Like windows into patients’ rooms, iPads are giving families the ability to see and communicate with their loved ones in the intensive care unit at Spectrum Health.
The virtual visits, made possible through donated iPads and technical assistance, have lifted the spirits of family members separated by illness during the COVID-19 pandemic.
“It is super touching to see patients able to talk with their families again,” said Maggie Simons, RN, BSN, nursing supervisor for cardiothoracic critical care at the Spectrum Health Fred and Lena Meijer Heart Center. “It is the best medicine to hear them laughing in there.”
Spectrum Health team members began looking for ways to create that virtual connection after a state policy on visitor restrictions took effect March 16. The restrictions, which prohibit hospital visitors except in limited circumstances, are designed to prevent the spread of COVID-19 and protect patients and health care workers.
Breaking the news to ICU patients and their families was heartbreaking, Simons said.
The night before the state policy took effect, she and other staff members explained it to family members sitting at the bedsides of patients in the ICU.
“That was a hard day,” Simons said. “A lot of people handled it better than I thought they would.”
Spectrum Health’s Information Services team began working to make virtual visits happen—creating a connection that was secure and complied with health care privacy regulations, said Amanda Plunkett, senior project specialist in Information Services.
Bank of America donated 200 iPads, and Byrne Electrical engineered and donated power adapters to support the virtual iPad stations.
And donations to Spectrum Health Foundation’s COVID-19 Response Fund will go toward purchasing iPads and other equipment and services needed during the pandemic.
IS employees then set up Microsoft Teams, a video-conferencing app, on the iPads. They helped the first family members download the app at home on their own devices.
“Most of the people I work with tell me, ‘I’m not technical,'” Plunkett said. “But I’ve never been unsuccessful in getting them set up.”
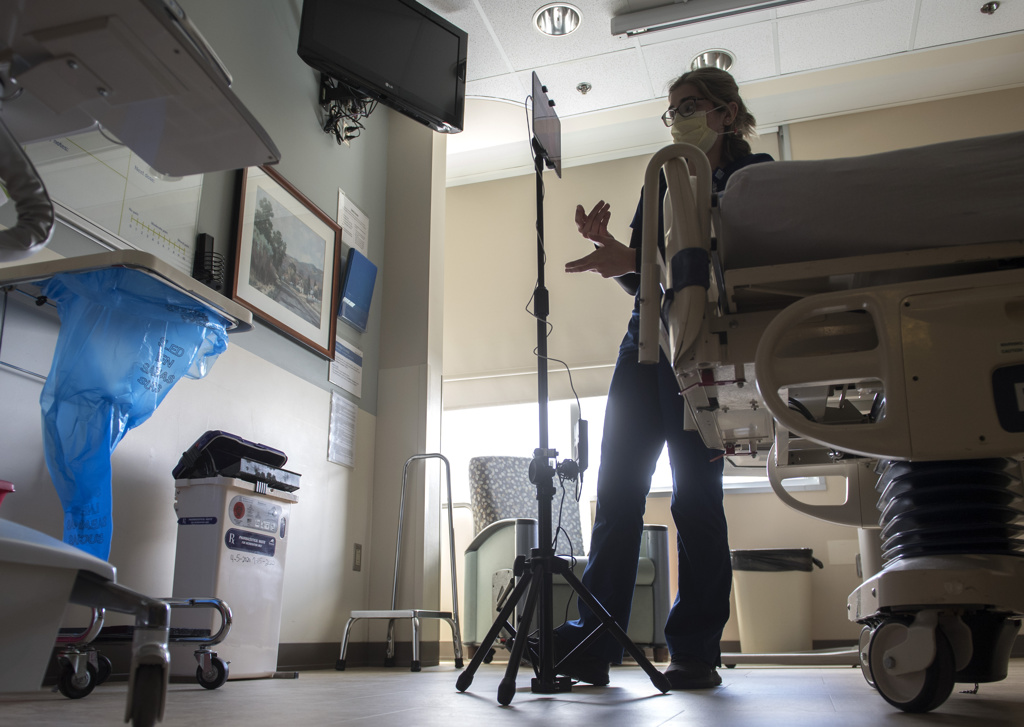
They then walked the ICU nursing staff through the initial connections. The iPad, mounted on a small tripod, may be moved to get the best view for patients and their families. Team members are also using laptops to connect patients with their families.
For about two hours in the afternoon, family members and patients visit through a live-stream connection.
The reaction from families?
“Joy,” Plunkett said. “It’s been really amazing. I hear a lot of thankfulness and appreciation. Even as people are worried and scared, they have just been appreciative for the opportunity.”
Family members enjoy seeing and speaking to their loved ones even when the patients are unable to communicate, Simons said. The nurses will give updates and explain the machines and medication that help the patient breathe.
“This has been huge for our patients and their families, just to help them feel a part of the care for these patients, so they can have some contact with them,” Simons said.
In some cases, the ICU patients have been able to take part virtually in family events—seeing a new baby or a child’s birthday celebration.
A healing connection
Once the first connections were in place, the staff from the All of Us research project at Spectrum Health took charge of implementing the program—and has brought it to all the intensive care units throughout the health system.
“It’s a good fit for the All of Us team,” said David Chesla, Spectrum Health director of research operations.
The staff members call patients’ family members to offer the service and set up the app. Sometimes they work with an adult child or grandchild to overcome technical hurdles.
As soon as the iPads became available, the nursing staff embraced the opportunity to connect their patients with family members through video chats.
“Our nursing staff has been handling this so phenomenally,” Simons said. “They dove right in. Nobody has complained about extra work. They are doing what they need to do to figure out this technology.”
In fact, the nurses find the virtual visits rewarding—and healing for their patients.
The ICU staff is dedicated to “patient-centered and family-centered” care, Simons said. The nurses and nurse technicians rely on family members to help them understand the patient and to know their likes and dislikes, particularly when the patient cannot communicate. The family might tell them what TV show to put on—or which ones to avoid—for a patient coming out of sedation. They can tell the nursing team the music a patient wants to hear.
“We value our families being here. A lot of times they are incredibly helpful to us,” Simons said.
Without family members present, the nurses can communicate with them on the phone. But seeing them on the iPad creates a more meaningful connection, she said.
The nursing team plays a key role in implementing the virtual visits, Plunkett said.
“I’ve been so impressed to see our busy nurses and nurse techs pause in their crazy schedules to make this happen,” she said. “I see so much empathy coming from the clinical staff.”







 /a>
/a>
 /a>
/a>
 /a>
/a>
This is such a wonderful thing you’ve all accomplished! Maggie: I admire your energy and leadership in this endeavor, as in all of the challenges you take on!
Thank you for reading and commenting, Molly. And I share your admiration for Maggie!
Our family was personally blessed by this program as we could not personally be with our loved one on Neuro ICU. Being able to tell him we loved him, prayed for him, and missed him was so healing for all of us. We are forever grateful for all those who made this service available during our crisis.
Your story touches my heart, Roze. Best wishes to you, your loved one and your family.