Paxton Florek ran the length of his living room, a joyful 3-year-old with places to go.
He stopped briefly for a hug from mom, checked on a toy and ran his hand along the window overlooking the wooded backyard.
The door opened, and Dad came home.
Paxton was all smiles as Dad swooped him up.
Wiggling, Paxton leaned toward the door and pointed, letting Dad know it was time for their daily 2-mile walk around the neighborhood.
Dad happily complied, walking beside his son as they headed down the sidewalk.
Not long ago, Luke and Anna Florek did not know if their son would ever walk, much less run.
Or if he would survive the aggressive tumor found in his brain.
Today, each step Paxton takes is a moment they treasure and celebrate.
“It has been a long journey to get to this point,” Luke said. “And he is doing phenomenal. Every day, we feel he is learning something new. And we get to watch him do it all.”
His progress astounds even his pediatric oncologist.
“To me, he is miraculous,” said Rebecca Loret de Mola, DO, of Spectrum Health Helen DeVos Children’s Hospital. “He has surpassed every single expectation I have had for him.
“He is a pioneer, 100%.”
‘We were … in fight mode’
Anna and Luke Florek welcomed their first child, Paxton, in November 2018.
“He was such an easy baby,” Anna said. “He was a great sleeper at night. He traveled with us anywhere we wanted to travel.”
There were no health concerns until he reached 10 months old.
Anna noticed subtle changes. Paxton seemed a bit shaky in the morning. When she lay him down, sometimes he looked disoriented for a couple of seconds, as if he were suddenly dizzy.
He started to wobble when he tried to sit.
In September 2019, Paxton’s parents took him to Helen DeVos Children’s Hospital.
An MRI revealed a tumor the size of a golf ball at the base of Paxton’s head.
“Surprisingly, we didn’t even cry when they told us,” Anna said. “We kind of were prepared for the worst, whatever that was.
“We were in shock mode and fight mode at that point in time.”
They asked their doctors: What next?
They met pediatric neurosurgeon Michael Bercu, MD, who explained that the tumor had caused hydrocephalus, a buildup of fluid in Paxton’s brain. In itself, that could be life-threatening.
The first step: place an external ventricular drain to relieve the pressure on his brain. That night, at 11 p.m. on a Friday, Dr. Bercu performed the procedure.
The surgery to remove the tumor began early on Monday morning.
At least a dozen people gathered in the operating room for the daylong, complex surgery, including Dr. Bercu and Justin Singer, MD, an endovascular neurosurgeon, as well as two anesthesiologists, nurses, advanced practice providers, technicians, a neuromonitoring team and a pediatric intensive care unit team.
“You need the whole team,” Dr. Bercu said. “I always say, the more eyes the better. The more hands, the better.”
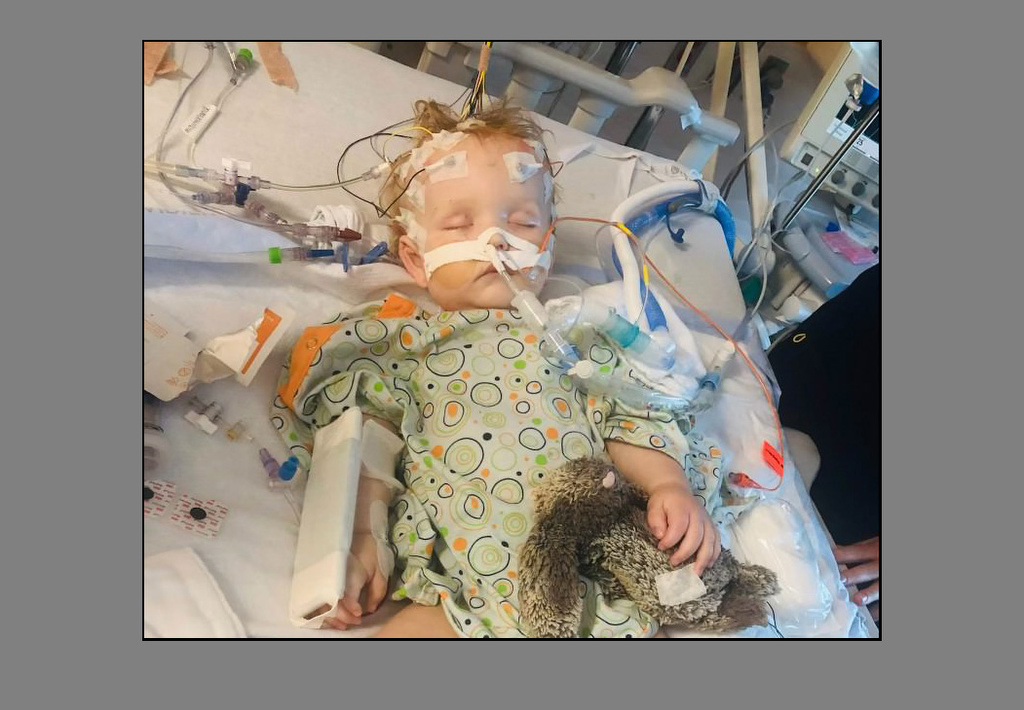
At the center of the room lay Paxton, a tiny infant.
The team spent two to three hours to prepare Paxton for the surgery—to position him and attach monitoring equipment and the GPS-like navigation system that would help guide the surgeons.
The tumor lay in a critical area, on top of the brain stem, which controls the basic functions of life, such as breathing and heart rate. It also serves as the highway for all communication between the brain and the body.
“No matter how many cases we do, every tumor is different,” Dr. Bercu said. “When there is a tumor growing and pushing on the brain stem, the anatomy is different. The tumor likes to go through all kinds of openings, into all kinds of corners.
“Things change and shift as you are working and taking out part of the tumor.”
Believing the tumor to be an aggressive, malignant one, Dr. Bercu hoped to remove it entirely—without damaging the brain stem or cranial nerves.
“We know with some tumors, even if you leave a very small piece, they will regrow. And the chance of survival is going to be much, much lower,” he said.
After the surgeons removed most of the tumor, they partially closed the surgical site so Paxton could undergo an MRI scan.
A sliding mechanism on the operating table allowed Paxton to be transferred into an MRI in an adjacent room.
The new MRI images confirmed the surgeons’ assessment. Paxton returned to the operating room, where they finished removing the tumor.
“At the end, we did feel all the tumor was out, and everything went well,” Dr. Bercu said. “We did not encounter any problems. All the brain stem and cerebellum and cranial nerves were preserved.”
A new diagnosis
He delivered the news to Anna and Luke, who had waited and worried for 14 hours during Paxton’s surgery.
“That was a huge relief,” Anna said. “We are very lucky to be in this day and age going through this kind of thing. He would have had zero chance in any other lifetime.”
As Paxton recovered from the surgery, the Floreks discussed his treatment plan with Dr. Loret de Mola, of the Ethie Haworth Children’s Cancer Center at Helen DeVos Children’s Hospital.
The analysis of the tumor showed Paxton had medulloblastoma, the most common type of pediatric brain cancer.
In older children, doctors treat the cancer with chemotherapy and radiation. Because Paxton was so small, they had to avoid radiation—it could harm an infant’s developing brain.
Instead, Paxton received high-dose chemotherapy and a stem-cell transplant, using his own stem cells.
He received other treatments and his tumor underwent a molecular analysis.
A few weeks later, the test results revealed a new diagnosis: He had an embryonal tumor with multilayered rosettes. Known as ETMR, it is a rare and extremely aggressive form of cancer.
“With the way science has changed and as we have been able to study these tumors, we have discovered they are different from medulloblastoma,” Dr. Loret de Mola said.
The new diagnosis did not change the treatment plan, but it meant Paxton faced an even tougher battle.
“That essentially made him even higher risk,” Dr. Loret de Mola said. “These tumors are incredibly difficult to treat, even with the maximum therapy we use for medulloblastoma treatment.”
In a decade of treating children who have cancer, she has seen only four cases of ETMR. Paxton is the only survivor.
‘It’s like a fog has lifted’
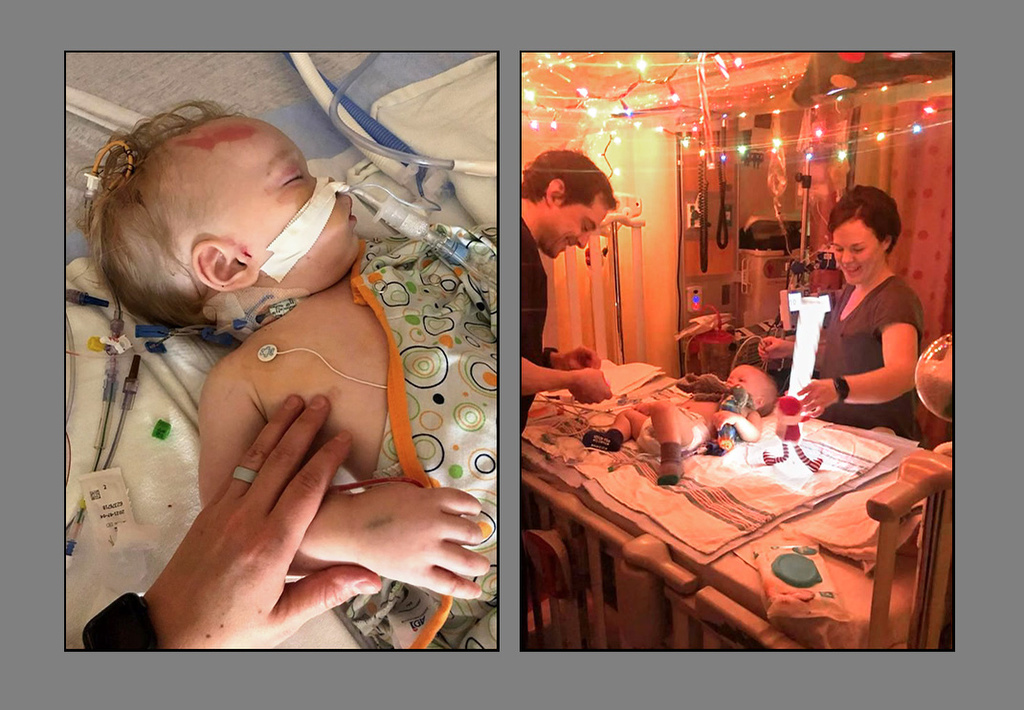
Paxton received four-and-a-half months of chemotherapy, enduring a host of side effects: fevers, rashes, nausea and vomiting.
He spent most of that time in Helen DeVos Children’s Hospital, occasionally going home for a couple of days between rounds of chemo.
He completed that therapy and received additional medications for the next two years.
Since then, repeated MRI scans have shown no evidence of the tumor.
“I would say he is in remission,” Dr. Loret de Mola said.
Paxton, the tiny survivor, has certainly been affected by the cancer and the treatments. He has hearing loss, autism and developmental delays.
But even so, his resiliency astounds his doctor.
Dr. Loret de Mola cautioned the Floreks that Paxton might have mobility issues. And while his balance is still a bit unstable, he runs passionately, joyfully.
Although non-verbal, he has learned to eat by mouth. And he sometimes communicates by making noises.
His personality has blossomed. He smiles and shows affection to his parents.
“It’s like a fog has lifted,” Anna said. “He is growing every day and surprising us with what he is capable of.”
Dr. Loret de Mola happily reports, “Paxton is clearly wanting to prove me wrong on every level. All the things he is doing and has achieved is just a miracle.”
With continued physical, speech and occupational therapy, the Floreks hope more gains lie ahead.
With each stride Paxton makes, his doctor sees hope—for him and for other children who will face this cancer in the future.
“All the things he has been able to accomplish in the face of a really big challenge is incredible,” Dr. Loret de Mola said. “He contributes greatly to our understanding of how kids deal with this therapy.”
Paxton’s journey
A children’s novel inspired Paxton’s unusual name.
On a road trip in 2017, Luke, a fifth-grade teacher, and Anna, an at-home mom, listened to an audiobook of “Pax.” The story by Sara Pennypacker features a resourceful young fox who undergoes a difficult journey.
They loved the book—and the name Paxton.
And now, they see their son embody the strength of the book’s character.
“He has adapted to any situation we have put him in,” Anna said. “He is our little fox.”




















 /a>
/a>
 /a>
/a>
 /a>
/a>
To have this lived-story put into words…done so beautifully & perfectly…thank you! I am the paternal grandma of Pax & am grateful for this article. You put the things in my heart inro words on a page! Quite a fantastic story & journey…Pax is so stinking cute!
Paxton is one special little boy. The parents were blessed when he joined their family. Congrats to all who helped him and Praise God, who heard all the prayers, who saved this precious child who would bring joy to those around him.
Thank you Jesus!❤️
Beautiful story. Contued health and good wishes
Our home church group has been praying for Pax since he was diagnosed; I love seeing all these pictures and reading all of the story. Thanks be to God!