Pizza. Chips. Mac-and-cheese. Candy.
A great big bowl of Lucky Charms.
All these food favorites made 10-year-old Walker Freese a happy boy.
Until they didn’t.
It happened gradually. But over many weeks, even the simplest snack made Walker sick to his stomach. He vomited after meals. He even threw up at night while he slept.
The transformation left his parents, Holly and Jason Freese, mystified. And with good reason.
Walker had a condition—called achalasia—that is rare even in adults.
“In children, the incidence is about 1 in a million children,” said John Schneider, MD, a pediatric surgeon with Spectrum Health Helen DeVos Children’s Hospital. “Walker really is one in a million.”
After treatment, Walker once again finds joy in a pizza dinner. But getting to that point took some detective work from his parents and doctors—and patience for Walker.
Losing weight
The first signs of trouble started to show up when the family went out to eat at restaurants.
Walker, then a fourth-grader and the oldest of three boys, would sometimes excuse himself during dinner to go to the bathroom. He did it at home, too, but it seemed more sporadic.
He didn’t say he felt sick or that he threw up, but Holly began to suspect that was happening.
“I remember thinking that he was hiding something,” she said.
She wondered if her son had acid reflux. She worried he might have an eating disorder.
The issue grew worse.
“He would drink a glass of milk, and it would all come up,” she said.
And then Walker began to throw up while he slept.
Holly took him to the pediatrician’s office. When Walker stepped on the scale, she realized he had lost 11 pounds.
The doctor referred him to Ryan Cox, MD, a pediatric gastroenterologist at Helen DeVos Children’s Hospital.
Dr. Cox performed an upper endoscopy, using a flexible camera to examine Walker’s esophagus, the pipe that transports food from mouth to stomach.
“The minute I put the scope down the esophagus, I saw it was full of food,” he said. “It made me think immediately of achalasia.”
Achalasia involves a degeneration of the nervous system of the esophagus that occurs over time. The valve at the end of the esophagus does not open to allow food to pass through to the stomach.
The condition affects about 10 in every 100,000 people—and typically affects adults.
“It is usually diagnosed between age 25 and 60,” Dr. Cox said. “In those younger than adolescents, it’s incredible rare.”
Walker underwent an upper gastrointestinal exam, which uses dye to track the flow of liquid. That test, too, showed that he had achalasia.
Dr. Cox put Walker on a diet of liquid and mushy foods, while referring him to Dr. Schneider for treatment.
Yogurt parfaits all day
For Walker’s mom, the diagnosis led to research about the unusual disorder. She made contact online with others who have achalasia, to learn more about the impact on their daily lives. She learned that many people struggle for years with symptoms of achalasia before they find a correct diagnosis.
“It wasn’t the result we wanted, but I’m glad that within two weeks we had a diagnosis and he could start getting well,” she said.
She relied on suggestions from the online community to come up with a liquid diet Walker would tolerate.
“One lady said the McDonald’s yogurt parfaits got her through so many tough times,” she said. “We would get eight every morning to last the day.”
On school days, she met Walker in the cafeteria at Dutton Elementary in Caledonia to give him a smoothie for lunch.
Although Walker’s system handled liquids better than solid foods, he still regularly vomited up his meals. He grew weaker, so his parents pulled him from his Little League baseball team.
The only thing that frustrated Walker was the liquid diet. He missed eating solid food. He handled all the other challenges with an easygoing, upbeat attitude.
“This kid has just amazed us,” Holly said. “He never complained about anything. I think this has been harder on me and my husband than on him.”
Ready for pizza
After two weeks on a liquid diet, Walker underwent surgery on his esophagus.
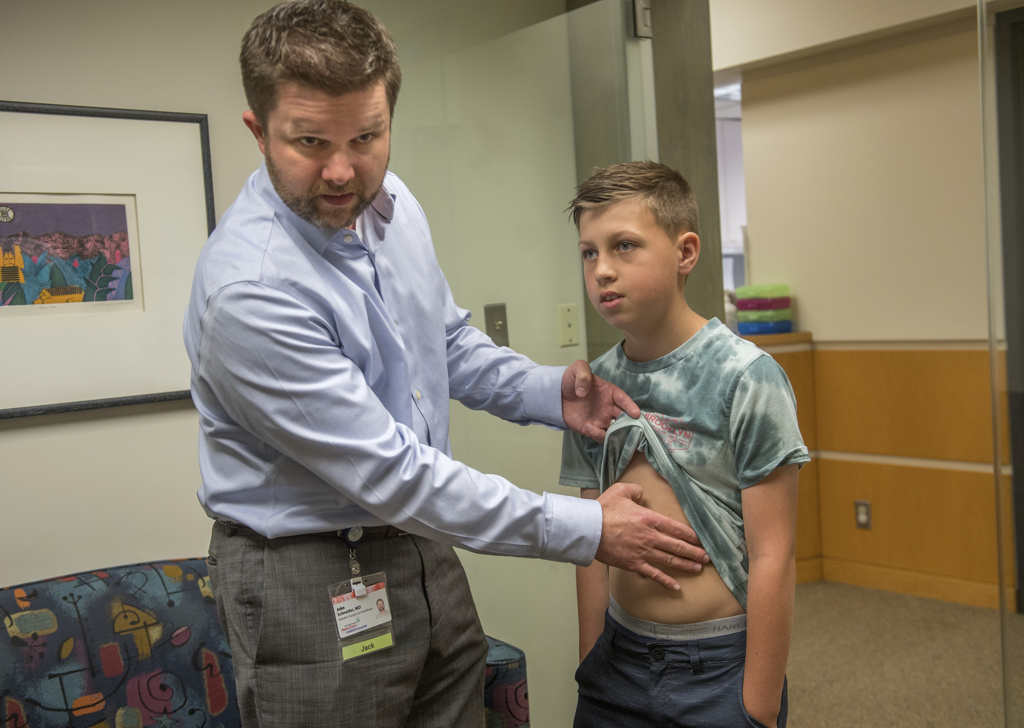
Dr. Schneider performed a laparoscopic procedure, using a tiny camera placed into Walker’s abdomen through his belly button. Through four tiny incisions, he used long, skinny instruments to split the outer muscles at the end of the esophagus.
“That releases the obstruction where those muscle fibers won’t relax,” Dr. Schneider said.
He also folded the stomach over to cover the end of the esophagus.
“Wrapping or folding the stomach changes the anatomy and geometry of the stomach to reduce the chance he is going to have reflux, where the stomach contents go back up into his chest,” he said.
Walker continued on a liquid diet as he recovered from surgery. A few weeks later, Dr. Schneider gave him the OK to try solid foods.
He chose pizza for his first meal.
Six weeks after the surgery, Walker visited Dr. Schneider. He was eating all his favorite foods, gaining weight and feeling stronger.
“He’s back playing sports with his friends,” Holly said.
Best of all, he no longer threw up after eating.
Doctors don’t know the cause of achalasia. It can be a chronic condition. Walker will continue to see Dr. Cox, who will monitor his condition.
“Overall his outcome has been fantastic,” Dr. Schneider said. “For right now, I couldn’t ask for anything better.”
Holly agreed.
“Walker isn’t cured but he seems to be 100 percent currently, so we will take that as a huge win and just roll with the hiccups along the way,” she said.
“We are blown away by Walker’s results and couldn’t be more blessed.”










 /a>
/a>
 /a>
/a>
 /a>
/a>
Praise God!
What a beautiful story about a brave boy!
I pray he will enjoy a wonderful, healthy and BLESSED life.
God bless Walker and his entire family!
Marilyn
Thank you for your kind comments. I’m sure the family appreciates them. And yes, Walker is an awesome kid.
The first picture of Walker leaning on his Mother’s shoulder is so powerful… and beautiful… what a handsome young man! I was especially happy to read the successful outcome – and hope it stays that way. Many continued blessings to him and his family.