Here are a few things 2-year-old Jada Elenbaas has never done: played with other children, gone to the grocery store or eaten in a restaurant.
But none of that compares with what she has done: Live and thrive without an immune system. Become the first child in Michigan to survive a thymus transplant.
And, of course, charm and delight her mom, dad and big brother.
The tiny girl with blond hair and deep blue eyes has lived her life in a bubble since a newborn screening test revealed she has an extremely rare condition called complete DiGeorge syndrome.
Only about 20 children are born in the U.S. each year with the condition. Most die before their second birthday, because they lack the ability to fight off infections.
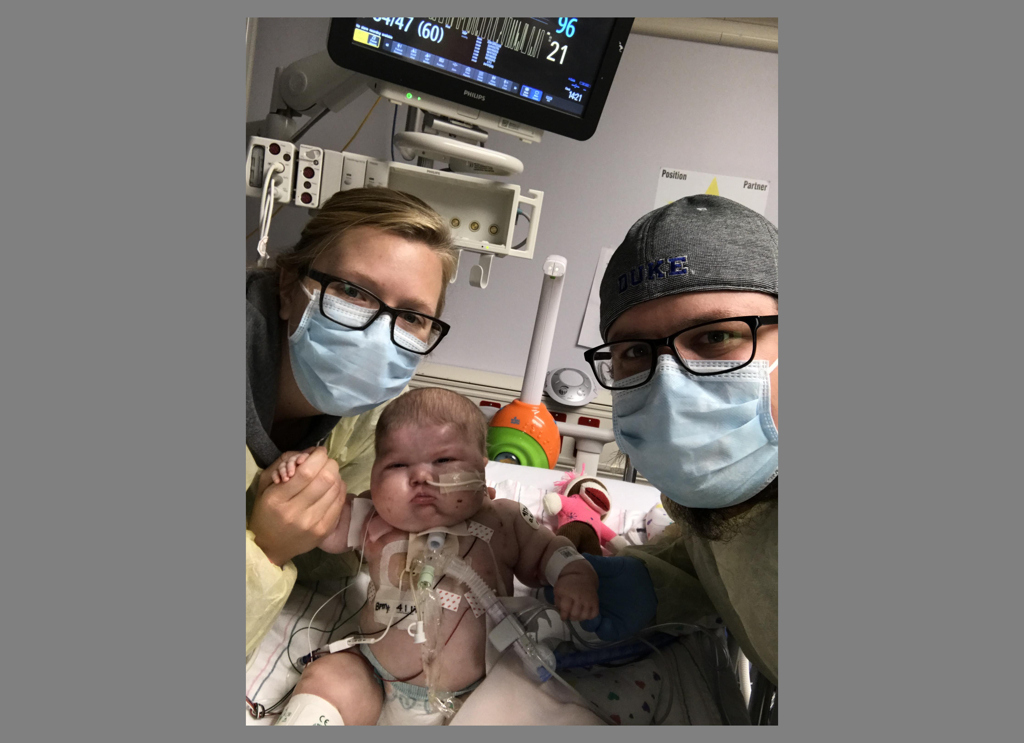
But Jada’s parents, Mike and Amanda Elenbaas, pin their hopes on a healthy future for their daughter, aided by new treatments, a team of medical specialists and vigilant care.
And there is Jada herself.
“She has always been feisty,” said her mom, Amanda Elenbaas. “I think that is what has gotten her through what she has (endured). She is a little miracle, that’s for sure.”
‘Terrifying’ news
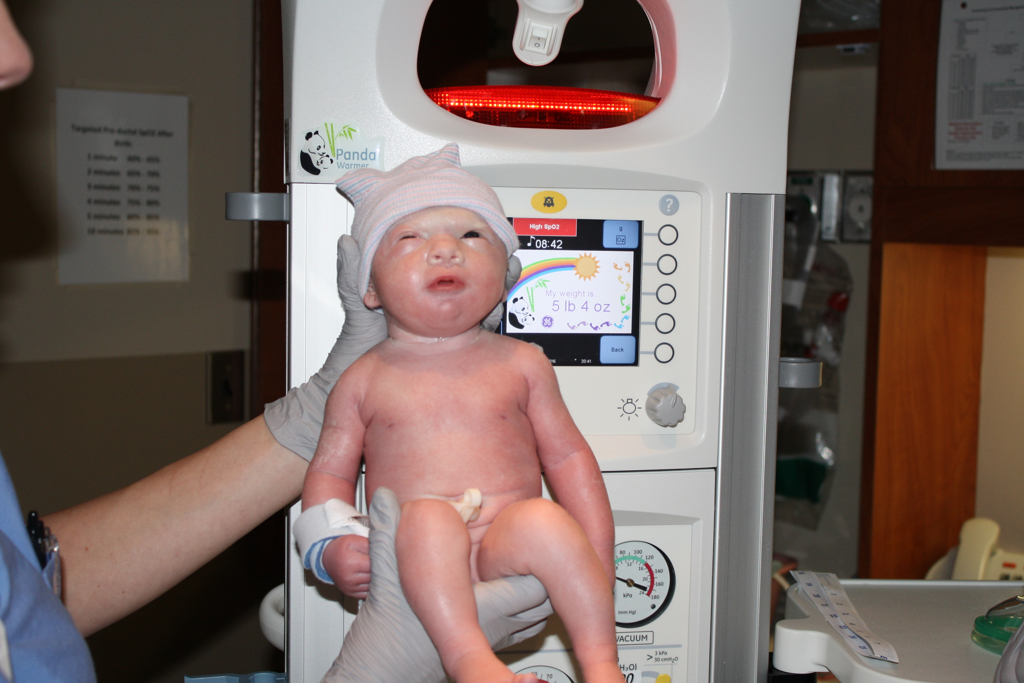
Born six weeks early, Jada spent her first days in the neonatal intensive care unit at Spectrum Health Helen DeVos Children’s Hospital. She weighed more than 5 pounds and appeared healthy, despite her early birth. Mike and Amanda, who had an 18-month-old son, Odyn, were eager to take her home.
Jada was 1 week old when they learned the results of the newborn screening test, which checks for genetic conditions. It showed she lacked T-cells, the white blood cells that combat infection.
Further testing identified the cause as complete DiGeorge syndrome, a condition that occurs when a child is born without a thymus. The gland plays a crucial role in a child’s immune system. It develops immature white blood cells produced by the bone marrow into T-cells, which fight off infection.
“But she was born with a defect that didn’t allow her thymus to develop, so all her T-cells couldn’t develop,” said Nicholas Hartog, MD, a pediatric immunologist.
Long-term survival would require a new treatment: a thymus transplant, available at only two hospitals in the world—and just one in the U.S.
In the meantime, protecting her from infections became the challenge.
“Any common cold virus could be deadly for her,” Dr. Hartog said.
Amanda and Mike reeled with the news.
“It was terrifying,” Amanda said. “I just remember holding Jada and crying.
Her parents have been absolutely fantastic in doing everything they do to keep her alive.
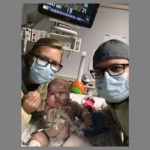
Isolation precautions began immediately. Mike and Amanda donned gowns, gloves and face masks every time they entered their daughter’s room in the NICU.
Jada came home from the hospital at 6 weeks, with a feeding tube and an extensive list of medications. But her stay didn’t last long.
In a few weeks, she caught a parainfluenza virus—a bug that causes sniffles or a sore throat in most kids.
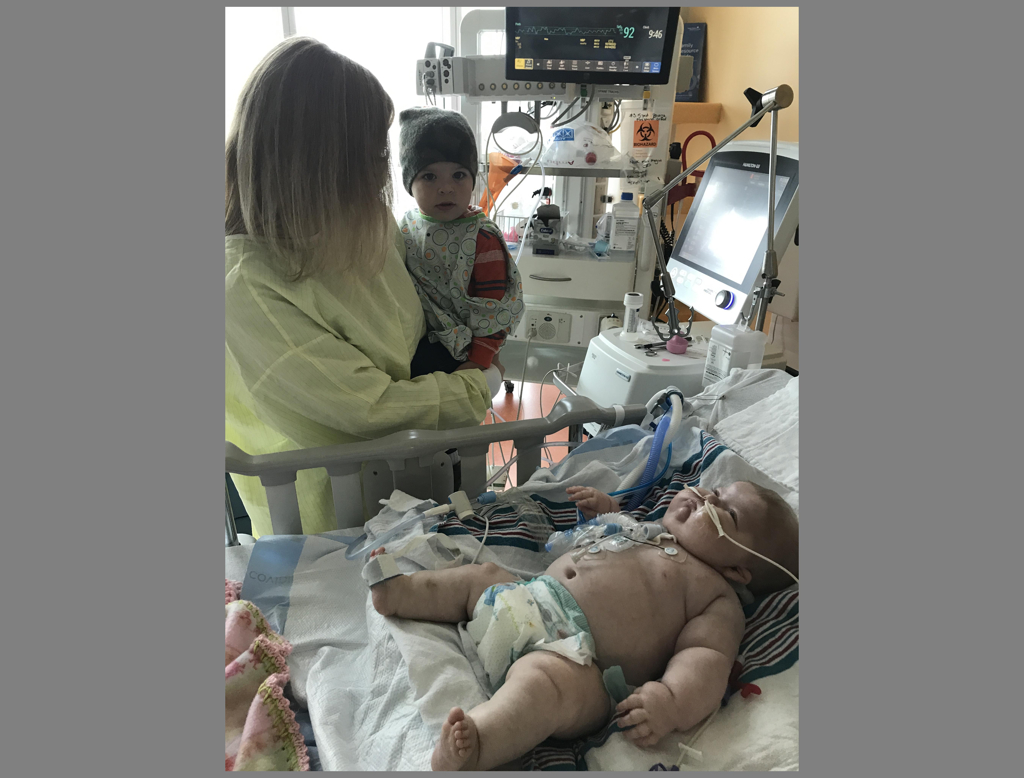
Jada almost died. She had a tracheotomy. She remained on a ventilator for over a year.
For most of the next 10 months, she remained in the hospital as doctors helped her fight the infection with a combination of medicines that included experimental antiviral drugs.
A thymus transplant
Meanwhile, Jada’s parents and her medical team prepared for a thymus transplant. She was 7 months old when a medical flight carried Jada and Amanda to Duke Children’s Hospital in Durham, North Carolina. Mike drove down to meet them.
At Duke, pediatric immunologist Mary Louise Markert, MD, has pioneered a surgery to transplant donated thymus tissue into children with DiGeorge syndrome.
The thymus sits on top of the heart. And when a child undergoes heart surgery, sometimes the surgeon must remove parts of the gland to operate. With the parents’ consent, that tissue can be used for a transplant.
On April, 4, 2017, the doctor implanted donated thymus tissue into Jada’s thigh.
A month later, the Elenbaas family returned to Grand Rapids. And their wait began. Would the transplant work? Would Jada’s T-cells begin to form?
For 18 long months, the answer was, “Not yet.”
Making life fun
In the meantime, Mike and Amanda maintained constant vigilance over Jada’s fragile immune system. To do that, they made big life changes.
They sold their house in Holland, Michigan, and bought one next door to Amanda’s parents in Hudsonville.
Amanda quit her job as a dental hygienist. She stays home most of the time. No visitors are allowed in the house, not even grandparents.
Four-year-old Odyn does not go to preschool or play dates. Instead, his mom home-schools him. He visits his grandparents next door.
Although Mike continues to work outside the home as a mechanical engineer, his co-workers understand the steps he takes to prevent contact with germs: frequent use of hand sanitizer and disinfectants and a rule against handshakes.
“It’s a crazy life,” Amanda said. “We don’t go on any dates. We kind of made our home our life.”
But within that protective bubble, Mike and Amanda have created a warm and engaging family life.
They play games, read books and watch movies. On nice days, they take walks. They spend time on the deck Mike built.
In summer, they watch movies outdoors and enjoy backyard fires. They share a fenced backyard with Amanda’s parents, and can visit with them in the yard.
On chilly winter days, they bundle up the kids for sled rides around the block.
Finally, we have a light at the end of the tunnel.
And they take field trips—always to places where they won’t encounter other people. Watching planes take off and land from the park at the Gerald R. Ford International Airport is a treat. They go to an isolated spot at the beach so Odyn can swim in Lake Michigan.
“Open air is very safe,” said Rosemary Olivero, MD, a pediatric infectious disease specialist. “We are concerned most about close exposures. In the open air, if somebody coughs, it floats off in the environment.”
To help her stay healthy, Jada takes a host of medications: to ward off bacteria, fungal infections, viruses and parasites. She receives shots of pooled antibodies, donated by plasma donors. She does not receive vaccines because her body can’t respond to them.
She still has a feeding tube. And although she still has a tracheotomy, she no longer needs a ventilator. She receives CPAP, continuous positive airway assistance, only at at night.
“She’s been out of the hospital for a year and a half, which is no small miracle,” Dr. Hartog said. “Her parents have been absolutely fantastic in doing everything they do to keep her alive.”
Early morning appointments
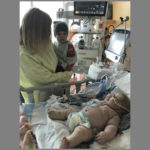
Overseeing Jada’s care is a team of pediatric specialists, who take great pains to minimize her exposure even to doctors and nurses. When she has an appointment for blood work, tests or a doctor’s visit, Jada sees as few people as possible. Dr. Hartog and Dr. Olivero typically are the only physicians she sees; the others rely on reports from them and test results.
And for Dr. Hartog, a visit with Jada is a joy.
“She’s adorable,” he said. “She’s super cute.”
For a recent visit with him, the Elenbaases arrived at 7 a.m., before any other scheduled patient visits. They pulled up in front of the Helen DeVos Children’s Hospital Outpatient Center and carried Jada across the lobby in a car seat with a cover draped over her.
“We wipe down the exam room with alcohol three or four times before she comes in to make sure there is no contamination in the room,” Dr. Hartog said.
Anyone treating Jada wears a gown, gloves and face mask.
“I never see her if I have had a whiff of illness in my household,” Dr. Olivero said. “If my child had an illness or my husband was sick in the past few days—no way. If any of us is feeling at all sick, we don’t even go there.”
At last, a hopeful sign
After a thymus transplant, T-cells usually appear within in about six months to a year, Dr. Hartog said. Sometimes it can take much longer.
But still, as the months went on and test after test showed no sign of T-cells, Mike and Amanda began to worry. With their doctors, they began to make preparations for a possible second thymus transplant.
Shortly before Christmas 2018, Amanda got a call from Dr. Hartog.
“I want to give you some good news,” he said.
At last, Jada had T-cells. Her count of 186 was low—a healthy person has 500-1,500.
“But two months ago, she didn’t have any. To have 186 is pretty good,” Amanda said. “It’s such a relief that things are finally starting.”
Complete DiGeorge syndrome often affects other systems, besides the immune system.
Jada has some delays in motor development and kidney issues. And she has a congenital heart defect—a hole in the wall between her heart’s upper chambers.
“It will probably need to be repaired at some point, but it’s not causing a ton of trouble,” Dr. Hartog said.
But for now, her biggest challenge is to build an immune system, and in that, she is making progress.
“Finally, we have a light at the end of the tunnel,” Amanda said.
Just to reach this point is a victory.
‘The boy in the bubble’
In the past, parents and doctors didn’t know an infant had complete DiGeorge syndrome until a first infection, which often proved fatal. Doctors hope a growing awareness of genetic disorders that cause immune deficiency will help more children like Jada.
Including severe combined immunodeficiency disorder to the newborn screening panel is a step in that direction. Michigan added it in 2012 and by December 2018, all 50 states included it.
That’s the disorder that affected David Vetter, a child known as the “boy in the bubble” in the 1970s and ’80s. He died at age 12 in 1984.
The disorder, like Jada’s diagnosis, involves a lack of T-cells, so the screening panel alerted Jada’s caregivers to her rare condition.
Since 2012, Jada is just the third child in Michigan diagnosed with complete DiGeorge syndrome.
Of all the factors that have brought her this far, Dr. Hartog gives special credit to the steadfast devotion of her parents.
“Amanda and Mike are fantastic,” he said. “They do everything we ask of them and then some.”
“They are wonderful people,” agreed Dr. Olivero. “Without them, she wouldn’t have made it.”



































 /a>
/a>
 /a>
/a>
 /a>
/a>
Praising God for Jada!
She is Blessed with Loving Parents, a Way Cool Brother & Sweet Grandparents!❤❤❤❤
So true. And Jada is a blessing to all who meet her, as well.
Thank you so much for sharing Jada’s life💕🙏🙏we never know what God’s plan is in all of this, she is making history and maybe saving lives. May God Bless you all! You are all in this together with friends that also care even if we can’t be with her. Prayer is a powerful gift.🙏🙏🙏🙏🙏🙏💕💕💕💕
Praying for a successful transplant. Best of luck!
What a testimony How God works in mysterious ways to provide hope for the future Jada is one of those Miracle kids 🙏 This article was beautiful It can send hope to all those parents who feel hopeless May God continue to give strength and encouragement to Amanda and Michael in the challenges they face as a family
Amazing journey told as a God’s story In The Elenbas family. Prayers change the heart of God and we will keep asking for Grace, Mercy and His love to follow you all each day. We believe In Miracles.