Ecstatic.
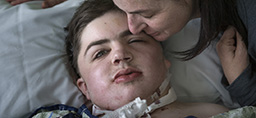
That’s how Mike and Debra Koster felt when they cradled their newborn son, Jonathan, 22 years ago.
Surprised, too.
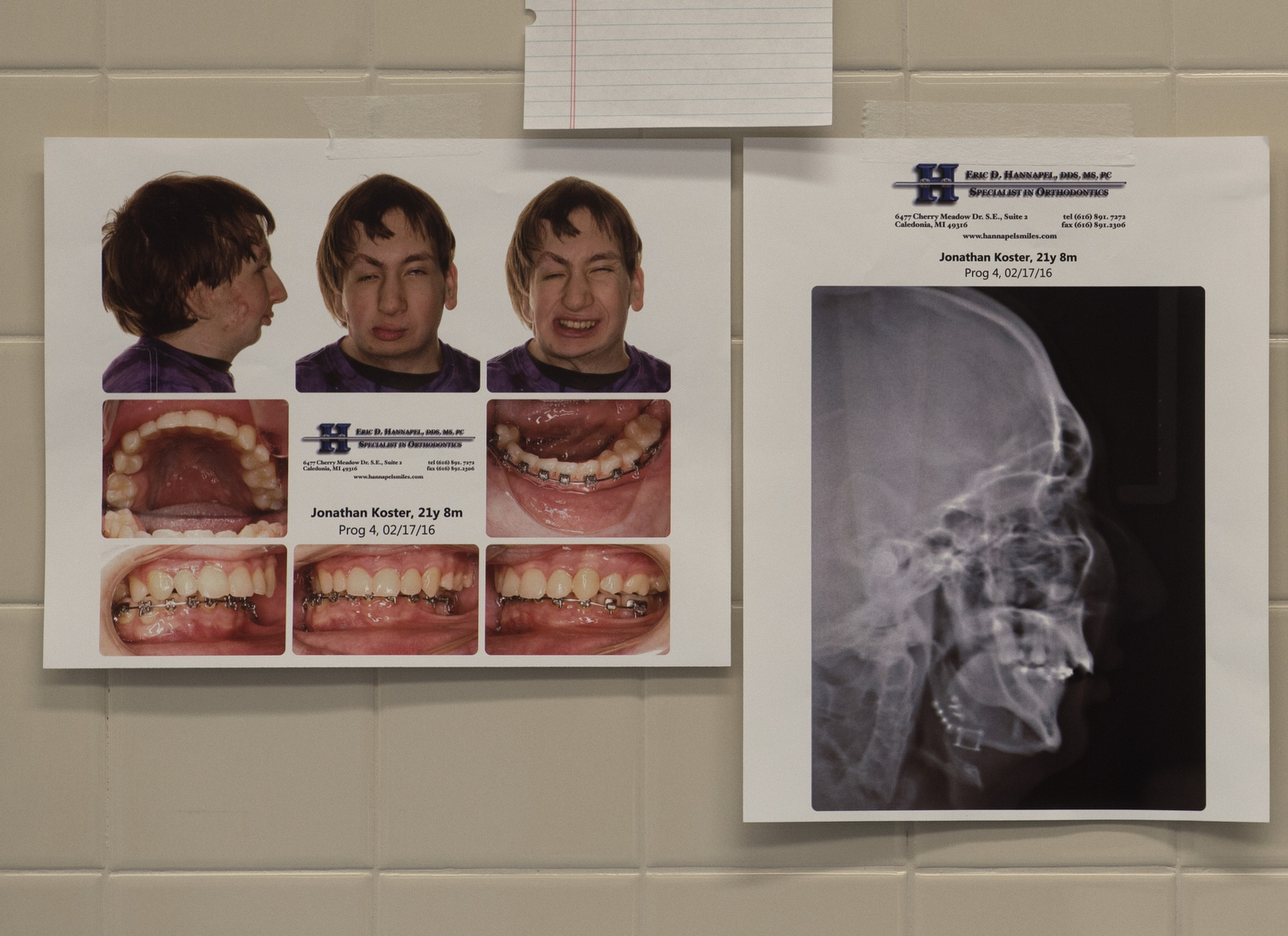
Until that moment, they did not know that one side of his face had not developed. He had no right ear, no right jaw bone.
But their beautiful boy had arrived into the world on a stream of prayers and longing. No birth defect could diminish their joy.
“I just asked the good Lord for one baby,” Deb says. She smiles proudly at Jonathan, now a young man who stands as tall as his mom.
The Kosters, who live west of Grand Rapids, Michigan, marvel at all the doors their son has opened for them, the people they have met through him and the medical advances they have witnessed.
That includes a recent development they once would have thought impossible―a titanium jaw for Jonathan.
For a unique person like Jonathan, you need a unique solution.
John Polley, MD, and John Girotto, MD, pediatric craniofacial plastic surgeons at Spectrum Health Helen DeVos Children’s Hospital, designed the prosthetic jaw to fit Jonathan’s unique facial structure.
The surgeons believe it’s a rarity—one of the first custom jaw implants created for someone born with hemifacial microsomia. That’s the name for Jonathan’s birth defect―a condition in which the lower half of one side of the face is underdeveloped. Because Jonathan never had a right jaw bone, the surgeons could not use a standard replacement joint.
“For a unique person like Jonathan, you need a unique solution,” Dr. Girotto says.
“He did great with it,” Dr. Polley adds. “It’s the best result that I’ve had with these severe grade 3 hemifacial microsomia patients in my 28-year career, so we are very excited about this technique.”
Jonathan, a veteran of 25 operations, takes the fuss over the new jaw in stride.
“It’s different,” he says.
An outgoing young man with an active social life, he would rather talk about his busy summer―which includes a week at a family camp for kids with special needs, a fishing trip with Dad and pool parties.
“I have so much that I can do,” he says. “I am a very good organist and pianist.”
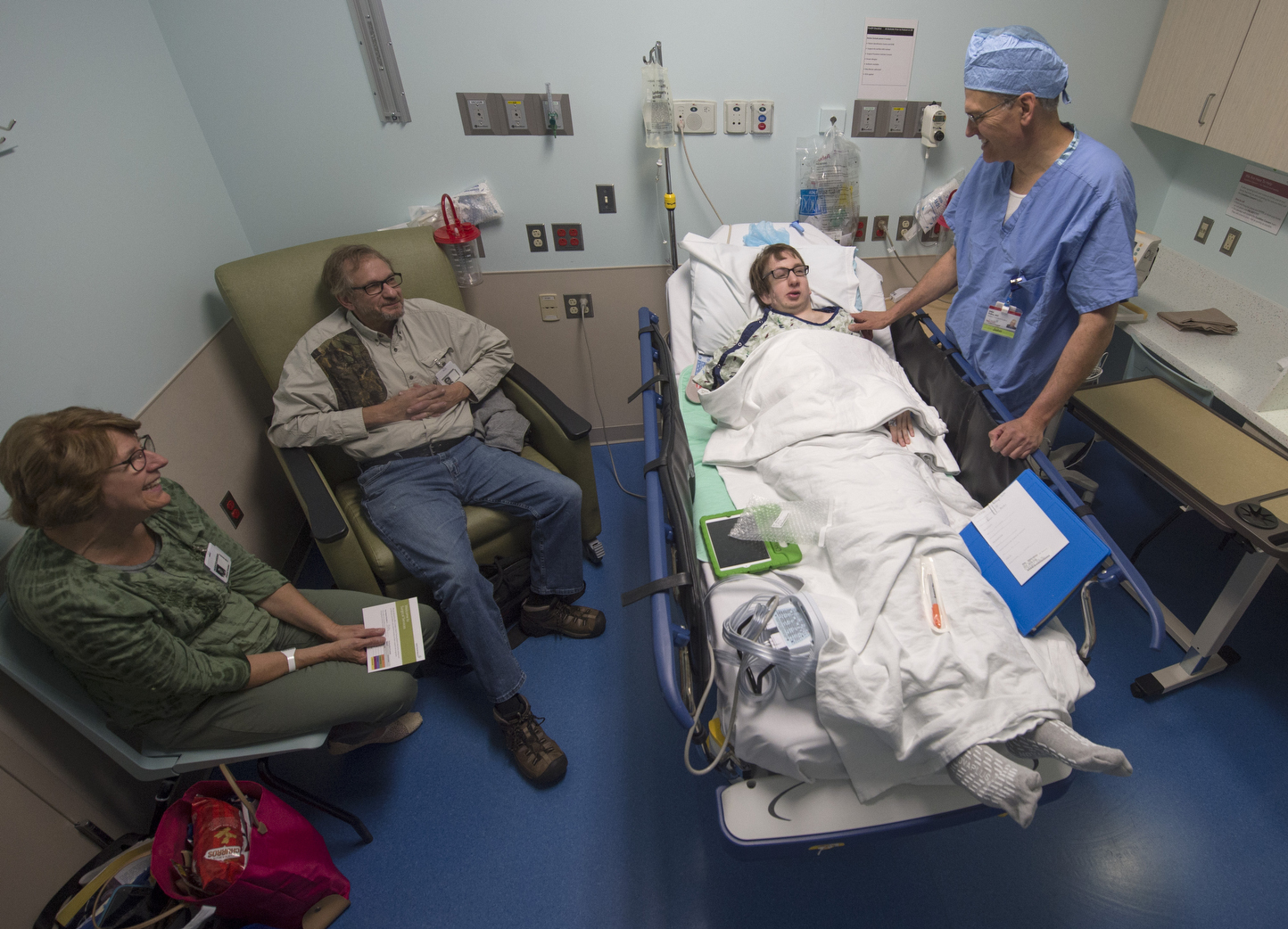
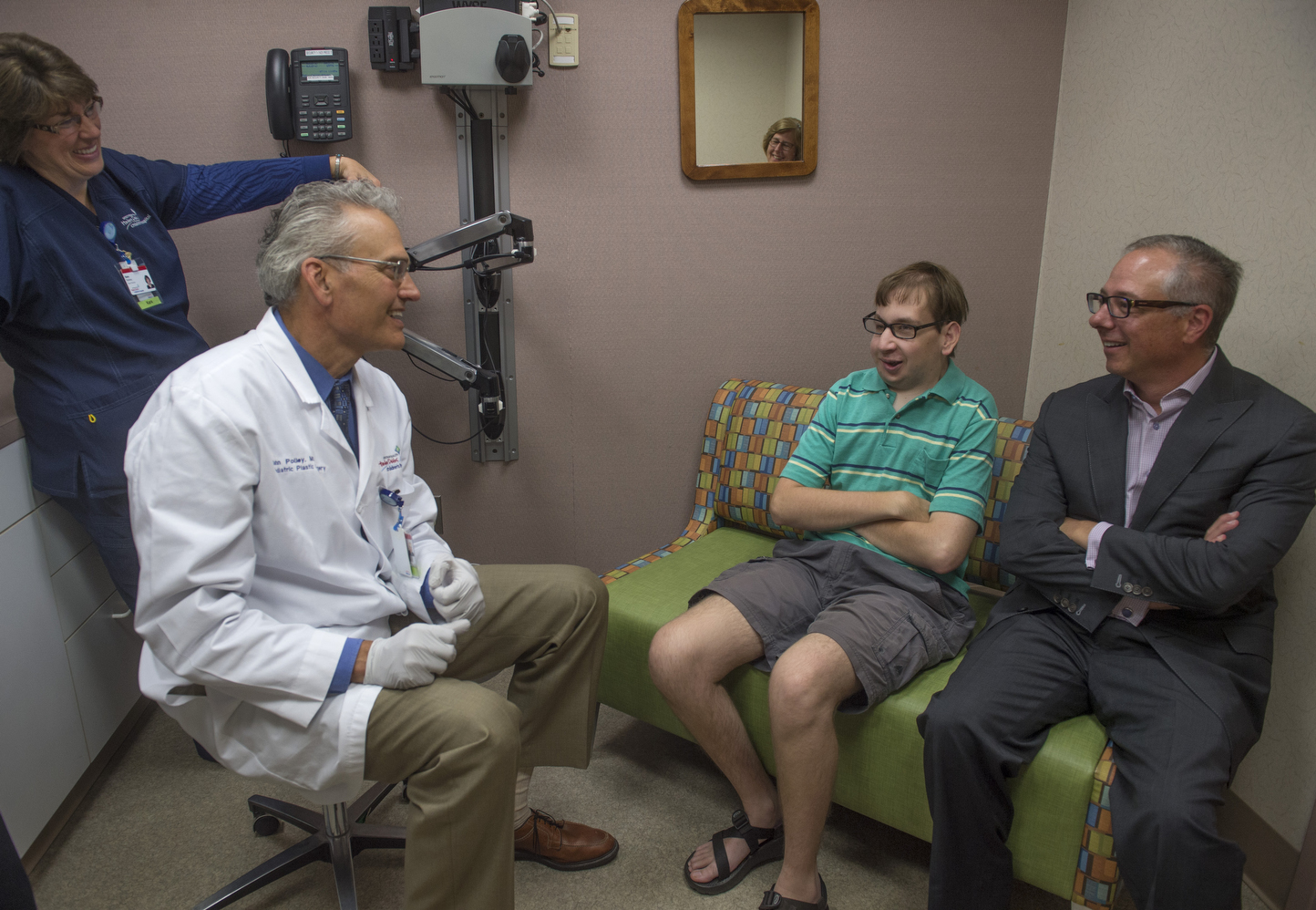
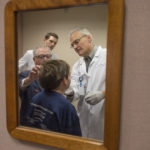
He poses for a photo with the doctors, sitting between them on a bench in an exam room, arms folded. A dream team. Tough and ready.
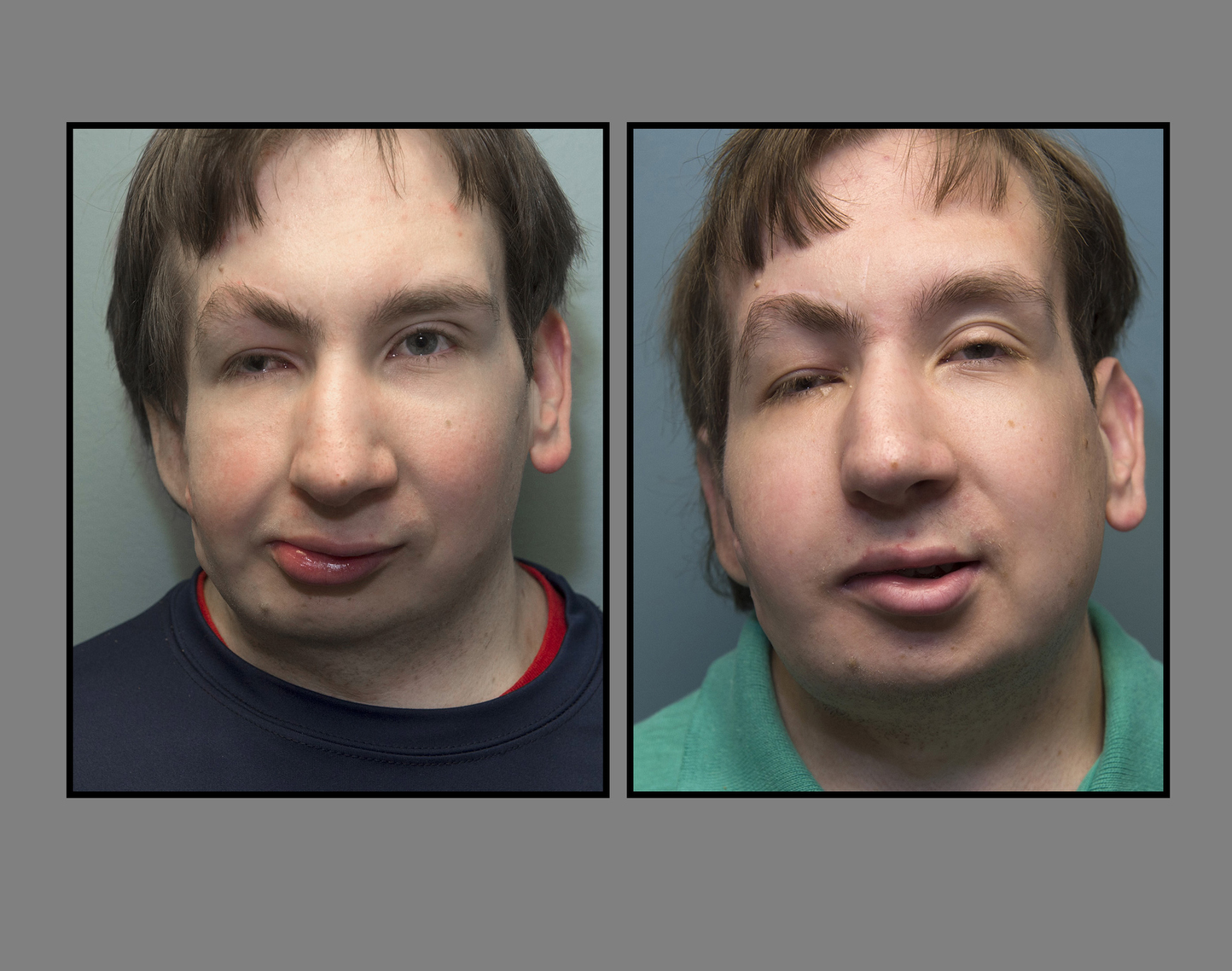
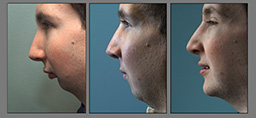
His parents appreciate the changes they see―how the new jaw makes it easier for Jonathan to eat and gives symmetry to his face.
“He’s got a nice straight smile, and his chin has come a long way,” Mike says.
Not expected to live
Deb, a licensed practical nurse, and Mike, a retired firefighter, dealt with fertility issues for a decade as they sought to start a family. They eventually decided to try in vitro fertilization. In 1993, at age 38, Deb had five eggs implanted.
“Just one took,” she says. “It was such a miracle right there.”
If we have him for 10 days or one year or a lifetime we will treasure whatever time we have.
But even as they eagerly awaited their first child, more troubles surfaced. Ultrasound scans showed their baby had hydrocephalus, a buildup of fluid in the skull. Doctors said there was so much fluid that they could not see a brain.
They didn’t expect their baby to live. If he did, he might survive only a year, they said.
Deb cried every day during the last month of pregnancy. She and Mike shared the grim news with only a handful of friends and family.
They hoped that medicine would have some answers for their child. And they prayed.
“Our faith was what we leaned on,” Deb says. “That’s what got us through.”
They decided to focus on the gift of each day. Mike summed up their attitude: “If we have him for 10 days or one year or a lifetime, we will treasure whatever time we have. It’s whatever the good Lord gives us.”
The operating room teemed with medical personnel when Jonathan was born on June 12, 1994, by cesarean section. He weighed 8 pounds 1 ounce. He had a full head of dark hair. To his parents’ joy, he could breathe.
Deb got to hold him for a minute.
“It was just wonderful. It was just unreal,” she says. “I could not believe that he really made it and he was breathing on his own. I felt so blessed that he was alive.”
Four days later, Jonathan underwent his first operation―a surgeon placed a shunt in his brain. With the excess fluid drained, his brain became visible on MRIs and CT scans. The Kosters excitedly asked doctors what that meant. What would their son be able to do and learn? No one could give them any answers.
‘A good heart’
Jonathan needed extra help from the beginning. Because of a cleft palate, his parents fed him with a tube for the first year.
He started special education services at 5 months. He reached developmental milestones later than most kids. But still, the milestones kept coming.
“We were amazed,” Deb says. “He would sit up. He would stand. I didn’t care if he was 3 years old and wasn’t walking―he was standing. And then the next year, he was walking. That was just huge.”
Doctors determined a stroke in utero likely caused the birth defects to his face.
Jonathan underwent surgery once or twice every year, and most of the operations were on his face. Robert Mann, MD, a pediatric craniofacial surgeon at Helen DeVos Children’s Hospital, repaired his cleft palate, improved his right jaw using cartilage from his ribs and created an ear so he could wear glasses comfortably.
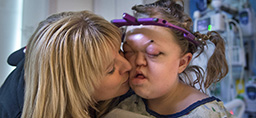
Jonathan made friends everywhere he went. At school. At camp. And especially at Twelfth Avenue Christian Reformed Church.
“His personality really blossomed at church,” Deb says. “He’s everybody’s buddy. And the church just surrounded him every step of the way.”
When Jonathan turned 11, the church organist began giving him piano lessons. And a musician was born. Jonathan now plays a full repertoire of hymns on the piano and organ and practices every day.
At home, Jonathan helps his dad with yard work.
“I like mowing the lawn,” he says.
Under Dad’s supervision, he takes friends on rides on an all-terrain vehicle, bouncing along a path mowed in the tall grass.
“This is where it gets fun,” he says as he zips around a curve.
Jonathan continues with his education, attending the Community-Based Instruction Program at the Ottawa Area Center. Through school, he volunteers at Sunset Manor, an assisted living facility in Georgetown Township. Once a week, he teaches an exercise class. And then he sits at the piano and plays hymns.
“This is my favorite,” he tells his audience on a recent morning. “So we’re going to sing all the verses.”
He launches into an enthusiastic rendition of “How Great Thou Art.”
“He really has a good heart,” Mike says. “He loves helping people out.”
Looking ahead, Deb can see Jonathan “in a performing mode.” The volunteer work might open the doors to employment. And that’s one reason for her interest in the prosthetic jaw implant.
“I’m thinking down the road, if he gets to perform in different nursing homes, it’s wonderful that he’s got a straight face,” she says.
A computerized solution
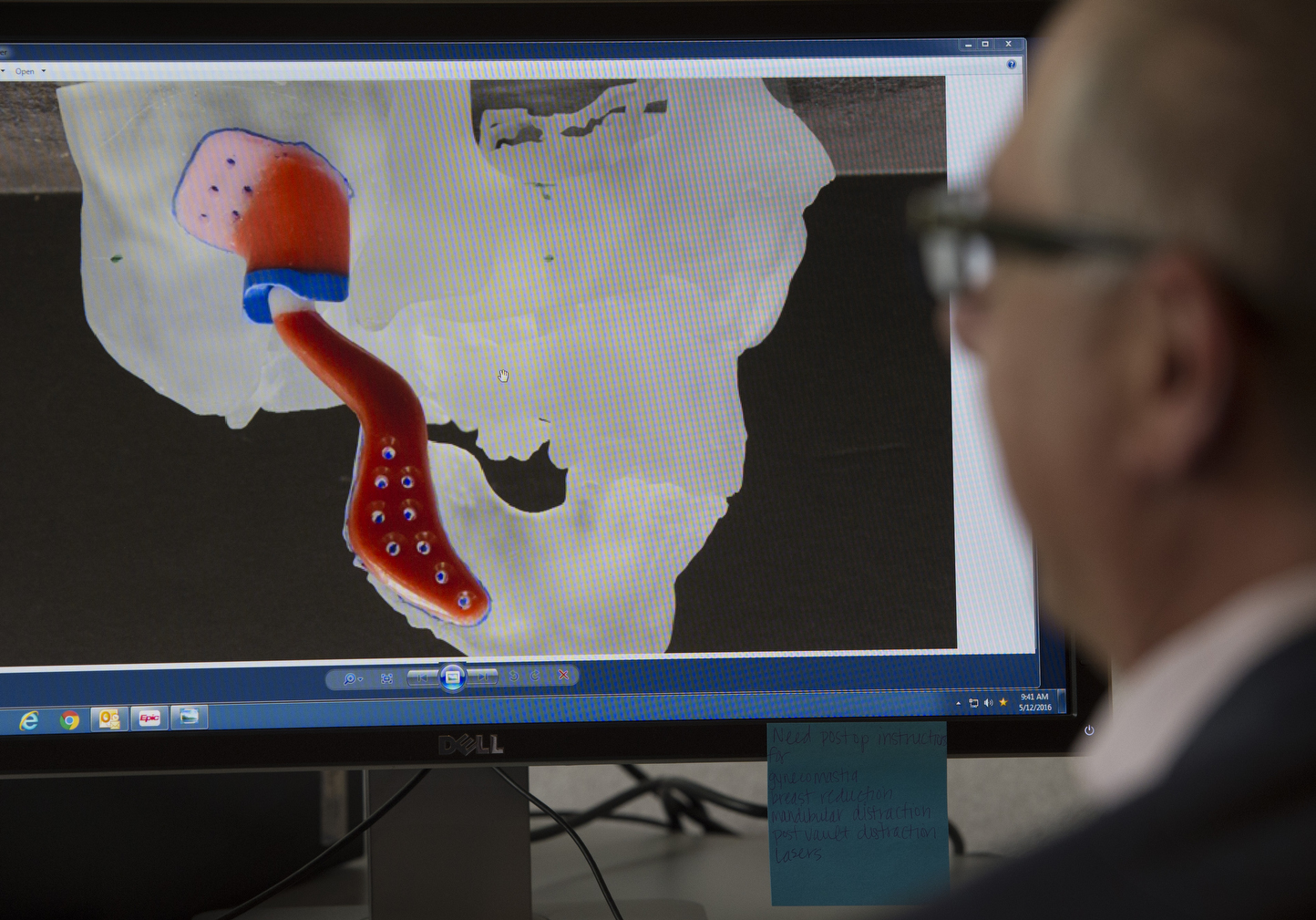
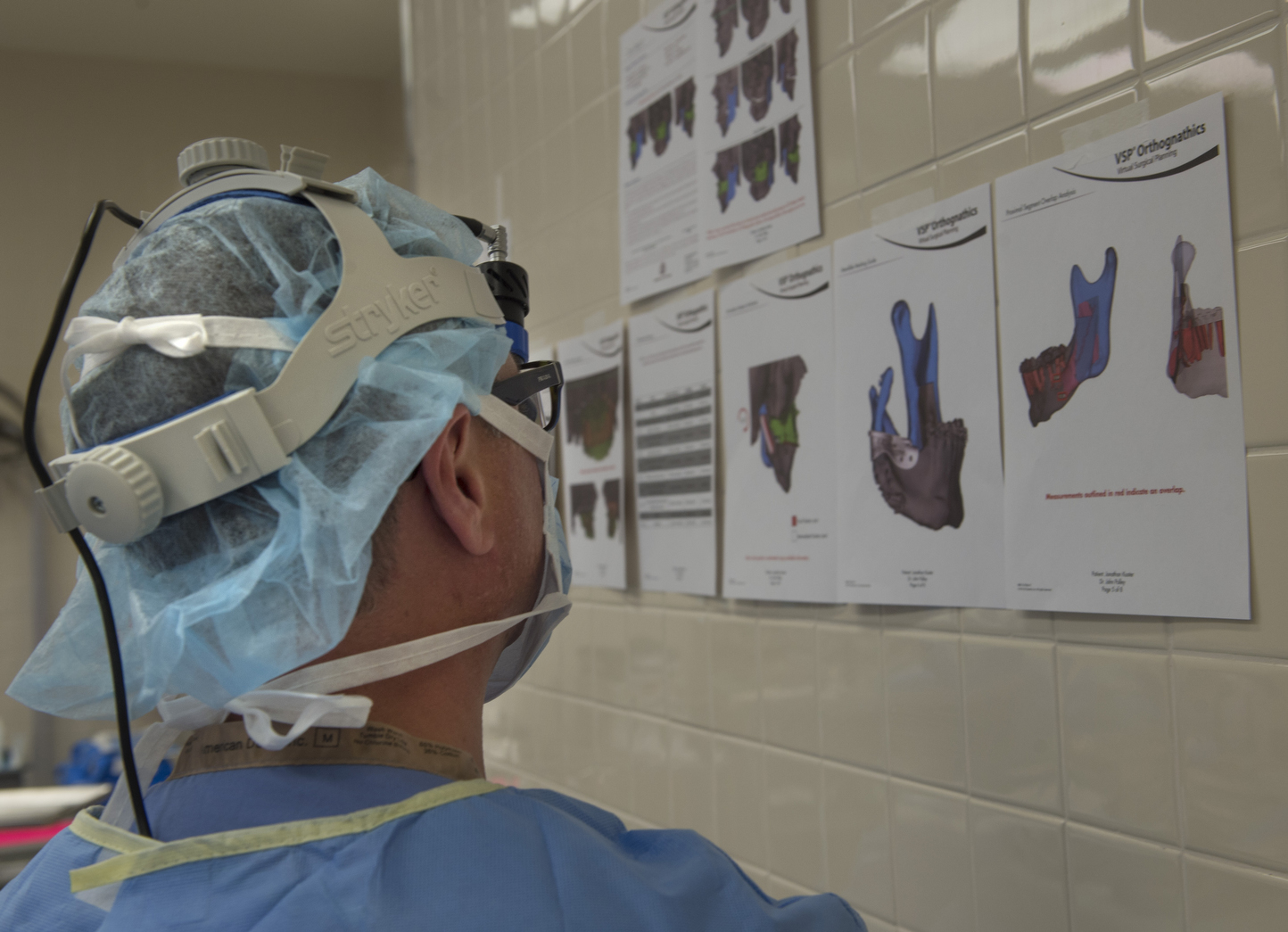
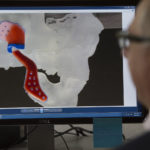
To design the implant, the surgeons used CT scans of Jonathan’s face to perform a virtual surgery on the computer. That allowed them to determine the dimensions for the missing jaw bone.
I can’t believe this is really him. I could have cried.
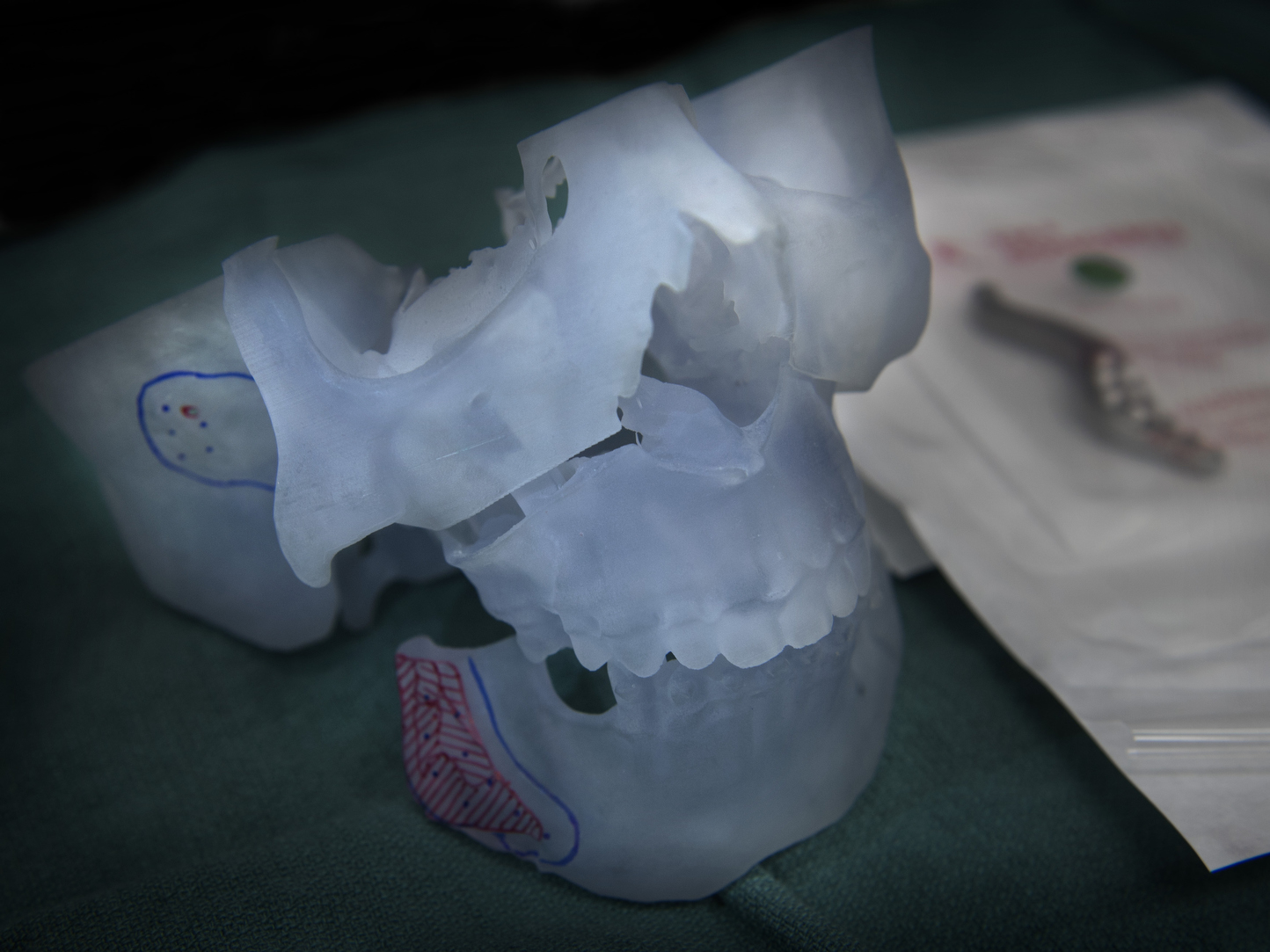
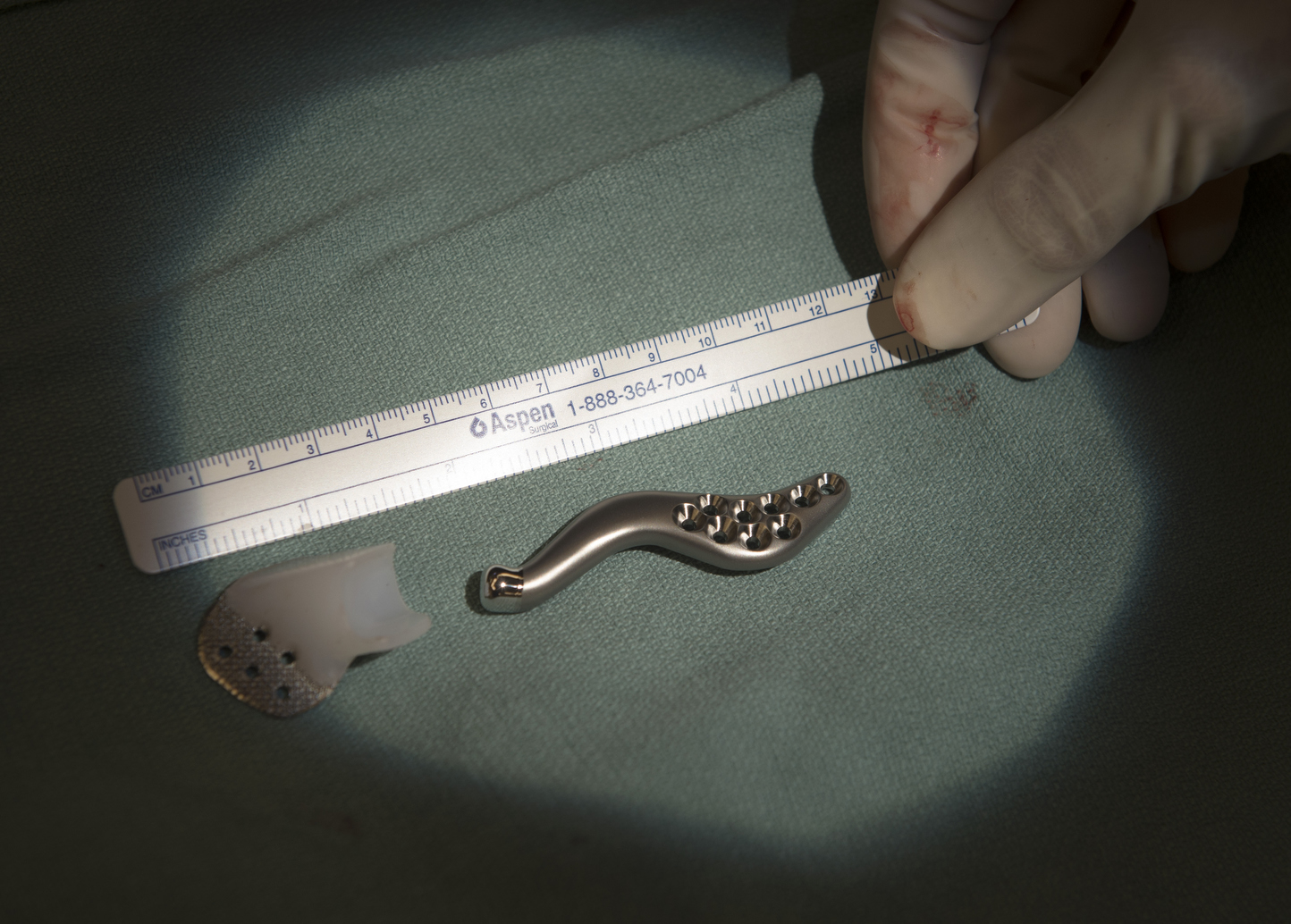
Using that data, TMJ Concepts in California fabricated a silicone socket with a titanium bone. And they printed a 3-D model of Jonathan’s facial structures―a clear plastic skull that showed where the implant would fit.
The computerized design allows for a precise fit, the surgeons say.
“They actually engineer each screw depth to match the bone thickness,” Dr. Girotto says.
“In the old days, we went in and we kind of knew what we wanted to do, but we never knew 100 percent because we didn’t have the accuracy,” Dr. Polley says. “Now, we are really accurate down to about a millimeter or so. When we go in now, it’s really just execution, getting everything to fit.”
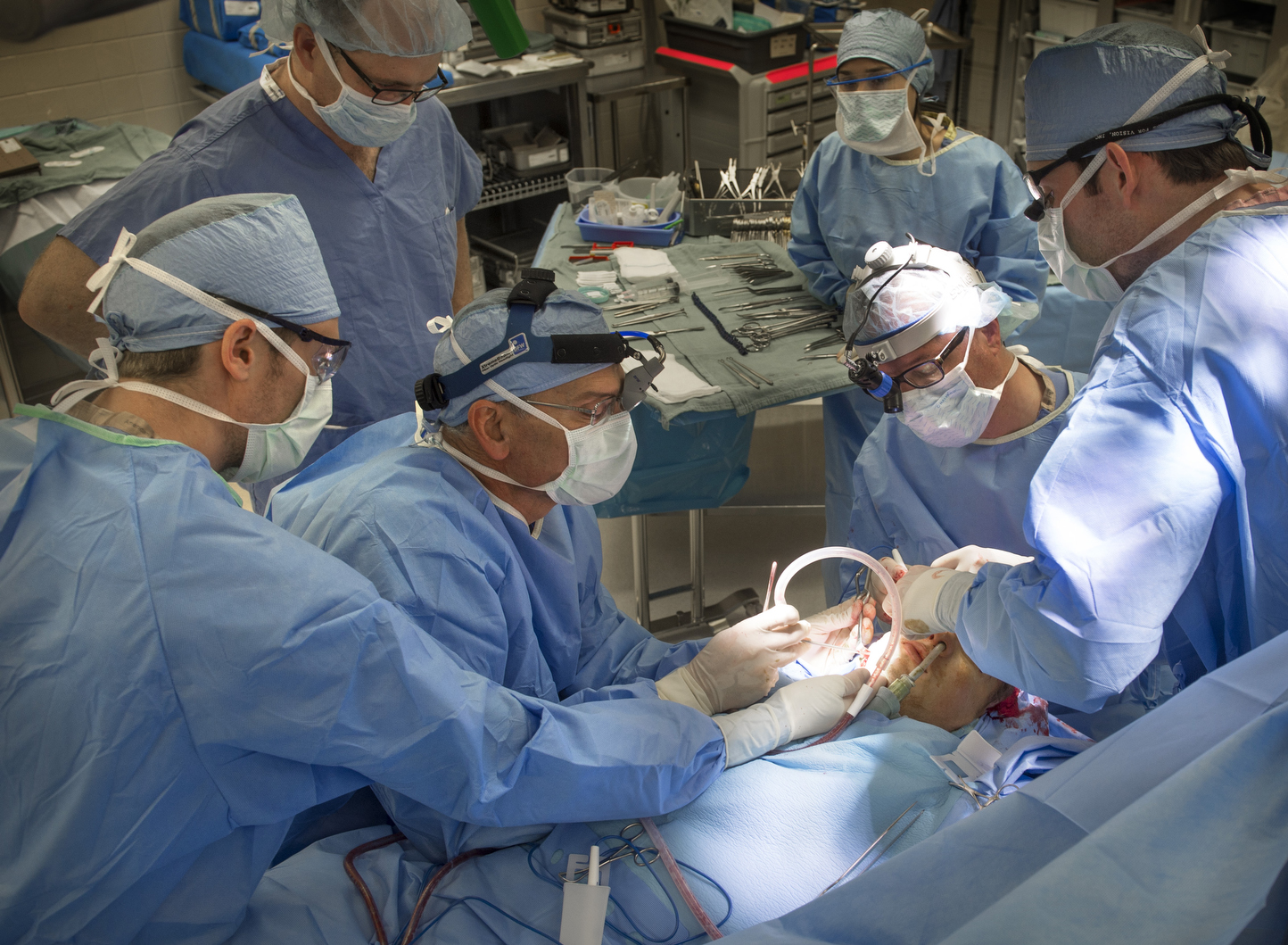
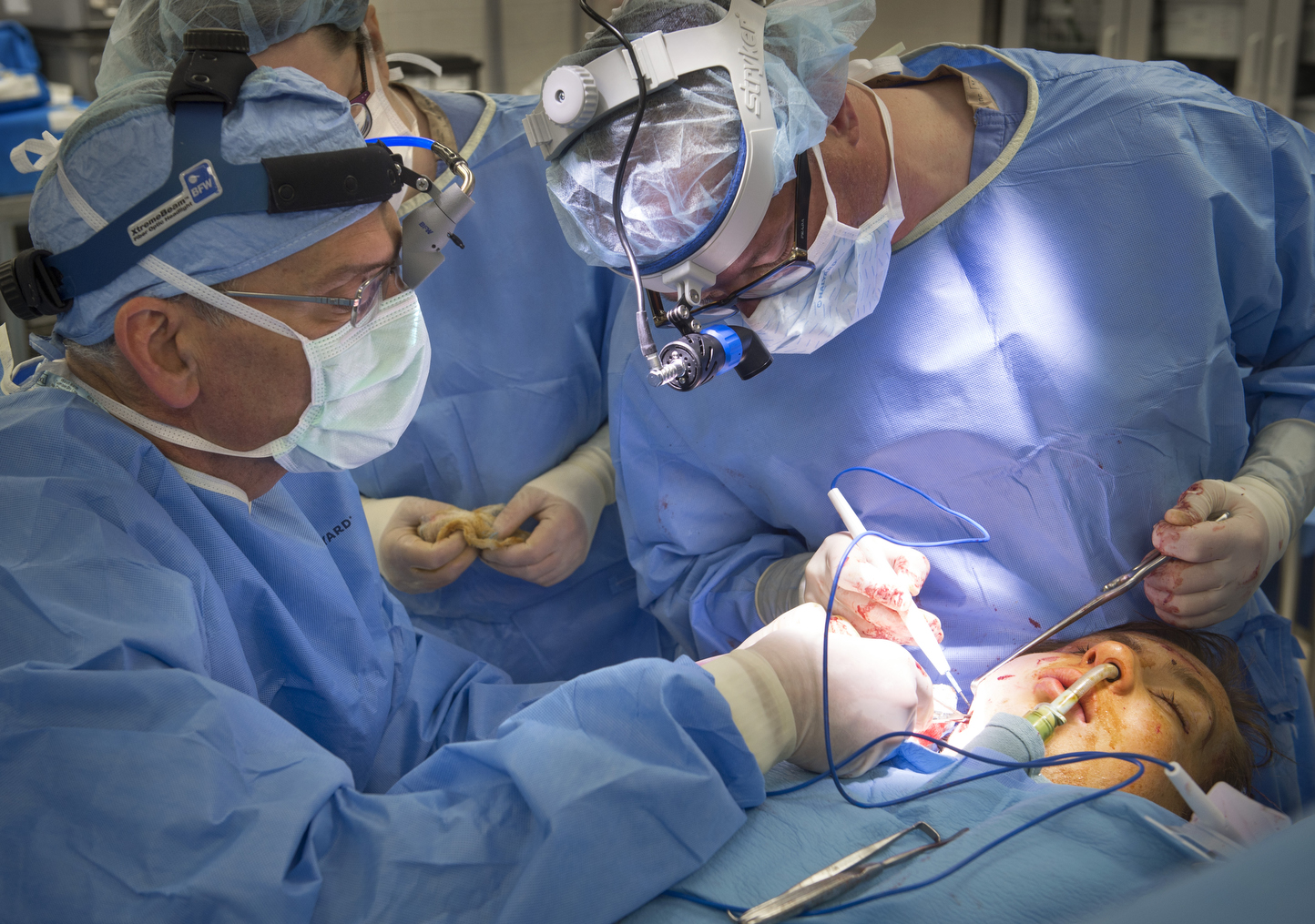
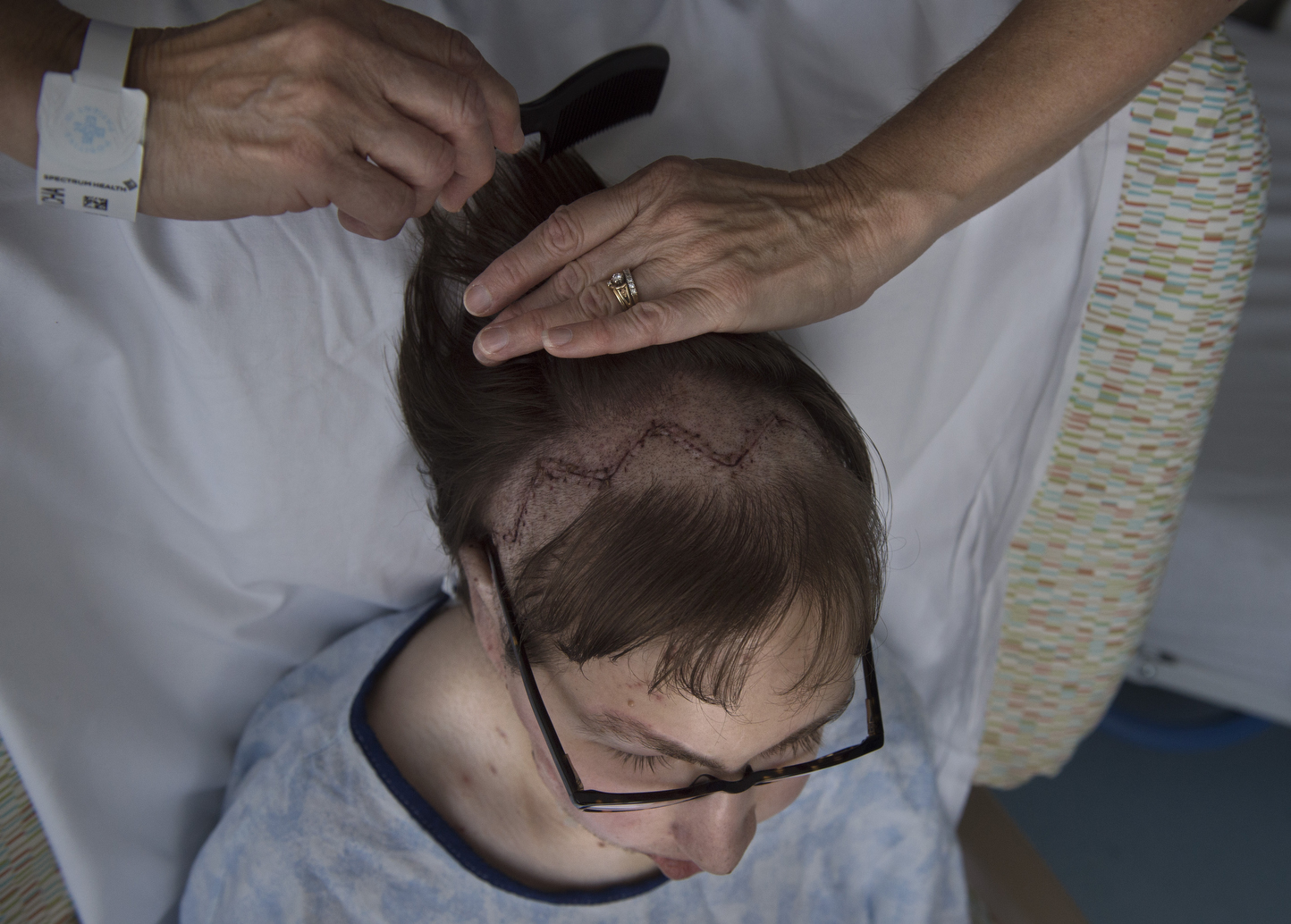
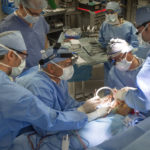
On May 27, Jonathan received the implant in an eight-hour operation at Helen DeVos Children’s Hospital. The surgeons operated on both his upper and lower jaw to move them to the midline position. They then secured the titanium bone and joint in place.
For the next two weeks, Jonathan’s jaw remained wired shut and he had to stick to a liquid diet. That was the toughest point of the process, his mom said. She wanted to make sure he consumed enough calories, but Jonathan grew tired of protein-powered milkshakes.
‘Blessed’
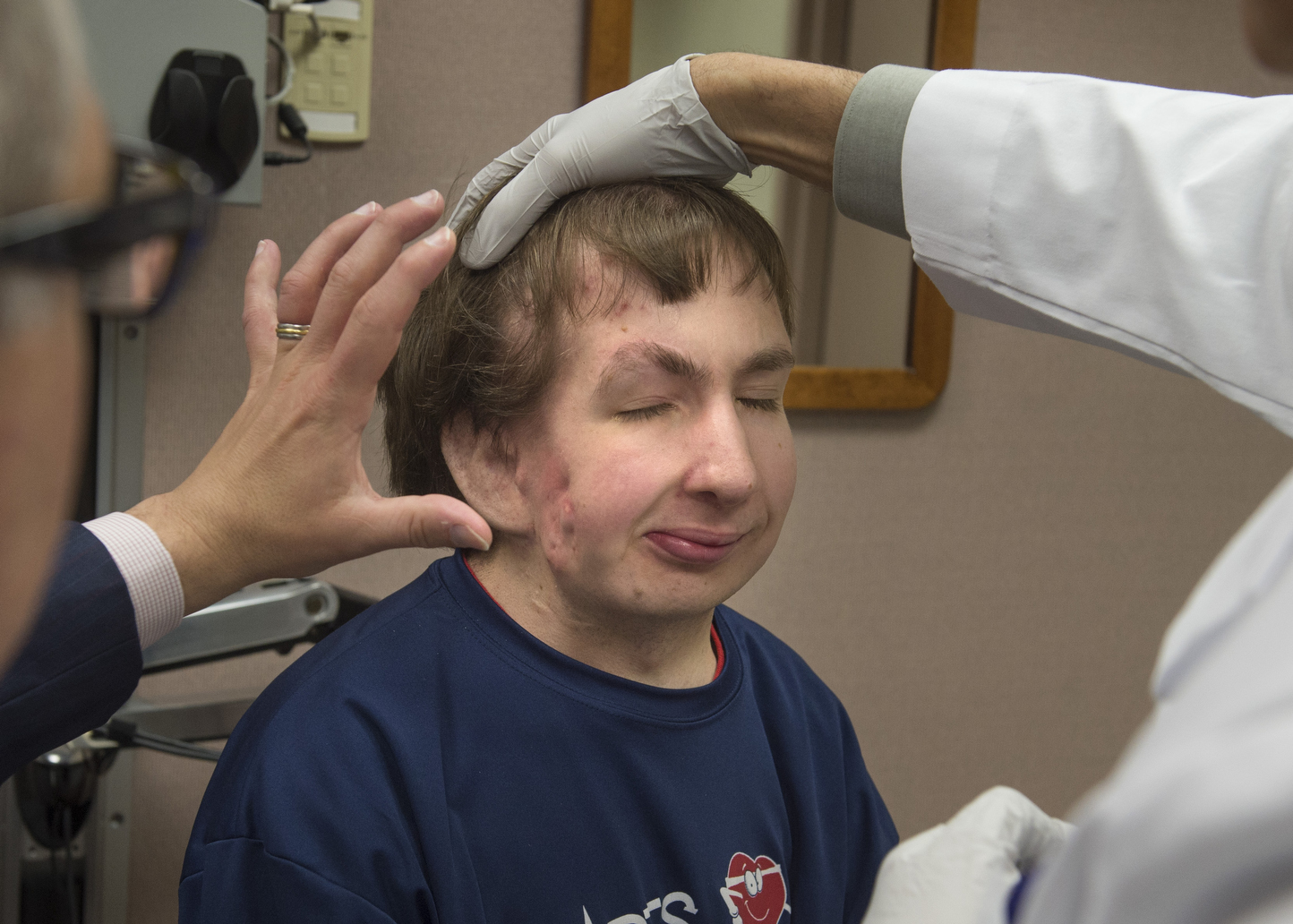
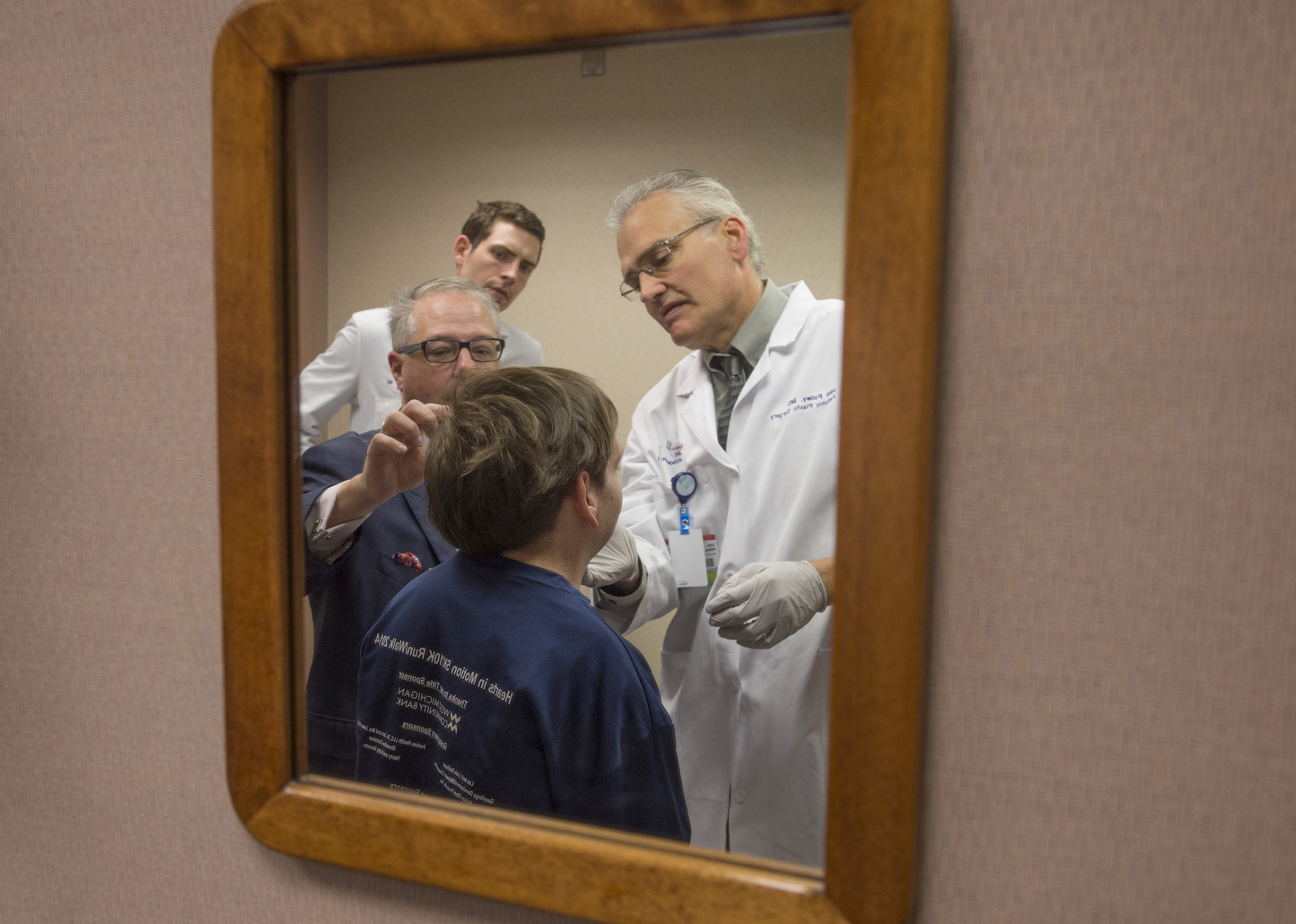
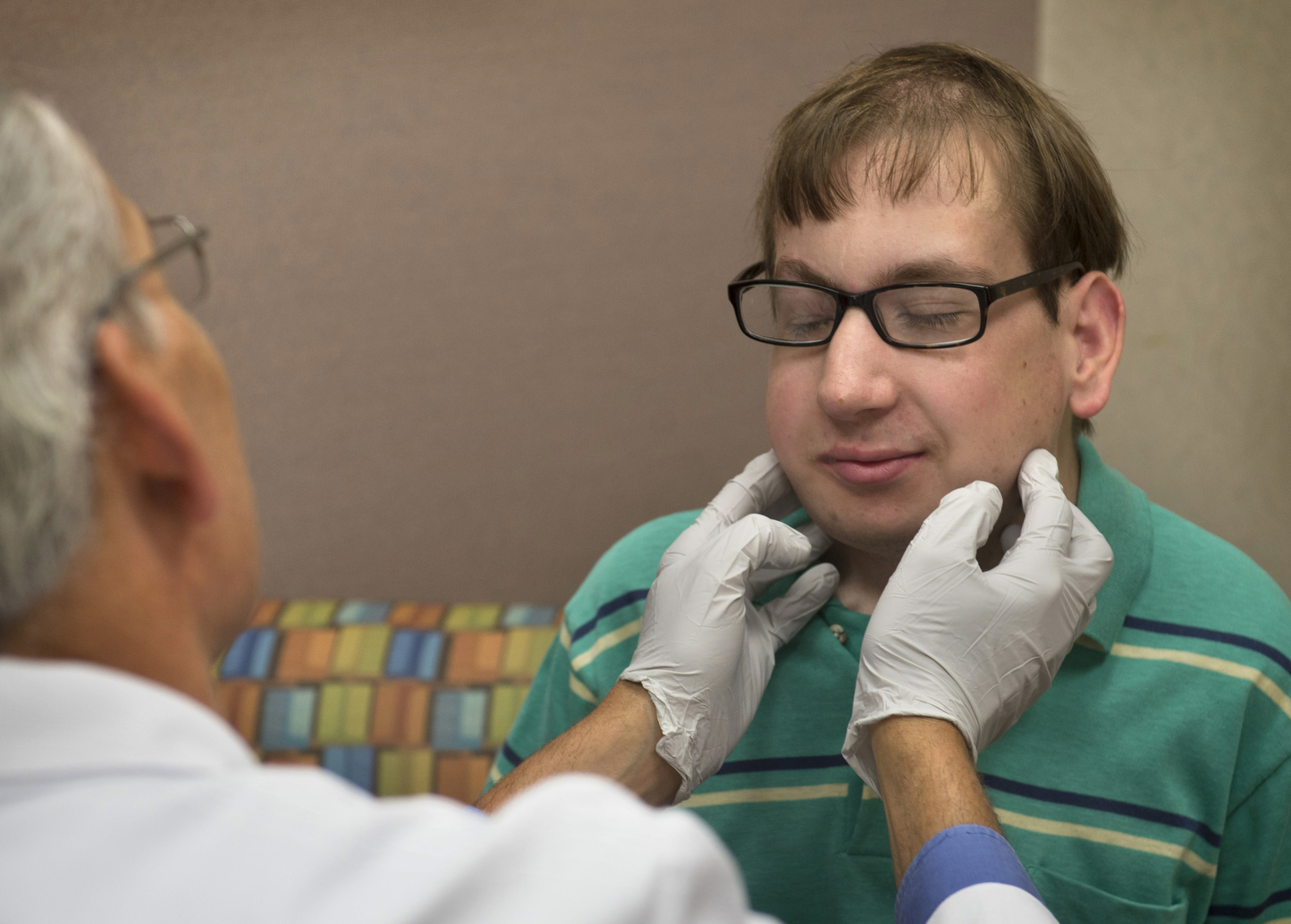
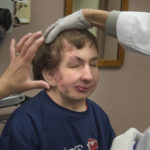
Six weeks after surgery, Jonathan smiles as he shakes hands with Drs. Girotto and Polley at a follow-up appointment.
Dr. Polley examines the new jaw. He notices how Jonathan’s features now fall into alignment. He encourages him to keep up with the exercises to open and stretch the jaw.
“You look great,” he says. “You look really good.”
At home, Deb notices gradual changes in Jonathan’s eating habits. In the past, she would cut up his meat into tiny pieces. But with his teeth in alignment, he tries a wider range of foods―including a bacon cheeseburger.
And she notices the symmetry of his face. One day recently, as Jonathan tells her about something, she is more captivated by his face than his words.
“He’s eye to eye with me and I’m looking at his face and I am thinking, ‘Oh, my word. Your face is so straight,’” she says. “I can’t believe this is really him. I could have cried. I thought, ‘Oh, wow. That is amazing.’”
Jonathan shrugs when asked what he thinks about the implant. He knows it’s a big deal. And he knows a lot of people love and care about him. Asked why, he smiles and looks a bit embarrassed.
“I don’t know,” he says. “I am blessed.”


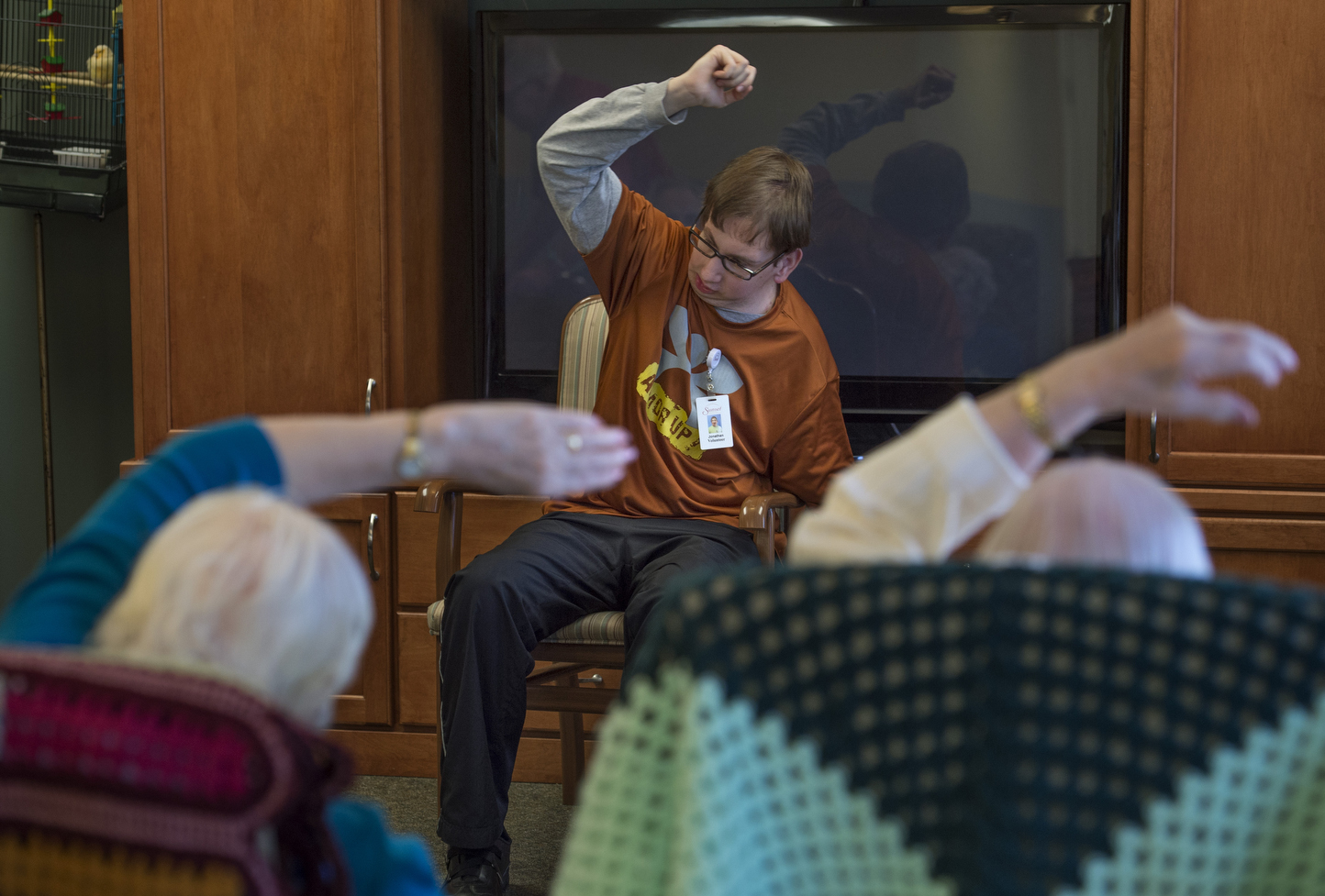












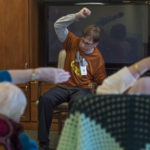





















 /a>
/a>
 /a>
/a>
 /a>
/a>
What a beautiful story! thanks so much for being so open to sharing 🙂 God has done some amazing work in this young man’s life, praying it continues!
Thanks for your comment, Stephanie. It really has been an honor to get to know Jonathan.
Amazing Grace for your son Mike. Continued prayers for your son and family.
Jonathan, your story is amazing and so are you!! So happy you have shared it and so thankful for the abilities God has given to your doctors to be able to perform the procedure with such accuracy. Keep on being the wonderful, young man you are, trusting God for continued blessings. We love you.
Thank you so much for reading this article, Tom and Sharon Visser!
Thank you for sharing your story, Jonathan! You’re an inspiration to many. Best, Cheryl (Health Beat’s editor)
Blessings all around! ❤️
Indeed!
Thanks for reading. And please share this story and Health Beat!
Wonderful story! Thank you for sharing your life story. You are an amazing young man Jonathan!
Beautiful, inspirational story. Thanks for sharing. God bless!
Jonathan you have a amazing life ahead of you. God has blessed you.
Jonathan, I feel so honored to know you. You are a true example of a wonderful Christian young man. You have been through so much but yet you are just happy to be you. You are a fighter and I am so glad that God blessed you with this surgery.
Jonathan, I am crying as I read your story! I remember the phone call I got from your Mom when she was pregnant with you, and were those doctors ever wrong! But God was right……He knew exactly what He wanted to do with you, and He has made you a blessing to everyone around you! To God be the Glory! Great things He has done! Love, Mike & Sharon, Jon, Michelle, & Nicole Van Oyen
Jonathan, you are indeed blessed to have these gifted doctors be creative with their skills. You are a real miracle. God’s blessings on you to be a blessing to others, especially with your music abilities.
Jonathan, you are indeed blessed to have these very talented and gifted doctors perform a miracle. God’s blessings on you to be a blessing to others, especially with your music abilities. Who knows what God has planned for you now!!
Oh Jonathon. Kris and I are so happy for you. All those years at SNW as we watched you get new facial surgeries. The most exciting year was when you got your ear. I will never forget the joy of that. God is truly good.
It’s wonderful to see all these comments. Jonathan clearly has touched a lot of lives.
What an amazing young man and how blessed are we to have HDVCH and such amazing professionals in our community!
Wow! Deb,I loved this! I saw this on my phone. This is wonderful for Jonathan. I know what you and Mike have gone through since his birth. Hope to talk to you again.