Michelle Knight convinced herself she had gotten used to the chronic pain that chipped away at her once-athletic lifestyle.
She’d long been a competitive athlete, running in multiple marathons. But by 2011 the pain hit a new level. She had to give up on running.
“It hurt so much,” Knight, 48, said. “I figured it was time to do more cross-training.”
So she switched to biking, swimming and, ultimately, triathlons.
But soon that hurt too much, too.
She gave that up after an Iron Man in 2017.
And somehow, things got even worse.
One day in 2018, halfway through the spin class she taught at a health club, the pain in her hips grew so intense she did the unthinkable: She climbed off the bike.
“I told the class I had to stop, that the pain was unbearable.”
She’d never felt anything like it.
“I had all four of my children without any drugs,” she said. “This was worse.”
Knight turned to orthopedic specialists at Spectrum Health, where an MRI revealed extensive arthritis in both hips.
She asked about joint replacement.
“I had to advocate for myself,” the Grand Haven, Michigan, resident said. “Because I was still in my 40s, that’s young for hip replacement surgery. But I had already tried all the more conservative approaches, including physical therapy.
“It was so bad I began using crutches to walk.”
The pain impacted her work as a hairdresser, which requires long days on her feet. But it also loomed as a major health threat.
“My dad died of a heart attack when he was young, in his early 50s,” she said. “I was 20—and that’s when I started running. I wanted to be healthier. And exercise has helped me achieve that.”
She didn’t want pain to force her into inactivity.
An inside scoop on outpatient
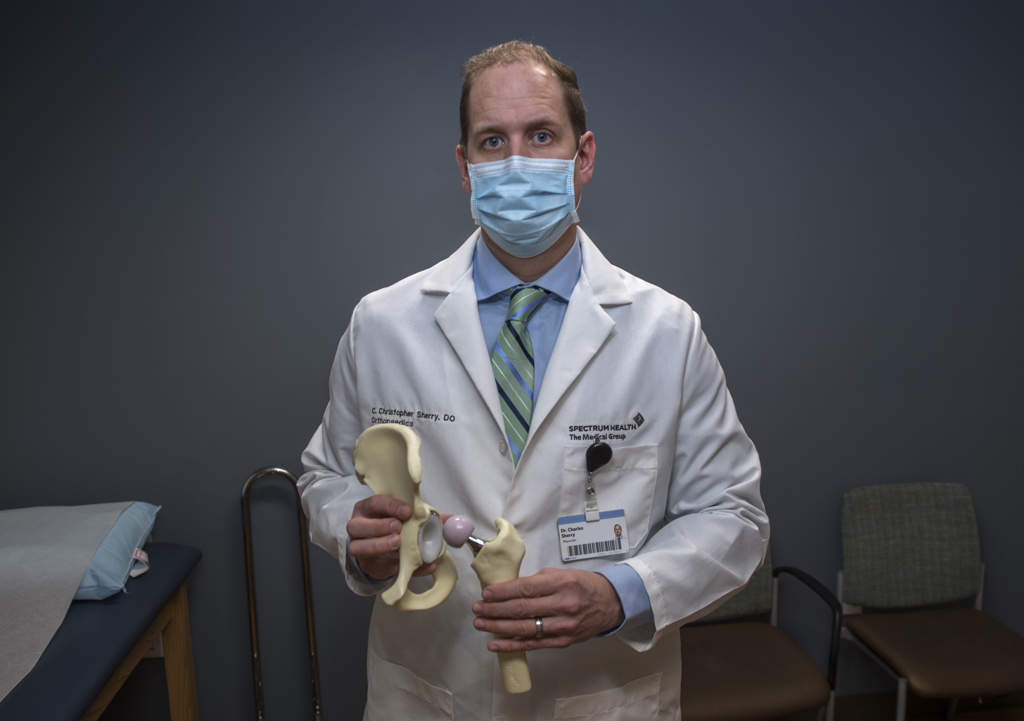
Knight quickly found an ally in C. Christopher Sherry, DO, an orthopedic surgeon at Spectrum Health Orthopedic & Sports Medicine in Grand Rapids.
He’s an expert in joint replacement surgery and he’s also an avid mountain biker and former runner.
“He understood how much working out means to me,” Knight said.
Increasingly, joint replacement makes sense for younger patients, Dr. Sherry said.
“Early on, we knew these replacement joints had a limited life span,” the doctor said.
Often, that meant encouraging younger patients to tough it out until they got older.
But that has changed.
“The technology is better and the new joints last longer,” Dr. Sherry said. “We can now get people back to real quality of life whether they are in their 40s, 50s, 60s or beyond.”
The procedure itself takes about 45 minutes.
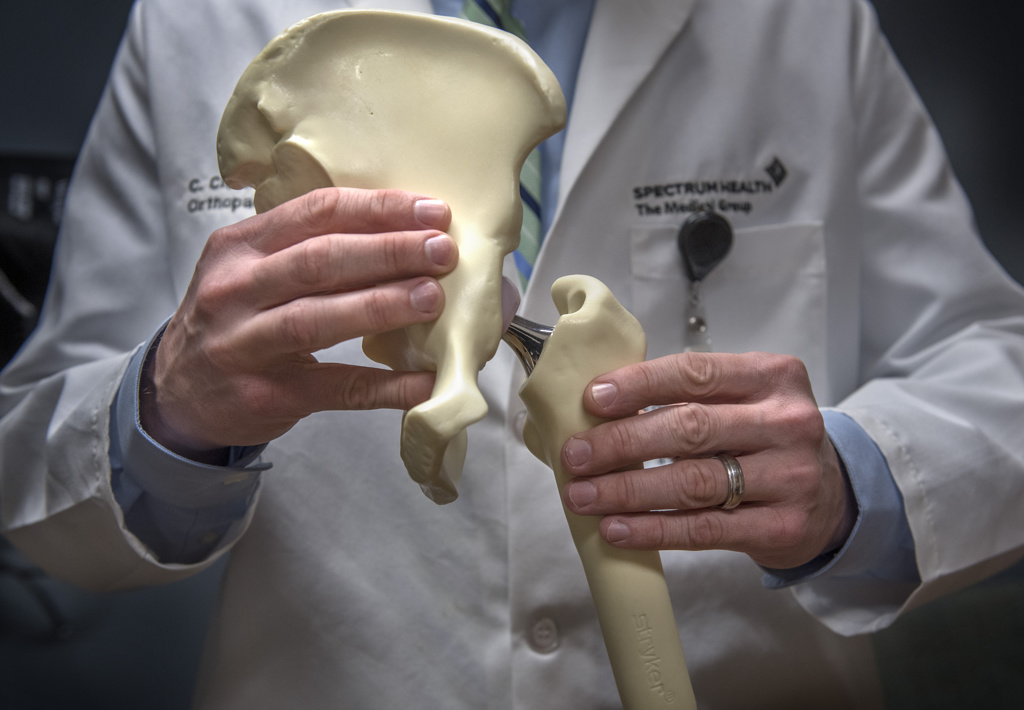
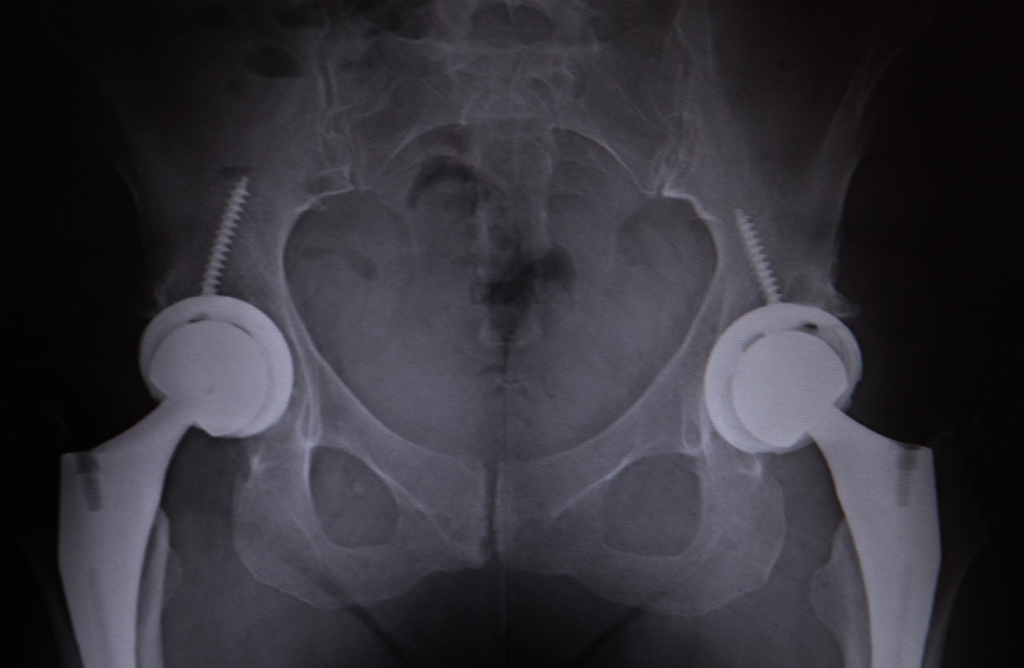
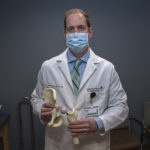
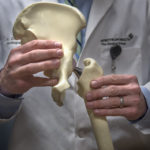
Surgeons remove the thigh bone’s femoral head, which fits in the hip socket, replacing it with a ceramic part. A metal prosthesis is placed inside the femur.
“We also grind down any residual arthritis in that socket, placing a metal and plastic device in there,” Dr. Sherry said. “This ceramic-on-plastic articulation is what forms the new joint.”
With solid evidence that these joints last longer, Dr. Sherry said the focus has shifted to improving the procedure itself, emphasizing outpatient treatment.
“We’ve gotten better at surgical techniques and we’re better at managing pain,” he said.
Typically, the procedure is done in the morning. By afternoon, patients are working with a physical therapist. And they go home that same day. This all lowers the cost.
“And it creates a better overall patient experience,” Dr. Sherry said.
He believes outpatient joint replacement will be chosen for the majority of procedures over the next five years.
Patients with heart, lung or kidney issues may require overnight stays. “And even then, most patients go home the next day,” Dr. Sherry said.
‘I get to have my life back’
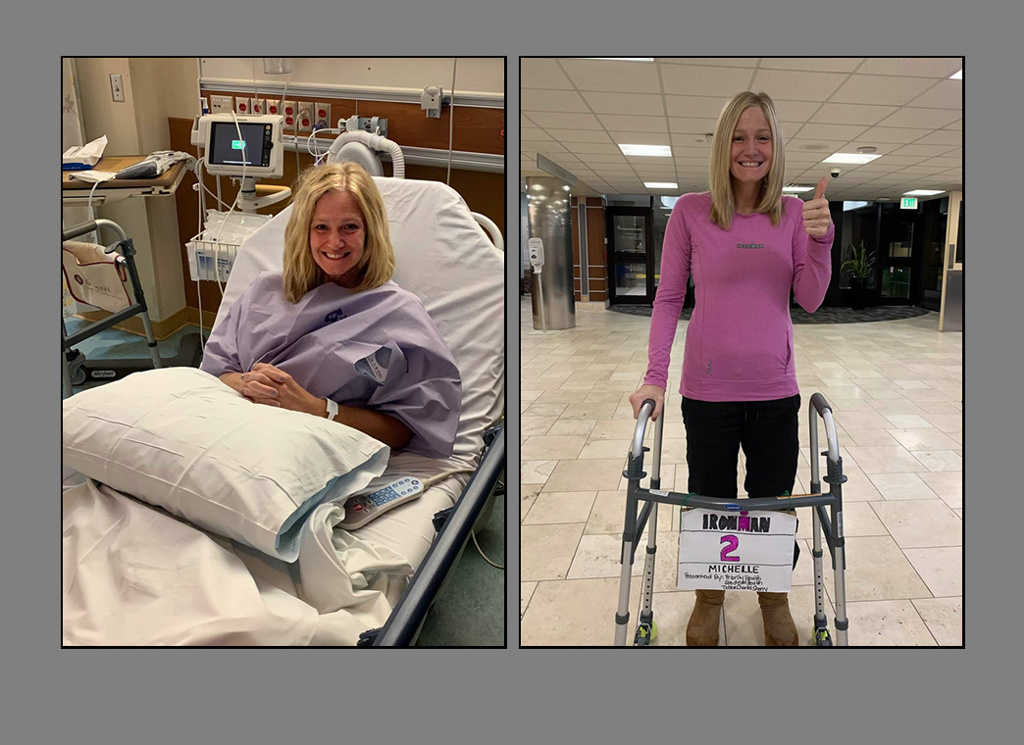
Knight underwent surgery on one hip and felt delighted to return home that same day. She immediately felt less pain.
She quickly began to practice walking and, within a week, found she could walk quite well.
Six weeks later, the doctor performed the procedure on her other hip. She then began physical therapy, which led to increased lengths for walks.
“Pretty soon, I could do a mile. Then two,” Knight said.
She returned to work six weeks later, missing a total of 12 weeks.
She has worked her way back up to 4- and 6-mile trail walks along Lake Michigan. She’s resumed cross-country skiing and plenty of mountain biking.
She hopes to return soon to teaching classes in the spin studio. She’s well aware of the limitations.
“High-impact activities and long distances such as marathons wear out implants sooner,” Dr. Sherry said. “So with younger patients, we encourage them to get back to lower-impact exercises, like swimming and biking. We want people to get their cardio in—they just may have to do it in different ways.”
For Knight, the newfound freedom is deeply meaningful. The experience has made her aware of just how much she lost out on for so many years by denying the extent of the pain.
“I remember thinking at one point, ‘It would be nice to get through the day without taking all this Tylenol,'” she said.
She’s still pinching herself that she gets to exercise now—without all that pain.
“I get to have my life back,” she said.


















 /a>
/a>
 /a>
/a>
 /a>
/a>
Dr. Sherry is great. He did my knee replacement in 2019. Even though I am older (72), I
Am anxiously waiting to get to work in the yard this year!
Thank you, Sherry, for your kind comment. We wish for you a great season of gardening and sunshine!