Stephanie Schlueter doesn’t have a drop of Irish blood in her family tree, but she looked forward to the Spectrum Health Irish Jig more than most.
As an RN with Spectrum Health Endoscopy, she’s participated in the 5K event dedicated to colon cancer for the past four years.
It’s always been a fun-filled event walking or running with co-workers, followed by brunch.
This year, it was a heartfelt event. And bet your bottom Blarney stone—Schlueter feels lucky.
In December, Schlueter, 36, learned she had colon cancer.
“Looking back, I had a change in bowel habits last summer,” she said. “I had started working out at the gym a lot harder in July and August. That’s when I noticed a change. I thought, ‘I’m exercising more, I’m getting healthier, I’m pooping more frequently and it’s smaller.’”
Unfortunately, her health suppositions proved wrong. Instead of getting healthier, a cellular beast threatened her body. And her life.
“The change in bowel habits was probably the first tip-off, but it didn’t register until later,” she said. “I thought it was all due to increased activity.”
Her symptoms surged—bloating, pain, cramping and constipation—symptoms similar to irritable bowel syndrome.
She asked medical professionals in her endoscopy practice if IBS could strike out of nowhere. She didn’t think so.
“Why would I have colon issues?” she said. “I’m healthy as a horse.”
Her co-workers suggested she visit her primary care physician.
“They worked me up for parasites,” Schlueter said. “All my labs were coming back normal. But my inflammation marker came back high.”
It was a sign of bad news to come.
She spoke with Courtney Ferch, MD, a Spectrum Health Medical Group gastroenterologist, who scheduled a colonoscopy.
“She was able to get me in early one morning outside of her regular lineup,” Schlueter said. “The upper scope was normal. But the lower one, they couldn’t get through because of a tumor. It was in my sigmoid.”
The tumor looked suspicious.
“From the pictures, it looked bad,” Schlueter said. “It just had that cancery look to it.”
Dr. Ferch called for James Ogilvie, MD, a Spectrum Health Medical Group colorectal surgeon.
“Luckily, Dr. Ogilvie was in the building,” Schlueter said. “They called him into the room. He couldn’t get past the tumor, either. That was on a Friday. He scheduled me for surgery the following Tuesday. It was super impressive they were able to get me in that quickly.”
And, super important. By the time her Dec. 19 surgery date dawned, the biopsy results were back. They confirmed what everyone suspected. This 36-year-old suffered from colon cancer.
“The cancer was growing inside the bowel, causing symptoms of a bowel blockage and bleeding,” Dr. Ogilvie said. “Surgery involved removing a small section of large intestine and the associated lymph nodes around the area.”
Schlueter said she feels fortunate.
“I didn’t need a bag or ostomy, which is super lucky,” she said.
Schlueter remained in the hospital for four days, her fiancé, Paul, by her side.
“We just got engaged two weeks before I got my diagnosis,” she said. “Talk about starting off with really serious stuff.”
After her diagnosis, they postponed the wedding until spring of 2019.
“I figured I’d lose all my hair and I didn’t want to be a bald bride,” she said. “Paul is so great, I think he was afraid to leave me alone after the surgery.”
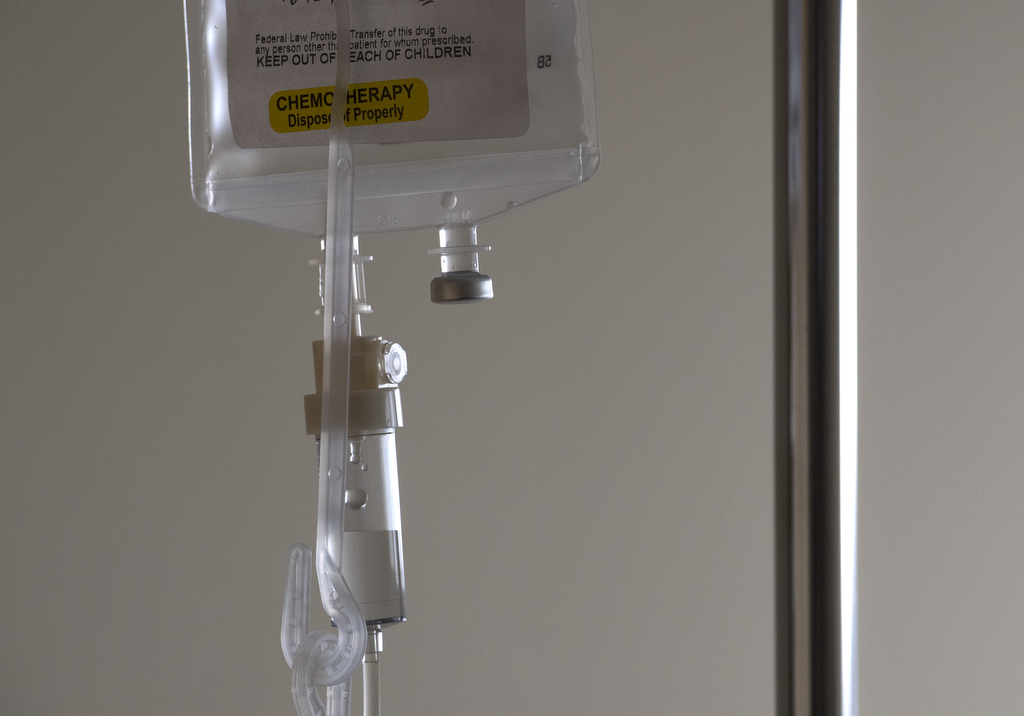
Next, chemotherapy commenced.
Schlueter didn’t need radiation because Dr. Ogilvie had been able to remove the whole mass. But there’s not much anyone can do to remove the mass of fear that lingers after a cancer diagnosis.
“We’re doing clean-up chemo,” she said. “I should be golden as soon as they get rid of the cancerous cells. It’s still scary. What if they miss cells? What if it comes back in six months as a liver metastasis or comes back in my lungs? I’ll be scanned pretty frequently, but it will be scary in between.”
Working in endoscopy, Schlueter sees first-hand that colon cancer isn’t an older person’s disease anymore.
“It’s becoming more and more common in young people,” Schlueter said. “There are a lot of theories—maybe it has to do with the HPV virus, what we’re eating or the chemicals we’re putting into our bodies. In my opinion, they should bring the age down from 50 as the start-screening age.”
In the last decade, colon cancer in people ages 35 to 45 has doubled, according to Dr. Ogilvie.
“The rate, however, is still 15 times lower than those 50 to 60 (years old) and 30 times lower than those over 70,” Dr. Ogilvie said.
Schlueter’s experience has sent her on an unintended mission—to encourage others to be on-guard.
“If people have a change in bowel habits or even bleeding, they need to see their PCP about it and they may need to push their PCP to consult a GI or colorectal doctor about having a colonoscopy,” she said. “People need to be their own health advocates these days.”
Schlueter feels blessed to have caught the cancer early, and blessed with a strong support system of family, friends and co-workers.
“I have really good co-workers,” she said. “They keep me going when I need to go or back off when I need time alone. It’s really been a blessing to have them.”
Tears streamed from Schlueter’s eyes as she spoke about what it meant to have the doctors and staff from endoscopy wearing T-shirts and participating in this year’s Irish Jig in her honor.
“I’ve got all these people that are excited to stand by me and be helpful,” Schlueter said. “It’s just amazing.”
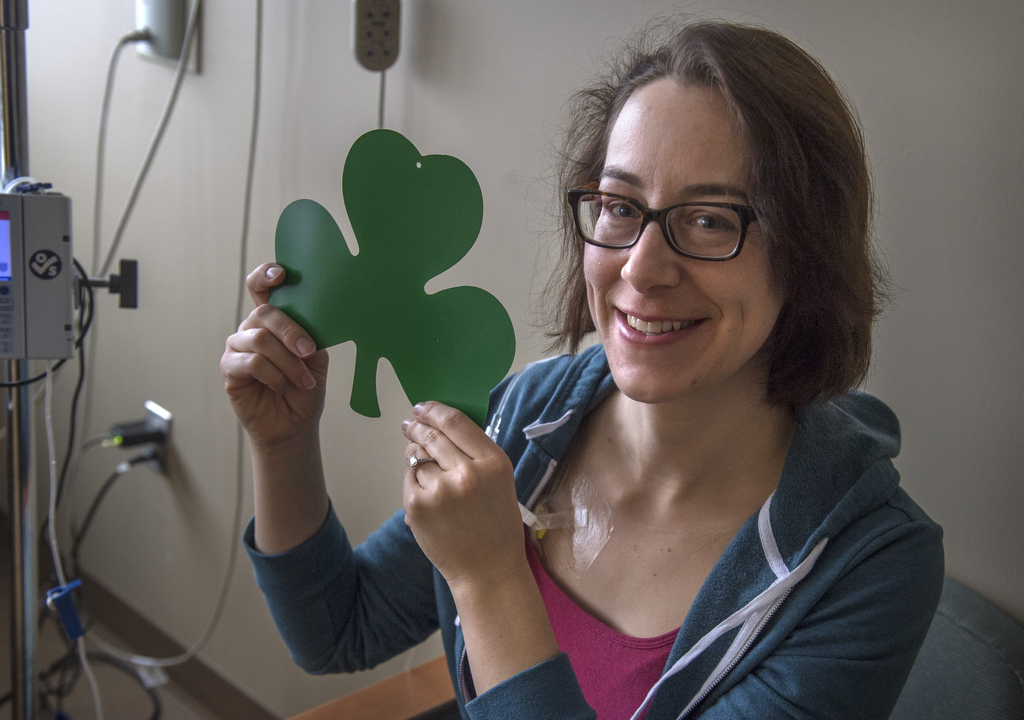


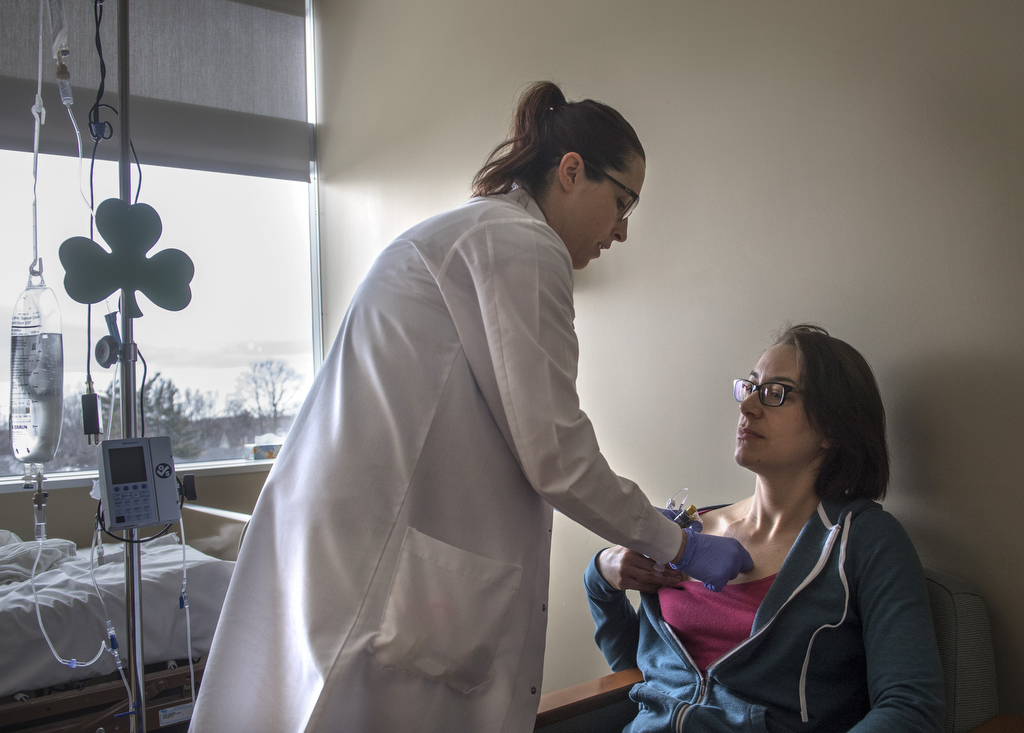












 /a>
/a>
 /a>
/a>
 /a>
/a>
Love the strength you display throughout this ordeal. You remain in my thoughts and prayers daily.