Jeff Porter kept himself in peak physical condition. He spent all winter training and had just completed his first marathon.
But in the first game of his over-40 soccer league last June, Porter planted his leg going after the ball, got tangled up with another player and collapsed in pain.
“Did I hear something pop out there?” one player asked Porter, 46, as he limped off the field.
“I think so,” Porter said.
Over the next few days, Porter lost all lateral mobility in his leg. At his daughter’s soccer game, he tried to move sideways to stop a rolling ball. His leg buckled.
“I knew something was wrong right then,” he said.
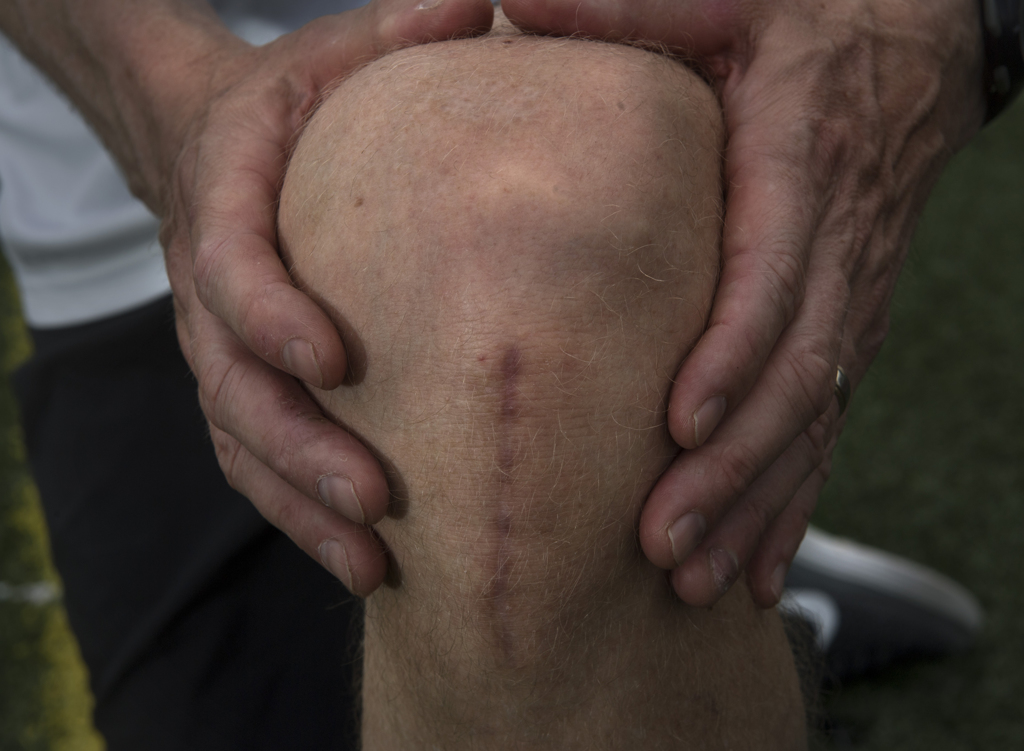
He set up an appointment with James Lebolt, DO, division chief of orthopedics for Spectrum Health Medical Group. An MRI revealed Porter had torn his meniscus and anterior collateral ligament, better known as the ACL, and sprained his MCL.
The night of the injury, Porter, who loves to ski, play soccer, swim, bike and run, swore he’d never play soccer again if he could just avoid surgery.
“I began bargaining with a higher power,” he said.
But surgery, the MRIs showed, was his only route.
‘Built like a 20-year-old’
Dr. Lebolt oversees about 100 ACL-repair surgeries each year. He’s former team physician for Virginia Tech athletics and trained under Dr. James Andrews, arguably the most famous sports surgeon in the country.
Porter’s type of total knee reconstruction surgery is not uncommon, especially for athletes. But those are always high-pressure cases, Dr. Lebolt said.
“I knew he was a high-level athlete that trained for different types of races, bike races and competitive events, and it’s always a concern for any athlete to help them get back to sport,” he said. “Luckily, he’s a 40-something-year-old built like a 20-year-old.”
Dr. Lebolt made the decision to use a piece of Porter’s own patellar tendon to repair his ACL. The downside? It can cause some lingering knee pain issues. But it’s twice as strong as the original ACL, so for athletes, they’re unlikely to ever tear their ACL again.
Another option is using a cadaver graft, but “it’s structurally weaker. Only half as strong,” Dr. Lebolt said. “I prefer the patellar tendon graft. Especially with athletes.”
Porter started physical therapy the day after surgery. He started with water-based therapy, then after eight weeks progressed to a stationary bike.
In mid-October, about three months after surgery, Porter got the OK to start jogging again.
He said Dr. Lebolt’s help didn’t end on the surgical table.
“The whole time, Dr. Lebolt had been very instructional on what not to do and letting things heal, and not hurting myself by not doing too much too soon,” Porter said. “Which, as a patient, was great. It’s what I needed to hear.”
Porter remembers his first post-surgery run vividly.
“It was uncomfortable, painful, but it was awesome to be able to do that,” he said.
“I slowly progressed from there, being able to run farther and with less pain every time. And when I saw Dr. Lebolt for my five-month checkup, he said, ‘You’re good, you can return to whatever you want to do.’ So I kind of got the green light.”
Because he qualified for the Boston Marathon when he ran his first marathon in 2017, Porter had a decision to make. He could try to train for it, or likely give up on that dream forever. Even for injuries, the Boston Marathon doesn’t allow deferrals to future years: You use your spot or lose it.
After consulting with his doctors, Porter made the decision in mid-January to try for it, but “with the mindset that if I got into longer runs and if it wasn’t feeling good, if the knee wasn’t holding up, I’d have to abandon it.”
Good cop, bad cop
Following Dr. Lebolt’s advice, Porter spent more time training in the pool and on a bike. He only ran two days per week.
“Dr. Lebolt is a skilled and excellent surgeon and also a very wise doctor in terms of advising me on how to recover,” Porter said. “He was my toughest critic in terms of saying, ‘You’re doing too much, I don’t want to see you out doing yard work.’ And, ‘More biking and swimming, you’ve got to think about long-term and what’s good for your knee.’ … It really helped me not push it.”
For his part, Dr. Lebolt said with athletes and active patients, the post-surgery advice is almost more important than the surgery itself.
“I want to be a voice in their mind when they’re exercising, almost like good cop, bad cop,” he said. “My goal is to get them back to the sports they enjoy, not near-term, but … to emphasize long-term and more moderation. I want to get them back to lifelong enjoyment of the sport, not just the next race or next year.”
But as spring neared, Porter’s outlook only improved.
“Each week, I was feeling stronger and better, and I was able to run Boston,” he said. “My knee felt better that day than it had any training run since surgery.
“It was an awesome experience: one, to fulfill that dream and two, to overcome an injury that I thought for sure I would not be able to run another marathon with and didn’t know what my life would be like.
“That was a huge overcoming-adversity moment for me,” he said.
Porter said he’s still not fully recovered, despite running the marathon in three hours and 33 minutes. His left leg still doesn’t have the muscle it did pre-injury. But Dr. Lebolt told him it’d likely take two years to fully recover.
As for any more marathons in his future?
“I think this was just a one-time thing,” Porter said. “I’m not sure I’ll do anymore marathons because of my knee. I want to preserve it, and I know I’m at higher risk.
“At this point, I feel like I accomplished what I wanted,” he said. “I still plan to run, ski, be as active as ever. … I just want to be healthy for a long time.”












 /a>
/a>
 /a>
/a>
 /a>
/a>
Dr. Porter has been my doctor for almost 13 yrs. He is wise, kind and has helped me thru some very difficult times. We have become good friends, and I watched him go thru this journey. He has great determination, strength of mind and body. He told me he would bring home a Medal for finishing the Boston Marathon, and he did! Way to go DR. Porter.