Terry Jacobs had his hands on the wheel of his semi, mid-curve on the on-ramp to I-57 in Kankakee, Illinois, when he had his first heart attack. He was 40 years old.
His chest clenched. He cringed in pain. Not knowing what was happening and not wanting to delay his delivery, Terry grabbed a Tums antacid tablet and drove another thousand miles to Amarillo, Texas, before seeking medical help.
“It was more important to me to get there, so I pushed it,” said Terry, 54, of Fennville, Michigan. “But who thinks they’re having a heart attack at 40?”
Twenty-plus years of the truck driver’s lifestyle had taken its toll, leaving him with heart disease, diabetes and eventually COPD.
“Mountain Dew, smoking and truck stop food—it’s the best thing for you,” he quipped.
A doctor in a Texas hospital inserted a stent to open a blocked artery, but Terry went on to have six more heart attacks over the next four years, the last one at a rest area outside Boonville, Missouri.
This one marked the end of his career as a long-haul driver. The damage to his heart was too severe to keep up with life on the road.
“He’s dying”
From there Terry’s health went downhill, and by 2007 he was so ill he landed in his local hospital with a grim combination of issues. When a kidney specialist saw him, she said, in Terry’s words, “You’d better get that man to Spectrum. He’s dying. He’s got way more problems than heart problems.”
The way his wife, Nancy, tells the story, once Terry got to the Spectrum Health Fred and Lena Meijer Heart Center, she “had his funeral planned.” But thanks in part to a cardiologist who successfully stented a blocked stent, the doctors managed to get him stabilized.
Terry resumed life at home with limited physical activity. With an implantable cardioverter-defibrillator keeping his heartbeat steady, he did what his body allowed him to do—some fishing, tinkering with cars and small projects around the house—but he never felt well and had zero stamina.
As his heart failure progressed, he showed all the classic symptoms, including abdominal swelling and shortness of breath.
“He couldn’t walk from here to that counter without stopping and gasping for air,” Nancy said, sitting in a local restaurant.
Lifesaving LVAD
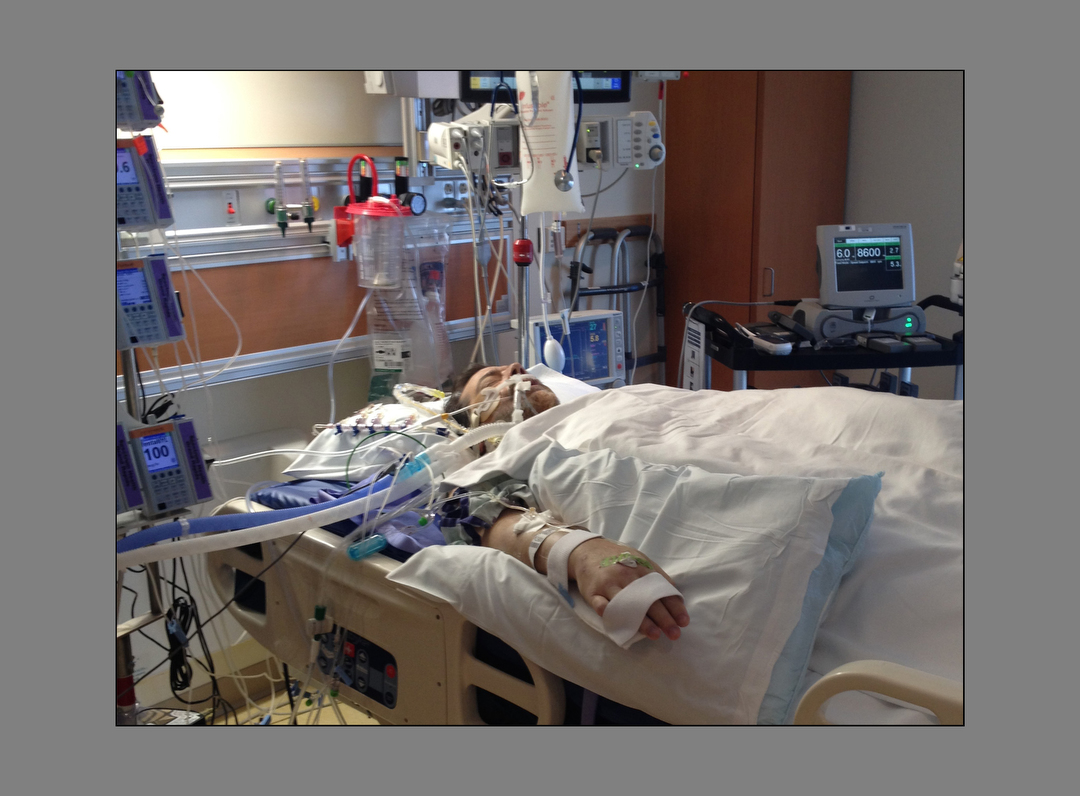
Late in 2014 death again looked imminent. When Terry entered the Fred and Lena Meijer Heart Center that December, his body was so full of toxins he was delirious and behaving unpredictably.
The heart failure team fully expected him to die, said Michael Dickinson, MD, medical director of the Spectrum Health Richard DeVos Heart and Lung Transplant Program and head of the Advanced Heart Failure Program.
But remarkably, Terry survived long enough to qualify for a left ventricular assist device, or LVAD.
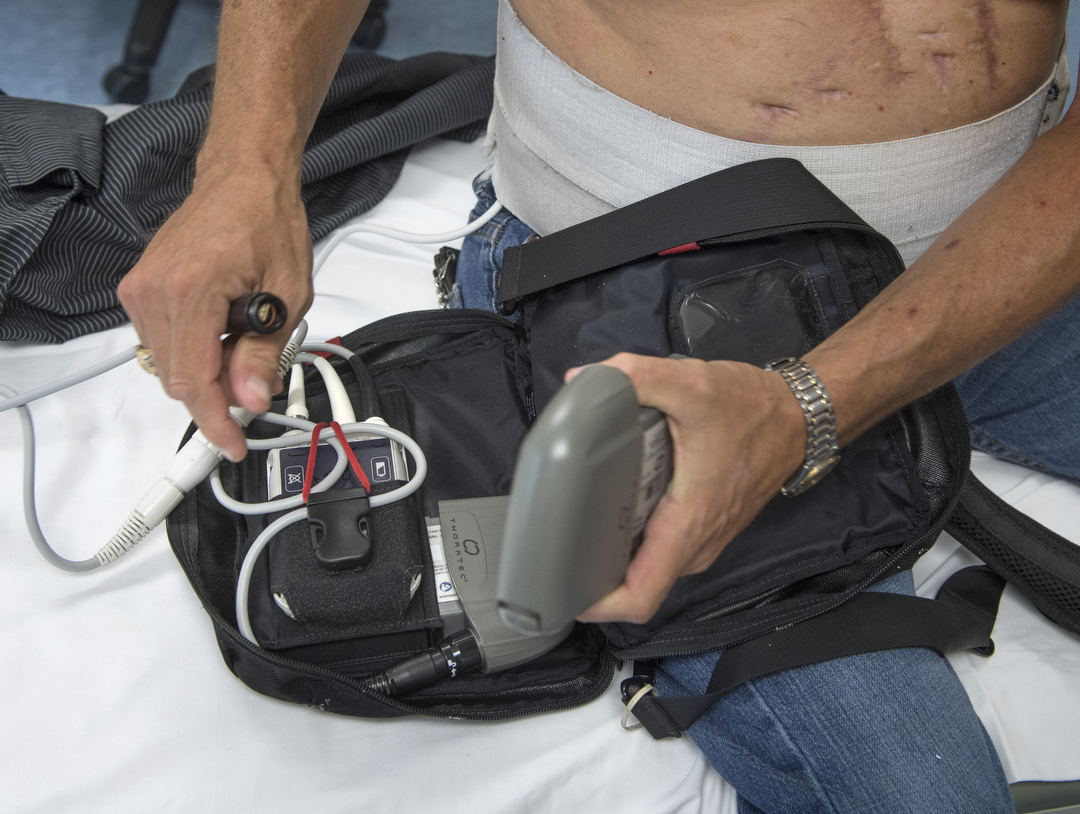
An LVAD is a mechanical heart pump with internal and external components. Internally, a device is attached to the weakened heart to help it pump blood out through the aorta to the rest of the body. Externally, a controller is strapped to the patient’s waist and a double battery pack hangs from the shoulders. Internal and external parts are connected via a driveline that passes through the patient’s abdomen.
For some patients an LVAD is a bridge device, keeping them alive while they wait for a heart transplant. For those who aren’t eligible for a transplant, the LVAD is considered a destination device.
Terry was in the second category.
“LVAD or die,” Nancy said.
They chose the LVAD, though as sick as Terry was, they knew there were no guarantees. The surgery was performed by Theodore Boeve, MD, a cardiothoracic surgeon who is now director of heart and lung transplant surgery and mechanical circulatory support at Spectrum Health.
Complications sprang up almost immediately for Terry—serious issues. Things were touch and go for weeks.
“I didn’t think he was ever coming home,” Nancy said. “It was bad. It was long.”
Making matters worse, two family tragedies struck during the 69 days Terry resided in the hospital. First a beloved niece died and then Terry’s brother died.
The medical team wouldn’t let Nancy tell her husband about either death.
“All the doctors and nurses knew what was going on at home,” she said, and they told her, “No, you can’t tell him—that would just crush him. He needs to worry about Terry and only Terry.”
But they didn’t leave her alone with her grief. Nancy said she received as much care and support from the hospital staff as her husband did, just in different ways.
“We always say if we hit the lottery we’d give them millions. They weren’t only great for him, they were great for me,” she said.
“We have a lot of friends there,” Terry added.
The strategy of letting Terry focus on healing worked, because sometime in early 2015 he turned a corner.
His critical issues resolved, the LVAD did its job and his body responded.
“It was fun to watch him go from being really sick, where we weren’t sure how well he was going to do, to when he suddenly got better,” Dr. Dickinson said.
In February 2015 Terry was discharged to rehab, and a few days later he went home.
Home to start a new life.
The way Terry and Nancy see it, the LVAD changed everything. Life in the Jacobs house divides along a line called “before the LVAD” and “after the LVAD.”
“When I got this and went home, I felt better than I have in 20 years,” Terry said.
Choosing to really live
Since that day, more than two years ago now, Terry is enjoying life in ways he couldn’t before—cutting wood, doing auto-body work, changing the oil in his Jeep.
“I might even do some things I’m not supposed to do, you know? Just try to do all you can do.”
He loves to go out in his custom 4×4 with anyone who wants to ride along—even his golden retriever, Sandy.
“I went out the other night, just me and my dog,” he said. “We went four-wheeling about 2 o’clock in the morning. I couldn’t sleep, and it was raining. We’re back in the woods and the mud is flying and the dog’s got her head out the window and she’s completely covered with mud.
“Well, I got stuck,” he continued, “so I had to pull my winch out, slog through it, hook up my winch, pull the Jeep out.
“And we just had a ball.”
This is the kind of story Dr. Dickinson loves to hear from his patients.
“One of the themes we have when we look at both LVAD and transplant (patients) is that we do this so that people can live, not just stay alive,” Dr. Dickinson said.
“We do these so that patients go home and live really full and active, complete lives.”
Part of his job, the doctor said, is helping patients who are facing a heart transplant or an LVAD insertion understand that to make it through the deep valley ahead of them—a high-risk procedure followed by weeks of hospitalization and rehab—they need something to live for on the other side.
“So we start talking to them about, ‘What are your goals, what do you want to achieve, what’s on the other side that’s worth going through this valley to get there?’”
Terry’s story is a tale of someone overcoming his limitations and barriers. But more than that, Dr. Dickinson said, it’s “a celebration of the human spirit, about people that choose to live.”
Terry’s recovery even earned him a spot on the heart transplant list. After 23 months, however, he was removed from the list because his antibodies became too high. Though this was a disappointment, it didn’t change his approach to life.
As Terry put it, he didn’t spend 69 torturous days in the hospital “just to come home and lay on the couch.”
The couple said having the LVAD is a way of life for them now, despite its downsides—the worst of which is that it prevents patients from being in or around water.
Today the two are planning for life after Nancy’s 2018 retirement. They’re getting ready to put their house on the market and buy something smaller so they can spend weeks on the road visiting the American West.
And they’re taking every opportunity to encourage heart failure patients who are contemplating an LVAD to say yes to the device. Sometimes he thinks his life was spared for this very reason, Terry said.
“This must be it,” he said. “This must be why I’m around.”
























 /a>
/a>
 /a>
/a>
 /a>
/a>
Dr. Dickerson was my cardiologist until he moved on. Great guy.
Enjoyed reading your story!! So great to see that you have a strong outlook on life and want to live it to the fullest!! Keep up the great attitude!
truly amazing <3
So glad you shared your story! You will inspire others.
Nancy, you and Terry give me so much hope for my husband John. He has COPD, diabetes. He is now on night time oxygen, but is still working. He drives truck locally. John has an appointment at Mayo in Sept. You both are so courageous, hats off to you both as Terry moves forward. I am so excited for you both. I will pass this story into Sydney. I am sure she would love to read it. Live life and enjoy everyday together. ❤
Thank you for sharing your ongoing journey with us. Love you both!