George Burhance isn’t medically trained, but he has no trouble talking shop with his electrophysiologist, Nagib Chalfoun, MD.
The two speak the same language.
Burhance worked for 25 years as an industrial electrician at the former Electrolux plant in Greenville, Michigan. Dr. Chalfoun is an electrician of the heart.
They met because Burhance was having trouble with his heart rhythm, and it didn’t improve with drug therapy. Things came to a head one day when he stumbled and almost fell at work.
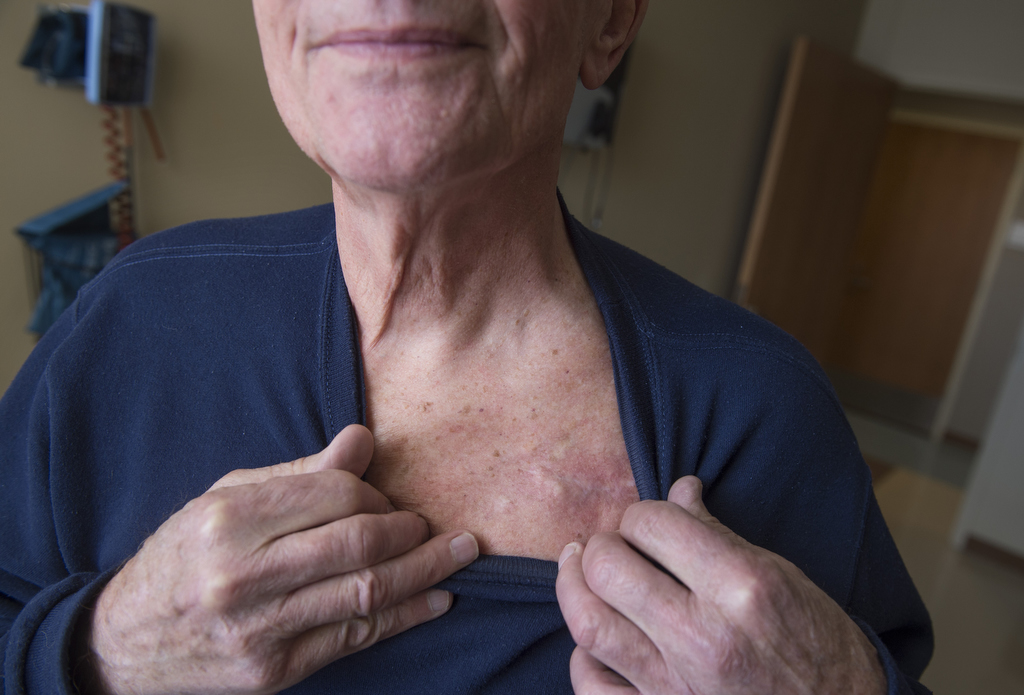
He was referred to Dr. Chalfoun, of the Spectrum Health Medical Group Cardiovascular Medicine team, who specializes in treating complex arrhythmias. The doctor stabilized Burhance’s irregular heart rate by implanting a biventricular pacemaker under the skin below his collarbone.
Pacemakers
A pacemaker is a small, battery-operated device that helps the heart maintain a steady beat when its natural electrical system malfunctions. Typically, pacemakers are used in patients who have a slow heart rate.
Wires called leads run from the device to the heart, sending electrical signals that tell the heart to beat. The signals are so mild that patients don’t even feel the pacemaker working.
A biventricular pacemaker is a special kind of pacemaker that delivers signals to both ventricles. Leads wrap around the left and right sides of the heart and synchronize the contraction of the chambers. This helps people who have weakened heart muscles feel better, Dr. Chalfoun said.

For most patients, the pacemaker is programmed to kick in on demand. It pulses as needed to help keep the heart rate above the minimum set by the doctor—60 beats per minute, for example.
Burhance’s heart rate was so erratic that on-demand pacing turned out to be insufficient. Because he had a problem called atrial fibrillation, his heart would sometimes race. He used medications to regulate his heart rate, but then it would sometimes get so slow that the pacemaker would kick in.
The combination of pacemaker and medications wasn’t working. Dr. Chalfoun knew Burhance needed something more.
“He needed to have his pacemaker take over complete control of the speed of his heart and run full time, as the captain of the ship,” Dr. Chalfoun said.
So in February, four months after implanting the pacemaker, Dr. Chalfoun performed a cardiac ablation to disconnect the top and bottom parts of Burhance’s heart, giving the pacemaker full control of the rhythm.
This conversion from on-demand to full-time pacing has made all the difference for Burhance, who at age 79 still works six days a week for a Greenville auto dealer.
“It’s been (a few) weeks now and so far it’s been great,” he said. “I really feel great.”
Implantable defibrillators
Whereas pacemakers are typically best for patients with a slow heart rate, a similar device, called an implantable cardioverter-defibrillator, is used in patients who have—or are at risk for developing—a lethally fast heart rate, such as ventricular tachycardia or ventricular fibrillation.
Defibrillators are like pacemakers in many ways: Both are battery powered, inserted with minimally invasive surgery, connected to the heart via leads and able to pace the heart if the rate goes too low. Both are also available in the biventricular version, which improves the heart’s pumping function. And most of today’s pacemakers and defibrillators are MRI compatible.
Here’s where defibrillators are different: They can save lives by preventing sudden cardiac arrest, which can come without warning.
A defibrillator constantly monitors the patient’s heart rate, looking for a life-threatening, out-of-control rhythm.
“It will go through its algorithm and say, ‘Does this picture match the picture of the normal heartbeat, or is it abnormal?’” Dr. Chalfoun said.
If the rhythm is abnormal, with a fast rate coming from the bottom part of the heart, the defibrillator may first send a mild pulse, like a pacemaker does. If that doesn’t reset the heartbeat, then the device will deliver a resuscitating shock.
And that’s a real jolt, Dr. Chalfoun said. “That’s kind of like getting kicked by a mule in the chest, is what some patients say.”
Not pleasant, but certainly better than the alternative.
“Sure, you’re going to get shocked, but you’re going to get your life saved,” Dr. Chalfoun said. “Every week (one of our patients) gets their life saved by these defibrillators. They’re amazing devices.”
Because of their lifesaving potential, defibrillators are like an insurance policy, Dr. Chalfoun said—both for patients with known arrhythmias and for those who have a genetic risk for arrhythmias.
“It’s like a backup generator,” he said. “One day—it might be five years … ten years from now—(the patient’s heart may) short circuit. But this thing’s going to be there and bring them back.”
Dr. Chalfoun is one of seven electrophysiologists in the Cardiac Device Clinic at Spectrum Health Fred and Lena Meijer Heart Center, one of the top heart rhythm programs in the nation. The team implants well over 1,000 cardiac devices per year, in patients like Burhance.
Patients typically love what the devices do for them.
“I think it’s a great thing,” Burhance said. “Of course, I had faith in my doctor. I just trusted him, and I feel better now than I did before this all started.”






 /a>
/a>
 /a>
/a>
 /a>
/a>
thank you so much my husband has defiballator and went to his heart to day his heart rate was low kinda of concern he didn’t ask questions I wasn’t there.
We’re glad this information could be of assistance to you, Brenda. Did your husband’s doctor print out a report regarding his appointment? Sometimes that can help fill you in to the situation if you aren’t able to be there. If there are concerns, please don’t hesitate to reach back out to your doctor to ask questions.
My son is 15 yrs old and has an ICD his has gone off multiple times since he received his implant in October of 2017. without it we would not have our son. He has his ups and downs wondering when it will go off again. He also knows that the device is his and our insurance that he will be with us for a long time. Now he can get on with his life and play the game of baseball that he loves so much. His dream is to play for Vanderbilt University. God willing he will reach that dream of his.
Thank you, James, for sharing your son’s story. It’s inspiring to others that he is able to live his dream playing baseball and is doing so well. Best wishes to him and to your family.