Mark Lackey lived 53 years with a hole in his heart.
He had no idea.
All those years he did heavy lifting, building habitats for lions and tigers in Texas, that hole was there.
Throughout his adventured-packed life, an opening lay in the structures of Lackey’s heart, robbing his body of oxygenated blood, weakening his lungs.
It caught up with him eventually. It turned the powerful, muscular guy into a weak, sickly man. By the time he found out what was wrong, he was too ill to have surgery.
“I was at the end of my rope,” he said. “I thought if I can’t get better, there is no sense in trying to live like this.”
To his great relief, an innovative new option emerged: a stent crafted just for him, which could be placed without open-heart surgery.
It took a team to bring it about—including the specialists at the Congenital Heart Center at Spectrum Health Helen DeVos Children’s Hospital, researchers at Michigan State University, the manufacturer of the stent and the U.S. Food and Drug Administration.
“I feel blessed, big-time,” said Lackey, who tearfully gave bear hugs to his doctors and caregivers after the procedure. “This right here is one of the toughest things I’ve ever been through.”
Given all Lackey has done in his life, that’s saying a lot.
‘Life to the fullest’
Growing up on a blueberry farm in Southwest Michigan, Lackey was a self-described adrenaline junkie. He’s been in several car accidents and numerous fights. He was struck by lightning. Always on the go, he hunts, fishes, rides bikes and plays volleyball.
“I lived life to the fullest and then some,” he said.
Life led him to Texas, where he built habitats for lions and tigers.
He once saved the life of a choking lioness by performing the Heimlich maneuver for 45 minutes―and after she revived, quickly exited the enclosure.
He put his wilder days behind him and in 2013 returned to Michigan. He reunited with his childhood sweetheart, Brenda, a widow raising three sons, and they married in 2014.
About two years ago, his health began to decline dramatically. The man who once hoisted telephone poles over his head could no longer walk across a room without stopping to catch his breath.
It seems like a miracle got pulled off. I feel very, very, very fortunate.
He developed a bad cough, which he thought was bronchitis. It went on for months.
“My heart rate was 130-something. It went up to 140 beats a minute at rest,” he said. Although healthy blood oxygen levels is above 95 percent, “my oxygen level was in the low 70s-high 60s.”
He saw doctors and had his lungs X-rayed, but an X-ray couldn’t detect the congenital heart defect. He did research online and thought he had damaged his lungs by using high-strength bug repellent for outdoors work.
“Not being able to breathe is awful,” he said. “I felt like I was sucking air through a straw.
“I couldn’t lie down. If I lay down flat, I didn’t know if I was having an anxiety attack or what, but I couldn’t breathe. For two years, I probably did not get a good night’s sleep.”
In May 2018, during a visit to his family doctor, his heart rate was so high and oxygen saturation so low that the doctor sent him by ambulance to a local emergency department.
From there, he was transferred to Spectrum Health Butterworth Hospital and admitted to the intensive care unit.
“He presented to the emergency room pretty much blue,” said Sihong Huang, MD, an adult congenital heart disease specialist. She was called to the ICU when tests showed an abnormal blood flow in his heart.
Lackey knew he was in rough shape. He cried, telling Dr. Huang he wanted to live. He worried about his wife, Brenda.
“I didn’t know if I was going to make it. I was scared,” he said. “My only fear was that I don’t want to leave her alone.”
A heart defect since birth
Lackey had severe pulmonary hypertension—pressure in the lungs, as well as an enlarged right heart ventricle.
An echocardiogram and CT scans revealed the cause: a congenital heart defect. A 1¾-inch hole lay between two blood vessels adjacent to the heart. The hole opened a gap between a vein that brings blood from the upper body to the heart and the atrial septum, the wall between the upper two chambers of the heart.
His heart condition was further complicated by mixing of blood—oxygenated blood from the lungs drained into the right side of the heart, or right atrium, instead of the left atrium.
Because of this complex defect, too much blood was being pumped to his lungs, putting abnormal pressure on the lungs and leading to pulmonary hypertension. His heart began to pump poorly oxygenated blood to his body. And his heart function weakened, and he developed arrhythmia.
His condition―diagnosed as superior sinus venosus atrial septal defect with partial anomalous pulmonary venous connection―typically would be repaired with open heart surgery if found in a young child.
But in Lackey’s fragile state, an operation would be too risky.
After diagnosing his condition, Dr. Huang shocked Lackey’s heart back to a normal rhythm and then treated him with medications that improved his condition by lowering the pressure in his lungs. She also consulted Joseph Vettukattil, MD, the co-director of the congenital heart center.
A congenital interventional cardiologist, Dr. Vettukattil has done pioneering work in creating 3D images of the heart and treating complex heart conditions with minimally invasive procedures.
He decided to explore a treatment that would block the hole by placing a covered stent in the blood vessel. It’s an extremely rare approach: He found only one other case reported in literature.
With help from 3D imaging, congenital heart center researchers and a 3D model printed by MSU’s biomedical engineering department, Dr. Vettukattil designed a stent that could be placed in the blood vessel through a catheter inserted in the femoral vein.
NuMED, Inc. manufactured the custom-covered and mounted Cheatham-Platinum stent.
Because of this innovative approach, the congenital heart team had to receive authorization from the FDA before using the device.
Once the FDA authorized it, Dr. Vettukattil met with Lackey to explain his plan. Lackey readily agreed to the procedure.
“This is kind of overwhelming,” he said. “I appreciate all the work everyone has put into it. I got faith in you guys. We will just roll with it.”
A test run
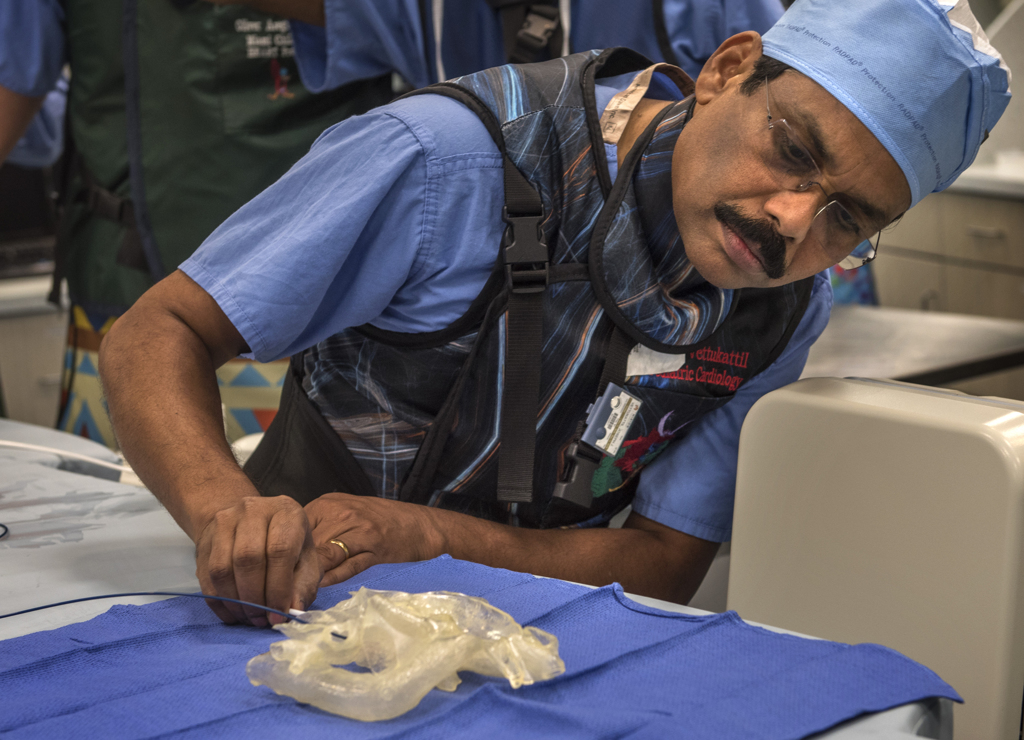
Dr. Vettukattil had two stents made so he could perform a test run before the procedure.
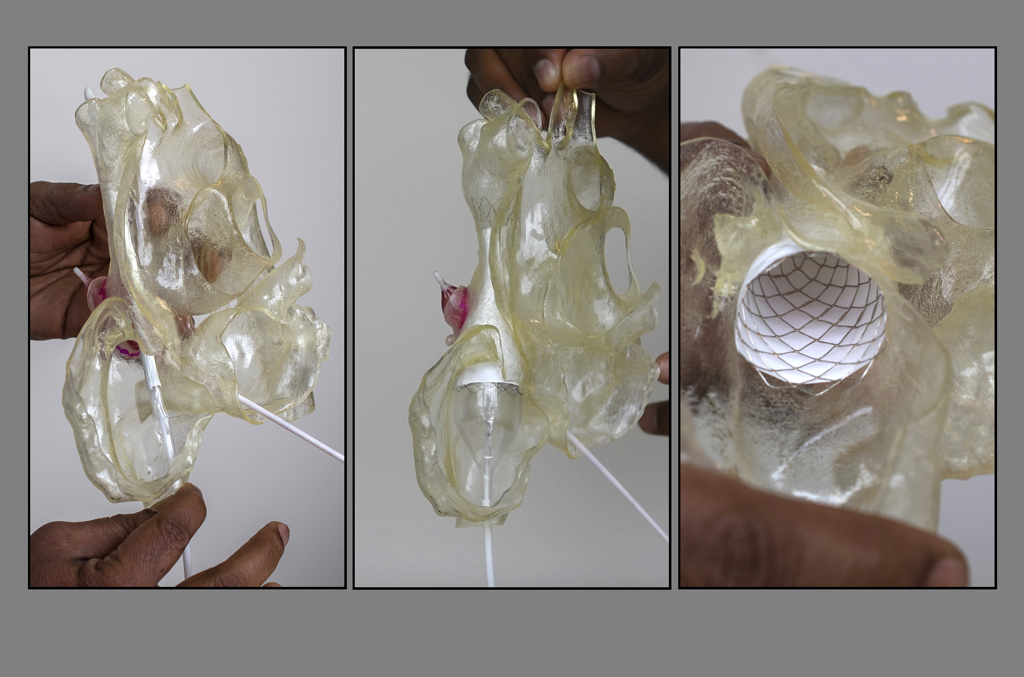
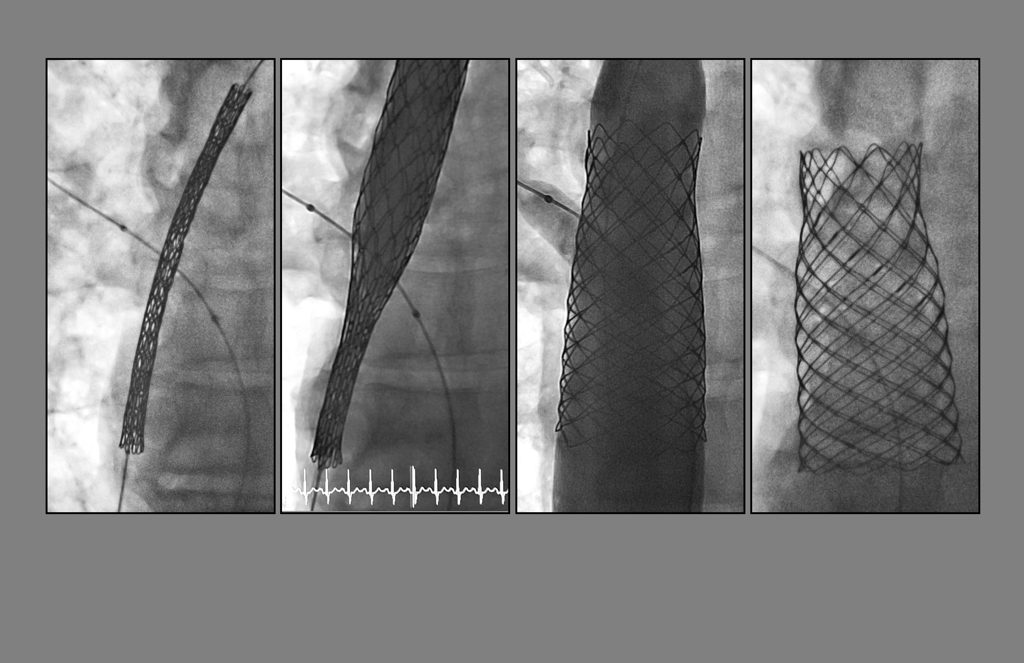
On May 21, 2018, he placed a covered stent inside a 3D printed heart model. The model, which mirrored the unique anatomy of Lackey’s heart, was cut in half, providing a clear view of the stent as it was placed inside the superior vena cava, the blood vessel where the hole lay.
The stent in place, Dr. Vettukattil next inflated the balloon inside it, expanding the stent to fill the width of the blood vessel.
As it grew wider, the 11-centimeter stent shortened in length to 7 centimeters. But when fully inflated, the stent successfully covered the hole, without blocking access to the blood vessel coming from the lungs. The test run showed the device would allow blood to flow into all the chambers of the heart correctly.
“It fit perfectly well,” Dr. Vettukattil said.
Deploying the stent
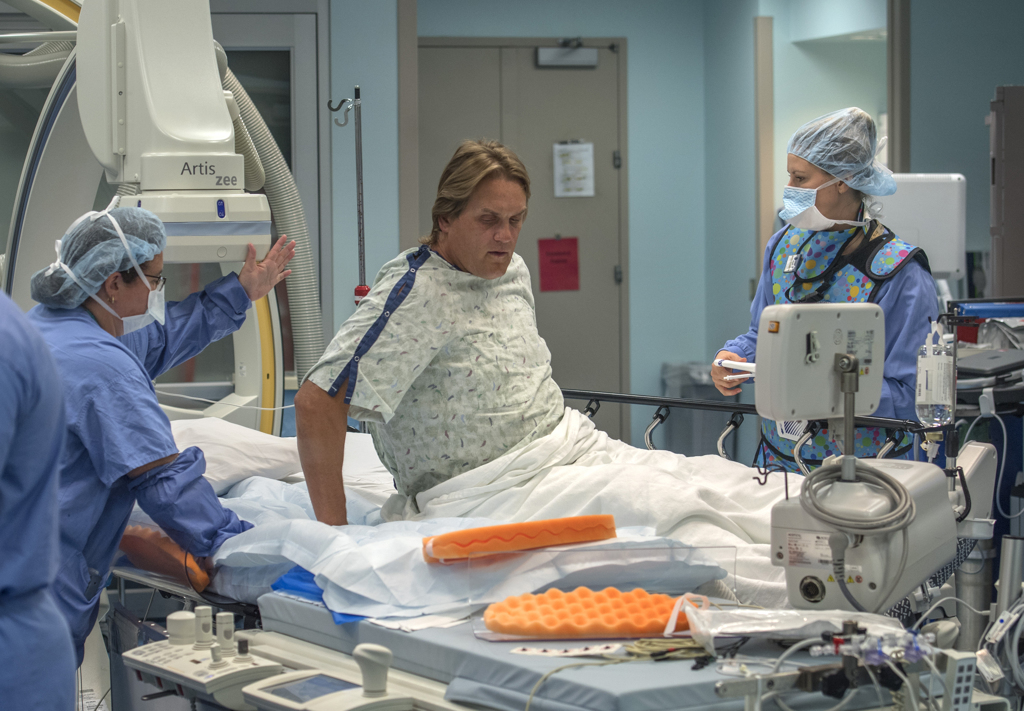
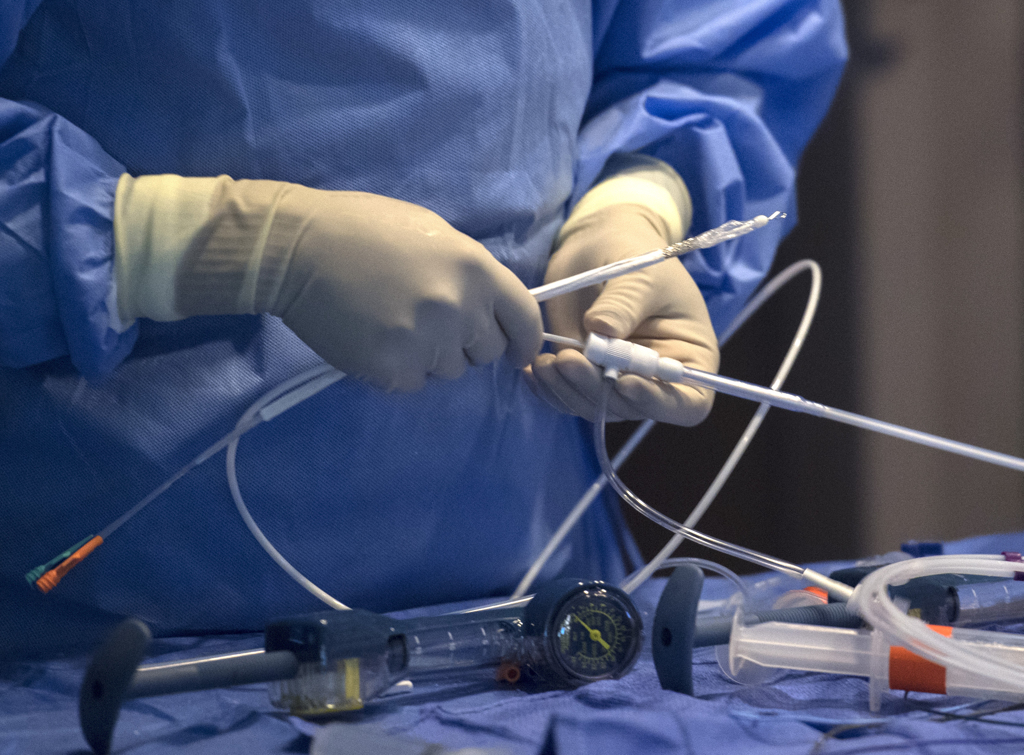
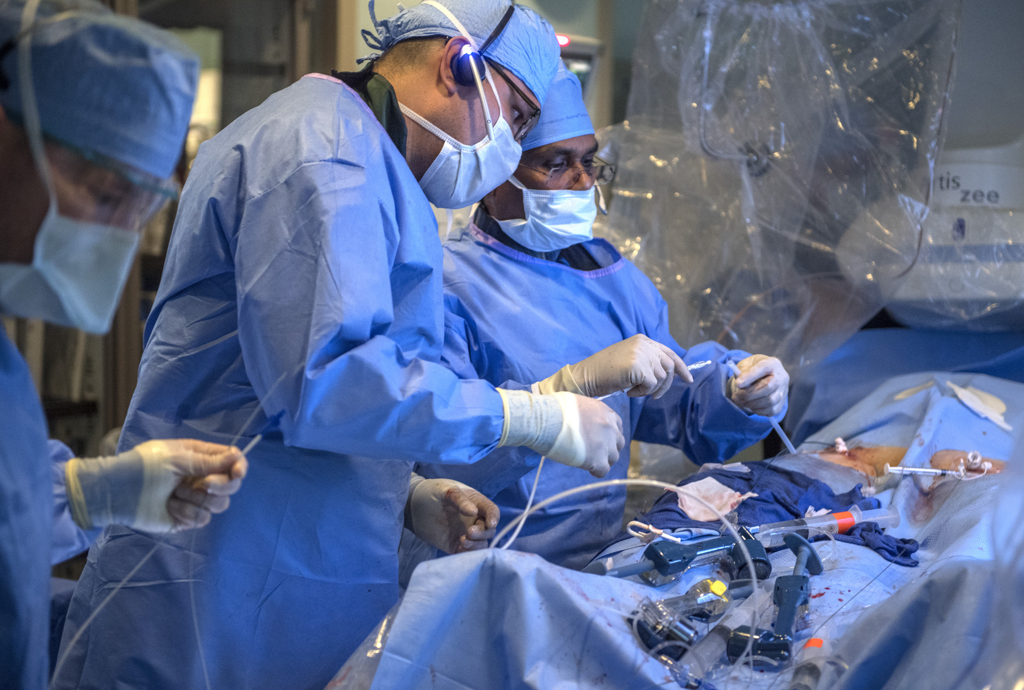
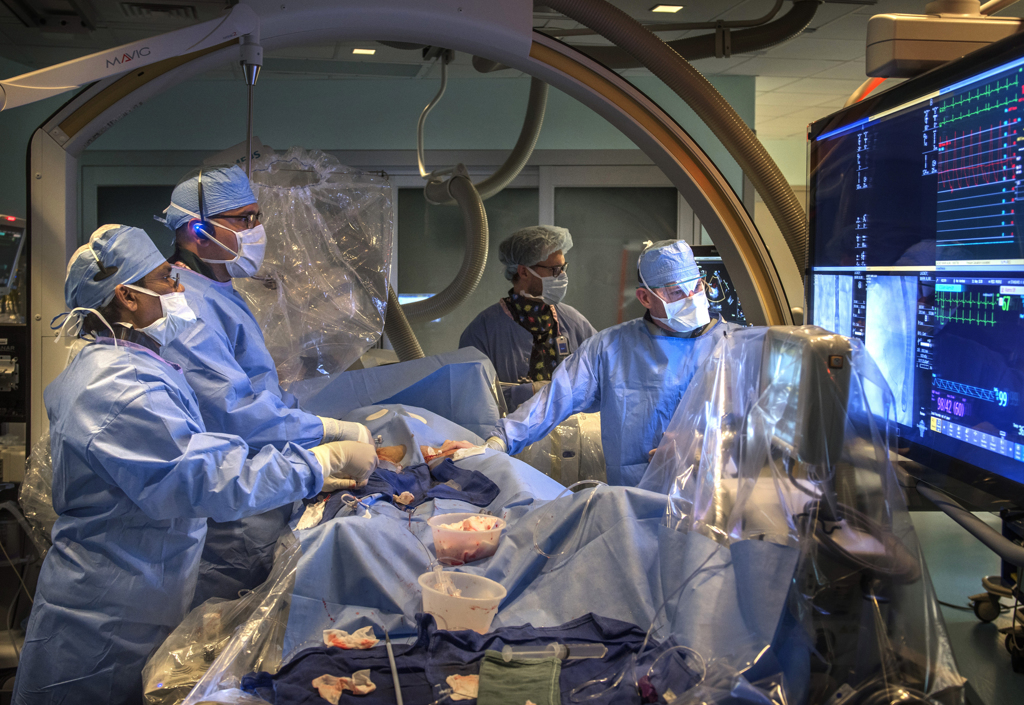
Ten days later, Dr. Vettukattil performed the same procedure, this time on Lackey.
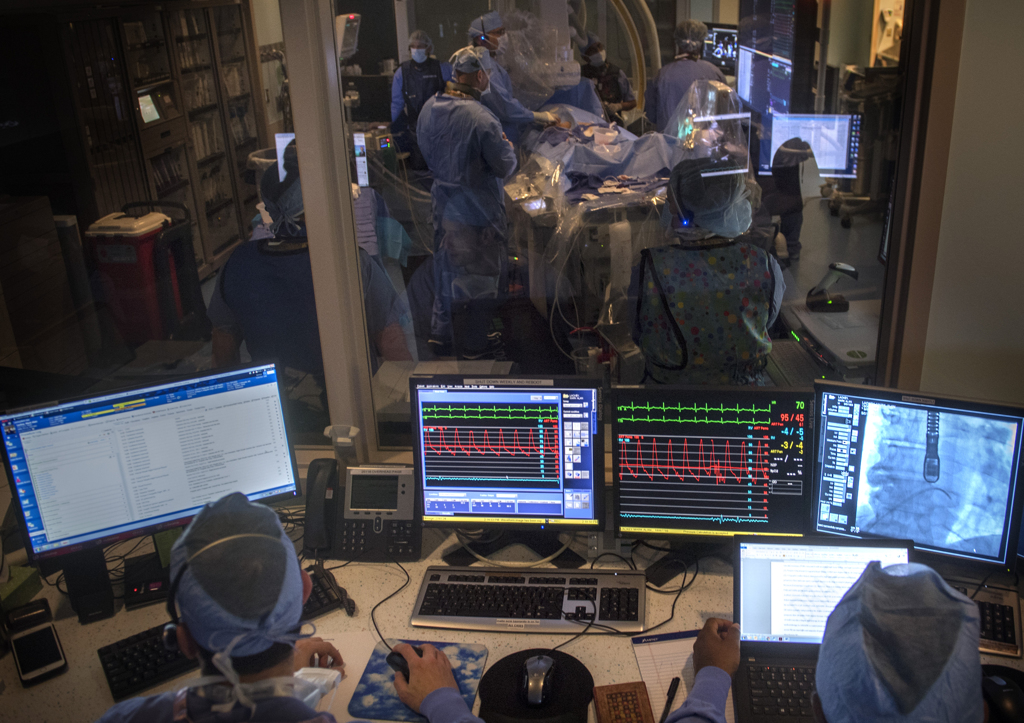
In the cardiac catheterization lab at Helen DeVos Children’s Hospital, surrounded by members of the congenital heart team and aided by real-time X-ray images, he guided the stent through a vein in the groin up to the superior vena cava.
With the stent in place, he inflated it with the balloon, then removed the balloon. An echocardiogram showed the blood flowing through the stent, bypassing the hole.
“It’s a good result,” Dr. Vettukattil said. “Based on the echo, it’s in a perfect position.”
Two weeks later, Lackey arrived for a follow-up visit and echocardiogram. The results: his enlarged heart had shrunk in size, blood flowed normally through the veins leading to his heart and the swelling caused by water retention had almost disappeared.
“Your heart function is still recovering,” Dr. Vettukattil said. “The pressure in the lungs is very high. It takes time for it to come down.”
Lackey will continue to see his adult congenital heart disease and pulmonary hypertension specialists to assess his heart and lungs and monitor medication. And Dr. Vettukattil advised him to avoid heavy lifting or exercise for three months. But in time, he should be able to return to all the activities he loves.
For Lackey, just being able to get a good night’s sleep and walk without losing breath is a big improvement.
“I kind of feel like Iron Man,” he said.
‘At 100 percent’
At his home in Mattawan, Michigan, Lackey marveled at the changes he has felt since receiving the stent. All his life, he believes he functioned at about 75 percent of his capacity.
“I look back on it now and I don’t think I ever was at 100 percent,” he said. “But until you reach 100 percent, you just don’t know that.”
And he marveled at the number of people and processes that came together to make his heart procedure possible.
“It seems like a miracle got pulled off,” he said. “I feel very, very, very fortunate.”




































 /a>
/a>
 /a>
/a>
 /a>
/a>
Amazing! This man is a miracle thanks to the DR’s at Spectrum.
Thank you all so very much for saving my cousin Marks life. Our family owes you a debt of gratitude. May God bless and keep you in his love and care.
Joy Smolinski, Russellville, AR
I think the whole medical team really enjoyed getting to know Mark and were happy they could help him. Blessings to you, too, Joy!
So glad God placed these wonderful doctors to do his miracle working power!! Sounds like you are going to do great!!