
Jason McFate and his physicians are not sure why epileptic seizures have plagued him for more than half his life, but he distinctly remembers his first.
“It started when I was 13,” Jason, now 29, recalled. “I don’t know how or why, but I had just got done taking a test and was just sitting at my desk waiting for the class to end.”
After 16 years of seizures, Jason recently underwent a neurosurgical procedure at Spectrum Health that promises a profound impact on his quality of life. He is eager to share the results of his surgery in hopes that the information may benefit others who share a similar life story.
Sixteen years of seizures
After that first seizure, the next few years proved to be difficult for Jason as grand mal and complex partial seizures occurred when he least expected them.
A grand mal seizure is the violent episode many think of when the word “seizure” is mentioned. Such a seizure often includes a loss of consciousness, convulsions, muscle rigidity and violent contractions. Complex partial seizures are more subtle, sometimes showing little outward sign that an individual is having one.
“During the complex partial seizure I’m awake and don’t completely lose consciousness,” Jason said. “I can hear, but I can’t respond.”
One of the most troubling aspects of the disease for the adolescent Jason, a lifelong Detroit Lions fan and former Rocket football player, was being prohibited from playing high school football.
And, of course, there were a few thoughtless classmates who tried to have fun at his expense. But that stopped pretty quickly, the Union City, Michigan, native recalled.
“I had some pretty good friends who would take care of things for me,” he said. Older brother Ryan, now 32, and younger sister Kim, 28, always watched his back.
It was Ryan whom he texted in the midst of one of his most terrifying episodes. Driving down the road alone in his car, he recognized the onset of a grand mal seizure.
“I have auras that will usually give me about one minute of warning before full onset of the seizure,” Jason said.
Aura is the term that describes symptoms occurring just prior to a seizure. These symptoms may include visual changes and distortions, auditory hallucinations, feelings of numbness and separation from one’s body, nausea, anxiety and even strange smells.
In this case, Jason’s aura gave him just enough time to stop on the side of the road.
“I pulled over, put my keys under the seat, and quickly texted my brother in Battle Creek, saying, ‘Come and get me. I’m having a seizure,’” he said.
The majority of epileptics—about 70 percent—are able to keep their seizures at bay with medication, but in Jason’s case, the effects of the drugs would wear off and seizures would start all over again within a year or two after beginning a new medication.
At 29, often suffering up to three seizures per week, Jason’s health issues threatened to interfere with his job as a group leader for an RV manufacturer. Jason’s wife, Tiffany, a nurse, has served as one of his closest health advocates and advisers. But she admits that the impact on Jason’s quality of life was becoming a challenge for him.
“It’s an unpleasant thing for Jason,” Tiffany said. “But we grew up together and I’m also a nurse, so seizures are nothing new for me. We got to the point where we had a routine.”
NeuroPace: Just the option he needed
When seizures reach the point where they seriously compromise quality of life, many epileptics opt for surgical removal of the part of the brain where the seizures originate. For those whose seizures originate in multiple locations or in areas that are too sensitive to remove, however, there are few additional options.
Fortunately for Jason, Spectrum Health is the only location in West Michigan and one of the few in the nation to offer just the option he needed.
The NeuroPace Responsive Neurostimulation System is an implantable therapeutic device designed to detect abnormal electrical activity in the brain and respond by delivering imperceptible electrical stimulation to normalize brain activity before an individual experiences seizures.
The device, a small microprocessor, is implanted into a cavity in the patient’s skull, with electrodes that attach to the brain to detect and electrically inhibit the onset of seizures.
NeuroPace is designed with people like Jason in mind.
“For patients with frequent and disabling partial onset seizures who have proven unresponsive to two or more medications and who are not candidates for actual removal of abnormal tissue, this may prove to be a viable and welcome treatment option,” said Konstantin Elisevich, MD, Ph.D., a neurosurgeon with Spectrum Health Medical Group.
Dr. Elisevich was part of one of the first clinical teams in the nation to participate in clinical trials using NeuroPace, and performed the first case in Michigan following FDA approval last year.
Important date with a robot named ROSA
Not only is Jason among the first patients in the state to receive NeuroPace, he is also the very first in West Michigan to have the device implanted with the surgical assistance of a robot.
Spectrum Health is among the first in the nation to offer patients ROSA, an advanced option for neurosurgery.
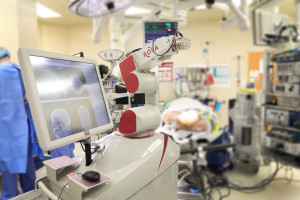
ROSA is a surgeon-directed robotic arm designed to assist during brain surgery. The use of ROSA improves accuracy and can significantly reduce total surgery time, including the time a patient is under general anesthesia.
“Robotic technology is at the forefront of the next generation of surgical treatments for epilepsy,” said Sanjay Patra, MD, a neurosurgeon with Spectrum Health Medical Group, who performed McFate’s surgery on April 14. “With these new technologies, we are accessing the deepest areas of the brain and expanding treatment of neurological disorders.”
The robot is used for cranial procedures requiring precise positioning and handling of instruments. The ROSA robotic device was designed to increase the safety and reliability of various neurological procedures without compromising established surgical protocols. ROSA acts as a reliable and accurate surgical assistant.
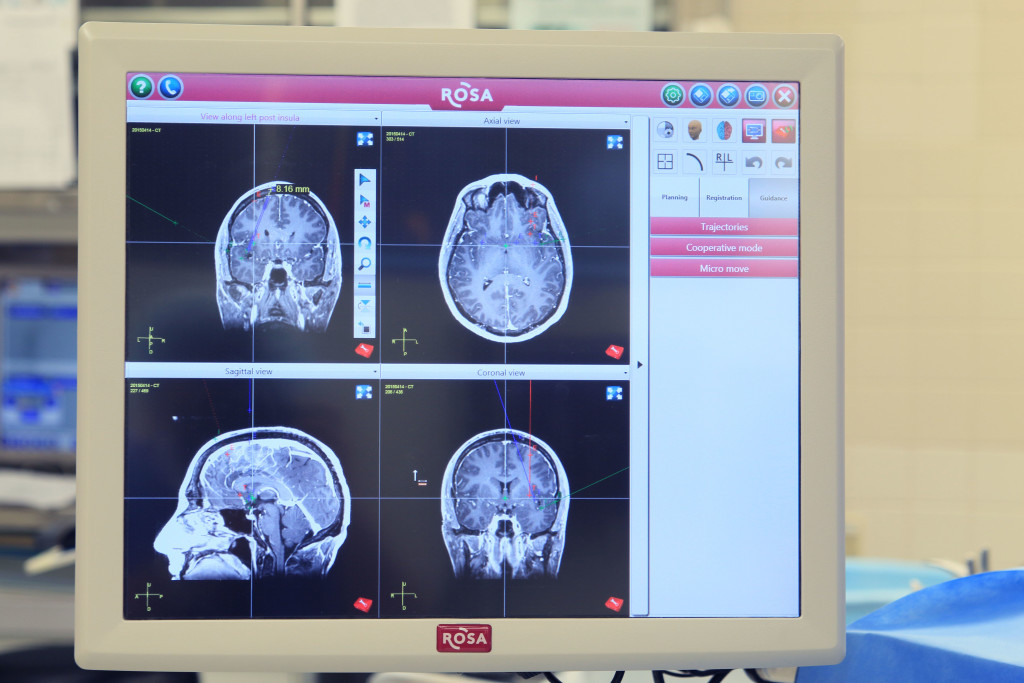
By using data from a patient’s MRI scan and precise positioning of the patient and robot, ROSA’s arm can be driven to the exact point and trajectory dictated by the physician.
“An important capacity provided by the ROSA technology will be our ability to unite a number of technologies to achieve improved patient outcomes,” Dr. Elisevich said. “These include utilization of additional tools such as Visualase, iMRI and advanced 3-D neuroimaging.”
ROSA can be used to assist with implanting electrodes that map regions of the brain affected by seizures, as in Jason’s case.
Additional uses of ROSA include placing electrodes for deep brain stimulation in patients with diseases like Parkinson’s, taking biopsies in critical, hard-to-access areas of the brain, and using the Visualase laser ablation system to destroy tissue in areas of the brain where seizures or tumors originate.
The use of this technology enables most procedures to be completed in less time, with minimal stitches and hair removal, reduced scarring and shorter hospital stays.
The road ahead
Since his surgery in April, Jason has had only three seizures, none of them grand mal. That’s down from the three grand mal seizures per week he was having when he decided to undergo the treatment.
He is grateful to be back at work, and to be able to take part again in cherished activities such as fishing, camping and target shooting.
It did take recovery time to get to where he is today, as is expected with any major surgery.
Jason spent a month in the hospital as surgeons introduced electrodes into his brain to pinpoint the exact origin of his seizures to prepare him for the implantation of his NeuroPace device. He spent an additional month at home recovering from surgery.
Throughout the process, Tiffany said her husband lost about 15 pounds of muscle mass. Physical therapy has helped him regain much of that.
“We knew it would be a long process,” she said, “but I’ve been relatively optimistic from the beginning, helping Jason to assess the risk factors.”
In the end, both Tiffany and Jason believe the surgery was worth it, and want to share their story with others.
“I hope this helps other people,” Jason said. “People need to know that it is better to do something than to have three seizures per week. It’s better to try it than to do nothing if the meds aren’t working.
 /a>
/a>
 /a>
/a>
 /a>
/a>