Elias Dababneh heard the car’s engine as he walked across the parking lot but he had no idea it was headed his way until he opened the door.
“Move! Move! Move!” a worker yelled.
He glanced over his shoulder and saw an SUV backing toward the door. He ran as fast as he could.
But the car came faster.
It smashed through the storefront, sending broken glass flying and drove completely into the store. The car’s rear bumper caught Elias as he tried to jump out of the way. It hurled him into the back wall and he crumpled to the floor.
“The first thing I was thinking was, ‘Oh man, I’m going to be out of work forever,’” he said.
He figured he had broken bones that would take a long time to heal. But the internal injuries inflicted in the crash posed the most immediate threat. They nearly killed him.
“It was a miracle he even made it to the hospital with that amount of bleeding,” said Charles Gibson, MD, a trauma surgeon in the emergency department at Spectrum Health Butterworth Hospital. “It’s a testament to how tough he is and also to his youth.
“It’s amazing he survived.”
In mere moments at a small market in Muskegon, Michigan, life changed dramatically for Elias, a 24-year-old man from Caledonia.
Four months later, he is back on his feet and getting stronger. But he still needs surgery to repair his abdominal wall, and months of recovery lie ahead.
Sitting in the kitchen of his family’s home in Caledonia, he talked about the crash and its impact on his life. As to the driver behind the wheel of the SUV, he tries not to dwell on that.
“I hope she knows what she did to somebody,” he said. “God will deal with her. I am past it. There’s nothing I can change about it. There’s no reason to keep holding on to it.”
It was hard to make heads or tails out of what was what. (The impact) basically obliterated the right side of his abdomen.
When Elias arrived at Spectrum Health’s Level 1 Trauma Center at Butterworth Hospital, Dr. Gibson knew only that he was a pedestrian hit by a car. Transferred from another hospital, Elias was on a ventilator and unable to speak.
Despite multiple transfusions, his blood pressure remained dangerously low. Worried he could bleed to death internally, the ER team took him to the operating room for damage-control surgery within minutes of his arrival.
His midsection had received such a powerful blow, “it was hard to make heads or tails out of what was what,” Dr. Gibson said. “He absorbed so much energy on that right side, those muscles ripped right off the bone. It basically obliterated the right side of his abdomen.”
He called in another critical care surgeon, Cathryn Chadwick, MD, to help with the surgery.
Elias had sustained severe damage to his bowels. The blood vessels that supplied the intestines were ripped in two. The surgeons began to clamp off the bleeding blood vessels. The torn arteries posed the most risk, because they carry high-pressure, high-volume blood pumped by the heart.
Next, they addressed the tears in his bowels, which leaked intestinal contents into his abdomen. They stapled them together to prevent further leakage and risk of sepsis.
As Elias feared, he did have broken bones: The crash cracked bones in his pelvis, spine, right femur, right heel and multiple ribs.
But the surgeons could not attempt to fix them right then. In trauma surgery, the goal is to address life-saving issues and wrap up the operation as quickly as possible. For a body that has already experienced trauma, surgery adds extra stress—taxing the heart and causing fluid loss.
“And there’s the fact that whenever your belly is open and you’re exposed to the operating room, you’re cold,” Dr. Gibson said. “When you get cold, your systems don’t work as well. You don’t clot blood as well. You’re not able to heal wounds as well.”
A team of 15 to 20 people, including the surgeons, the anesthesia team, nurses and technicians, worked on Elias.
“It literally took all those people to pull that off,” Dr. Gibson said. “We really had to move fast. There can’t be any wasted moves or any wasted time.”
With the bleeding stopped and his blood pressure stabilized, they closed the belly and moved Elias to the intensive care unit. The operation lasted about 1 1/2 hours.
Elias was still critically ill, but Dr. Gibson was just relieved that he had lived to fight another day.
“There were several times during the operation where his blood pressure was really low and I didn’t think he was going to make it off the table,” he said. “I thought he was going to die.”
Elias’ parents, Evette and Atif, and his sister, Eleyan, waited anxiously at the hospital while the medical team worked to save Elias’ life.
“We didn’t know what happened,” Evette said. “We didn’t know if he was alive.”
When he got out of surgery, they saw Elias in the ICU. When he woke up, he tried to communicate, but couldn’t speak on the ventilator. Tears flowed as he pressed his mother’s hand.
She asked what he wanted. His phone? Keys?
He shook his head. Tried to speak. He wanted a rosary.
The kindest patient
The next night, Dr. Gibson checked on Elias in the ICU and was pleased to see how much better he looked.
Elias reached up his hand for a fist bump with the surgeon. He mouthed the words “Thank you.”
“He is one of the kindest, nicest patients we have ever taken care of,” Dr. Gibson said. “I don’t think I’ve ever had a patient thank me so much.”
That evening, family members filled him in on the details behind Elias’ injuries. He saw a video posted by news outlets, showing surveillance footage of the car crashing into the store.
“I had no idea a car had gone through a building and caused all these things,” he said. “It was surreal.”
Elias passed his breathing trial sooner than expected and was able to have the ventilator removed within a day or two.
But after a few days, a new problem surfaced. Elias developed pain on his right side and some fluid build-up.
A new CT scan showed that the ureter, the tube that drains from the kidney to the bladder, had been torn in two. That injury initially had been obscured by all the other damage in the abdominal area.
The doctors placed a tube to drain the kidney into a nephrostomy bag temporarily.
Meanwhile, Elias continued to recover and grew stronger. He was eager to move ahead with physical therapy.
“He was itching to get up every time I saw him, even though he was in considerable pain,” Dr. Gibson said. “He wouldn’t complain. He just wanted to get better and to go home.”
Progress came slowly at first. With so much damage to his core muscles, the smallest movement could be excruciating.
“Even the simplest things like getting up with the physical therapist would skyrocket my heart rate to 170,” Elias said. “It was so much work.”
At times, he became discouraged about the road ahead.
“You weren’t supposed to make it off the operating table,” Dr. Gibson told him. “This is hard but not nearly as hard as what you’ve been through.”
Seeing her son so helpless broke Evette’s heart. Elias had always been so independent, never asking for help. In fact, he often had been her helper—when she had surgery and when she injured her neck in an accident.
With time, Elias realized how much he took for granted the everyday moments in life—the ability to put on his socks, get a glass of water or pick up his phone. He developed a deep appreciation and respect for all those who helped him—the doctors, therapists, nurses, technicians, cleaning staff and nutritional services.
“Everyone at Spectrum Health was completely amazing and they made it a lot easier,” he said.
Planning a pilgrimage
It wasn’t just the staff that aided his recovery, Dr. Gibson said. Elias had plenty of support from family and friends.
He always had a visitor at his bedside. The room was filled with cards and flowers. And the Dababneh family, who immigrated from Jordan when Elias was 1, greeted every staff member and visitor with a tray of baklava.
After three and a half weeks, Elias transferred to Mary Free Bed Rehabilitation Hospital, where he spent another three and a half weeks in rehab.
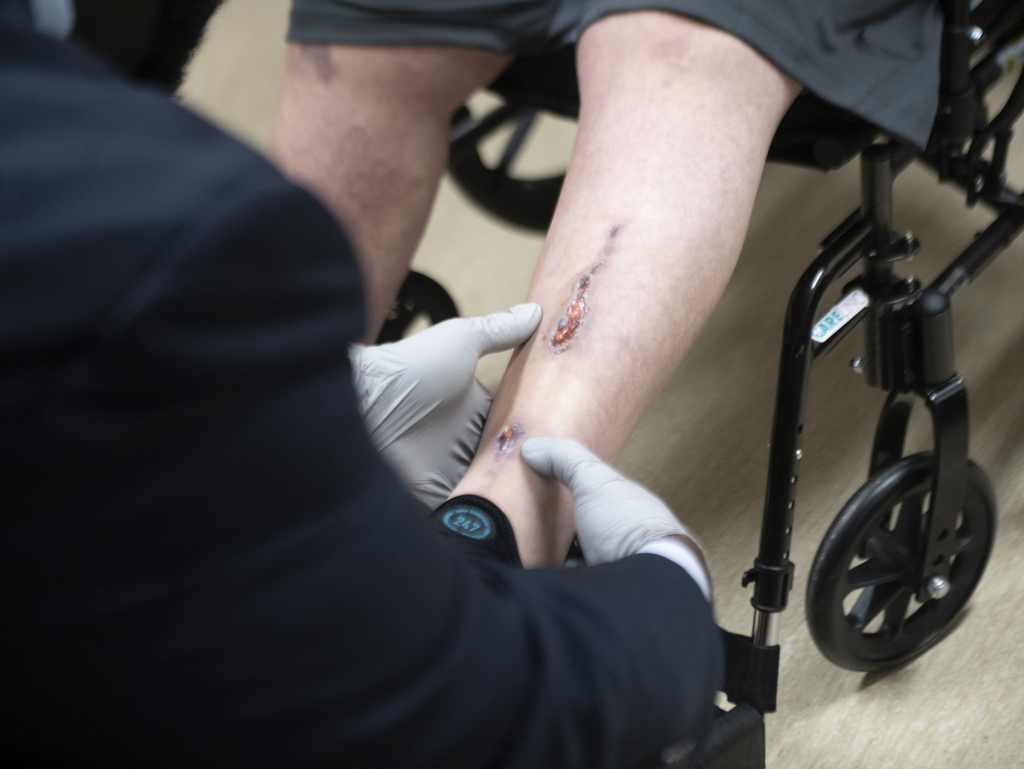
Once home, he continued to return for visits with the Spectrum Health wound clinic to ensure continued healing of the wounds on his abdomen and legs. He also continued with outpatient therapy.
On a recent afternoon, at an outpatient physical therapy session at Mary Free Bed, he talked about how much stronger he has become. He has progressed from using a wheelchair to a walker to a cane—and can walk shorter distances without any assistance.
In a balance exercise, he stood on one foot, while tapping three cones with the other.
“This would not have been possible even a month ago,” he said.
In a couple of months he will undergo hernia surgery to reattach the abdominal muscles torn from the pelvic bone.
The step will make a big difference in his long-term recovery, because the muscles hold in place the organs in the abdomen, said Luke Durling, MD, a Spectrum Health acute care surgeon who specializes in hernia repair.
Without those muscles, “the intestines, the kidneys are out of place,” Dr. Durling said. “It’s not comfortable.”
Once he recovers from that surgery, Elias looks forward to returning to his job working for a wholesale distribution company.
And for the Dababneh family, a trip to the Middle East is in the future. They want to visit relatives in Jordan. And they want to go to the Church of the Holy Sepulchre in Jerusalem.
“I told my husband when he is done with everything, the first thing I want to do is take him to that church and thank God,” she said.
“You just feel holy when you are there,” Elias said.
Digging deep
For Dr. Gibson, Elias’ survival brings home the value of a team approach to trauma care. During that first surgery, when Elias’ life hung in the balance, he remembers thinking what would happen if Elias did not survive.
“Things don’t always go to plan and you have to think on the fly,” he said. “I started thinking, ‘What if this goes wrong? What’s my next step? And if he can’t make it, what am I going to tell his mom?
“It kind of inspires you to dig deep and put everything else out of your mind and focus on getting the job done.”
And getting that job done—at that moment and in the many moments involved in Elias’ survival and progress toward full health—required the efforts of a vast network of people.
It began with first responders and the regional hospital that treated and transferred Elias. And it continued with the trauma team at Butterworth Hospital, which encompasses acute care surgeons, anesthesiology, operating room staff, nurses, advanced practice providers, respiratory therapists, technicians, social workers and rehab specialists.
“Our team is always ready and capable to handle anything from the simple to complex because we have a cohesive group of people with one common goal of returning patients to their loved ones in the best condition possible,” Dr. Gibson said. “Success stories like Elias’ simply do not happen without every member of the team being ready and capable of doing their job when called upon.”
















 /a>
/a>
 /a>
/a>
 /a>
/a>
Wow u
Guys r amazing and very compassionate to ur patients ! What a great team of professionals with big ❤️❤️ And much respect to u
For what u do
And deal
With what an amazing true story of this kind young Man U
Beat the odds
He definitely beat the odds, and you’re so right – both he and his team of caregivers have huge hearts. Thanks, Amie, for your kind comment and for being a Health Beat reader!
Dr. C.J. Gibson is rock star at Spectrum Health Butterworth. We are so blessed that he returned to West Michigan after his fellowship. He is an excellent example of what a trauma surgeon should be…calm, steady, decisive, confident, humble. Every time I work with the trauma surgeons at Butterworth during an emergency, I am amazed at their life saving skills! They keep people alive that were at death’s door, and they truly care about their patients.
Thanks for sharing your perspective on Dr. Gibson and the trauma surgeons, Elizabeth. I think he would be the first to say it takes a team to make these success stories happen.
This is my son’s good friend and just an amazing story!
His is truly a remarkable story! Please feel free to share this story far and wide with your network of friends and family, Peggy! Best wishes, Cheryl
You all accomplished a mighty work that night.Everyone from EMT’s,Physicians,nurses,OR techs worked together to keep him alive.On the unit everyone there worked to make sure any complications were addressed immediately.This is trauma care at it’s finest.God bless you all.