Dale and Kathy Knoper stopped trying to converse during car rides a few years ago because it became impossible for Dale to hear his wife over the noise of the road.
He stopped watching TV news, too, because he’d catch only half of what the anchors said.
Even with high-end hearing aids, he didn’t hear well.
Social isolation
As his hearing gradually declined, Dale found himself staying home more often after work and on weekends.
When he had appointments, he’d ask Kathy to come along to help interpret. Going to church proved a challenge, too, because he couldn’t understand a lot of the words spoken, even if he connected to a loop system.
“I became quite isolated,” said Dale, of Allendale, Michigan. “It was easier to stay home than to go out in society by myself.”
It wasn’t just personal frustration that kept him home. He didn’t want to be an annoyance to others.
“Whoever you’re dealing with, you know they’re going to get frustrated with you, too,” he said. “I said that over and over and over: I don’t hear well.”
Last year, at age 60, Dale asked his primary care doctor if anything else could be done for his hearing loss. The doctor referred him to Gregory Artz, MD, a specialist in otology and neurotology with Grand Rapids Ear, Nose and Throat. Dr. Artz is credentialed to operate at Spectrum Health hospitals.
After conducting some hearing tests, Dr. Artz discovered Dale fit the narrow criteria for a new technology, the hybrid cochlear implant.
Spectrum Health’s first hybrid
The hybrid implant is a niche product for adults who have extremely poor hearing in the high frequencies, yet retain some of their natural hearing in the low frequencies.
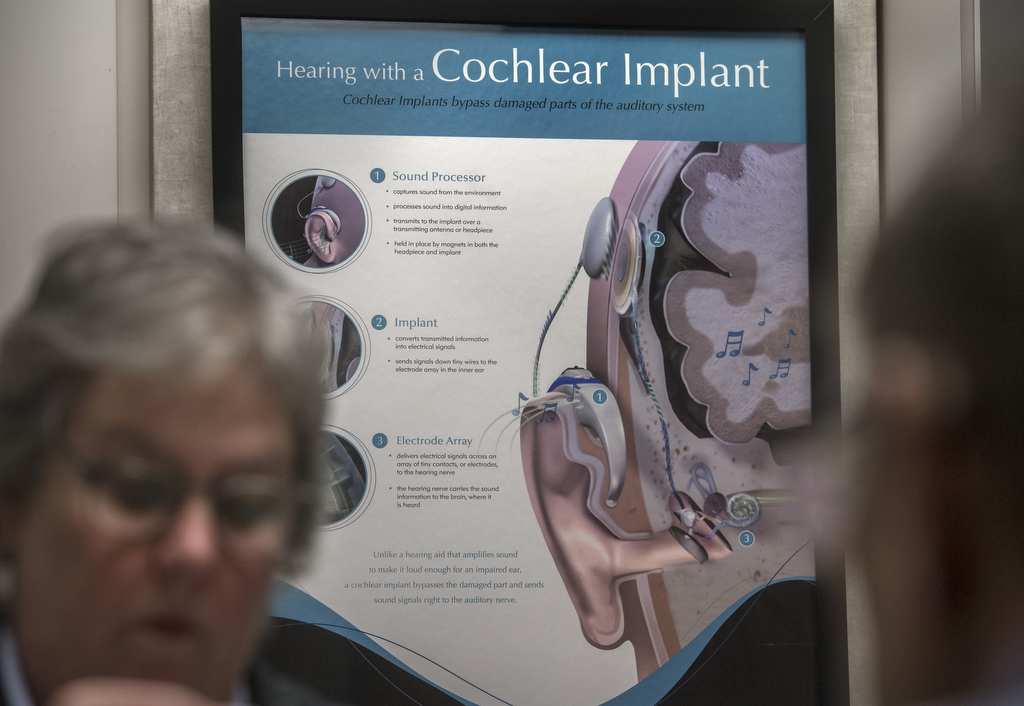
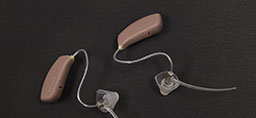
The system uses a combination of electrical and acoustic technologies—an electrical implant to stimulate the high frequencies in the inner ear and an acoustic hearing aid to amplify the low frequencies through the ear canal.
“Basically, with the hybrid, it gives them the best of both worlds,” Dr. Artz said. “They maintain their natural low-frequency (hearing) and the implant aids them in their high frequency.”
The hybrid technology is applied to the patient’s worst ear. In Dale’s case, his right ear. He can continue to use his traditional hearing aid in his left ear.
Dr. Artz has performed hundreds of traditional cochlear implant surgeries, but Dale would be his—and Spectrum Health’s—first hybrid cochlear implant patient.
The FDA approval is new enough and the candidacy criteria are restrictive enough that Dale became the first good fit that Dr. Artz and his colleague Robert Daniels, MD, encountered for this technology.
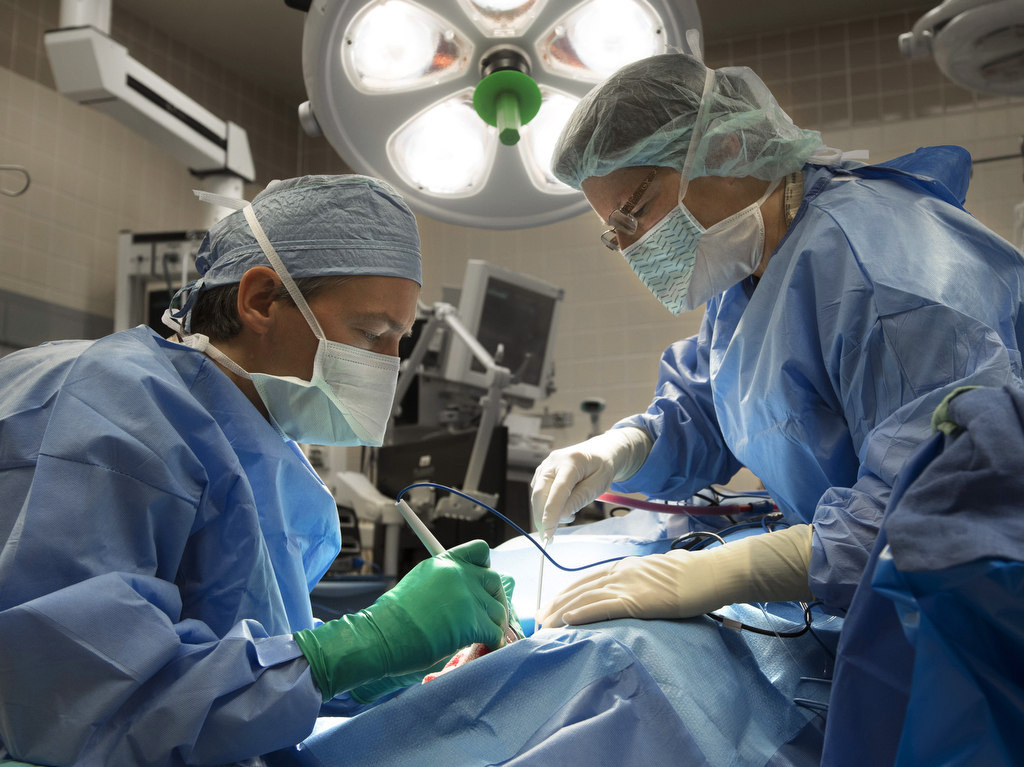
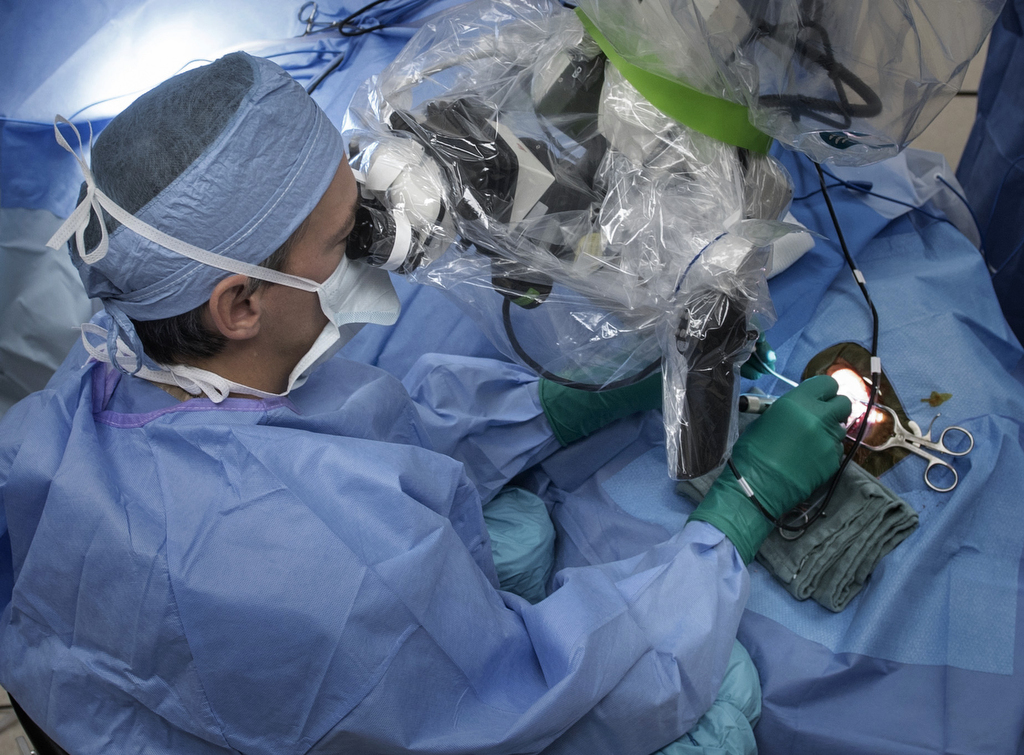
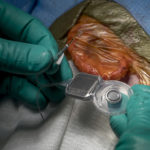
Though the product is new, the implantation surgery for the hybrid device is essentially the same as for a traditional cochlear implant, Dr. Artz said.
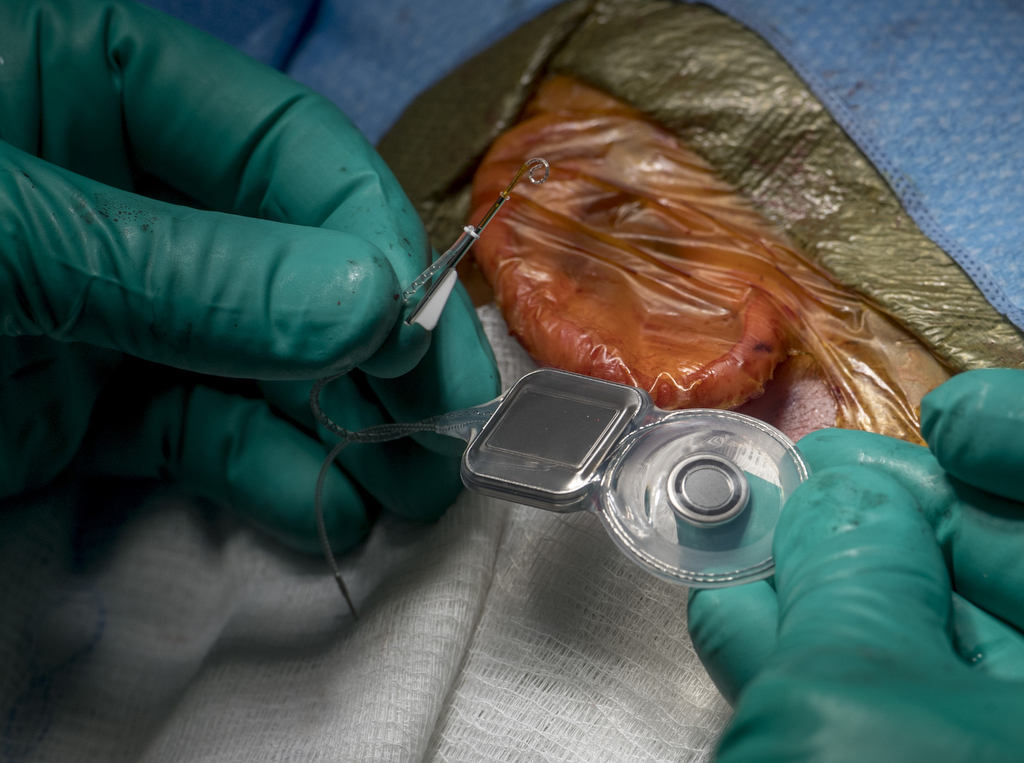
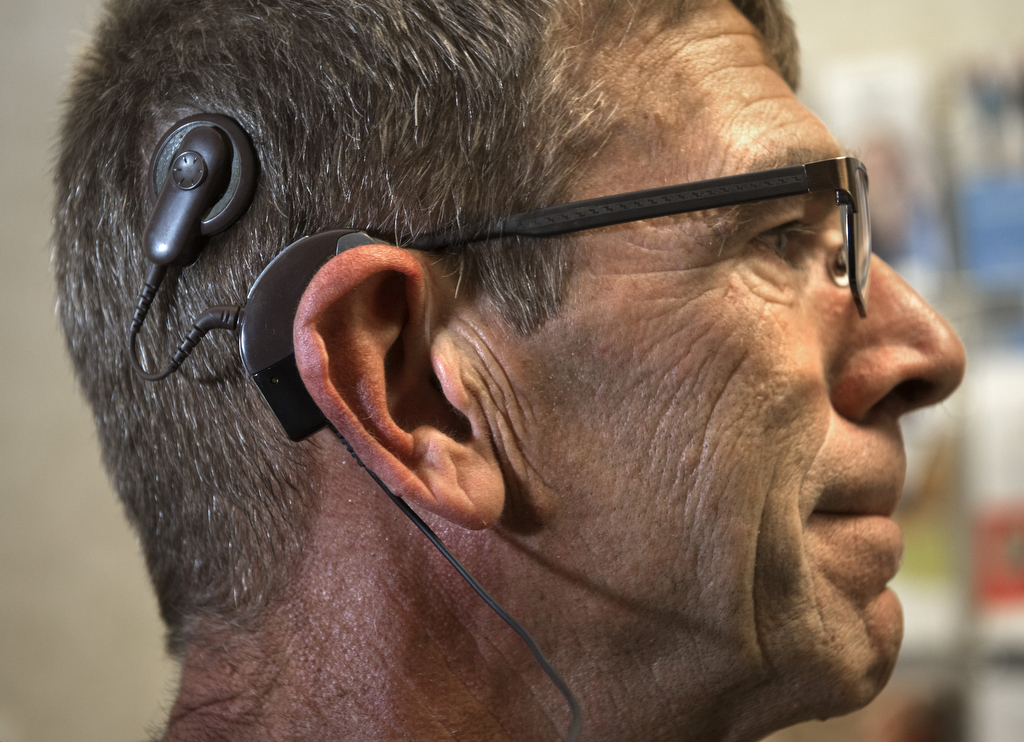
In both procedures, the surgeon inserts a thin, disc-like receiver under the skin behind the patient’s ear and feeds an attached electrode into the spiral-shaped inner ear, or cochlea. An external processor snaps into place against the implant with magnets and the two parts form a programmable system.
The main difference in the hybrid implant is that its electrode is shorter. It doesn’t have to be inserted as far into the cochlea to do its job.
For Dale, the decision to have the surgery came easy. First, his employer’s insurance would cover it (whereas Medicare does not). Second, even though there was a risk that inserting the electrode would damage his residual low-frequency hearing, communication had become so difficult for him that he figured it would be worth the risk.
‘Myself again’
Dale had the surgery in March 2017 at Spectrum Health Butterworth Hospital. After a month of healing, he paid his first post-op visit to the Spectrum Health Audiology department to have his implant activated.
Lisa Miller, MA, an audiologist on the Cochlear Implant Team, worked with Dale to customize the settings on his processor. She then sent him into the sound booth to retake some of the hearing tests he’d taken before the implantation.
The moment of truth had come.
The results? Precisely what the team had hoped for.
“His audiogram is essentially normal all the way across, through the high frequencies,” Miller said.
Dale now periodically returns to the audiology department to have his processor’s programming tweaked and his hearing retested. One test, for example, checks his ability to recognize individual spoken words using his right ear only. Before implantation, he scored a 34 percent with his hearing aid on. At three months after his implant was activated, his score on the same test had doubled to 68 percent. At six months, he hit 86 percent.
The team expects these numbers to continue improving.
“After the patient gets their activation, it sometimes can take several months before they really start to maximize benefit, because their brain has to get used to a different input,” said Kirsten Kramer, AuD, an audiologist with the Spectrum Health Cochlear Implant Team.
Dale is amazed at the difference the technology has made for him, both personally and on the job at Godwin Plumbing. For one thing, he’s no longer afraid to take phone calls, because he uses an accessory that sends the audio directly from his cell phone to his implant.
He also loves being able to interact with his five young grandchildren, who definitely notice the difference in him.
“You’re way more social,” Kathy said. “You’re way more apt to go talk to somebody, whereas before you would avoid those situations because you didn’t want to look stupid, you know, by not hearing what they’re saying correctly.”
Dale agreed completely.
“I’m kind of myself again,” he said.
Patients like Dale are exactly why Dr. Artz does what he does. “They still have a lot of energy and vigor and life to live, and they just can’t hear,” he said.
“So this is an amazing option.”




















 /a>
/a>
 /a>
/a>
 /a>
/a>
Calling our ins. Company. This would be a godsend. Thank you