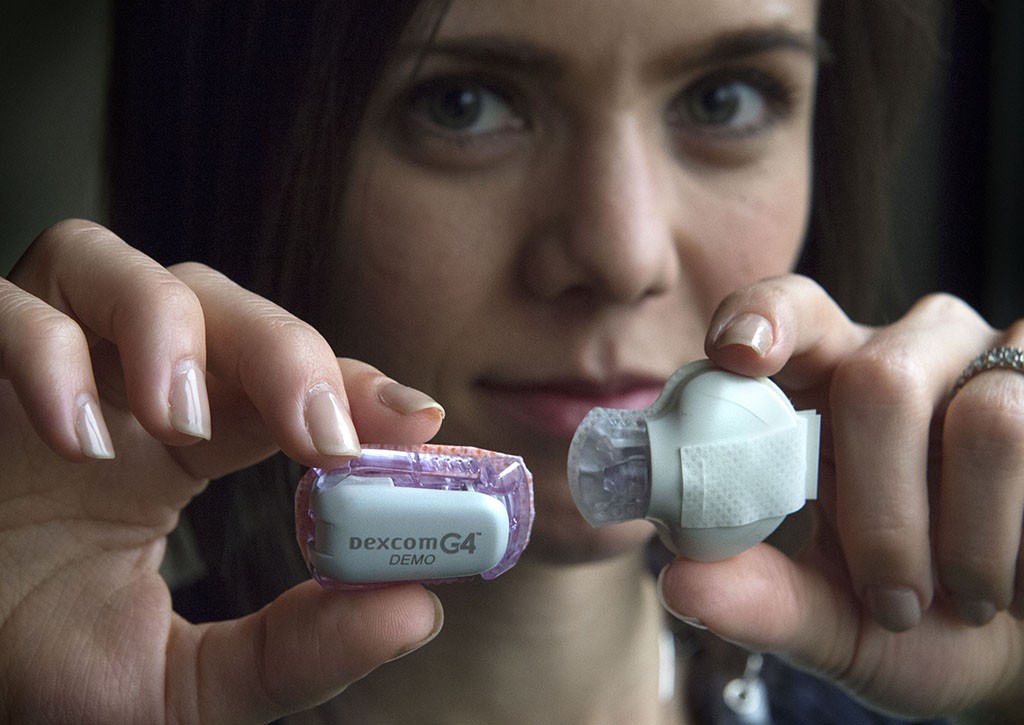
For years, people with Type 1 diabetes and many with Type 2 diabetes have had to test their blood glucose level by repeatedly sticking one of their fingers with a needle–an inconvenient but necessary self-administered discomfort.
But recent years have seen tremendous advances in the technology of blood glucose monitoring that have reduced the frequency of blood glucose checks, and may eventually eliminate those unpleasant needle sticks forever.
“There are more resources available now” for those who need extensive monitoring or have difficulty recognizing low blood sugar, said Annie House, RD, CDE, diabetes program education coordinator in Spectrum Health Medical Group.
“I’m optimistic,” added Aaron Kowalski, PhD, chief mission officer and vice president of research for the Juvenile Diabetes Research Foundation. “The last year or two is probably the best period of research development I’ve seen.”
Several companies and one university have announced they’re working to develop glucose monitors that don’t require skin penetration with a needle.
A research team at the University of California in San Diego said it has had preliminary success with a “temporary tattoo” continuous glucose monitor that’s worn on the wrist and reads changes in skin fluids through electrochemical sensors. And Google Inc. has announced it is working with a European drug manufacturer to develop special contact lenses that measure blood glucose levels in the wearer’s eye fluid.
In Europe, the Freestyle Libre, a minimally invasive patch manufactured by Abbott Labs, a U.S.-based pharmaceutical company, is already being worn by some diabetes patients. The patch, which reads blood glucose levels through a small sensor just 4 to 5 millimeters under the skin, lasts for 14 days before requiring replacement. It isn’t yet approved for use in the United States.
Although none of these products are commercially available in the United States, it is expected that will change in upcoming months and years. The increase in less-invasive technologies is painting a significantly brighter picture for people with Type 1 diabetes.
Preceding these recent announcements, the commercial success of glucose monitors in the early 2000s was the biggest step forward since the introduction of finger-sticking needles in the 1970s. Before then, diabetes patients checked their glucose level by testing their urine.
Increasingly popular since their introduction, continuous glucose monitors require a sensor worn under the skin and connected to a device worn on the abdomen or another part of the torso. These types of monitors are an advance over repeated one-time needle sticks because they improve convenience and provide real-time glucose readings. They are especially beneficial in helping people recognize blood glucose trends so they can have confidence in their decisions to treat appropriately.
“Continuous glucose monitors have become more common and can be a valuable tool” in blood glucose management, said Spectrum Health’s Annie House. Additionally, monitors can be set to alert someone if their blood sugar is outside of the desired range, and will automatically alarm at critically low levels.
“Drawing blood multiple times a day is obviously a burden, but it’s critical information,” Dr. Kowalski said.
He was diagnosed with Type 1 diabetes at age 13.
“I had 31 years of sticking my finger” to check my glucose level, he recalled. Dr. Kowalski obtained his monitor in 2005. It sends readings straight to an app on his cell phone. Advances such as this have resulted in significantly fewer finger pokes for many people.
The key word, he said, is “non-invasive”–being able to monitor blood sugar levels with complete accuracy and minimal discomfort. “If you could get all the information you want without bothering the person, that’s the Holy Grail” of blood glucose monitoring technology, he said.
Making the next generation of monitors—the needle-less devices—a commercial reality is quite difficult, he said. For example, eye fluid varies during the day, as does the fluid released by our skin. For a device to monitor these changes and get regularly accurate readings will take years of research.
“These are the practical things that we need to work through,” Dr. Kowalski said.
Meanwhile, the current generation of monitors continues to get more sophisticated, with the newer models better able to discern trends in a person’s glucose level over time or to send the results directly to a caregiver or a parent or loved one. And in the next few years, devices that combine an insulin pump with a glucose monitor to automatically control a patient’s insulin levels—basically, an artificial pancreas—will be introduced.
“These technologies are a bridge to a cure,” Dr. Kowalski said.
Ideally, researchers will eventually devise a practical way for the body—possibly through stem cell technology—to know how to self-adjust improper glucose levels. The foundation is supporting research into just this, and an experiment is going on now with volunteer diabetes patients using a prototype product, with support from the foundation and the Institute for Regenerative Medicine in California.
This is what is called “encapsulation” research, he said, and that’s where we want to be.
“There’s a revolution going on in glucose monitoring,” Dr. Kowalski summarized. “We are approaching the day when there will be kids with diabetes who will never have to stick their fingers.”
 /a>
/a>
 /a>
/a>
 /a>
/a>