On a frigid morning in January 2022, four members of the DeWind family—mother, daughter, granddaughter and nephew—climbed into their Chevy Suburban for a short drive to visit a relative.
As they crossed a small bridge on M-45 outside Allendale, Michigan, the vehicle hit black ice and spun out across the center line.
“I remember my daughter saying, ‘Mom, I’m losing it, I’m losing it, what should I do?’” said Kim DeWind, 54, of Zeeland, who rode in the passenger seat beside her daughter, the oldest of five adult children.
She told the kids in the back seat to hold on tight.
“I remember seeing the pickup come over the hill. And I thought, ‘We’re going to get it bad.’”
Indeed they did.
The truck and SUV collided. Three of the SUV’s occupants were injured, two of them critically.
Kim and her 6-year-old granddaughter took the worst of the impact, each sustaining crushing injuries on the right side.
When Kim’s husband, Jeff, arrived on the scene from his workplace up the road, he grasped the gravity of the situation in a heartbeat.
“My daughter’s a nurse … and she had her daughter, my granddaughter Nora, in her lap. And she said, ‘Dad, I think she’s dying—and I think Mom may already be gone by now,’” Jeff said.
“I did 16 years on my local fire department as a first responder, and I’ve seen a lot,” he said. “I didn’t hold a lot of hope out that either would survive, standing there on the edge of the road.”
Level 1 trauma
A pair of ambulances transported Nora and Kim to the Level 1 Trauma Center at Spectrum Health Butterworth Hospital. Pediatric trauma specialists received Nora and admitted her to Spectrum Health Helen DeVos Children’s Hospital.
Meanwhile, the trauma team assembled to await Kim’s arrival in the trauma bay.
The team’s initial assessment looked grim: She had low oxygen levels, an elevated heart rate, poor blood pressure, bad coloring.
Doctors immediately began basic lifesaving interventions: a chest tube to drain fluid from the chest cavity; intubation to open her airway; a central line for administering blood, fluids and medication; and an arterial line to monitor her unstable blood pressure.
Inserting the chest tube presented a special challenge because Kim’s ribcage had suffered grave damage.
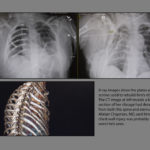
As soon as she seemed stable enough, doctors took Kim for a CT scan to determine the extent of her injuries. Imaging revealed multiple severe traumas, including one of the most dangerous possible issues: a tear in her main blood vessel, the aorta.
“This is a potentially devastating injury,” said Alistair Chapman, MD, an acute care surgeon on Kim’s care team.
“The vast majority of trauma patients that have an aortic injury do not make it to the hospital alive.”
The torn aorta instantly became priority one. With Kim still in the CT scanner, the trauma doctors began alerting their consultants, starting with the on-call vascular surgeon.
As the team moved Kim to the surgical ICU in preparation for an aorta repair, Gaby Iskander, MD, division chief of acute care surgery, ducked out to meet Jeff, who had arrived in the ER to await news of his wife and granddaughter.
“He gave me a quick rundown—that they saw a tear in the aorta and that they were going to try to put a patch on that and that he needed to get moving,” Jeff said.
“So I just signed my name and said, ‘Yeah.’ He said, ‘Do you have any questions?’ I said, ‘No, I’m good—go.’”
Cardiac arrest
Up in the ICU, as Kim’s doctors discussed their plan for addressing her full roster of injuries, they faced a new crisis: cardiac arrest.
Kim’s heart stopped, right there in the surgical ICU.
The nursing team began chest compressions as the two lead surgeons scrambled to see if they could identify the cause of the arrest.
After several minutes of intense effort, including the insertion of a second chest tube, Kim’s pulse returned, and the team breathed a collective sigh of relief.
The intensity of that moment has stayed with him, Dr. Iskander said.
“The fact that her heart stopped—it just took a toll on me,” he said.
“We get so attached to our patients, especially in the ICU and in trauma. … You don’t want anything bad to happen to them.”
Though far from stable, Kim needed to go straight to surgery.
As they rolled her down to the operating room, Jeff had a brief chance to see his wife. A medical social worker met him in the waiting room and ushered him down the hall to see her off to surgery.
“I knew a torn aorta was a really bad sign,” Jeff said. “I figured we were probably at the end.”
For the next couple of hours, the vascular surgeon, with the support of a skilled trauma and anesthesiology team, worked to stent her torn aorta.
After the successful procedure, Kim came under the care of the ICU team and Jeff was able to see her again—alive, though still touch and go.
All the while, Jeff kept in close touch with his daughter, watching over little Nora at the children’s hospital next door.
Though “she wasn’t out of the woods yet that first 24 hours,” Nora ended up leaving the hospital eight days later, he said, and has recovered well. She’ll have a follow-up surgery in July to remove the hardware in her leg.
Chest wall repair
The next morning—hospital day two—Kim’s vitals and lab work looked good enough that the team felt comfortable sending her for her next surgery, to repair a broken humerus.
With that taken care of, doctors prepped for the next day’s surgery—her chest wall reconstruction and diaphragm repair.
For that kind of work, Dr. Chapman is the hospital’s go-to surgeon.
“I spent a couple of days examining her CT scans, thinking about how I’m going to approach this once she’s stable enough to undergo a really long operation,” Dr. Chapman said.
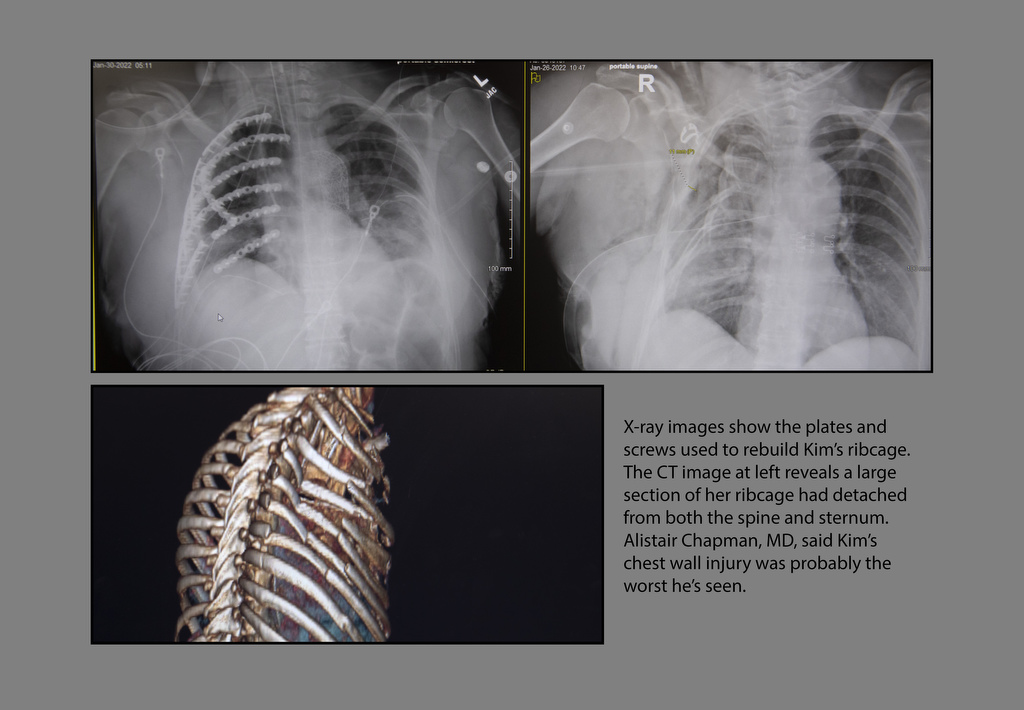
Kim’s chest wall injury was probably the worst he’s seen.
“Her chest cavity was basically crushed, and the ribs that are supposed to be on the outside of the chest were almost adjacent to the heart, in the center of the chest,” he said.
Kim had what doctors call flail chest, meaning a large section of her ribcage had detached from both the spine and sternum.
“The entire right side of her chest wall was not contributing to her work of breathing,” Dr. Chapman said.
In total, Dr. Chapman fixed 15 fractures using 12 titanium plates and 94 screws—the most hardware he’s ever used in a chest wall repair.
By now, just two days after the car crash, the major surgeries were over and Kim’s care team could take stock of her additional injuries—including trauma to the mid and lower spine, a lung laceration, liver laceration, shoulder blade fracture, collarbone fracture and vertebral artery injury.
All of these, they determined, could be treated non-surgically as she rested in an induced coma, fighting a fever, attached to a ventilator.
Strength to fight
The big question looming in the background had to do with Kim’s neurologic function. An early MRI of her brain showed that she’d suffered multiple strokes, likely from the disruption of blood flow caused by her aortic injury.
When her neuro exams remained poor on hospital day six, the ICU team placed a tracheostomy in her neck, knowing that would make it easier for her to eventually come off the ventilator.
They also inserted a feeding tube to deliver nutrition into her digestive tract.
As the ICU team monitored her around the clock, Kim’s family, church and community prayed.
Around day eight, Kim remembers hearing her daughter’s voice.
“I don’t think I was awake … but I remember these words, and she just said, ‘Mom, if it’s too much, we understand and we can let you go.’ She said, ‘Mom, do you even want to fight? Do you have the strength to fight?’”
And Kim nodded very gently—her first bit of communication since arriving at the hospital.
“I remember that, so that’s pretty cool,” Kim said. “I knew I was in bad shape, but I just made a decision that I was going to fight with all I got because I wanted to live.”
Fight she did, with seemingly miraculous results.
The next day, Kim could nod her head. The day after, she opened her eyes and became more responsive. She recognized family members and spelled out words by pointing at a letterboard.
Before long, she came off the ventilator, then the feeding tube.
“Every day was super substantial, noticeably better,” Jeff said.
On day 13, Kim moved out of the ICU. Just two days later, she discharged to Mary Free Bed Rehabilitation Hospital, where she spent two weeks in acute rehab before going home.
“To see how incredibly far she’d come in four weeks was just, you know—the miracles don’t seem to end. She survived the aortic tear. That’s so rare. She didn’t have brain damage through all that—that’s, I think, also really rare,” Jeff said.
“And then the fact that she’s only at Spectrum for 15 days and then another 14 at Mary Free Bed—all those things are just incredible to me.”
Jeff isn’t alone in his astonishment. Kim’s doctors, too, expressed awe at her survival and recovery.
“Given all her injuries and given how her injuries looked, it’s just a miracle that she’s alive,” Dr. Iskander said.
She overcame staggering odds to survive this event, echoed Dr. Chapman.
“An aortic injury—the chance of surviving that injury is less than 1%,” he said. “And then the chance of surviving a blunt cardiac arrest is also less than 1%.”
Much of the credit goes to his colleagues on the trauma and ICU teams, he said.
“When you think about having a highly functioning trauma system, there are a lot of elements to maintaining that,” Dr. Chapman said.
“It’s just cool to see it play out for a patient in the way it did for her.”
‘An amazing moment’
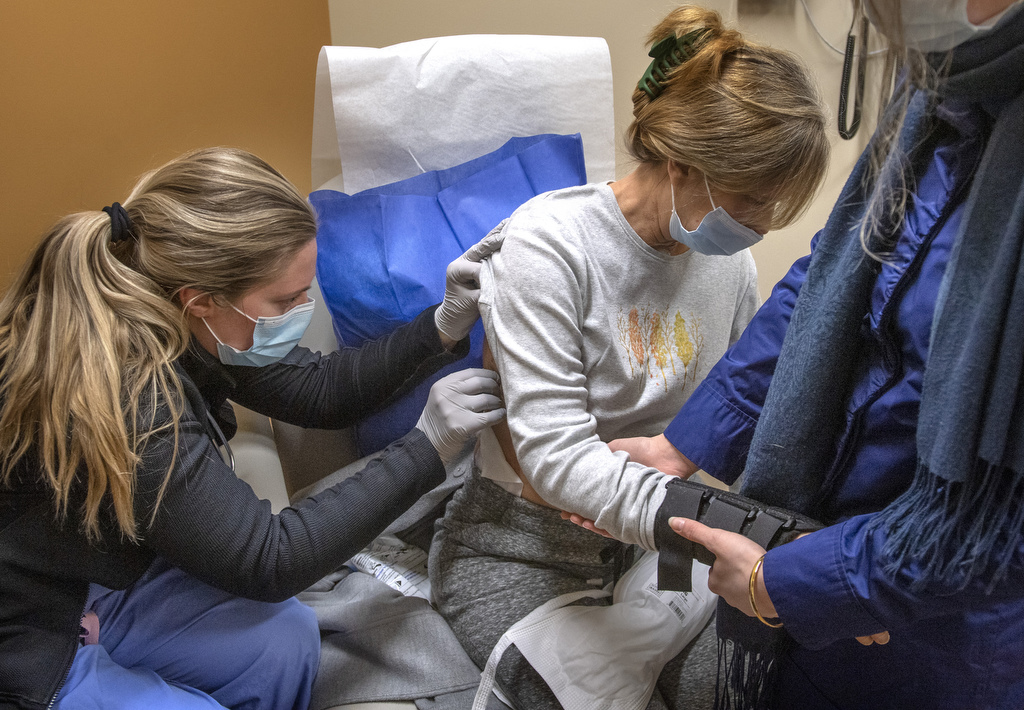
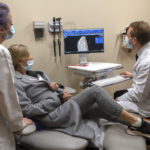
When Kim came back to Butterworth Hospital for her first appointment at the Spectrum Health Multidisciplinary Trauma Clinic, several of her doctors made a point of stopping by to see her.
“It was a huge joy … to see somebody that was badly injured go back to their family, go back to their granddaughter, go back to their daughter and be able to enjoy this—enjoy their family, and their family enjoy them,” Dr. Iskander said.
“I still get emotional every time I think about this patient.”
For the DeWinds, the reunion was equally meaningful.
“You could just sense this emotion in the room, from all of us,” Kim said. “It was an amazing moment.”
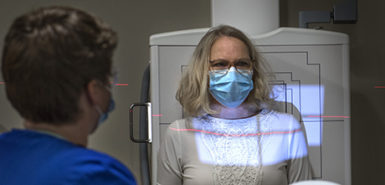
Back at home, Kim continues a long process of physical and occupational therapy to regain strength and function throughout her upper body.
Day by day, week by week, she can see progress.
“I’m surprised how tired I am. But I’m doing more than a week ago,” she said. “I’m gaining.”
She hopes to eventually get back to the part-time job she loved, working in a small family restaurant, where the regulars have become friends.
But even if she goes back to work, she doesn’t plan to fill her calendar the way she used to.
“We want to clear our plate and enjoy life,” Kim said. “I’m going to live life a little fuller,” treasuring her six grandchildren and the other loved ones who almost lost her.
The whole experience remains overwhelming for her.
“In a good way,” Kim said.
“Oh man, I appreciate things so much.”














 /a>
/a>
 /a>
/a>
 /a>
/a>
Hip hip hooray for the teams!!!
Haleighluia for Kim and family and friends!!
AND OH! MY GOD!!!!
Kim is a true miracle of God today. So many people around this state were lifting her up in prayer and God heard our prayers and put her under the best care possible to accomplish her miraculous recovery! Praising God for hearing our prayers!
Kim,
Reading your story just gave me goose bumps. What a God we serve. It is obvious God has big plans for your life and the life of your family. Your will to live is just nothing short of amazing. I know you have the support of your family because I know your mom and dad. They have been friends for many years. As a matter of fact I used to baby sit you and your sister Lori. I have fond memories of all of you. You will be in my prayers as I know your journey will be difficult. I hope you feel the power of prayer of people that don’t even know you and your family. May God continue to bless and hold you in the palm of his hand.
Jeff is my cousin and we were all praying for Kim.
Brings tears to my eyes reading this account of events.
I was with Kim and Jeff two weeks ago and she has made remarkable progress.
Thanks for sharing the Miracle!
Wow….what an amazing story of love, hope, endurance, & healing. Praise The Lord!😘🙏🏻✝️👏
As one of the many who prayed for Kim and her granddaughter, it’s so beautiful to hear the rest of the story. May God’s blessings continue to cover them!
Amazing and miraculous story! Prayers were ascending immediately and continued every day from Arkansas ! Being a ER and surgical nurse for many nurse ……I’m in awe of your miraculous recovery, of the trauma and surgical team you had , and your determination, Kim! We serve an amazing God! He is not finished with you here in earth…. I still continue to pray for you , Nora, Adien and Megan! May He continue to bless all of you!
I’m good friends of the Hosteters ! They are like family !
We watch Chicago Med and this story about Kim was just like one of their shows!!
It is an amazing story of Faith, determination, skilled doctors, loving family and excellent care!!!
What an amazing story of recovery! I am so thankful for Kim and her family–that is quite something to overcome. I am also so thankful to read this as a Surgical ICU team member. We often don’t get to see the continued recovery of our patients once the transition out of ICU happens. Makes me proud to be on the team of these expert and skilled colleagues!
Michele,
I just read your comment to the story posted in spectrum health publication about my accident the end of January.. we’re you one of the nurses that helped with my care? I do wish I could give some “ thank you’s” to all the staff who helped me & our family
Your story is inspiring Kim and bring courage to those who sometimes lose sight of the God who answers prayer and gives good gifts every day. Thank you
I’m Dave Woods’ dad, therefore am related to Jeff, and testify to the miracle of KIm’s recovery, How great is our God! Nothing is too difficult for Him. Kim’s story is exhibit A.
Jeff is my cousin and we were all earnestly praying. So exciting to read this story and get the details. God truly is amazing!
Thank-you so much for this article. What a journey. The love and support that surrounds these survivors is powerful. The healing work folks do out in the world is sooooo meaningful. The science that helps the professionals heal. The skills. The dedication. You are all so loved. The Felsk Family prays for you all. May you have peace and healing on the rest of this journey.
What an amazing story and testament to God and the power of prayer! I worked in the ER at Spectrum Butterworth for 25 years. I was riveted to your story. Thank you for sharing.
Makes my heart happy to see you out living your life Kim! What an amazing recovery you made- keep up the hard work and enjoy every moment ❤️
My wife was diagnosed with acute myeloid leukemia 6 years ago and was treated by Butterworth’s cancer center. She has been cancer free for five years now. Just another of our Doctors and the wonderful facilities we have in “our Town.” Hooray for what they have accomplished!
Truly a miracle! What an awesome God who holds us all in His hands!