Peace out, NICU.
Noah Markle, the youngest born survivor at Spectrum Health, is heading home.
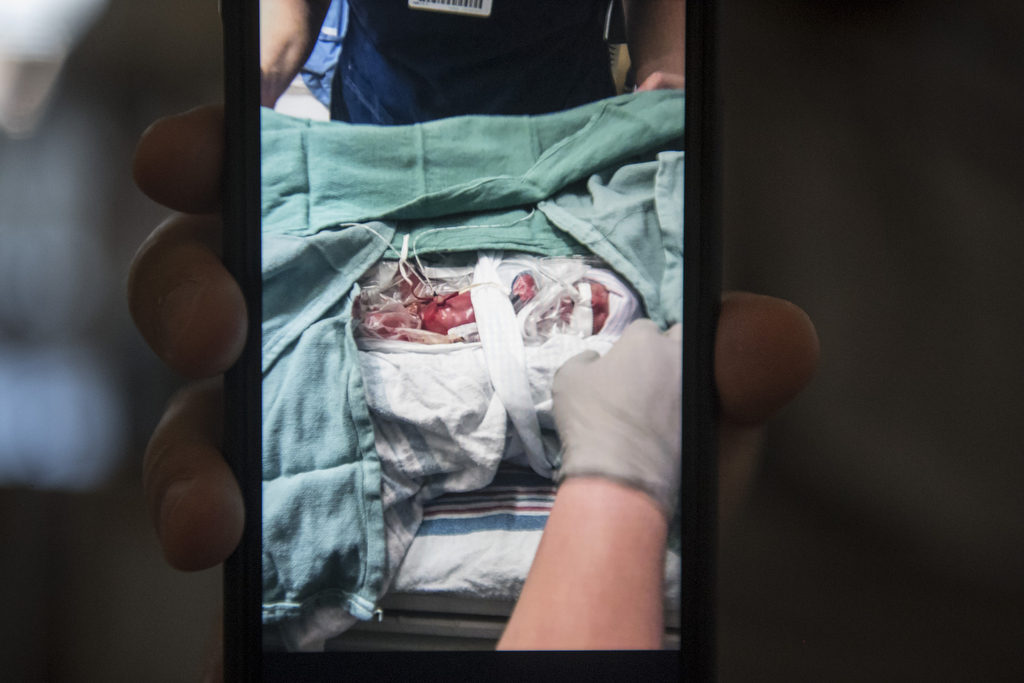
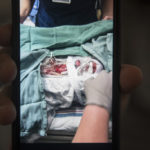
He made his debut on a winter day, after only 22 weeks and 4 days gestation, weighing a mere 1 pound, 4 ounces.
On a bright spring afternoon four months later, he checked out of the Helen DeVos Children’s Hospital neonatal intensive care unit—just one week after his official due date.
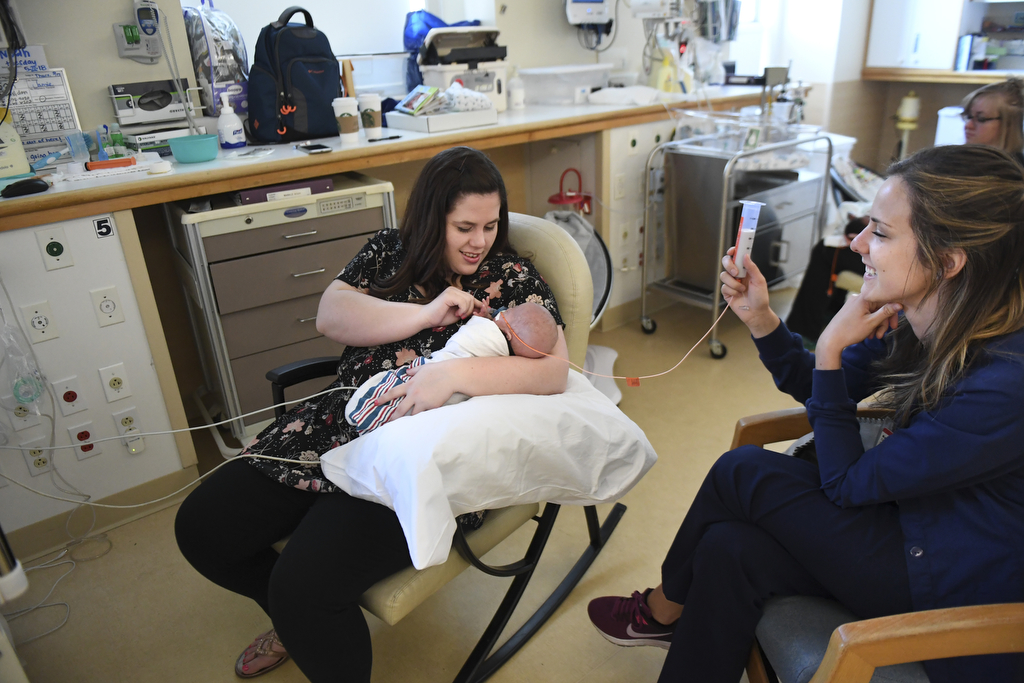
“It’s awesome,” said his mother, as she cradled her son, now a healthy 7-pound, 3-ounce chubby-cheeked boy. “MiracleMarkle is our hashtag.”
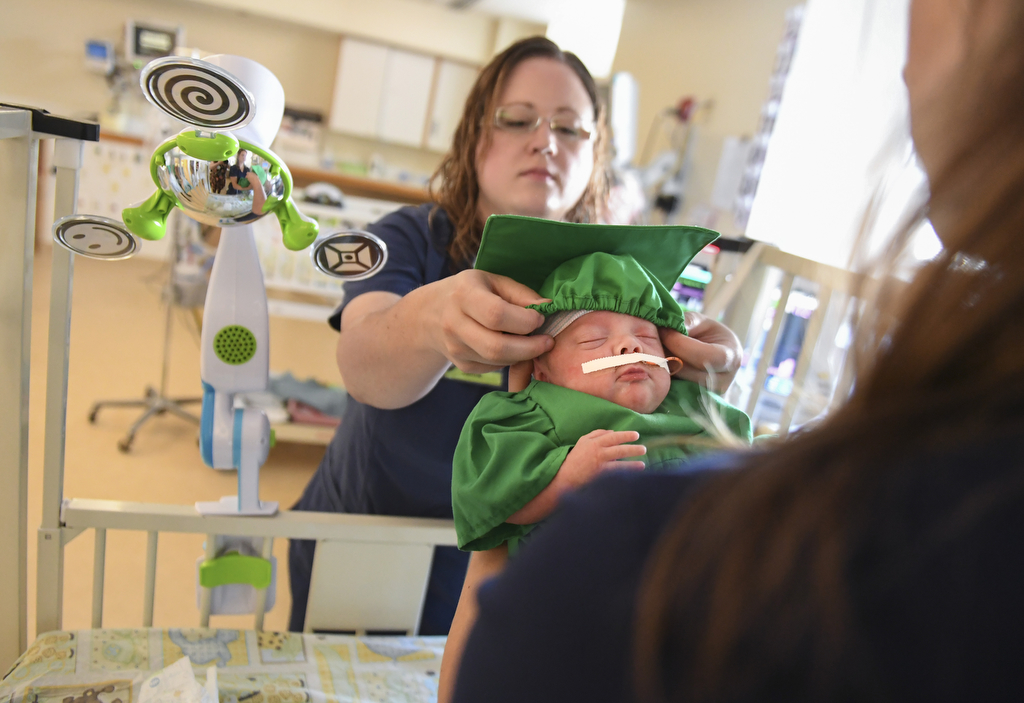
The nurses and doctors who nurtured Noah through this journey joined the celebration as Don and Rebecca Markle prepared for Noah’s NICU graduation. They hugged mom and dad and posed for pictures with Noah.
“Most of us who have cared for him could not have predicted this course,” said Benedict Doctor, MD, a neonatologist at Spectrum Health Helen DeVos Children’s Hospital. “He has done remarkably well.”
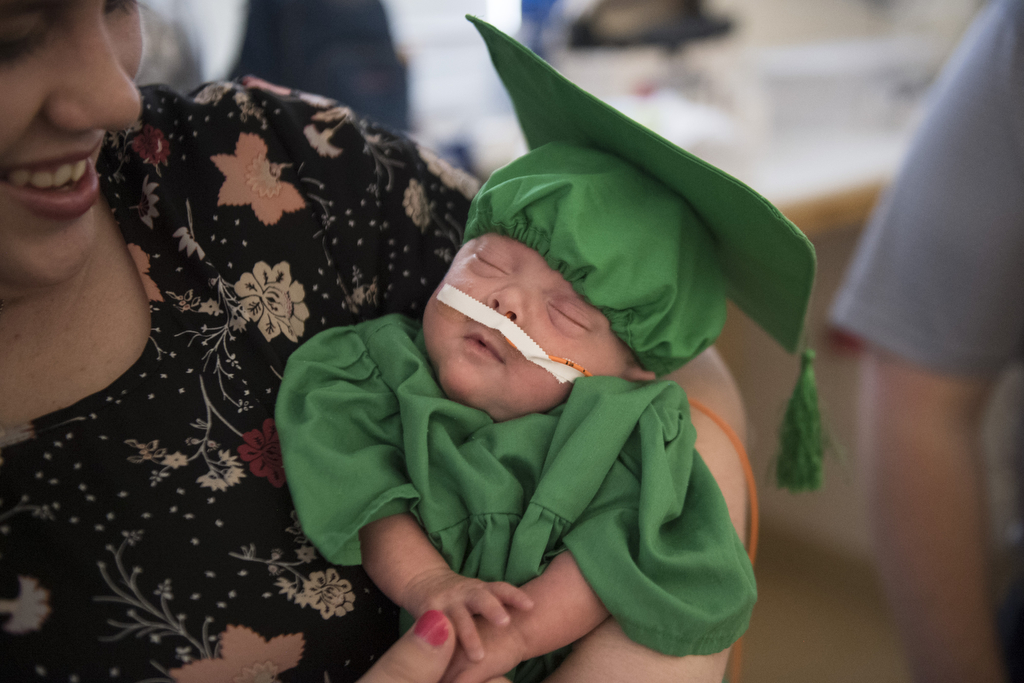
The star of the celebration seemed as mellow as the message on his blue onesie—“Peace out, NICU.”
He peered through one eye, opened both to look around a bit, squirmed and yawned. Then he closed his eyes and slept as peacefully as, well, a baby.
A source of comfort
Noah’s victory over his against-the-odds battle felt especially sweet to the Markles because they know the pain of loss. Before Noah, they had two babies who did not survive—their daughter, Gracelyn, born at 17 weeks, and their son Duke, born at 20 weeks.
When Rebecca learned of her pregnancy in August 2017, she sought care from Spectrum Health maternal fetal medicine specialists. She received treatment for a weak cervix, a risk factor for premature delivery.
And she worried.
“Every day being pregnant,” she said, “(I thought) ‘Is this going to be the day we lose him? Is this going to be the day we lose him?’”
He was so small. Like a little baby bunny.
At 20 weeks, she went on bedrest and received progesterone shots to help prevent early labor. But at a 22-week doctor’s appointment Jan. 5, it became apparent labor would likely start soon. Her doctors admitted Rebecca to the hospital.
Before birth, Noah received medications to improve his chance of surviving: antibiotics to protect against infection, magnesium to protect against cerebral palsy, and steroids to help his breathing and blood vessels in the brain, said Erin Fricke, MD, a maternal fetal medicine specialist.
Just one hour later, after a short labor, Noah made his entrance in the Family Birthplace at Spectrum Health Butterworth Hospital.
In the delivery room, Rebecca worried that, like his siblings, her new baby might not survive.
“I kept saying, ‘Is he moving? Is he alive?’” she recalled. “And he came out squirming.”
Noah went first to the warming bed, and Dr. Doctor placed a breathing tube. Other members of the NICU delivery room team helped establish breathing support and delivered therapy to his lungs. His vital signs stabilized.
“I was just like, ‘Praise the Lord,” Rebecca said. “I knew God had big plans for this baby.”
Dr. Fricke asked Don and Rebecca what name they had chosen for their son. They hesitated. They had not yet narrowed their list of favorite names to a single one.
“I said, “Uh, Noah,’” Rebecca said. “I looked at my husband, and he said, ‘Sure.’”
They later learned Noah’s name means “to comfort.”
“I think that’s just perfect,” Rebecca said. “He’s our healing.”
Beating the odds
Noah spent the next several months in the NICU’s small baby unit, which provides specialized care to “micro-preemies,” those born at 27 weeks gestation or earlier. The dimly lit, quiet room provides a low-stimulation, womblike environment that aids babies’ brain development.
“All of our care is done by two people,” said Kamera Daniel, RN.
As one person provides the needed care—such as a diaper change—the other provides comfort and support for the baby.
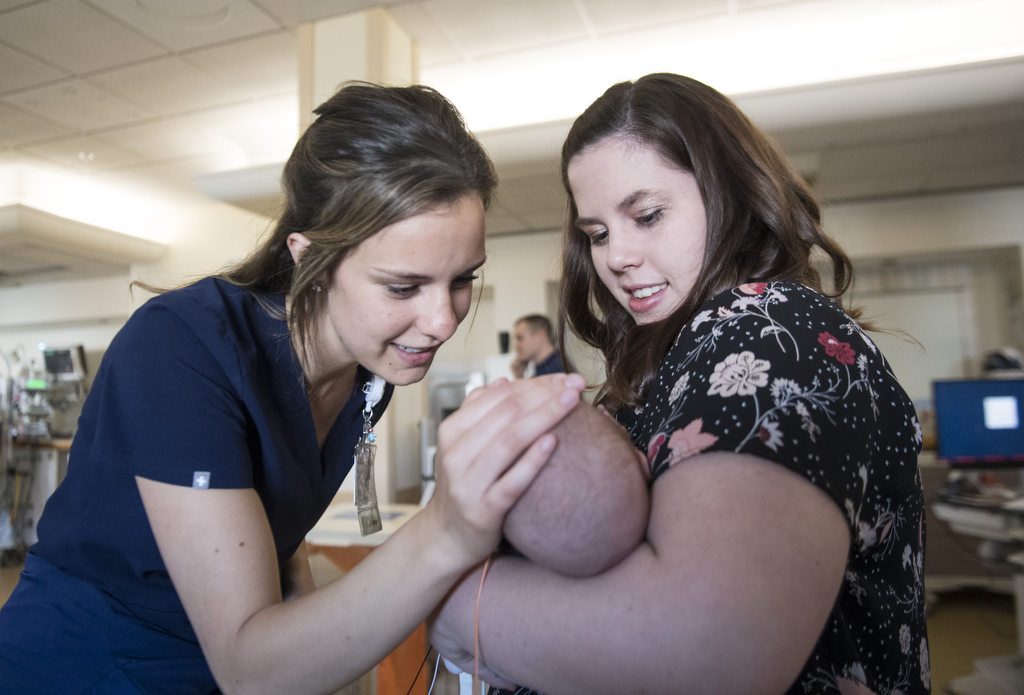
Thirteen days after his birth, Noah’s parents held him for the first time.
“He was so small,” Rebecca said. “Like a little baby bunny.”
He’s our hero. He’s not even 6 months old, and you can look up to him and say what a big fighter he is.
For a baby born at 22 weeks, the odds of survival are less than 10 percent, Dr. Fricke said.
Premature babies can have a number of life-threatening complications, such as brain bleeds, problems with the digestive tract, breathing and heart issues. Despite some rocky moments, Noah avoided major complications.
“He has grown really well,” Dr. Doctor said. “When babies are really sick, it’s hard to get them enough calories to keep them growing. But his growth has tracked along normally the entire time.”
Noah’s size at birth may have helped his survival. Although 1 pound, 4 ounces sounds tiny, “that’s a pretty big size for a 22-week baby,” Dr. Fricke said.
She held Noah in her arms on his NICU graduation day and smiled down at the blond, brown-eyed boy.
“This is so, so awesome,” she said. “I’m so incredibly happy for you guys.”
Hero baby
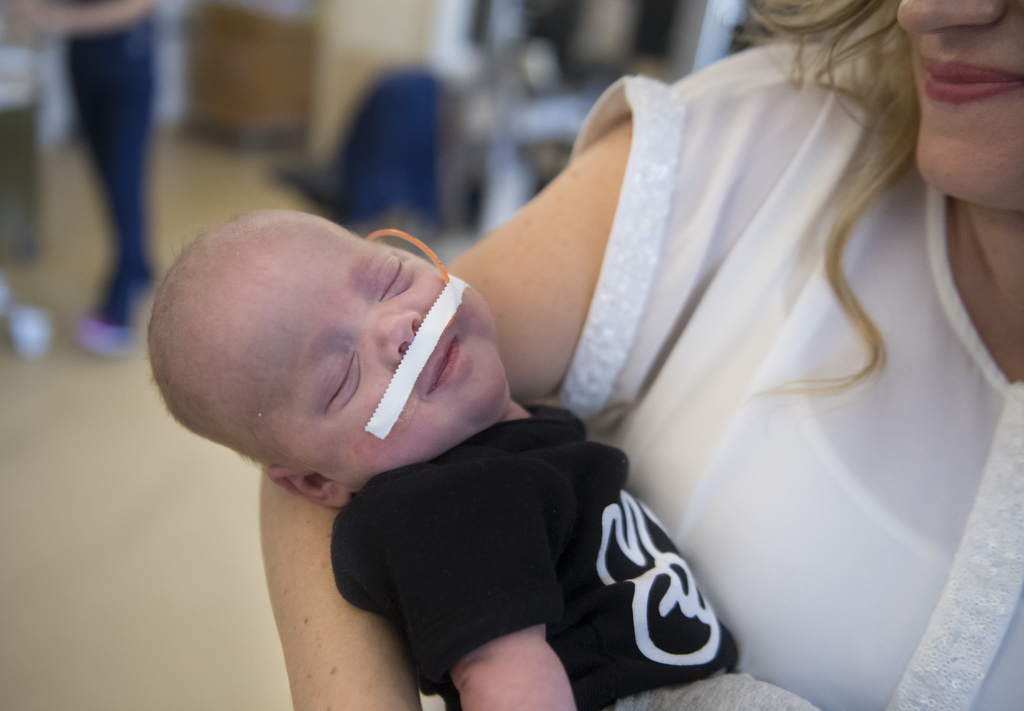
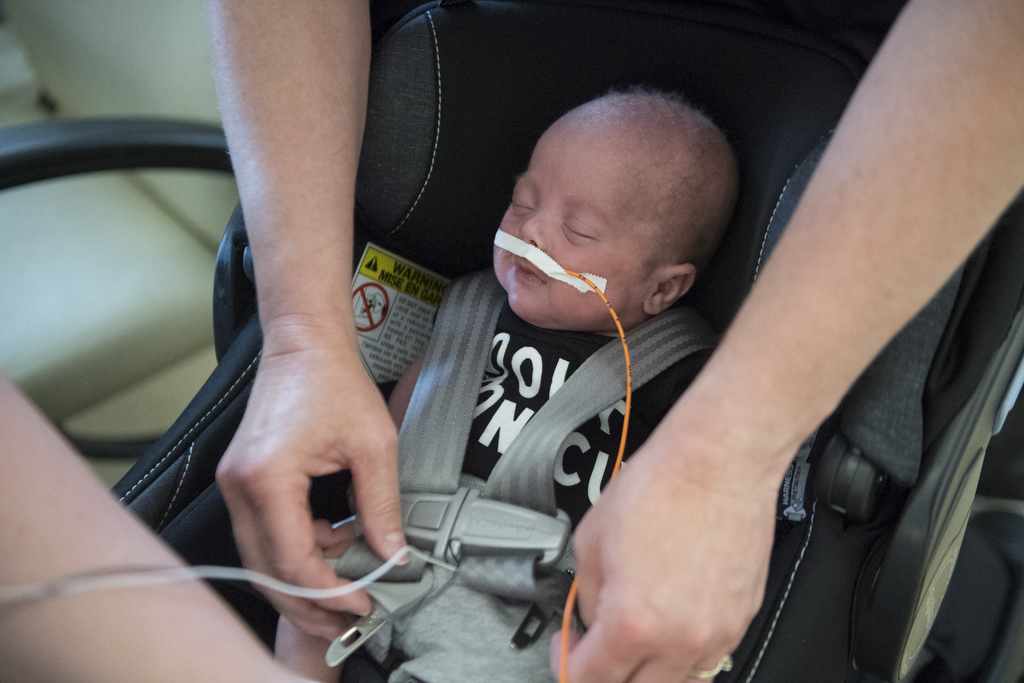
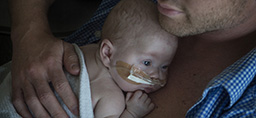
Four days after his homecoming, Noah nestled in his mother’s arms at his home in Comstock Park, Michigan. He had a heart monitor and used a feeding tube for supplemental nourishment. And he will continue to see a pediatric ophthalmologist and other specialists for checkups.
But in general, the Markles focused on soaking in the ordinary joys of life with an infant at home—stroller rides and morning cuddles—while looking forward to seeing what their baby boy does next.
“I’m excited to see his personality develop,” Rebecca said. “He already is a feisty little guy. He needed that to survive.
“Not a lot of people get to say their kids are their hero,” Don said. “But it’s true. He’s our hero. He’s not even 6 months old, and you can look up to him and say what a big fighter he is.
“It will be awesome to be able to tell him about himself, so he knows there is nothing in the world he can’t do—because he has already been through so much.”












































 /a>
/a>
 /a>
/a>
 /a>
/a>
No one will ever feel in their heart the love that we have for this child. He is our great-grandson and the hole in our heart has been replaced by God’s marvelous Grace! We both look at him and marvel at the feelings and emotions that we have for this precious child. Words can never express the love that we have as well. We have watched the expressions of love and concern that the doctors and nurses have shown while he was in the most fabulous facility in this country, “Spectrum Health Helen DeVos Children’s Hospital.” What a blessing this facility has been to all of us throughout the four-month period. Only the blessings from God and these marvelous, professional, and compassionate people could accomplish! We are blessed!!! Thanks so much to each of you and blessings be on each of you.
Thank you so much for your kind words and amazing testimony. Best wishes to you and little Noah for a blessed life together.
We are so thankful to God with you!!
my niece Olivia was born at 22 weeks as well in 2016 and no ones ever heard of her..
1 lb 3 ounces.
That’s amazing, Chloe! Thanks for sharing and reading. Best wishes to Olivia and her family. 🙂
My son DeCarlos was born 3-2-21 at 27 weeks.. he was 1.2 pounds. We still have a long journey to go but seeing these stories gives me hope and reassurance for a smooth recovery and homecoming!! Thanks spectrum health!!!