Like a bird flitting back to the nest, 5-year-old Pheenyx ran across the lawn for a hug from mom.
Gresha Eberly wrapped her arms around the girl―her youngest child and only daughter.
“My little princess,” she said. “She definitely is what started me on the road to recovery.”
A smile and a quick kiss, and Pheenyx was back with her brothers, playing catch.
The fleeting mother-child moment, blooming casually on a sunny summer day, seemed a long way from the early days of Gresha’s pregnancy with Pheenyx.
Fear hung like a shadow over her life then. Fear of telling people she was pregnant―and addicted to drugs. Fear of losing her children. Fear of withdrawal.
And fear of seeking prenatal care, because she worried a doctor’s appointment would lead to all her other fears.
I survived something that is killing a lot of people. A lot more people can survive this if they have the right tools and the right support.
And yet it was that first prenatal appointment with a Spectrum Health Maternal Fetal Medicine specialist, four months into her pregnancy with Pheenyx, that opened the door to sobriety for Gresha.
She still marvels at what she found behind that door―a better life for herself and her family
“My addiction kept this whole world secret from me for so long,” she said. “Once I started getting into recovery, all my five senses were coming back full-force. It was like a whole new world was introduced to me.
“It’s hard to explain, but everything is brighter.”
Now, she shares her experience with addiction and recovery in hopes of helping other women dealing with substance use disorders during pregnancy.
“Don’t wait to get help,” she said. “If you can reach out to just one person, do it. You don’t have to die from this disease.”
But she understands why women are reluctant to seek help. She knows the stigma society places on addicts.
“Coming out and saying you’re an addict while you’re pregnant, you don’t get the very best feedback,” she said.
Through an online blog and in talks she gives to medical students, she works to counter that stigma, to put a human face on the issues of addiction and pregnancy.
Rural areas hit hard
Gresha, a 34-year-old woman from Lake Odessa, Michigan, is among the growing number of women in the U.S. dealing with substance use disorders during pregnancy. The issue parallels the nation’s exploding opioid epidemic, fueled by prescription painkillers, heroin and fentanyl.
In 2012, nearly 22,000 babies were born with the drug-withdrawal symptoms of neonatal abstinence syndrome. That’s a five-fold increase since 2000, according to the National Institutes of Health.
The issue hits rural areas particularly hard. Maternal opiate use in rural counties was nearly 70 percent higher than in urban areas―8 per 1,000 childbirth hospitalizations, compared with 4.8 in urban counties.
Cara Poland, MD, an addiction medicine specialist with the Spectrum Health Addiction Rehabilitation Program, has a special interest in working with pregnant women with substance use disorders. She admires the courage of those who seek treatment.
“These women often encounter a lot of judgment and misunderstanding of their disease,” she said. “That can increase the amount of fear they have of coming forward.”
Illicit opiate use increases the risk of miscarriage. As with any pregnancy, the odds of a healthy pregnancy increase with prenatal care. Women with a pregnancy complicated by opioid addiction would receive medication-assisted treatment as part of their treatment for their addiction, Dr. Poland said. The most common medications used are methadone and buprenorphine (commercially known as Suboxone or Subutex).
Methadone is not known to cause any long-term developmental effects on the child. Buprenorphine has not been available as long, so there is not long-term developmental data available. Directly after birth, Dr. Poland said, some babies will undergo withdrawal, which can be safely treated by pediatricians and is not known to have any long-term effects on the child.
Effect on the family
Gresha’s struggle with addiction began when she used prescription painkillers to treat back and knee pain. She took a double dose one night, and within 10 minutes, she got out of bed and started cleaning her house. She began taking three or four doses at a time.
“I felt weightless, like I was unstoppable,” she said. “They became my best friend after that.”
Doctor shopping, she eventually got prescriptions for Norco, Ritalin and Xanax. A month’s supply would run out in a couple of weeks. And then she would go to Lansing to buy drugs on the street. When money ran low, she snorted heroin.
“When I was doing drugs, my whole being was about getting pills,” she said.
Her husband, Devin, became frustrated as rent money went to drugs.
We know that pregnancy is a time when people make great changes in their health and great changes in their lifestyle because of that responsibility to that unborn child.
“We would lose houses. Money would come up missing,” he said. “It was terrible, absolutely terrible. I did whatever I could to help her. But no matter what, she wouldn’t admit she had a problem.”
He and Gresha spoke openly about her addiction and recovery as their sons, Aden, 14, Steehl, 9, and Reign, 7, and daughter Pheenyx played in the backyard.
It was an idyllic setting―an acre of mowed lawn on a dirt lane, surrounded by corn and bean fields. The kids played with four kittens, born recently under a bed.
The older children remember the tough days of addiction and were with Gresha when she suffered seizures, brought on by drug withdrawal. The younger children just know there was a time “when Mommy was sick.”
The couple, together for 14 years, separated briefly when Gresha was pregnant with Pheenyx. Devin didn’t know about the pregnancy. Gresha had told everyone she had a miscarriage.
“I didn’t want to stop using,” she said. “It was a weird, crazy, sticky situation.”
Getting clean
Four months into the pregnancy, she made her first prenatal appointment with a maternal fetal medicine specialist at Spectrum Health. She had an ultrasound, and when the scan revealed a baby girl, Gresha began to cry.
The doctor also told Gresha she tested positive for opiates, amphetamines and benzodiazepines (like Xanax). He referred her to an addiction specialist with Spectrum Health’s Center for Integrative Medicine.
She began medication-assisted treatment and received counseling―reluctantly, at first. Through treatment, she began to understand how the disease of addiction affected her brain.
“It seems like every appointment I had an aha moment,” she said. “It gave me a better understanding about myself.”
Pheenyx arrived five weeks early, at 4 pounds, 10 ounces. Small but healthy, she grew quickly.
“She is a very smart little girl,” Gresha said. “I’m very lucky to have her.”
She and Devin reunited. They got married. Although Gresha suffered a relapse, she has now been in recovery for nearly four years.
She considers Oct. 13, 2013, her “clean day.”
Today, Devin said, life “is great.” They play baseball, camp and hunt as a family.
“I don’t stay in bed all day,” Gresha said. “I still have not-good days. But I’m alive. I’m here and I’m taking care of my kids.”
‘I survived’
Gresha’s story of recovery mirrors the journey made by many other women, Dr. Poland said. In seeking treatment, they change two lives―their child’s and their own.
“We know that pregnancy is a time when people make great changes in their health and great changes in their lifestyle because of that responsibility to that unborn child,” Dr. Poland said.
When that lifestyle change involves treating an addiction, “the biggest barrier is fear of judgment,” she said. “When they come to see me, there already is so much guilt and shame that comes with this disease.”
As the opioid crisis hits epidemic levels, Dr. Poland said it affects women―and pregnancies―across all socioeconomic levels.
And that’s the message Gresha wants to drive home.
“I want to tell people that addicts aren’t just people living under bridges or deep in the inner city,” Gresha said. “Addiction is out there. It doesn’t discriminate by race, religion―anything.”
This fall, she plans to become trained as a recovery coach through Recovery Allies.
“I survived something that is killing a lot of people,” Gresha said. “A lot more people can survive this if they have the right tools and the right support.”





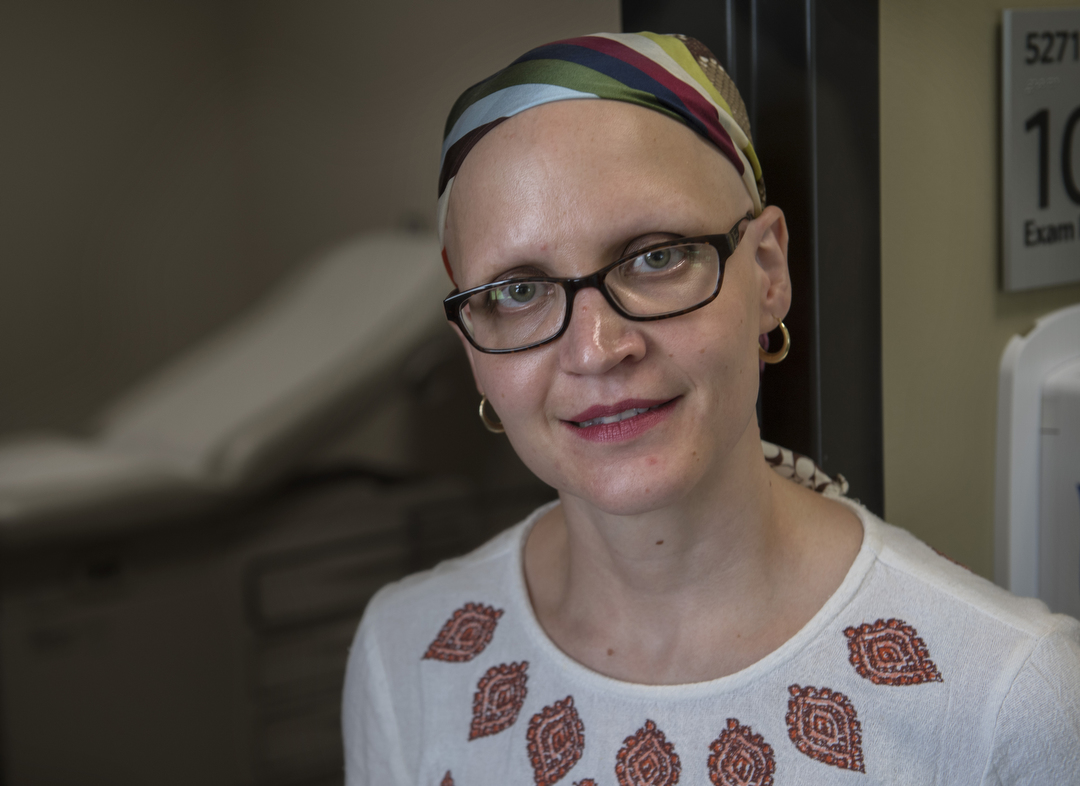
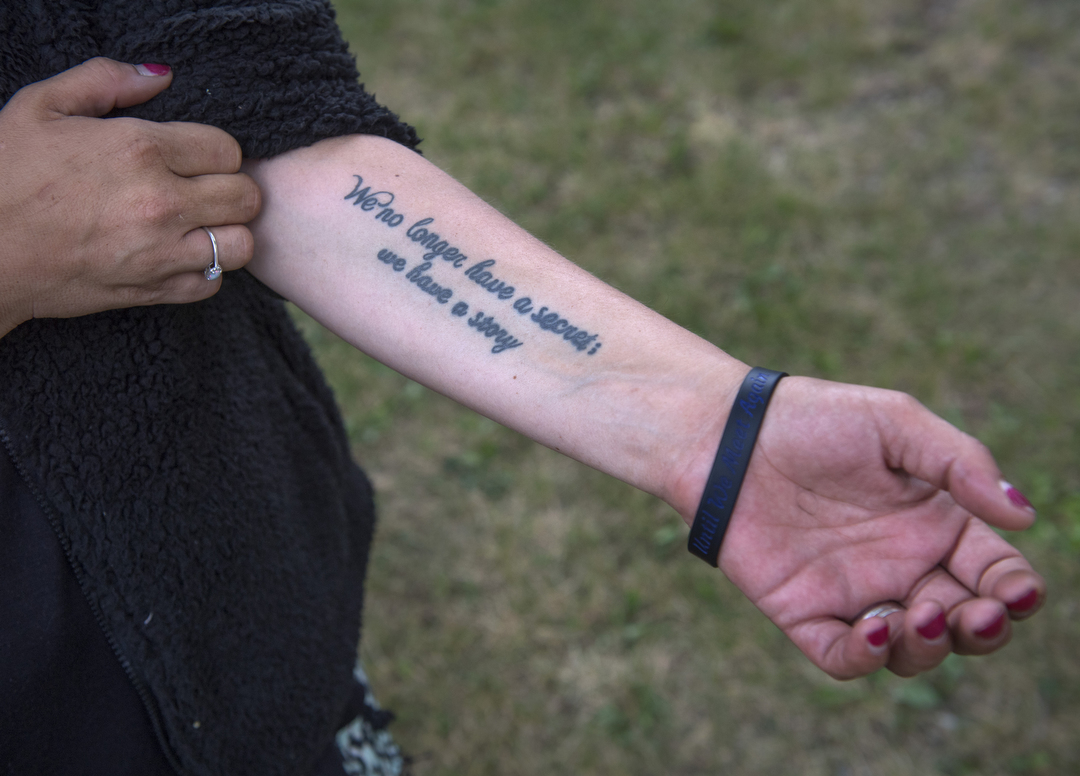



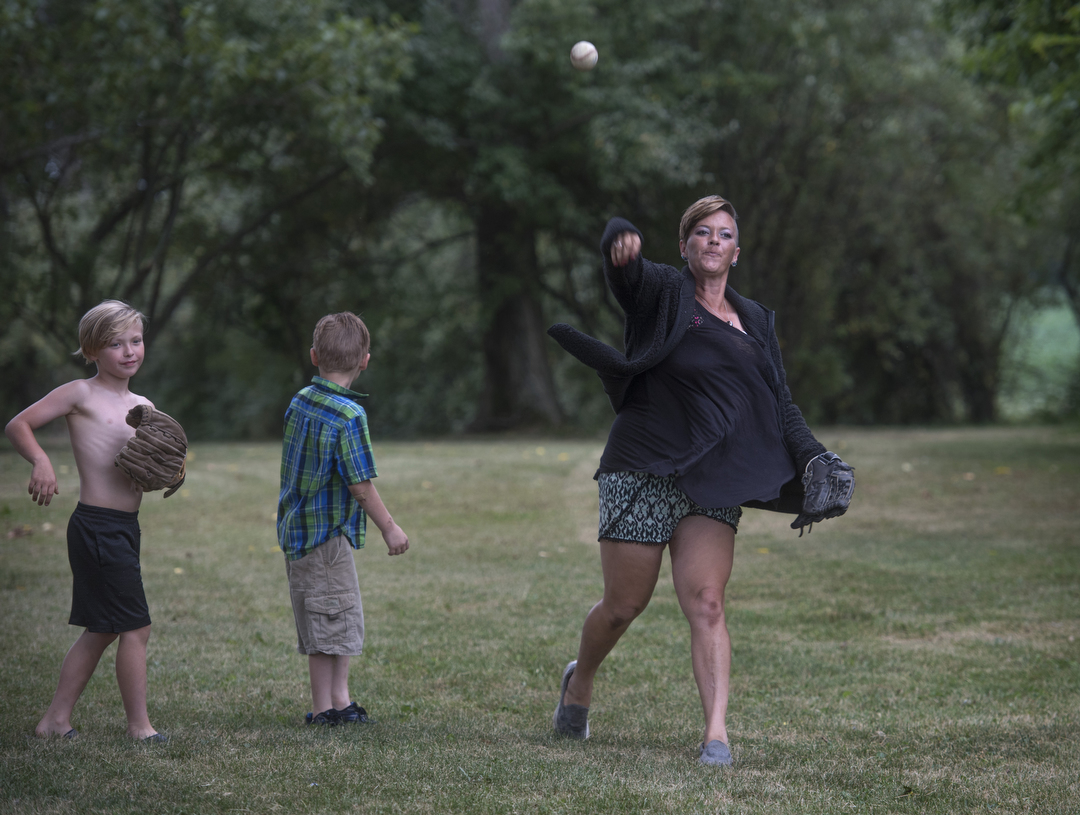












 /a>
/a>
 /a>
/a>
 /a>
/a>
I truly enjoyed reading this. Gresha you have my love and support all the way. I’m very proud of you both. Devin and you share a love that will last a lifetime until eternity and after.
I love you all so much ❤
What a lovely comment, Sue. I’m sure it will mean a great deal to Gresha.
This was beautiful and hopeful! I live in a family that struggles with addiction, it is nice to hear a success story! INSPIRING! So happy for you and your family 🙂
Gresha Eberly certainly is inspiring. Thanks so much for reading and commenting.
You are a true inspiration to me. I’ve been struggling with my son and his addiction for some time. It destroys the entire family and causes so much pain and depression. I am so thankful for you and your family that you are conquering such a hard thing.