Diane Peterman tried everything.
She ordered remedies off the internet. She used over-the-counter medications that worked for friends. She visited multiple doctors in Northern Michigan near her Onaway home not far from the Mackinac Bridge.
But nothing could stop the hot flashes, night sweats, sleeplessness, weight gain and lack of energy she suffered during menopause.
“I started menopause three-and-a-half years ago,” Peterman said.
Life hasn’t been the same since.
She averaged 25 hot flashes or night sweats a day. Scalding. Miserable.
“All my friends in menopause said, ‘Try estrogen,’” Peterman said. “When I went on estrogen, the hot flashes disappeared.”
But another issue surfaced: migraine headaches.
She tried cutting the estrogen patch in half for a lower dosage. Migraines continued. She tried a quarter of a patch. Same result.
Peterman, who has worked for over three decades as a school superintendent’s administrative assistant, said the condition messed with her daily life.
“I saw a neurologist,” she said. “He checked for a brain tumor because I had visual migraines, with auras and pressure. They call it vascular migraines. They affect your vision and ability to drive.”
The neurologist ran multiple scans before finally discovering the culprit.
“He asked, ‘Are you by chance on an estrogen patch?’” Peterman said. “I took it off and threw it away. That was no longer an option for me.”
But what was? She needed to find someone who understood her symptoms and could assist.
“I tried cutting all caffeine out and exercising more,” she said. “I have no energy and just don’t feel good. No matter what you do or where you go, you are uncomfortable. I’ve never had anything like this and was so frustrated.”
She increased her exercise. Decreased her calories. Weight loss remained elusive.
“I wear a Fitbit to keep track of my steps, but it also keeps track of how many times you are up in the night and I averaged eight times a night. It gets to the point where I am just exhausted. I just pray my daughters don’t go through this.”
Frustrating. Tiring. But always warm.
“Some days I just hate the way I feel because I’m so sick of burning up and being sweaty,” she said.
Staying cool
In the winter, she keeps her bedroom thermostat at 50 degrees because of night sweats. Her husband piles on the blankets to keep warm.
“My husband (Tom) can look at me and tell,” Peterman said. “You can’t even disguise them. I use cool washcloths on my neck, dress in layers and drink a lot of ice water. I have bought a cooling mattress, cooling mattress pad and cooling pillows. If it said ‘cool,’ I bought it.”
She has spent more than $1,000 in search of a solution. But nothing worked. She knew it. Her husband knew it.
“When a hot flash starts, I go out on the porch in the winter and you can see the steam come off my body,” she said.
Perhaps not only physical steam, but emotional and spiritual steam.
With hope evaporating, and options dwindling, frustration built.
Peterman’s daughter, who lives near Grand Rapids and works at Spectrum Health was aware of unique services in Women’s Health and recommended the Midlife, Menopause and Sexual Health practice.
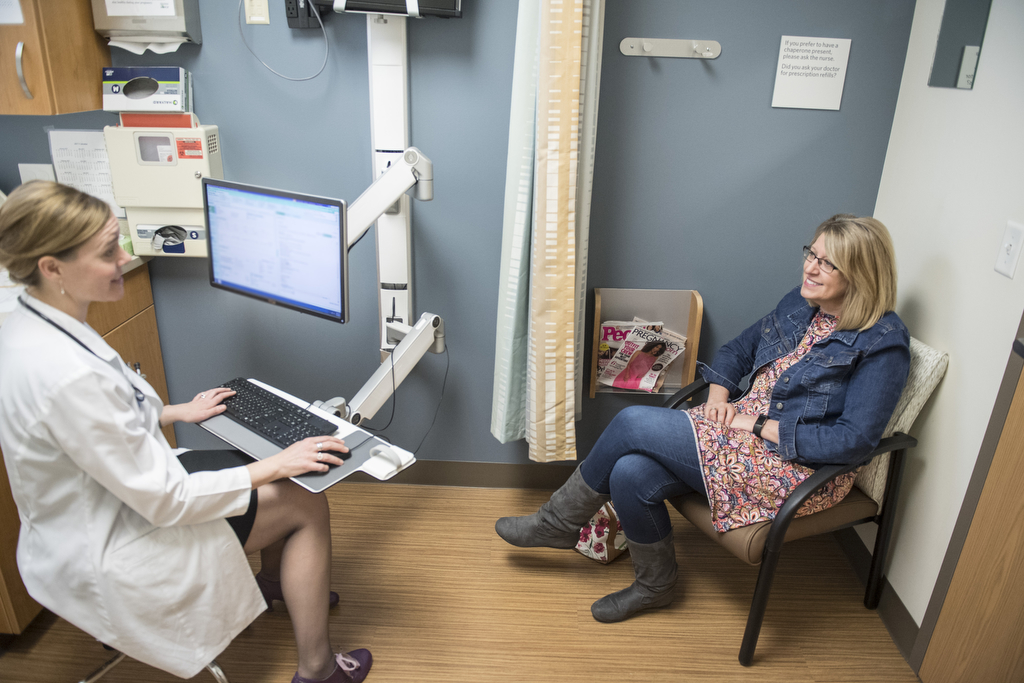
Peterman made an appointment with Natasha Peoples, NP-C, NCMP, a Spectrum Health Medical Group advanced practice provider who is specialty trained and nationally certified in caring for patients with menopause concerns.
“My daughter said you need to see a menopause specialist, your symptoms are extreme and beyond normal,” Peterman said. “My glasses were steaming up my hot flashes were so bad.”
Peterman had her first appointment with Peoples in late December.
Peoples took her off the medication another doctor had prescribed and put her on a new medication that other menopausal women found helpful.
Peterman said her hot flashes have dropped to about half of what she used to have, and she has also lost some weight.
For the first time in a long time, she feels hope.
“I keep a gratitude journal,” Peterman said. “I’ve always been a very positive person, happy and busy. It’s not that I’m depressed. I just don’t have the energy I used to have.”
Her seven grandchildren, with whom she spends as much time as possible, spur her on.
“I want to have energy to keep up with the seven grandchildren without struggling,” she said.
She credits Peoples for leading her on the first steps to improvement. Finally she felt “heard.” After three and a half years of chasing remedies, she’s experiencing her first symptom relief under People’s care.
“She’s a very sweet, compassionate person who is also very knowledgeable,” Peterman said. “Since she is a menopause specialist, this is what she does all day long and she sees every situation. She has already helped me and I’m hopeful she will continue to help me improve so I can get back the quality of life I had before.”
Complicated journeys
Menopause is different for every woman, according to Peoples, but Peterman’s journey has been particularly challenging.
“Diane’s symptoms are somewhat complicated due to the fact that she has hormone-mediated migraines, so hormone therapy is not an option for her,” Peoples said. “It’s not uncommon to experience the most severe and disruptive symptoms in the years just before or after the final menstrual period, as is the case for Diane.”
Making lifestyle changes and switching medications helped Peterman.
“Learning her triggers and patterns for hot flashes has been helpful,” Peoples said. “Being aware of how her daily habits can make a difference is a motivating factor. Her hot flashes have improved.”
Peoples said menopause transition symptoms—hot flashes, night sweats, difficulty sleeping, mood changes, vaginal dryness, decreased libido and irregular bleeding—are like an out-of-control roller coaster ride, “one that we hope to help them navigate.”
While some menopausal symptoms are genetic—think, “How was menopause for my mother?”—other symptoms can be related to lifestyle, according to Peoples.
“They are more severe for women who drink caffeine or don’t drink enough water, for those who don’t exercise and those who smoke,” Peoples said. “Weight gain and poor sleep can both be caused by menopause but also contribute to worsening symptoms.”
For women suffering from severe symptoms, it’s important for them to realize they are not alone.
“We all do it differently, but we all do it,” Peoples said. “Talk to your peers, talk to your provider and come and talk with us. We hope to help empower women to make the transition in a way that maximizes health and minimizes distress and discomfort.”
Take a hard look at your daily habits.
“Drink water, keep a good sleep schedule, exercise regularly, make healthy diet choices—watch out for sugar—and practice meditation or mindfulness,” Peoples said. “All of these choices will make a difference.”


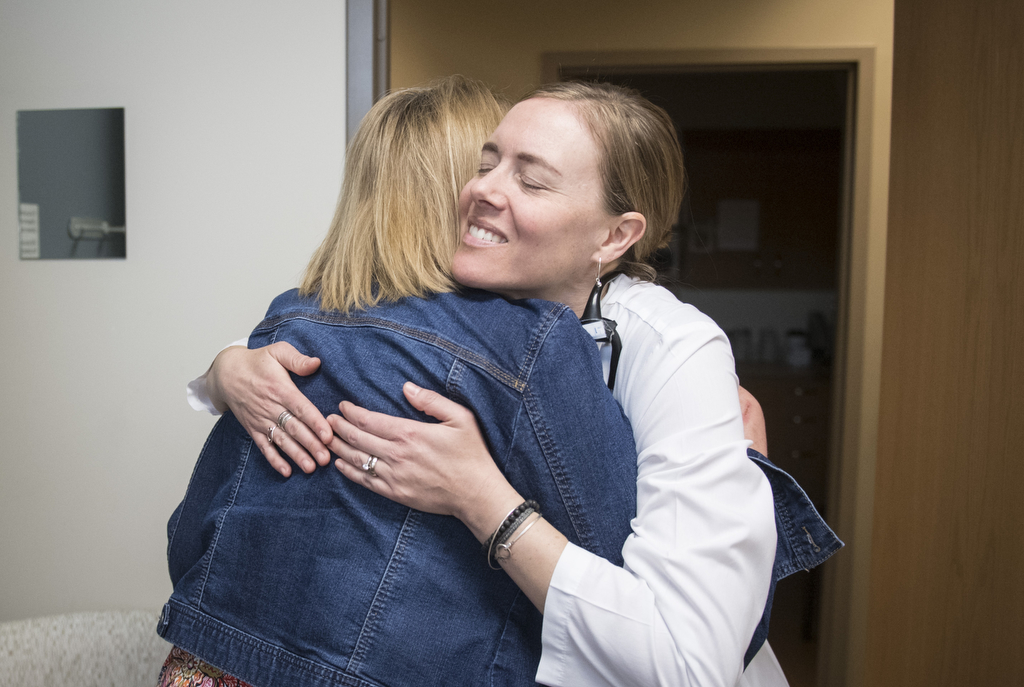


















 /a>
/a>
 /a>
/a>
 /a>
/a>
Diane Peterman is my daughter and I have watched her struggle with this for the past 3 1/2 years and prayed for her everyday. I am so happy she is getting some relief but will be happy when she can be a normal person and enjoy her family and keep up with the grandchildren. She is a very positive person and believes her faith in God will lead her in the right direction for the help she needs. Thank you to Dr. Natasha Peoples who believes in her and giving
her the help she needs.
Oh my goodness, I have those same symptoms and I live in North Carolina . Can you suggest a Doctor in the area. The night sweats are the worst.
Hello and thank you for being a Health Beat reader. If you live that far out of state, you may want to check the NAMS database to find an certified expert in menopause – https://www.menopause.org/for-women/find-a-menopause-practitioner Best of luck to you!
Do you also offer solutions for those of us who have hot flashes due to Tamoxifen? Effexor had too many side effects
Hi Deb – Yes, Spectrum Health’s team of women’s health experts have an in-depth understanding of how the side effects of cancer treatment can sometimes induce early menopause symptoms. Part of their clinic focuses on this issue. To schedule an appointment, call 616.267.8520. Best wishes to you, Deb.
Also, you may be interested in this story about the Spectrum Health Cancer Menopause and Sexual Health Survivorship Clinic – https://healthbeat.corewellhealth.org/life-after-fallopian-tube-cancer-melon-tumors-ovaries-puppy-love/
What a wonderful coincidence to see Diane featured in an uplifting article. We (my wife, Betty, retired from teaching in Onaway) remember Diane as a most positive and caring individual. So, to read about her health issue struggles and to see her positive results, it warms our hearts for she truly deserves this! We hope that her positive results will continue and ultimately provide the complete relief she is seeking.
Do you look at natural remedies? I have been able to keep the hot flashes at bay for the most part though my family says the house is cold all the time while I am comfortable. But the weight gain is making me crazy and I have issues with sleep as well.
Do you have anyone who specialises in POI / POF?
Hi Lisa, Thanks for reaching out. We highly recommend you consult with an expert within our women’s health team. To learn more or to schedule an appointment with the Spectrum Health Midlife, Menopause & Sexual Health team, call 616.267.8520. They’ll be able to connect you with a doctor who will meet your needs. Best wishes to you.
I was put on the hormone patch for post menopausal symptoms. It was very helpful for hot flashes, but I have noticed an increase in migraine headaches that I hadn’t associated with the patch until this article. I am currently weaning off the patch for other reasons. Now I am hopeful the headaches will subside too.
Hi Theresa, We’re so glad you found this Health Beat article helpful. We sure do hope your headaches get better. If that doesn’t do the trick, definitely connect with your physician for help. Best wishes, Cheryl
I have been a patient of Natasha Peoples and really appreciate everything she has done for me. I didn’t have the hot flashes problem to the extent that Diane had but experienced the loss of energy and unexplained rashes. Natasha is very knowledgeable and personable and treats the whole person, not concentrating on a single symptom as some medical professionals may do.
So glad you had such an awesome experience with Natasha, Mary. Thank you for sharing, and may you have a blessed 2019. 🙂 Cheers, Cheryl
…i’m almost 10 years into medically forced menopause from cancer, I can’t take any hormone replacements due to other medical condition. Every doctor I see or have seen don’t seem to have a solution and its become a chronic issue for me. Affecting my life on every level…I would love to meet a medical professional that might be able to help
This article was amazing to read. I have been dealing with God-awful hot flashes and night sweats for almost 3 years now and NOTHING seems to help! I will be contacting Dr. Peoples!!!
Hope you get the relief you seek, Amy! Best wishes to you!
Went through hot flashes at night and servere sweats and during the day also. I was taking vitamin d to much of it. Side effect of vitamin d servere sweats and hot flashes. My dr. Could not find the problem. I did. After off of vit. D in 4 days it went away
I was on estrogen and progesterone therapy for about ten years – until diagnosed with hormone positive breast cancer. As soon as I stopped taking those 2 hormones, I could also stop taking my daily and “as needed” migraine medications. I also stopped taking Prilosec! So I went from 5 medications to none. I feel that my ob/gyn doc was not monitoring my use of the hormones closely enough. I was just the “next patient” who received 15 minutes of time annually. The hormones were prescribed to alleviate hot flashes.
So glad you’re doing well today, Doria.