
“They are very much a relationship-type of person,” Winger said of PICU nurses.
They have strong personalities, too.
“They’re able to speak up for themselves and their patients to get what they need,” Winger said.
The PICU at Helen DeVos Children’s Hospital has a capacity for 24 children on the main floor, with additional room for 12 on another floor. The typical stay for a child of any age is about three to five days, although it can be three months or more depending on the severity of a child’s illness.
Jackson was in the PICU for three and a half months, during which time Amanda and her husband stayed at the Renucci Hospitality House, a minute’s walk from their son. They were with him constantly.
The only break in their bedside vigilance came in the fifth week, when Amanda was treated for a pulmonary embolism she had developed. She was laid up for five days, her husband doing double-time from one medical unit to another.
“My husband, poor guy, was running between the heart center and the children’s hospital,” she said. “He amazed everyone with his strength.”
Complicating matters further, they learned Jackson had three serious and, quite possibly, fatal lung diseases.
It wasn’t the first time the couple had been struck with devastating news about their son. The day after Jackson was born, medical staff had suspected the infant’s host of problems was a sign of Trisomy 13, a chromosomal condition that causes birth defects and severely limits a child’s lifespan.
“It was the worst weekend of our lives,” Amanda said, recalling the grueling wait for test results that first weekend. “I didn’t know what was going to happen.”
She and her husband decided to send Jackson into surgery, uncertain if any underlying issues might affect the outcome.
“It was just this continuous series of decisions,” Amanda said.
They ultimately learned Jackson does not have Trisomy 13, and the cause of his many ailments remains unknown. They also later learned his lung diseases, while serious, are not necessarily fatal.
Through all this, Amanda said, the nurses were constant companions.
“They experienced all of it with us,” she said. “I don’t think I can explain that moment when someone tells you the first things about your child, all that’s going on. You can’t get someone to feel that, what it’s like. But the nurses experienced that with us. Their caring touch just made it that much better.”
When the Miles family departed Helen DeVos Children’s Hospital on Jan. 27, they left behind them a state-of-the-art facility. But they took with them to their West Olive, Michigan, home something more valuable: connections and trust to last a lifetime.
Spectrum Health’s Visiting Nurse Association will assist the Miles family for at least a year, while caseworkers assist with medical equipment and other needs.
“It’s working out well,” Amanda said. “They visit once a week. The lady who comes out is wonderful, we talk about her kids and Jackson; it’s the beginning of a great relationship.”
She added: “One of the nurses called me from Helen DeVos and checked to make sure everything is going well.”
As Jackson continues his journey, the months and years ahead may occasionally see the Miles family reunited with Helen DeVos Children’s Hospital staff. Amanda is confident her son will prevail, given his strong spirit and the wealth of resources at Spectrum Health Medical Group.
“He’s a little fighter,” she said.
 /a>
/a>
 /a>
/a>
 /a>
/a>
Amanda not sure if you remember me, Herbie and Charlene are our daughters. We have kept your little one and you and your husband in our daily prayers. So glad Jackson made it home, will continue to keep you all in our thoughts and prayers. God Bless.
I do remember… The whole family! Thank you for the prayers. We have been so blessed so far with all the support. His carepage is http://www.carepages.com/carepages/UpdateonBabyJackson. I hope everything is going well for you all!