Roxanne Nelson dreaded lung cancer surgery.
“I thought it would be just horrible,” she said. “My imagination is as big as a hip-roof barn.”
She expected weeks of slow, painful recovery. Weeks when this always-busy volunteer would feel like an invalid.
But there was one thing her imagination did not foresee: that her surgery would be a minimally invasive operation, performed with a da Vinci robot.
Nelson, a 65-year-old woman from Ionia, Michigan, became the 1,000th Spectrum Health patient to undergo lung surgery using the da Vinci robot.
The da Vinci surgery “has a huge advantage for the patient,” said Charles Willekes, MD, the cardiothoracic surgeon who performed the operation.
“Instead of a 15-centimeter (6-inch) incision, they have four 1-centimeter incisions. There’s far less pain, definitely less bleeding and less chest wall trauma.”
And Nelson rebounded much quicker than she ever expected.
“This is fantastic,” she said three weeks after the operation. “I am like Wonder Woman. I am doing everything now.”
Nervous but hopeful
Nelson learned she had lung cancer in August 2018. She had undergone tests to monitor possible symptoms from a closed head injury 11 years earlier.
A CT scan revealed a spot on her left lung, which turned out to be cancerous.
A former smoker who kicked the habit years ago, she said her autoimmune diseases put her at risk for lung cancer.
“When you get that term cancer, it’s devastating,” she said. “And lung cancer is even more devastating.”
She didn’t know how she would cope with the surgery to remove the lower lobe of her left lung.
It is really unbelievable how (the da Vinci system) has changed thoracic surgery.
She keeps busy yearlong with volunteer projects for her Ionia community—helping to plan the Ionia Free Fair and its Ladies Day program, Toys for Tots and the Ionia Fall Festival. She lives on a farm with her husband, Mike.
“I eat breakfast standing up. I eat lunch standing up. The only time I sit down at home is to eat supper,” she said. “I thought if I have to be a couch potato for months, this woman is going to be insane.”
She worried about how her autoimmune diseases would affect her ability to handle surgery. And because she has allergies to common painkillers, she wondered how she would manage the pain.
By the time she arrived at Spectrum Health Meijer Heart Center for her operation, she had read up on robotically assisted surgery. And that made her hopeful.
She was still nervous, but hopeful.
“I think this (approach) is less invasive,” she said as she waited in a pre-op room with her husband and her daughter, Karen Leak. “You’ve got less healing time and less blood loss.”
Cardiothoracic surgeon Edward Murphy, MD, performed the first da Vinci robotic lung surgery at Spectrum Health in 2007.
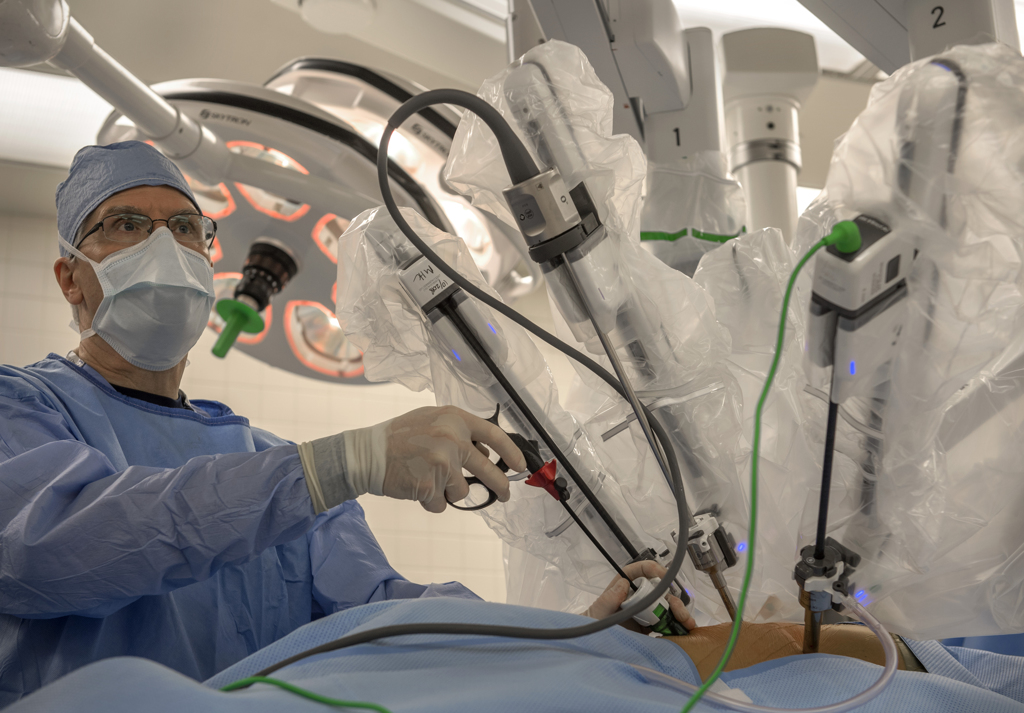
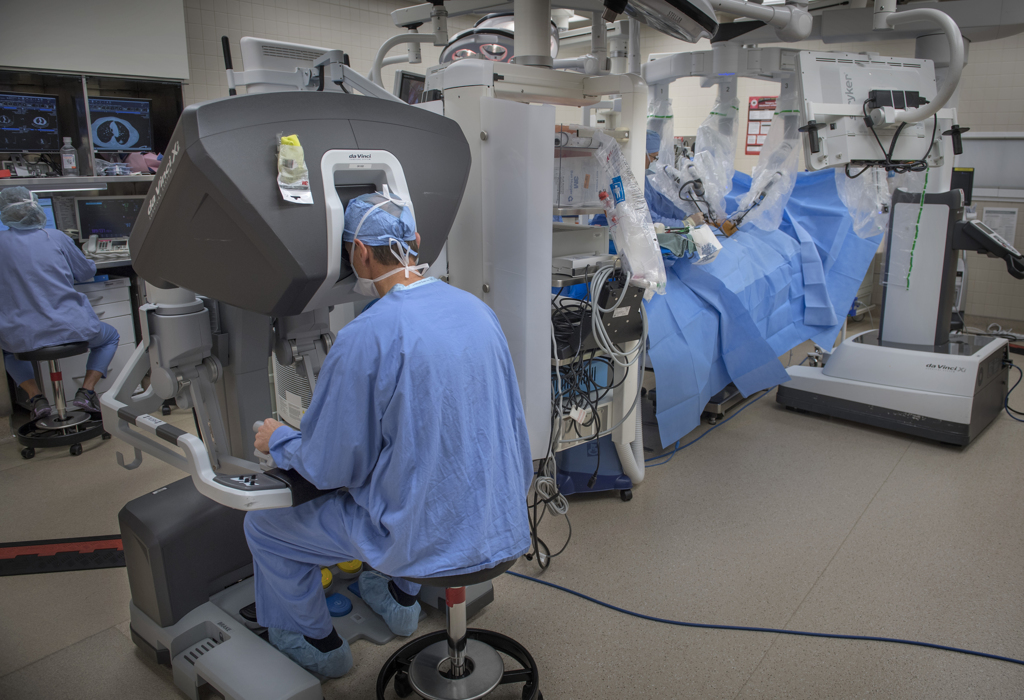
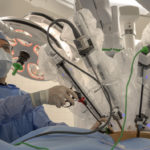
The system is operated by a surgeon sitting a few feet away from the patient at a console. The surgeon operates the tools at the console, guided by a 3D view of the chest cavity provided by a powerful camera. The robot mimics the precise movements of the hands on the surgical site, operating through tiny incisions.
“It’s not just pushing a button or holding a button,” Dr. Willekes said. “You put your fingers on the console and into the controller and they follow perfectly the movements of your fingers—whether you are squeezing something hard or whether you turn your wrists up with your fingers. It is very intuitive that way.”
And the robotic device has greater dexterity than the human hand.
“It can go in 360 directions in 360 rotations,” Dr. Willekes said. “At each point in the circle, it can turn another entire circle. It’s amazing that way.”
As the da Vinci improved over the years, its use in lung surgery increased, Dr. Willekes said. Now, Spectrum Health surgeons use it in 80 percent of lung surgeries.
“The latest model caused the leap,” he said. “The developments in it have allowed us a broader application.
“It’s more nimble. The arms are lighter and thinner. And it’s actually able to position itself on the patient when we tell it where the operating field is.”
Another big advance: The da Vinci now has its own stapler.
“That is a critical part of dividing structures in the chest. It allows us to control airways and blood vessels to the lung with 100 percent certainty,” Dr. Willekes said.
Game changer for docs, patients
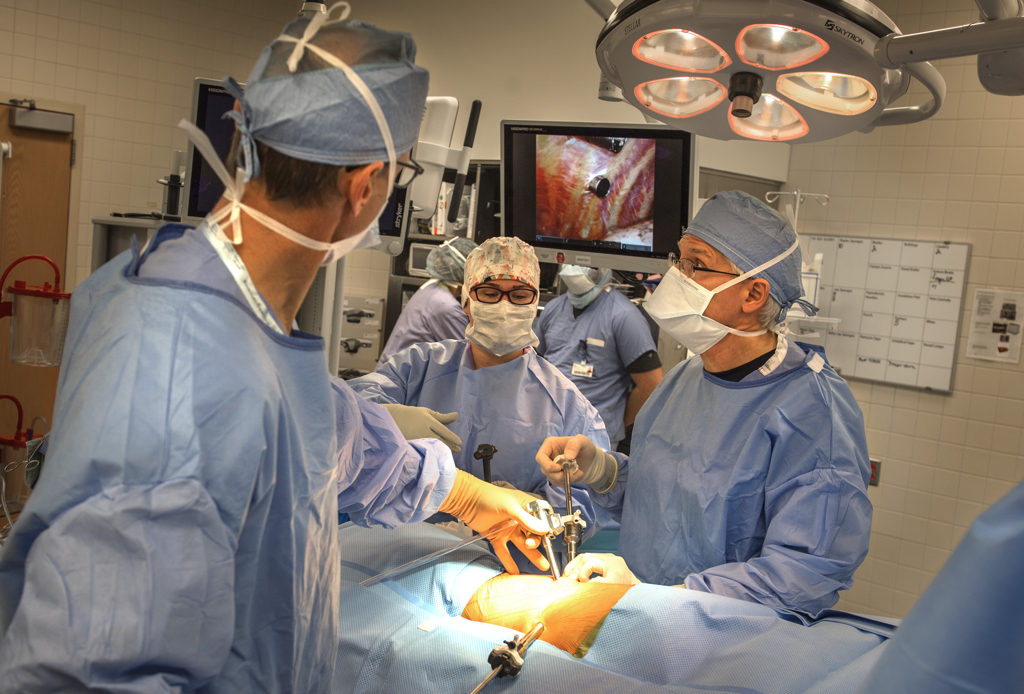
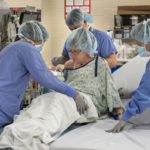
As Nelson arrived in the operating room, she was greeted by the same surgical team involved in the first da Vinci robotic lung surgery at Spectrum Health.
Dr. Willekes received assistance from physician assistant David Drew, PA-C, and nurses Joanne Schepers, RN, and Tracy Middaugh, RN.
The surgeon made four keyhole-sized incisions in her chest. Into each incision he placed a long narrow tube.
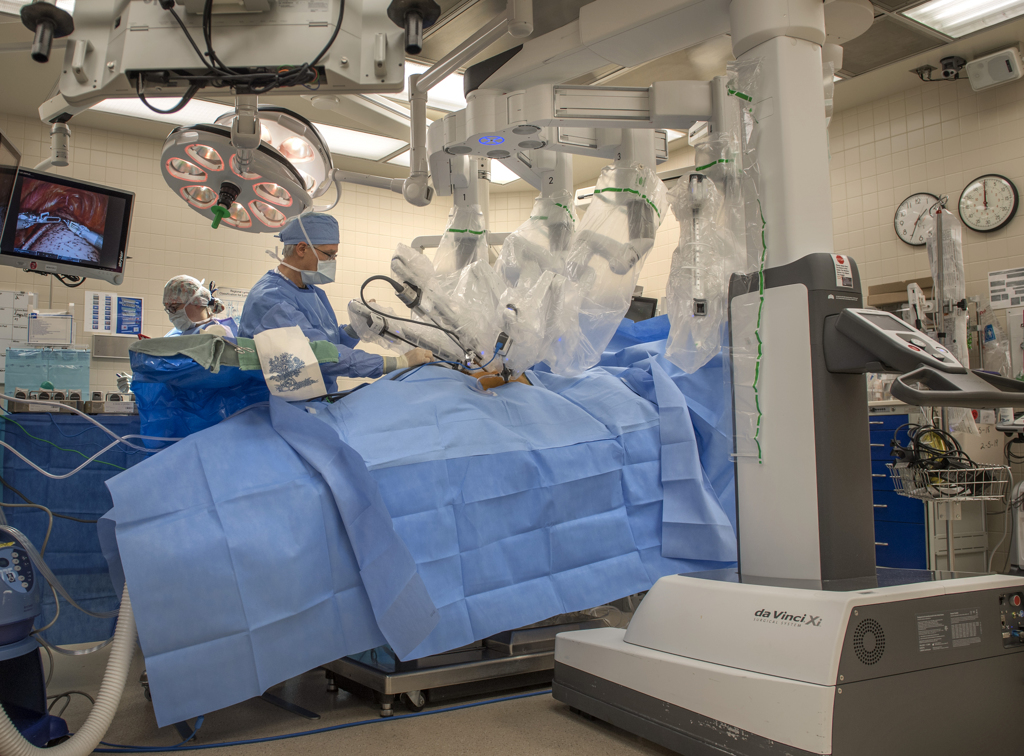
“We’re ready to dock,” he said.
The team brought the da Vinci robot to the table, where its arms extended into three of the tubes.
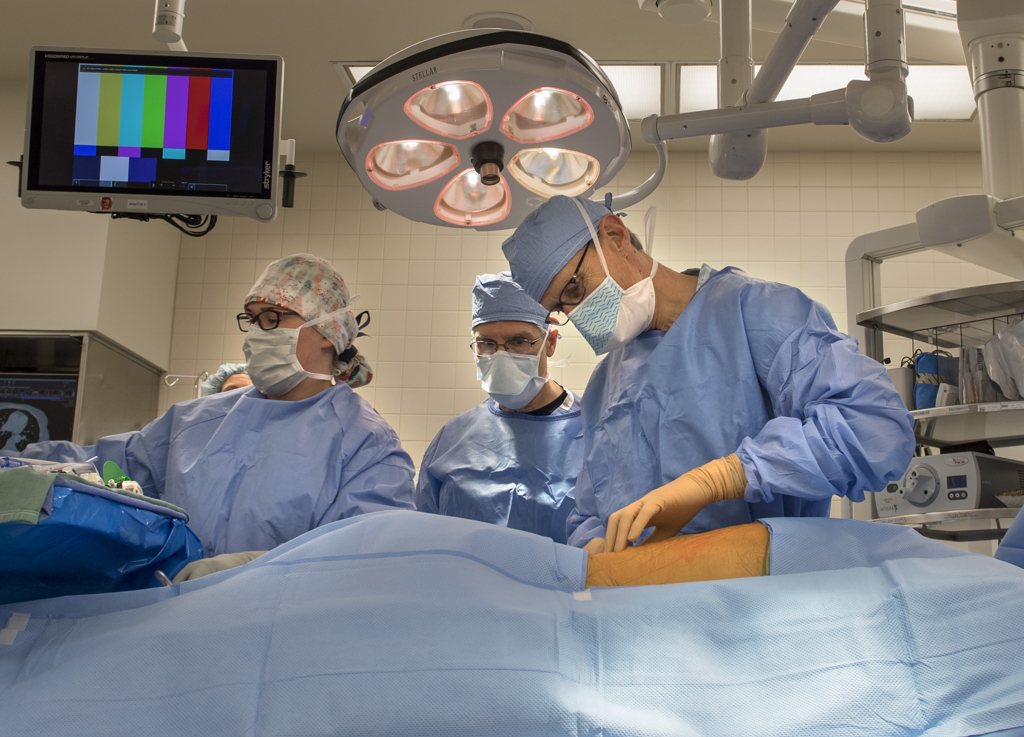
One of those arms held a scope with two cameras that provided a 3D image of the chest cavity for Dr. Willekes, who sat a console at the foot of the operating table.
His viewfinder—and a screen above the table—showed the inside of Nelson’s chest in full color. Ribs arched overhead. The lung, its folds rising and falling with breath, lay below.
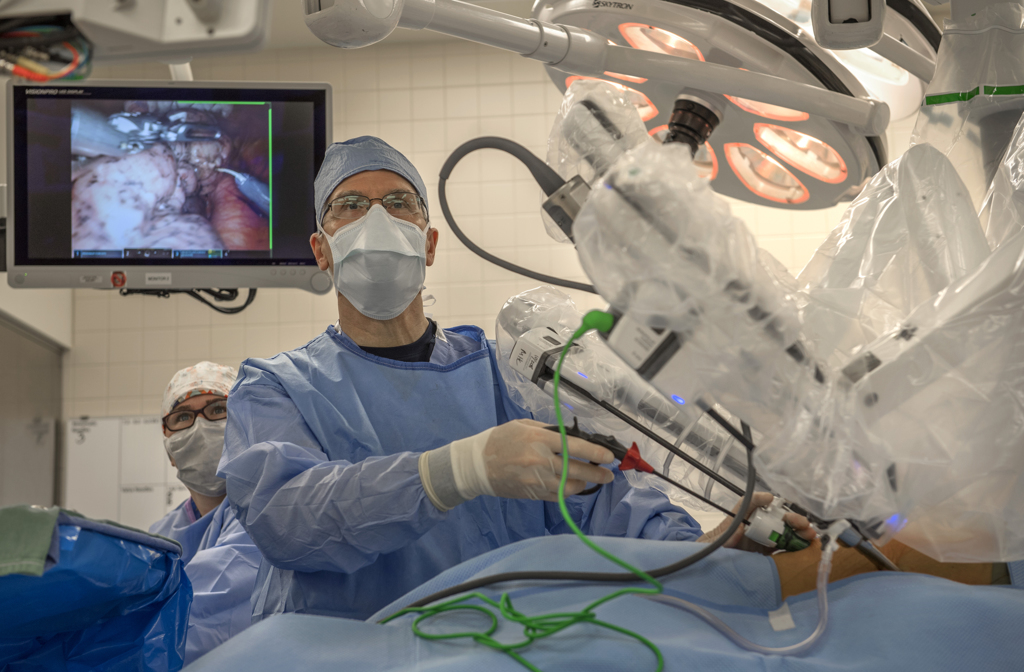
As Dr. Willekes moved his arms and hands, the arms of the robot swirled above Nelson’s chest. With grasping forceps, scissors and a hot knife—a scalpel that cauterizes tissue—he separated and removed the lower lobe of the lung as well as 17 lymph nodes.
Drew assisted in removing each item, using a tool placed through the fourth tube.
“We actually have better vision (using the da Vinci),” Dr. Willekes said. “I spent the first 20 years of my career trying to look into a hole in the chest. We were always working in a well.”
The 3D camera grants a clear view of the entire chest. He no longer has to lean down and angle for a look at difficult-to-see areas—or expand the incision.
“It’s almost as if you’re sitting inside that body cavity operating on that tissue,” he said.
And by lessening the physical toll of a long surgery, it carries ergonomic benefits for the doctors.
“It’s a game changer for the patient and the surgeon,” he said. “It is really unbelievable how it has changed thoracic surgery.”
Three weeks later
Not long after surgery, Nelson received good news from her doctors. Her cancer, determined to be stage 1, was removed in the operation. Biopsies of the lymph nodes showed no sign of cancer.
She found herself quickly returning to her usual activities and household chores.
“Yesterday, I did two loads of laundry and I vacuumed,” she said, three weeks after her operation. “I never expected to do this so soon. I am more than thrilled.”
The Food and Drug Administration approved the da Vinci surgical system in 2000 for laparoscopic procedures. Since then, surgeons have used it in a variety of areas, including cardiac, obstetrical and prostate procedures.
Dr. Willekes and Dr. Murphy received extensive training in 2006 before starting to perform lung surgeries in 2007.
In thoracic surgery, the system is used for lobectomies and in operations on the thymus gland and the esophagus.
In lung surgery, cases where the surgeons don’t use the da Vinci system include lung cancers that have invaded the chest wall and operations performed in areas with scars or distorted anatomy from previous surgeries, Dr. Willekes said.
“We still have to be selective about it,” he said. “But now, most (lung) patients are candidates for it.”








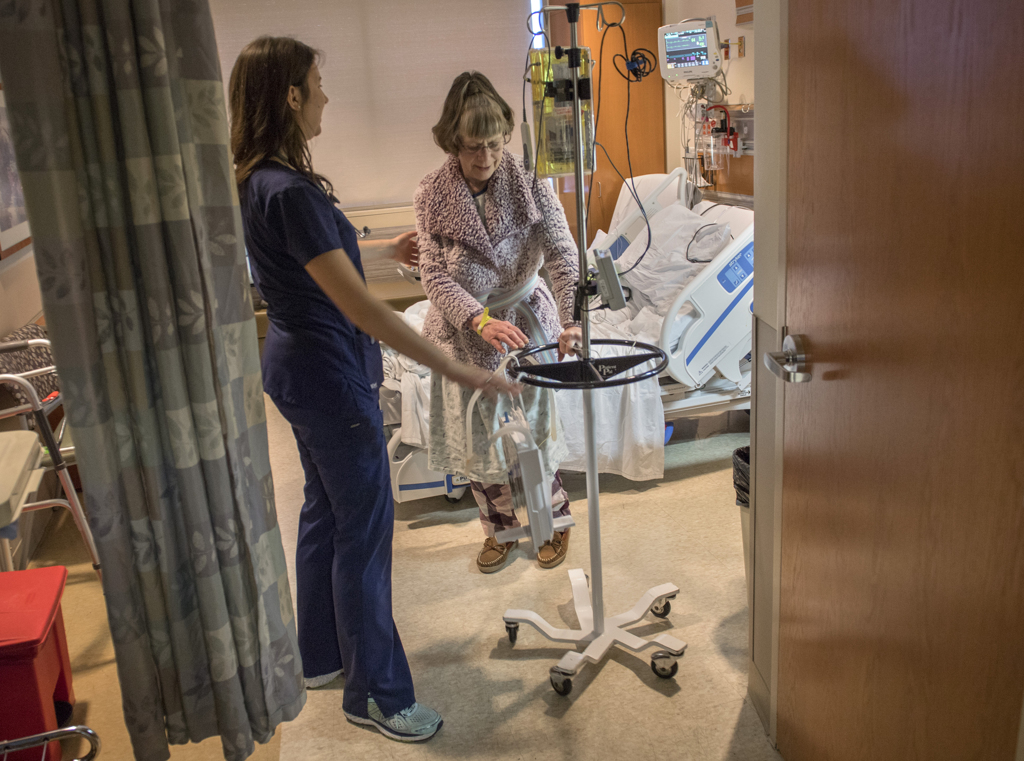
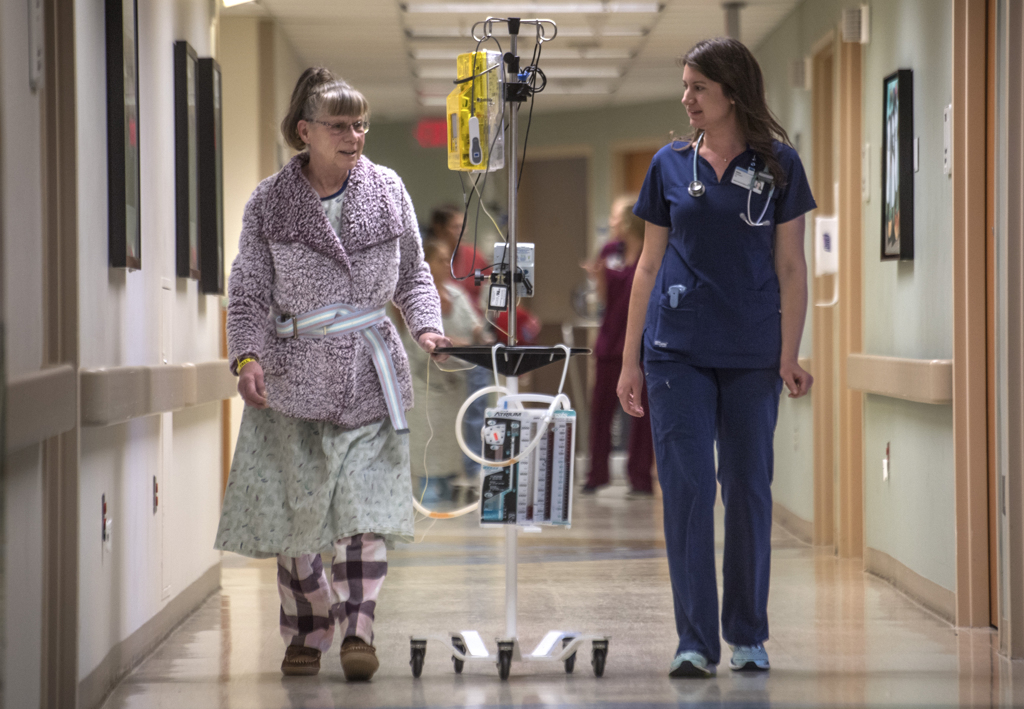





















 /a>
/a>
 /a>
/a>
 /a>
/a>