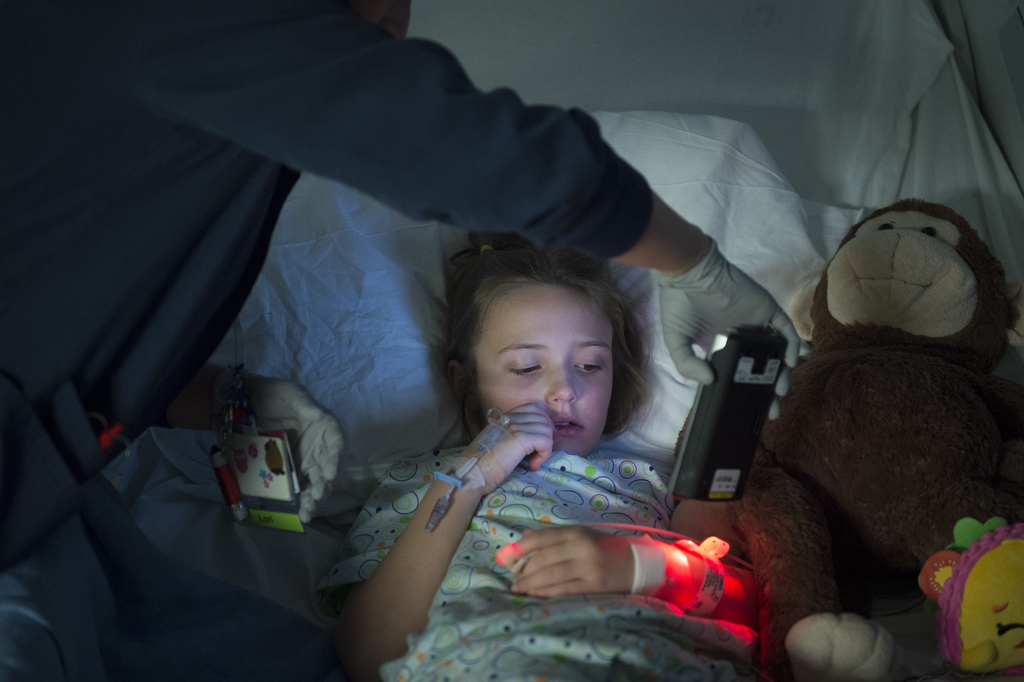
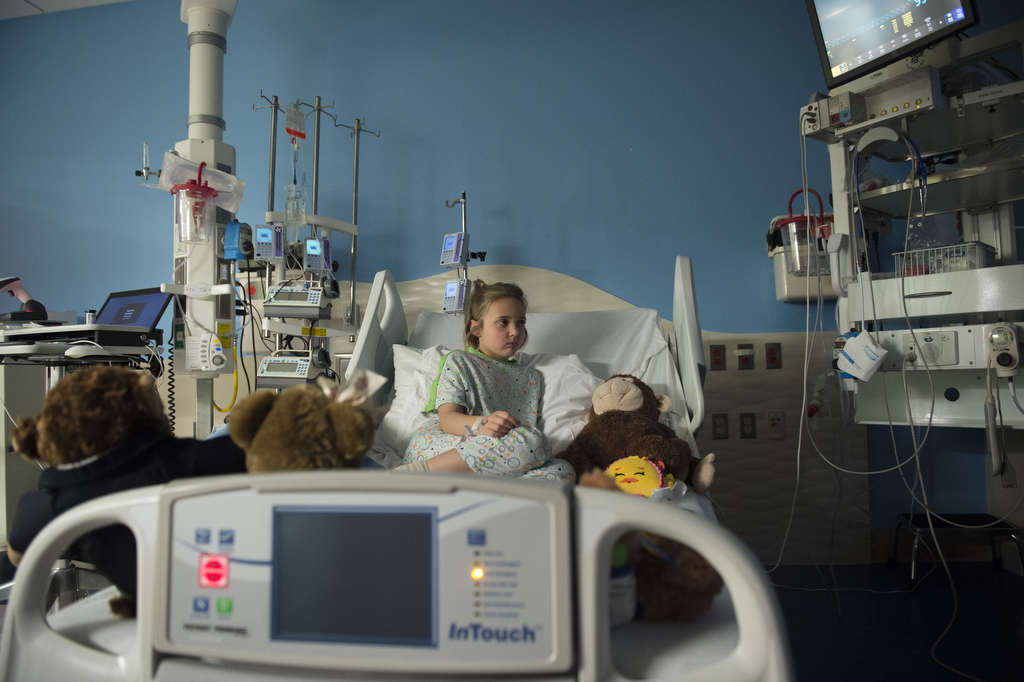
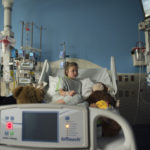
On a recent Wednesday afternoon, Emma Scott reclined in a hospital bed in room 803 of Spectrum Health Helen DeVos Children’s Hospital, watching the movie “Tomorrowland.”
Her dad, Jason, sat at the foot of the bed, watching with her.
On this day, the family was more concerned with reality than science fiction; more concerned with today, than tomorrow.
But the tomorrows will definitely be different for Emma, 7. She’s been diagnosed with Type 1 diabetes.
Yaw Appiagyei-Dankah, MD, a Helen DeVos Children’s Hospital pediatric endocrinologist, said about 1 in 450 children nationwide is diagnosed with Type 1 diabetes, which is no longer referred to as “juvenile diabetes.”
In this often genetic auto-immune disease, the pancreas stops making insulin, the hormone that pushes sugar from blood into the cells to produce energy.
About 200,000 children under 20 years old have diabetes, with 18,000 new cases diagnosed each year.
Common symptoms include excessive thirst and urination, weight loss, lethargy and wetting the bed at night.
“When symptoms are not detected early, the child can go into diabetic ketoacidosis with nausea, vomiting, abdominal pains, heavy breathing, fruity odor or breath and confusion or coma,” Dr. Appiagyei-Dankah said.
Just like that, life changed
Emma’s symptoms came masked, as if late for a Halloween gig. Slow-burning at first. An innocent cough. A general sense of not feeling well.
“She had been coughing like everyone else at school was,” said Emma’s mom, Liz.
Liz took her to a walk-in clinic near their Shelby, Michigan, home. Diagnosed with a sinus infection, they picked up meds for treating it.
Next, Emma started vomiting and breathing became difficult.
Liz said they took her to the emergency room in Shelby. Not long after, Emma was in an ambulance speeding toward Helen DeVos Children’s Hospital in Grand Rapids.
“It was intense,” Liz said. “She was more stable because she had IV fluid and an insulin drip in. They think with her being sick that she had a virus that brought on the onset of diabetes.”
And just like that, life changed.
“She’s understanding that she’s going to have to poke her finger a couple of times a day and she’s going to have to do shots a couple of times a day.”
Emma will fit the shots in among the other must-dos in her 7-year-old world—playing with Barbies, Legos, riding her bike, drawing, coloring and meeting up with her Girl Scout troop.
While at the children’s hospital, the Scott family got a major education in diabetes care from the diabetes educator, dietitians and doctors.
“They talked us through counting carbs and we practiced doing shots and checking blood sugar,” Liz said. “It’s a huge sigh of relief. They said there is no dumb question and that we could call any time of the day or night. It’s very comforting.”
In retrospect, Liz said there were signs. Emma drank a lot of water, apple juice and milk, and in turn, urinated frequently. The irritability makes sense now, too.
“She would go on these swings of being normal Emma to ‘Leave me be, I just want to lie here,’” Liz said.
‘Going to live normally’
Besides sugar tests and injections, the family will now count Emma’s carbs.
“However many carbs she’s consuming we’re going to have to counteract that with her insulin,” Liz said.
Emma can still munch on her favorite foods—hamburgers, cheese pizza, meatloaf, tater tot casserole and lasagna—she’ll just have to be careful with insulin adjustments.
“We’re going to live normally,” Liz said. “We just have to count what we eat and make sure she has the insulin on board before she eats it. The dietician showed us an app for our phones that we can use to quickly look up foods if we’re out to eat. It’s been a scary whirlwind but we’re getting educated so we can make it all good.”
‘Times have changed’
Dr. Appiagyei-Dankah said Emma is progressing well.
“She came in severe diabetic ketoacidosis,” he said. “She has improved significantly and has now been switched to insulin injections. Her prognosis is good. A long time ago, being diagnosed with Type 1 diabetes was almost a death sentence, but times have changed.”
Unlike Type 2 diabetes, Type 1 has nothing to do with dieting or eating too much sugar.
“It is not preventable,” Dr. Appiagyei-Dankah said. “At the same time, there is no cure for it as of now, even though there is a lot of research going on in this area.”
As long as Emma, her parents and the diabetic team work closely together, he said there’s no reason Emma can’t live a normal life.
“Even though taking care of the diabetes demands a lot of time and effort, our goal in treatment is to let the children be children—grow up normally, go to school and participate in sports, camping, sleepovers. With good diabetes management, children these days can grow up to be whomever they want to be.”




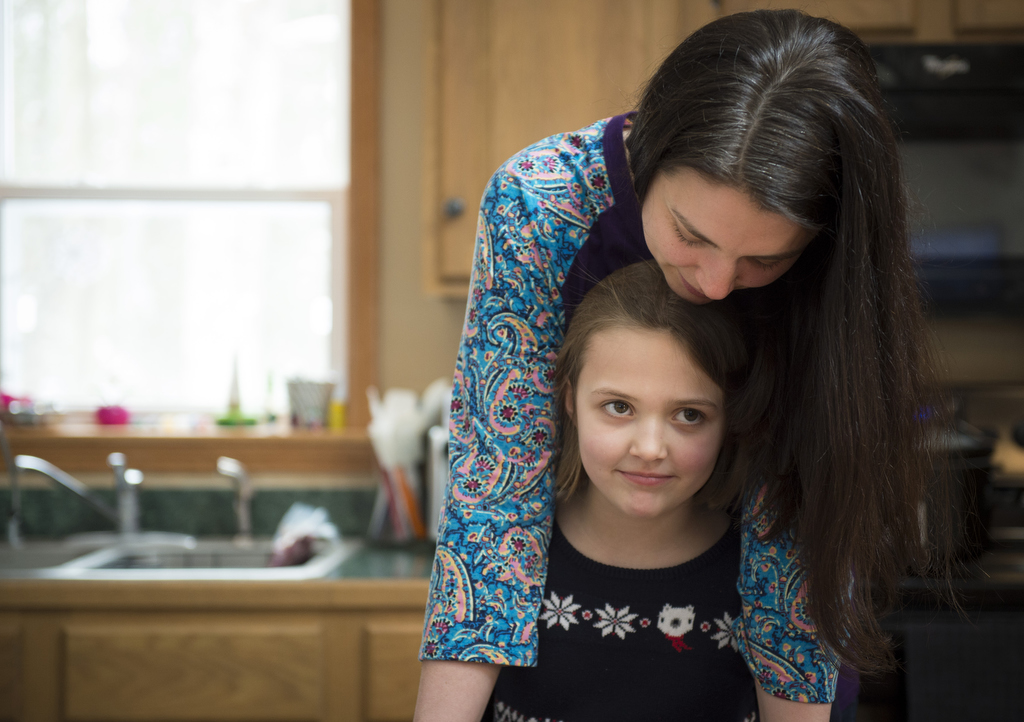





























 /a>
/a>
 /a>
/a>
 /a>
/a>
I recommend that she gets a insulin pump. It will make life a lot easier. My son is type 1 and we as a family has lived with this together since he was 11, he is now 30. The main thing is recognize the signs. The signs of when she is to low and when it’s to high. My emergency responders don’t have the equipment to see how high the sugar actually is. That can be just as dangerous as you all ready know. I can go on and on. Good luck and let her be a kid.
This family is a fantastic example of taking a critical health issue, learning all they can about how to control the physical and emotional aspects of the disease and becoming a wonderful “poster family” of healthy living. Thanks for the example.