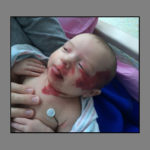
The spot appeared on Avaree Hunt’s cheek a week or two after birth, a strawberry-red dab that looked like a tiny birthmark.
It grew fast.
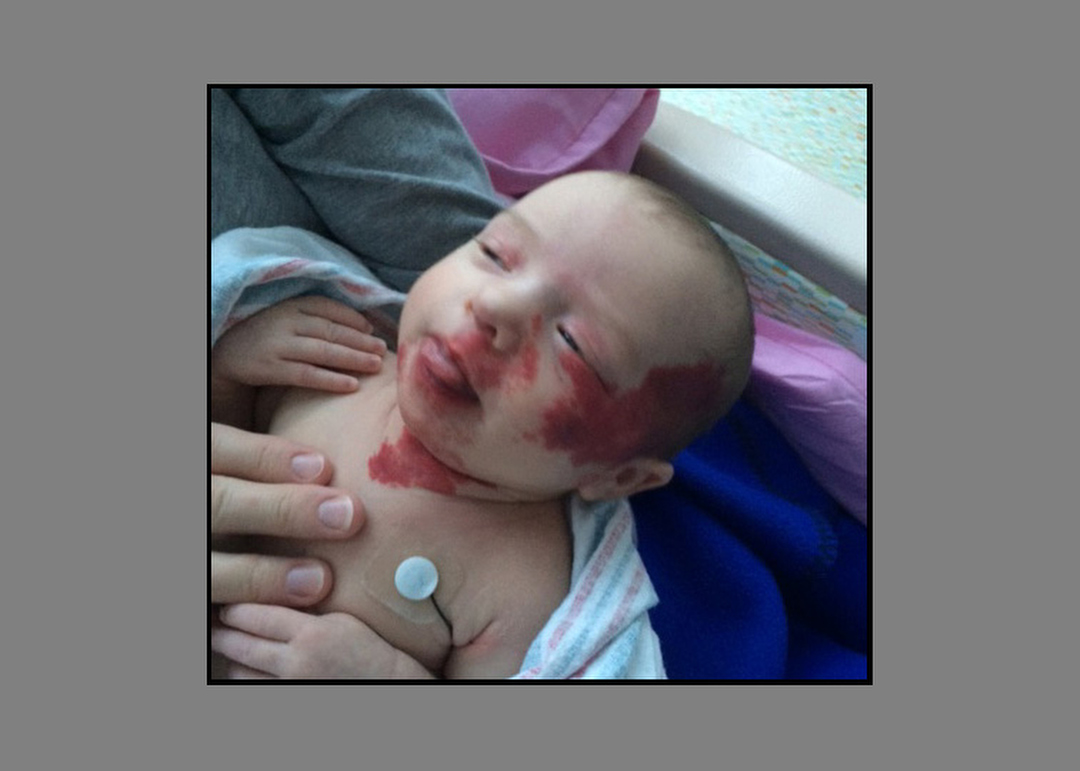
By the time Avaree was 1 month, the red patch spread across the left side of her face and along her neck.
“It was a very big surprise,” said her mother, Lauren Hunt. “It progressed very quickly the first weeks of life.”
As they met with doctors, Lauren and Seth Hunt learned their daughter had a hemangioma, a common condition in newborns caused by an abnormal buildup of blood vessels. Although it eventually goes away on its own, some children need monitoring, medication and surgery to prevent complications.
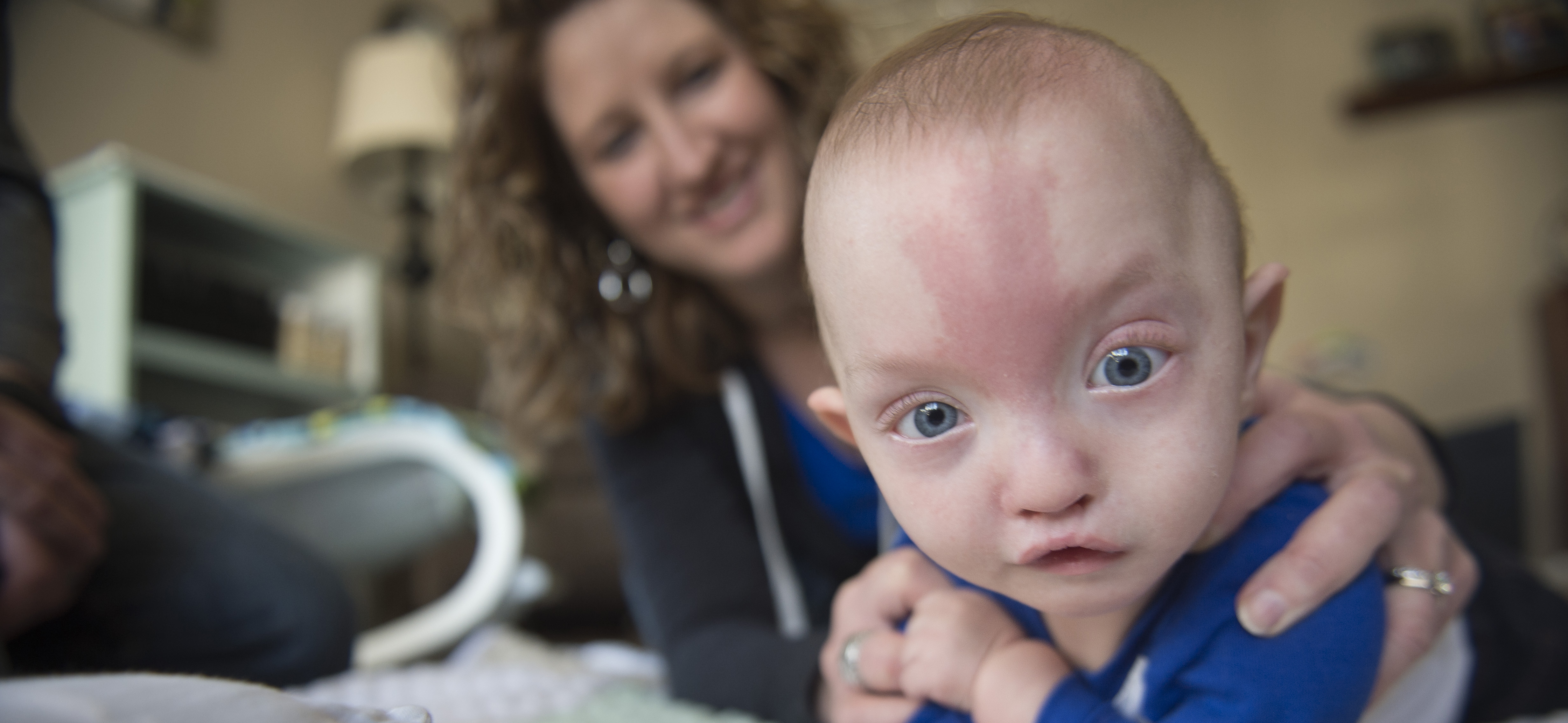
For Avaree, a happy, green-eyed baby girl, it took a team―a group of specialists at Spectrum Health Helen DeVos Children’s Hospital who work together to treat vascular anomalies in children.
Common for kids
Avaree and her twin brother, Greyson, arrived Jan. 16, 2016, both healthy babies. Avaree tipped the scales at 7 pounds, 12 ounces, and Grayson weighed 6 pounds, 15 ounces.
When Avaree’s hemangioma started to appear, the Hunts’ primary care physician referred her to Kristen Snyder, MD, a pediatric hematology-oncology physician who also specializes in treating hemangiomas and other vascular anomalies.
The parents quickly learned about hemangiomas and some of the risks associated with them.
“It was very stressful, especially because I had her brother at home, too,” Lauren said. “We were in the newborn phase, trying to get it all figured out. And to have her be so medically sensitive and us not really knowing what we were looking for―it was definitely stressful.”
Hemangiomas occur in 5 to 10 percent of babies. They are far more common than many parents realize, Dr. Snyder said. Hemangiomas are not always seen by others because they may occur in spots normally covered by clothing. And they fade away over time.
“The natural history of this is it grows rapidly in the first six months of life,” Dr. Snyder said. “From six months to 12 months, it grows less rapidly. After 12 months of life, even if you don’t treat these hemangiomas, there’s a switch that goes off that tells them to start going away. But that process of going away can take years.”
A hemangioma typically affects just the skin. But Dr. Snyder knew Avaree’s hemangioma, because of its location, could affect her internally, particularly her airway. She discussed Avaree’s condition in a meeting with the multi-disciplinary vascular anomalies team at Helen DeVos Children’s Hospital.
“That’s one of the things that was comforting. The smartest people who know about this are all talking together―this has to be good,” Lauren said. “It makes you feel a little better.”
Chad Afman, MD, a pediatric otolaryngologist, examined Avaree’s trachea and found the hemangioma in the subglottis, intruding in the airway just below the vocal chords. This explained her noisy breathing, he said.
“That’s the narrowest part of the airway for a child,” he said. “If Avaree did not respond to medical treatment, she would require surgery.”
The effect of the subglottic hemangioma on Avaree quickly became clear.
The next day, she began to have more trouble breathing and eating, Lauren said.
Avaree spent two days in Helen DeVos Children’s Hospital, as the team monitored her breathing and began medical treatment.
Breakthrough treatment
Avaree started a short course of steroids and also began to take a blood pressure drug called propranolol to reduce the size of the hemangioma. Quickly, her noisy breathing improved and her hemangioma began to slowly fade.
Propanolol represents a breakthrough in treatments for hemangiomas, Dr. Snyder said. In years past, children who needed medical treatment received steroids and other chemotherapy agents, which caused side effects including a suppressed immune system. Additionally, the alternatives were not as effective, and surgery was more common.
However, in 2008, French physicians reported an interesting development that occurred when they treated a child who had both a heart condition and a hemangioma. They gave the child propranolol for the heart condition, and were surprised to see the hemangioma “melted away,” Dr. Snyder said.
In 2014, the Food and Drug Administration approved the drug for infantile hemangiomas.
The medication commonly causes colder extremities. And it may cause low blood sugar, so parents are asked to feed a child after giving the medication. But overall, it causes less serious side effects than previous drug therapies.
Because the hemangioma covered her cheek, Avaree also saw a pediatric ophthalmologist to see if it affected the optic nerve. But her eye exams have not turned up any problems, Lauren said.
For most of the first year of Avaree’s life, the medication reduced the size of the hemangioma and kept complications under control.
She grew bigger, got her first teeth, learned to crawl and started talking. She played outside, danced and sang along with music, and played with her twin, Grayson, and 6-year-old brother, Maverick.
But in early January, near her first birthday, she caught a respiratory virus and ended up in the emergency department because she had trouble breathing. She took two rounds of steroids to reduce inflammation.
As she continues to grow and the hemangioma shrinks, the threat of surgery on the airway becomes less and less over time, Dr. Afman said.
A small, red spot
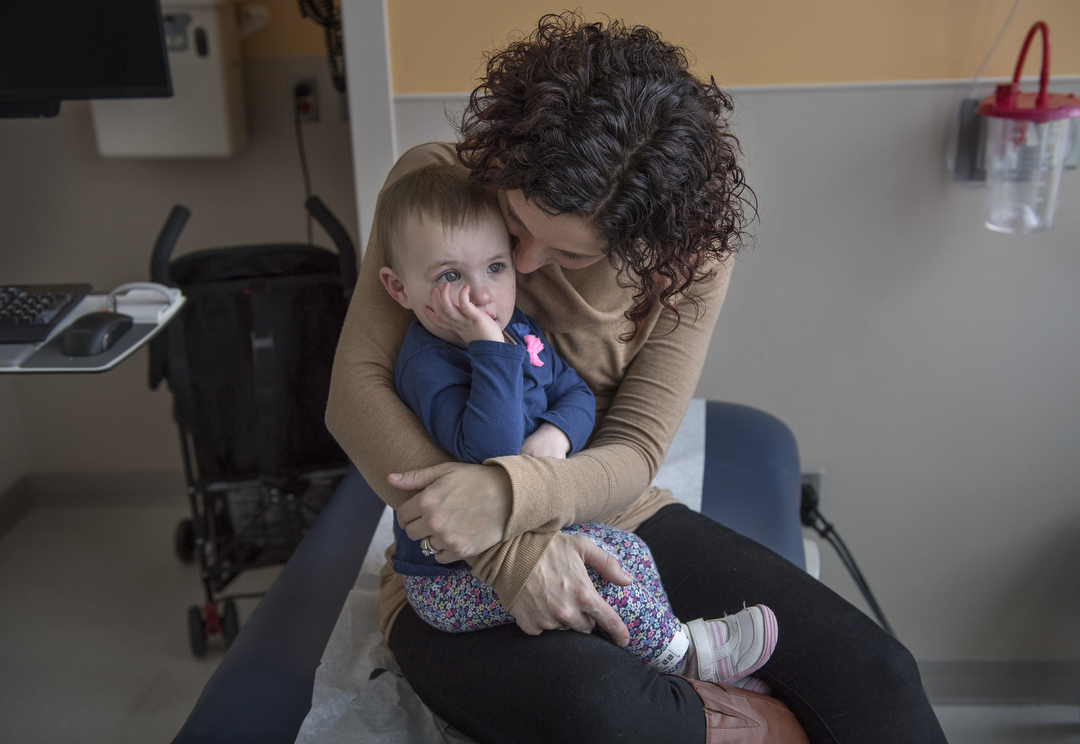
At 14 months, Avaree returned to Dr. Snyder’s office for a follow-up visit.
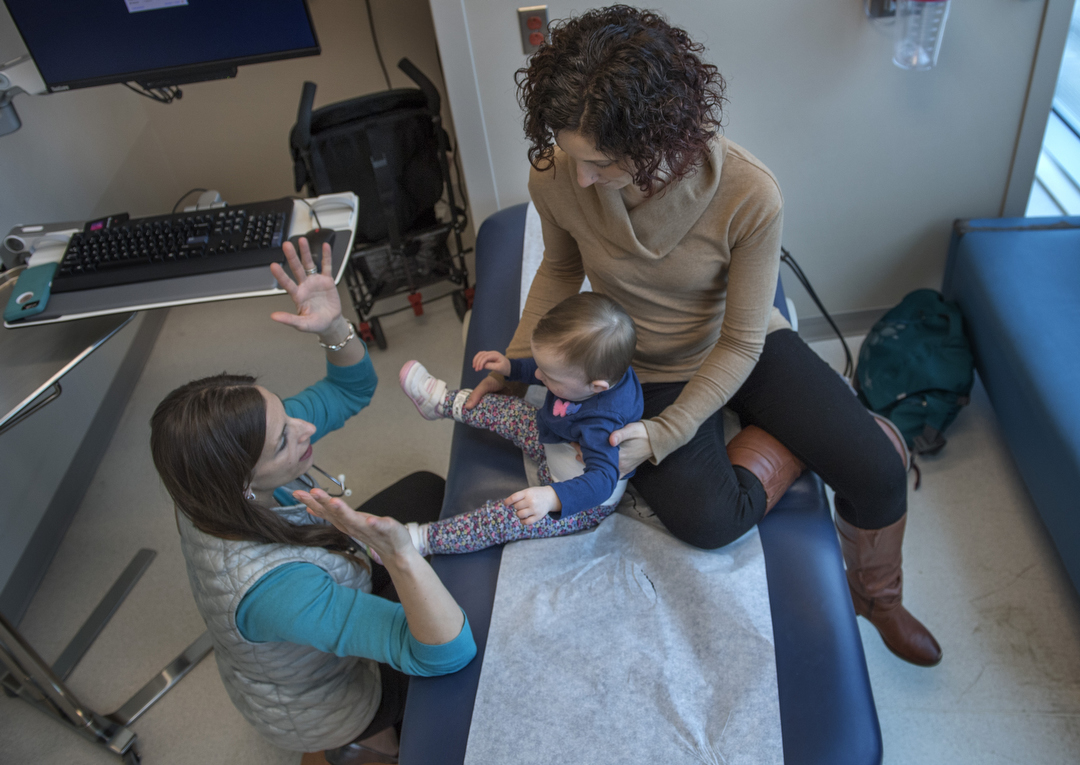
No longer an infant, she crawled across chairs and the exam table and babbled excitedly.
“She’s a cutie tootie!” Dr. Snyder exclaimed as she examined her.
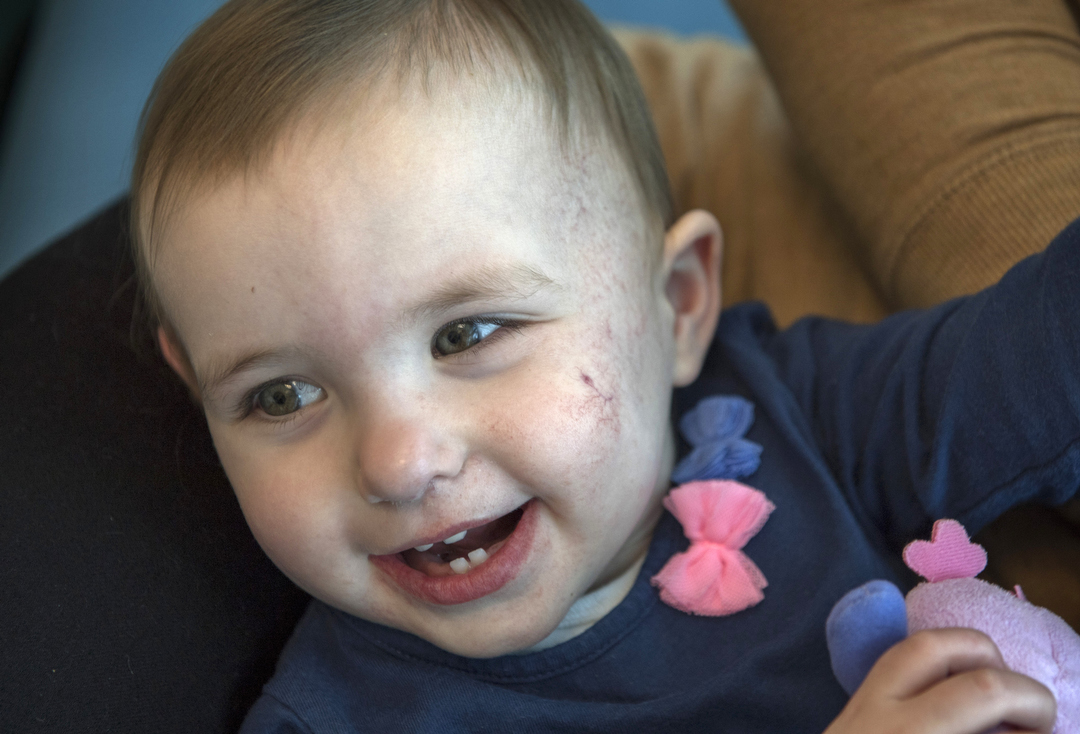
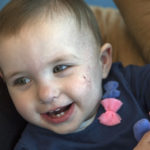
The hemangioma had shrunk considerably. It appeared as a small red spot on her left cheek, surrounded by a faint web of blood vessels.
Dr. Snyder decided it was time to wean Avaree from the medication. She would take a half-dose for a week and then stop taking it all together.
And Dr. Afman planned to examine the airway again.
“It is expected as she continues to grow and the hemangioma in the airway shrinks, she will no longer have breathing problems or require additional procedures,” he said.
The lines on Avaree’s cheek and neck will continue to fade, Dr. Snyder said. Some children eventually go to a plastic surgeon for laser treatments to reduce the redness.
“Later on, maybe when she’s older, if the redness hasn’t faded away to your liking, then you can do laser therapy,” Dr. Snyder said.
Lauren said she looked forward to moving past treatment. But she appreciated the medication and specialized care that helped Avaree through her first year.
“I think one thing that’s important is the team approach,” she said. “Dr. Snyder and Dr. Afman coordinated everything together.”
She encouraged parents to consult a specialist if their child has a hemangioma.
“Get it checked out just to make sure it’s not internal,” she said. “It can never hurt to have an assessment.”









 /a>
/a>
 /a>
/a>
 /a>
/a>