At her Gilda’s Club cancer support group, Michelle Mucha has made friends with a man who always says, “By the grace of God and the power of a clinical trial, I’m here today.”
The power of a clinical trial.
That’s what sprang to mind when Mucha found out that her breast cancer, first diagnosed in 2014, had spread to her chest wall, lymph nodes, lung tissue and liver. This, despite undergoing two surgeries, countless rounds of chemotherapy and 32 radiation treatments in the ensuing two years.
Ongoing chemotherapy might give her about three more years of life, her oncologist, Amy VanderWoude, MD, told her a year ago. This cancer was aggressive.
“That hit hard — hit really hard. I’ve lost all four of my siblings and a dad and a stepdad to various reasons … so I’m like, I can’t tell my mom this,” Mucha said. “She can’t lose another kid.”
Firm resolve
A retired police officer and former medic in the Army Reserve, Mucha, 56, made a decision: “I’m not going to let this beat me.”
So she asked Dr. VanderWoude about clinical research trials.
Dr. VanderWoude works for the Cancer & Hematology Centers of Western Michigan, located in Spectrum Health Cancer Center at Lemmen-Holton Cancer Pavilion.
The doctor found two treatment trials that Mucha might qualify for.
The first study rejected her because she has rheumatoid arthritis, an autoimmune disease. But the second trial gave her the green light. She enrolled and began treatments in July 2016 — a 21-day cycle, with CT scans every nine weeks.
The fight had begun.
The research study, sponsored by the drug maker AbbVie, targets adult breast cancer patients in stages 3 or 4 who are not currently on a chemotherapy regimen and who test positive for an inherited mutation of the BRCA1 or BRCA2 genes.
This mutation, which Mucha has, greatly increases a woman’s risk of developing breast and ovarian cancers. It is also associated with increased risk for other types of cancer.
The clinical trial hinges on adding an experimental drug to a pair of standard chemotherapy drugs. The new drug, a PARP inhibitor, aims to stop the growth of BRCA cancer cells by interfering with their ability to repair themselves.
Shrinking lesions
Mucha’s early scans looked promising. At each nine-week milestone, progress continued. Her tumors were shrinking.
At the same time, however, her rheumatoid arthritis waged a battle of its own, causing complications that landed her in the hospital three times in December. Her clinical research nurse, Mollie Lockard, RN, feared she might have to pull out of the study.
But she kept fighting and stuck with the trial. By spring, most of her cancerous lesions had disappeared.
Except for one.
“There was a spot in her liver that I didn’t really think would go away all the way,” said Lockard, who is closely involved with Mucha’s care. “That one was kind of hanging on.”
Treatments continued. Then came another CT in late April. This scan showed nothing.
After starting with tumors totaling 6 centimeters in length, Mucha found herself with a total tumor size of zero. It’s what health care providers call a complete response to treatment — something Lockard’s supervisor said he’s never seen in a treatment trial for stage 4 cancer.
“And I’m like, ‘YES!’” Mucha said, recalling her response.
“I guess you could say I’m kind of scrappy, kind of tough,” she said, laughing.
“Kind of?” asked her son, Malcolm, 20, sitting beside her in a coffee shop. “If someone tells her she can’t do something, she’ll look them dead in the eye and go, ‘Watch me.’”
Making plans
Today Mucha is doing so well that the study’s sponsor has given her permission to alter her treatment schedule so she can take a couple of trips this summer.
One will be a road trip with her husband, Jeff, across the northern United States. They plan to drive up through Michigan’s Upper Peninsula and take U.S. Highway 2 as far west as they can — “probably out to Glacier (National Park) if we can make it,” she said.
And for a week in July, the family will carry on their tradition of volunteering as lighthouse keepers at the Crisp Point Light on Lake Superior.
These plans align with her new priorities in life: enjoying the people in her life and finding something to appreciate in every new day.
“Before, I was always worried about my garden being weed-free,” said Mucha, who worked as a horticulturalist at Frederik Meijer Gardens & Sculpture Park for 14 years after leaving law enforcement. “Now I’m more concerned with spending time with people.”
Mucha said fear of the cancer’s return will always be in the back of her mind, but she’s not letting it bother her as much right now.
“I’m just going to have as much fun living life as I can,” she said.
Her case is a great example of the promise of using targeted, genetics-based cancer therapies.
“We’re finding out that cancer is not just cancer — there’s so much more to it,” Lockard said.
More and more, treatments will be individualized.
Results like Mucha’s give cancer researchers a “dose of energy,” Lockard said.
“You hope that you find something that will provide hope for these patients,” she said. “To be able to do that—it means a lot.”

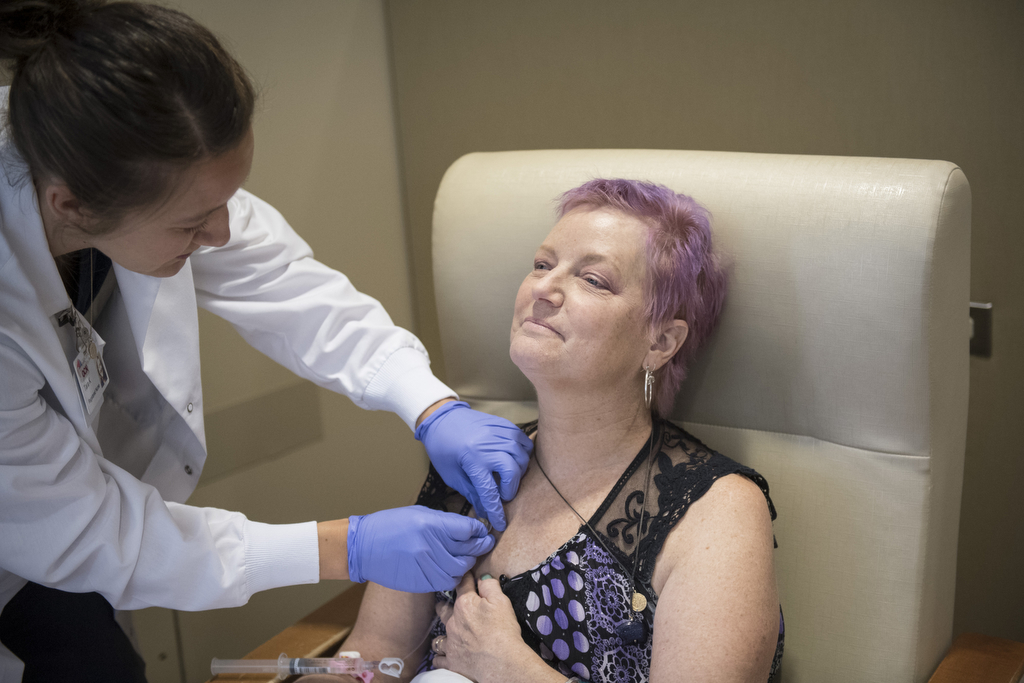
























 /a>
/a>
 /a>
/a>
 /a>
/a>
Wow! What a strong and brave woman! I Iove this story of hope and strength even in the midst of heart break and uncertainty! So happy for her!
Thank you, Heather, for your great comment! We agree 100 percent – she is a super strong, amazing woman. 🙂
I was Michelle’s nurse navigator when she was first diagnosed. It was evident then that she was a fighter and a free spirit – great characteristics that have fueled her on her journey!! Great job Michelle! Jeff – you are a great spouse and caregiver!
As a cancer patient myself with the BRCA2 genetic mutation, i am excited for you on many levels. You are a warrior! Praying for continued success for you and the clinical trial. We are Blessed!
Aw, what a sweet comment, Linda! Best wishes to you, too, on your journey!!
Yeah Michelle!
Keep speaking “Life” Michelle! What a great testimony!
I love this story! I am also a brac2, stage 3b, grade 3, triple negative, breast cancer survivor Michelle – 12 yrs March 4 😊 I participated in a clinical study with a new drug as well. I will pray for a complete mind, body & soul healing 💕
She passed away a day ago from her cancer rip
Very sorry to hear this, Liz. Thank you for letting us know.