If you have Parkinson’s disease, you probably take a cocktail of medications to reduce debilitating symptoms including tremors, stiffness, slowed movement and walking problems.
For some, it’s not enough.
The medicine may wear off too quickly. Symptoms may fluctuate widely throughout the day. Or you may have dyskinesia, a bothersome, involuntary wiggling that happens when the medication is at a peak dose.
There’s no cure for Parkinson’s, a disease that affects about 1 million Americans.
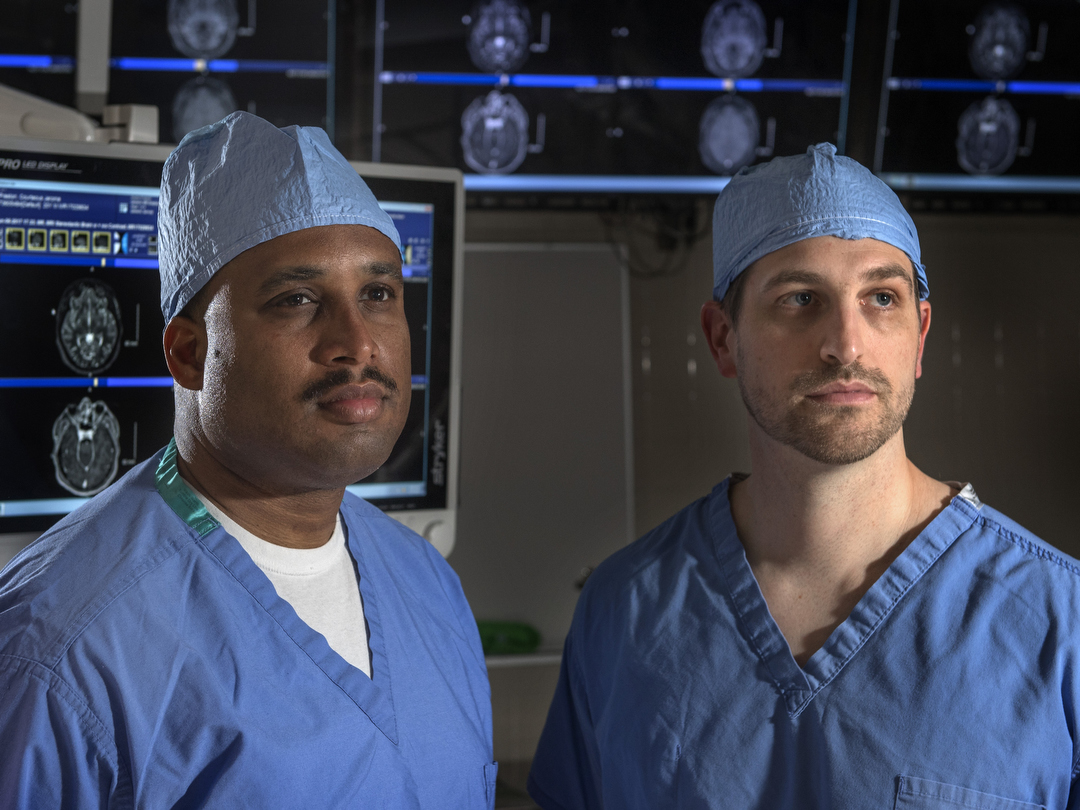
But, for some patients, deep brain stimulation could help, according to R. Ross Coleman, MD, a movement disorders neurologist with Spectrum Health Medical Group.
Deep brain stimulation uses electrodes that are about the size of spaghetti noodles to send high-frequency signals to areas of the brain that control movement. About 10 percent to 20 percent of Parkinson’s patients may be good candidates for the procedure at any one time.
Think of it like a pacemaker for the brain.
“It smooths out their motor problems so they don’t have wide fluctuations throughout the day,” Dr. Coleman said. “In the correct patient, it can make a huge difference.”
After surgery, the neurologist programs stimulation to optimize outcomes. Patients can then, with guidance from their neurologist, use a remote control-like device to adjust the electrical stimulation as needed.
Brain surgery with your eyes open?
Historically, deep brain stimulation procedures required the patient to be awake during surgery—a scary thought for many people.
Dr. Coleman compares it with a road trip.
“If you’re driving through Europe and roll down the window you can hear the language being spoken, you can tell what country you’re in, and perhaps even what region of that country,” he said.
“It’s the same with the brain. Listening to the brain cells and communicating with the patient during surgery helps us map the brain precisely and then turn electrical stimulation on to monitor results and avoid side effects.”
But being awake for brain surgery isn’t for everyone.
For some people, it creates anxiety. And patients must stop taking their meds before surgery, which immediately brings back their Parkinson’s symptoms.
A new alternative
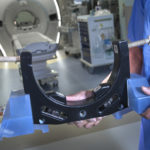
Variations of surgical treatment for Parkinson’s have been around since the 1950s, but now there’s a new development: Patients have the option of “asleep DBS,” or what surgeons call “interventional MRI-guided DBS.”
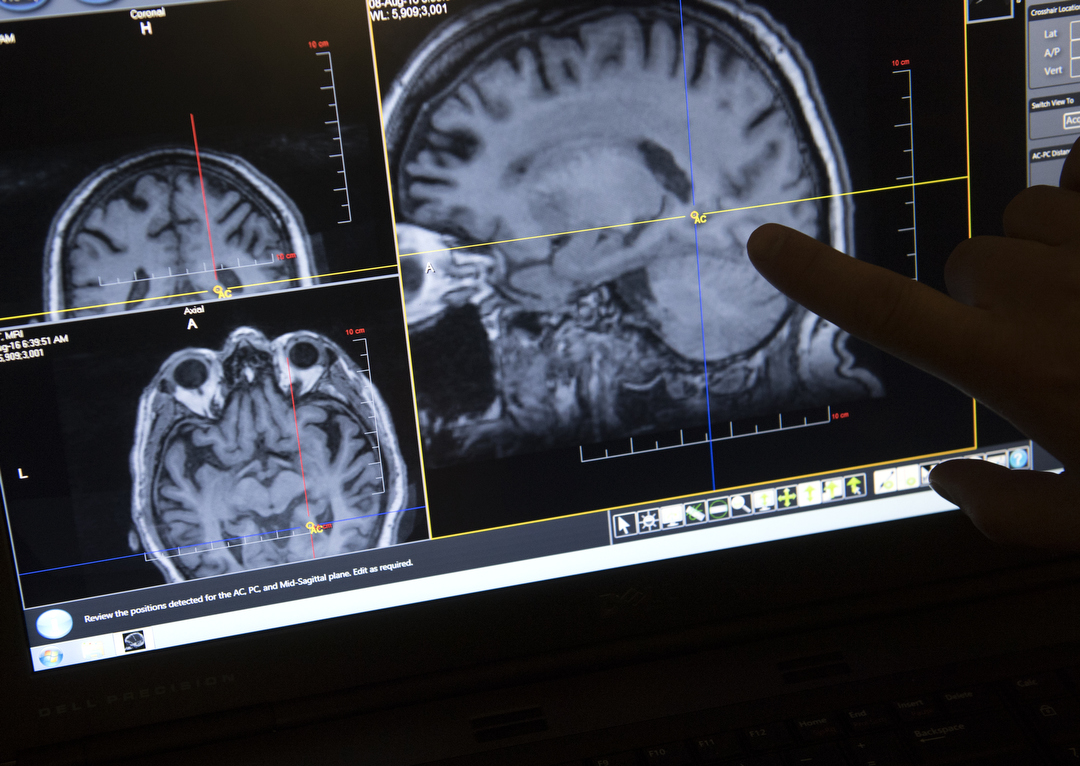
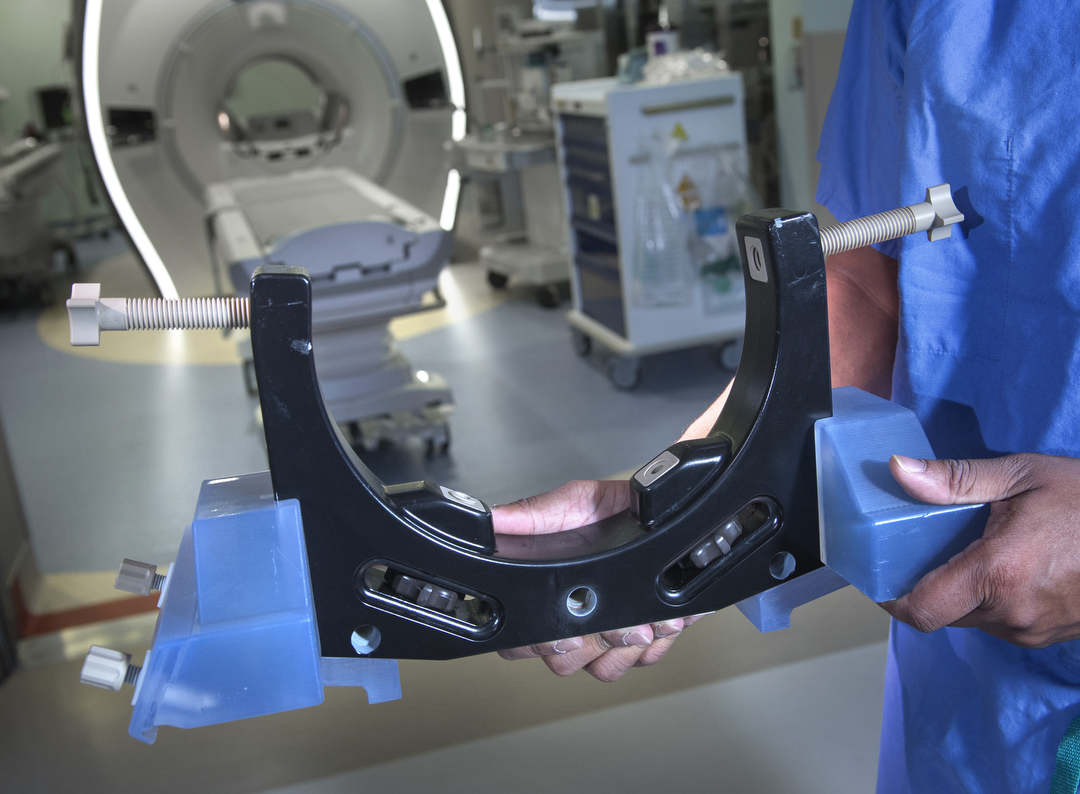
“This procedure is based on years of experience,” Dr. Coleman said. “Patients are given anesthesia, so they are ‘asleep’ inside the MRI equipment during surgery. We use real-time MRI images to accurately place the electrical leads.”
This offers the benefits of deep brain stimulation to people who can’t tolerate the traditional approach.
Best of all, it’s working. The Journal of Neurosurgery and other experts have documented that outcomes for sleep DBS appear to be similar to having the traditional “awake” version of the surgery.
Fast track pre-screening
To qualify for deep brain stimulation, patients must be checked out by a number of specialists to be sure they’re good candidates.
Fortunately, Spectrum Health has developed a two-day, fast-track system that lets patients see specialists from neurosurgeons to neuropsychologists, speech therapists, physical therapist and occupational therapists all under one roof.
“It’s very patient-friendly, and it lets us look at the patient’s overall health to quickly evaluate whether DBS surgery is appropriate for them,” Dr. Coleman said.


 /a>
/a>
 /a>
/a>
 /a>
/a>
I would like more information about this to see if I am a candidate.
Hi Richard, thanks for being a Health Beat reader.
You can get more information about deep brain stimulation from the Comprehensive Multidisciplinary Parkinson’s Disease Clinic at Spectrum Health. Call 616-267-7900.
I am honored to work along side Dr Coleman at SHMG neurology. He is an amazing neurologist!