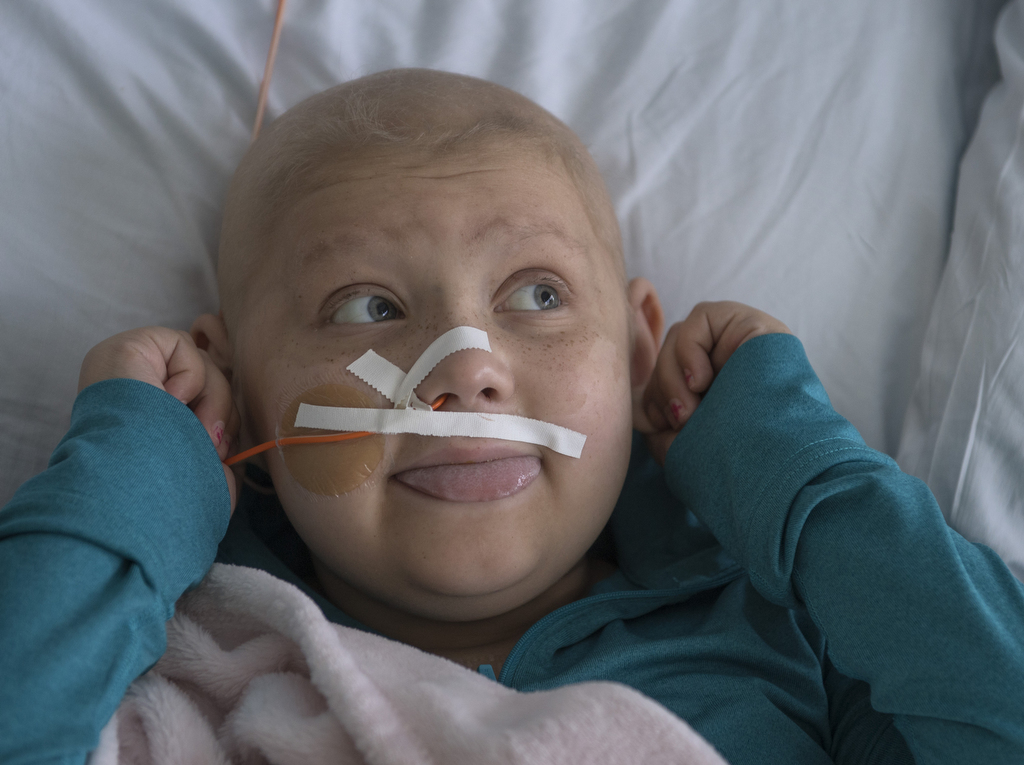
Lily Goodwin’s oncologists use a lot of words to describe her—strong, determined, energetic, honest, ornery, spunky and mature beyond her years.
Her mom calls her smart and sensitive.
Colleen Thompson, who leads a volunteer team that serves pediatric cancer patients and their families at Spectrum Health Helen DeVos Children’s Hospital, calls Lily extraordinary.
“She’s an amazing little girl who is a much older soul than somebody should have to be at that age,” said Thompson, coordinator of the Pediatric Oncology Resource Team, or PORT.
How does Lily describe herself?
“Funny and nice.”
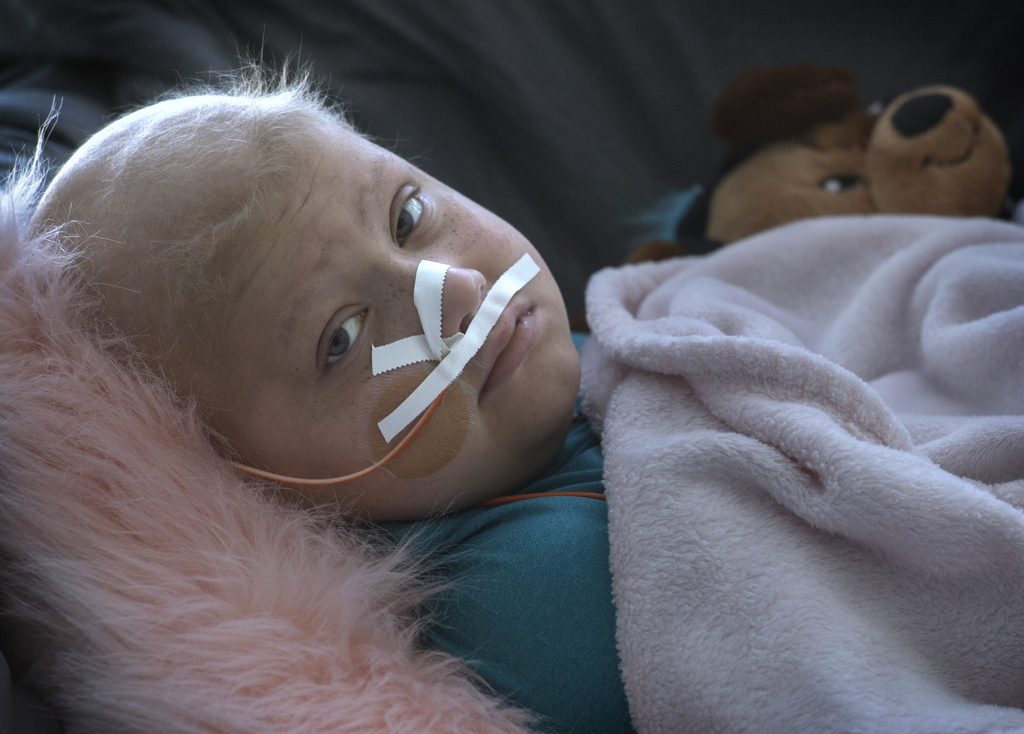
Those two simple words help round out the picture of this resilient girl who last year found herself, at just 7 years old, plucked out of her carefree life and dropped into a world of cancer, chemotherapy and bone marrow transplants.
After everything she’s been through, it’s a joy to see the humor still shining through, Thompson said.
“She is just so funny. She has, like, a wicked sense of humor.”
Seeking survival
Some days, though, it’s hard to find the bright side.
I take every bit of good news as my ‘new’ news. I try to not think about the bad things.
Lily was diagnosed in July 2016 with an uncommon form of leukemia called acute myeloid leukemia.
In one week’s time—what her parents now call Mack Truck Week because of the colossal impact it had on the Ionia, Michigan, family—Lily went from feeling weak and nauseated to being admitted to the Pediatric Intensive Care Unit at Helen DeVos Children’s Hospital.
Her white blood cell count soared dangerously high—so high it caused two hemorrhagic strokes before the doctors could clear her for chemotherapy. After the strokes, Lily needed therapy—speech, physical and occupational—to help her find words and recover from weakness on her left side.
At the same time, her pediatric hematologist-oncologist, Deanna Mitchell, MD, discovered that Lily’s leukemia had a genetic mutation called FLT3, pronounced “flit three,” which makes it much more difficult to put into remission.
A bone marrow transplant offered her only meaningful chance for survival.
Preparing for transplantation involved four brutal, pain-inducing rounds of chemo—the last one designed to kill off any remaining cancer cells and to condition her body to receive the donor’s marrow.
“It’s a hideous experience,” Thompson said, referring to both the preparation and the lengthy high-risk period after transplant.
To lift their spirits, every child who undergoes a bone marrow transplant here gets a “Project Dream Room”—a makeover of their post-transplant room in the hospital, courtesy of PORT, a multifaceted program funded entirely by donors. Lily chose a butterfly-and-flowers theme accented with her favorite color, teal.
By November 2016, four months after her diagnosis, Lily prepped for transplantation. Because there was no family match for Lily’s bone marrow, her transplant came from an unrelated donor found through the National Marrow Donor Program.
The transplant went as planned, and just in time for Christmas, Lily was allowed to go home, though she remained in isolation.
Sucker punch
For the next three months at home, things looked encouraging.
“She was doing great,” Lily’s mom, Kim Girlie, said. “She wasn’t getting sick—she flew through the first transplant.”
Close to reaching 100 days post-transplant—a major milestone on the road to recovery—she relapsed. The leukemia had returned.
The news hit the family like a blow to the gut.
“It was a complete sucker punch,” Girlie said.
Lily returned to square one, or worse. Because now the leukemia proved more aggressive than ever, and the drugs available to target it weren’t working.
Out-of-state relatives came to visit, not knowing how much longer they would have to see Lily.
I have tremendous hope.
In May, Lily’s doctors gave her leave to spend a week with her family at Disney World while she still felt up to it. The trip, sponsored by the Make-A-Wish Foundation, took place over Mother’s Day. Lily’s favorite ride? Space Mountain.
Upon her return, she was again admitted to the hospital. Her health began declining as the cancer cells took hold. In June, she teetered on the brink of life and death.
“We were bringing in hospice in the background,” Girlie said.
After consulting with experts around the country and unsuccessfully petitioning drug companies for compassionate use of investigational drugs, Dr. Mitchell landed on a drug newly approved for adults with FLT3-positive AML—but not children.
Thanks to Dr. Mitchell’s advocacy, the family’s insurance company approved Lily for this new drug, Midostaurin. The hope, the prayer, was that the drug would bring Lily’s leukemia into remission.
“And that one did nearly achieve remission,” Dr. Mitchell said. “Her blast count went down to 3 percent,” indicating a greatly reduced level of leukemia cells in her bone marrow.
A second transplant
As long as cancer cells remained, however, the only hope for a cure would be a second bone marrow transplant and high-dose chemotherapy.
A second transplant is always more dangerous than the first because of increased risks of complications, according to Aly Abdel-Mageed, MD, the section chief for the pediatric bone marrow transplant program at Helen DeVos Children’s Hospital.
“Sometimes when we’re in this situation, the patient has suffered significant toxicity or damage to the organs from the first transplant that precludes going through a second transplant,” he said.
What Lily had going for her, Dr. Mageed said, was that “her organ systems were in relatively good shape to tolerate a second transplant, especially with the intensity that we needed to use to, hopefully the second time around, get rid of her leukemia.”
After careful conversations, Lily, her parents and her medical team decided “that we are not ready to give up and we’re going to try to still go for a cure, despite the odds being against us,” Dr. Mageed said.
One more person not ready to give up: Lily’s bone marrow donor.
“That particular donor was so motivated, and expressed commitment to donate again for Lily if need be,” Dr. Mageed said, even though the donor and Lily are strangers. “It’s a reassuring feeling for all of us, that none of us is in this alone.”
On July 19, Lily underwent her second bone marrow transplant. She also received a second Project Dream Room makeover from PORT, this time centered on the Mexican sugar skull tradition.
Now, two months later, her family and medical team are cautiously optimistic.
“So far she has done relatively well,” Dr. Mageed said. Her heart, lungs, liver and kidneys tolerated the conditioning regimen and the transplant process fairly well, and at this point there is “no evidence of leukemia.”
As Dr. Mitchell said, “The cells in her bone marrow are all from her donor. We’re not seeing her leukemia population—so that’s great. Will it sustain? I don’t know.”
Holding onto good news
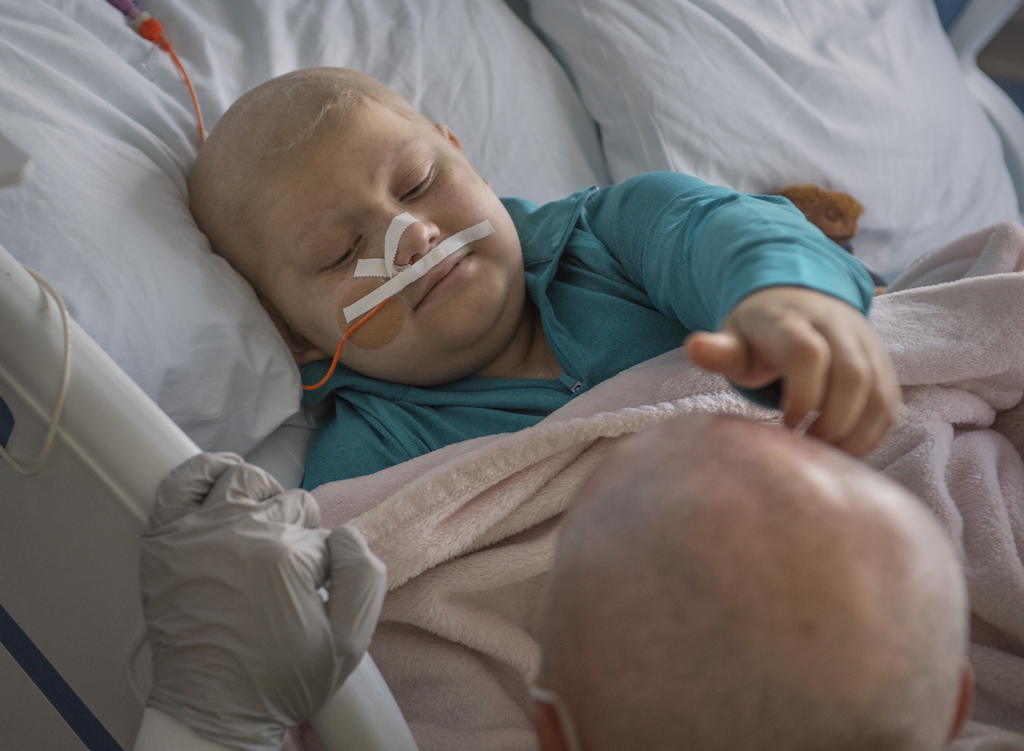
The goal today is to give Lily’s organs time to heal and let the graft—the healthy cells infused—take over and keep the leukemia at bay.
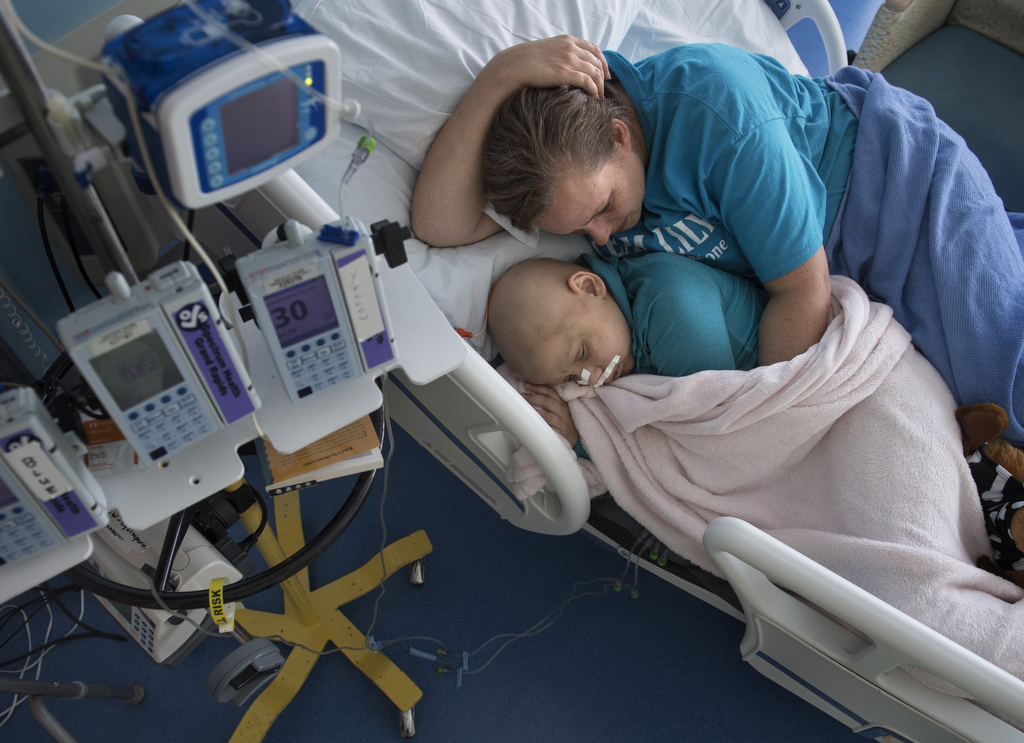
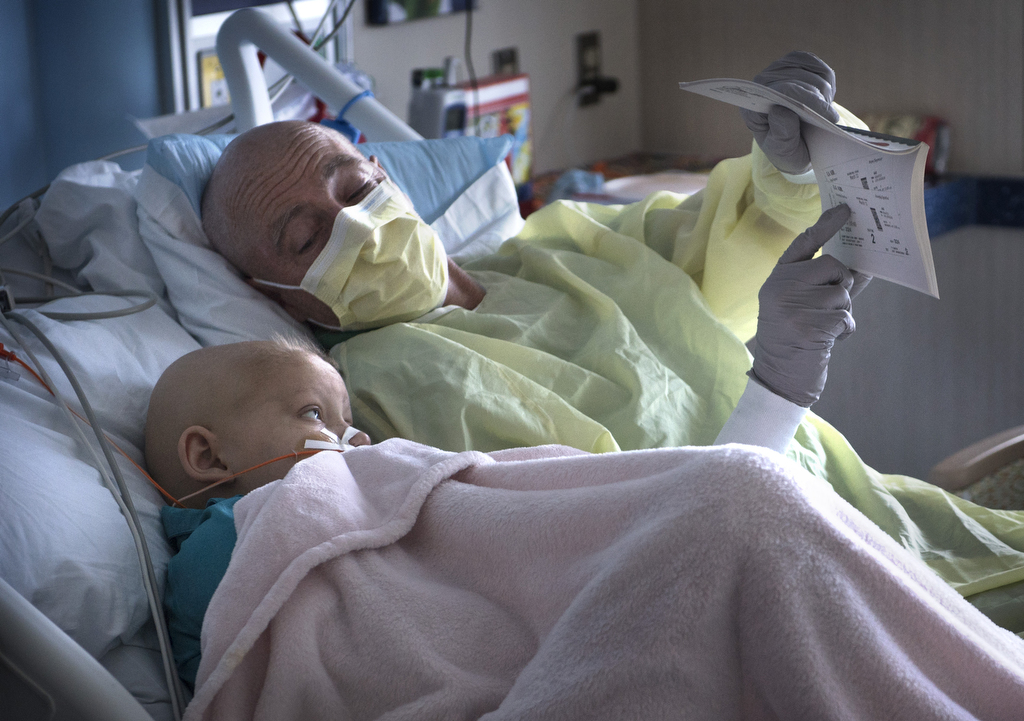
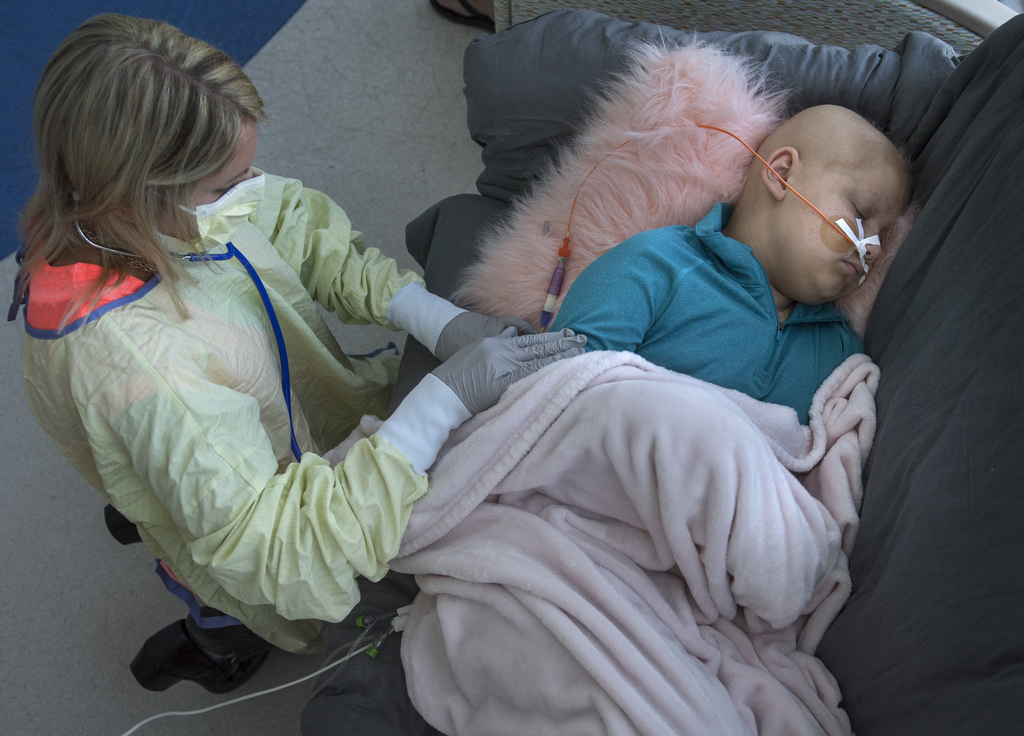
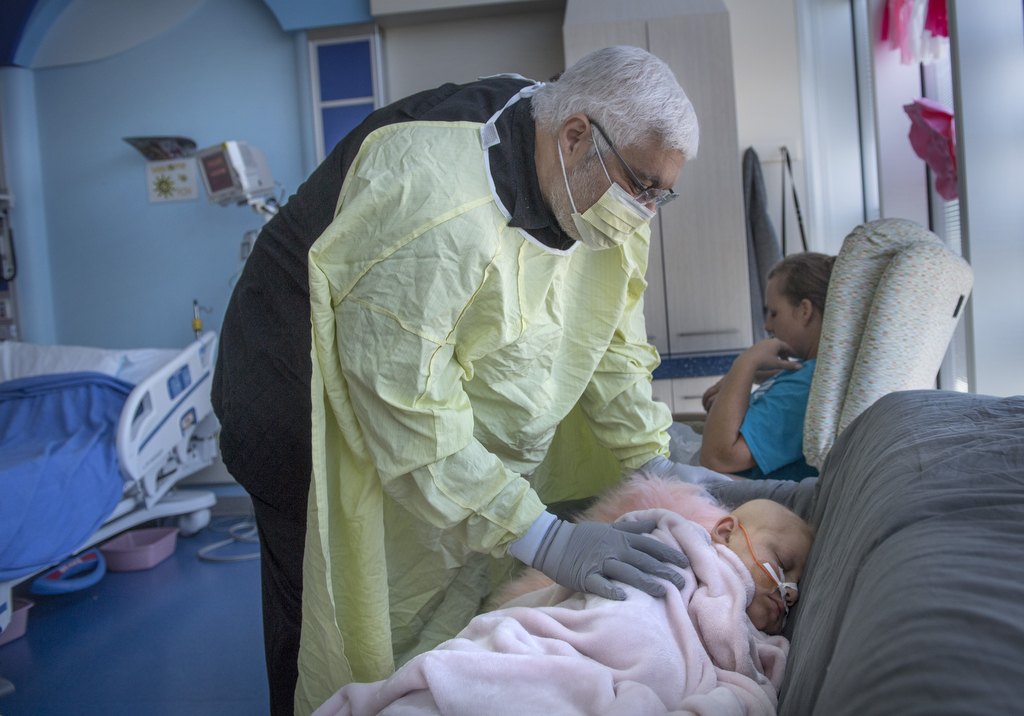
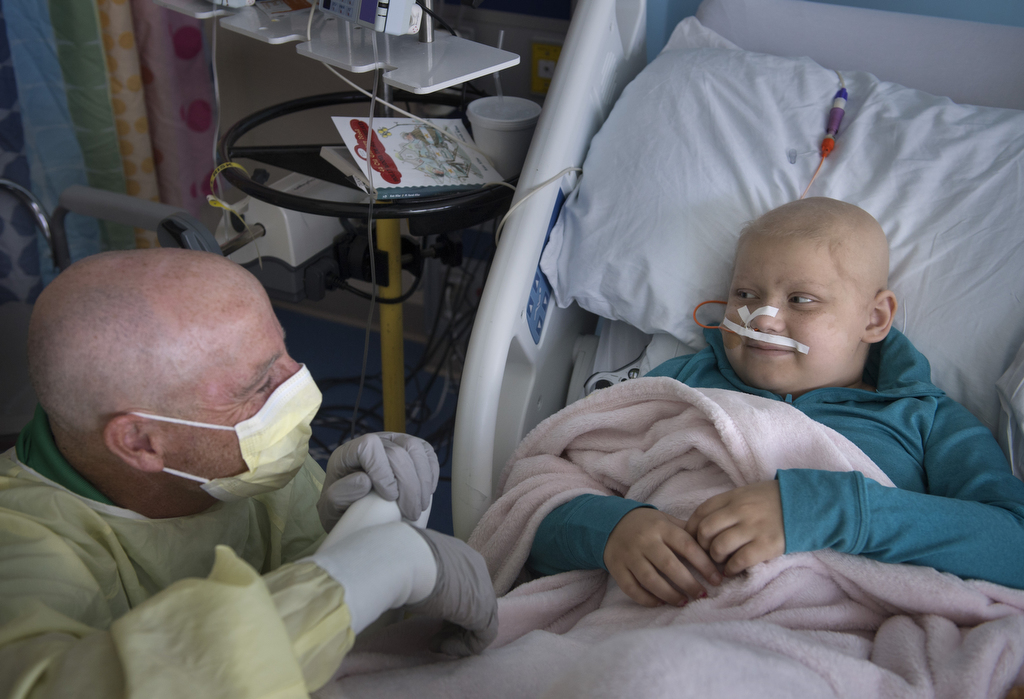
As she bides her time, a team of hospital staff members keeps her engaged and entertained. Child life specialists read, joke and play games with her. Thompson and many others—teachers, nurses, social workers—keep tabs on her daily progress and help mark milestones.
In July, Lily celebrated her ninth birthday. It’s the second year in a row she’s had a birthday in the hospital, and right now she’s not sure how to think about the future.
“It’s hard. It’s hard for her to believe that it will get better, because we told her all that before and she ended up back here,” Girlie said. Plus, she just doesn’t feel very well—she’s suffering abdominal pain from colitis, a result of the chemo.
Yet at the same time, there’s good news. No signs of leukemia in her bone marrow. “That part is amazing news,” Girlie said. “I take every bit of good news as my ‘new’ news. I try to not think about the bad things.”
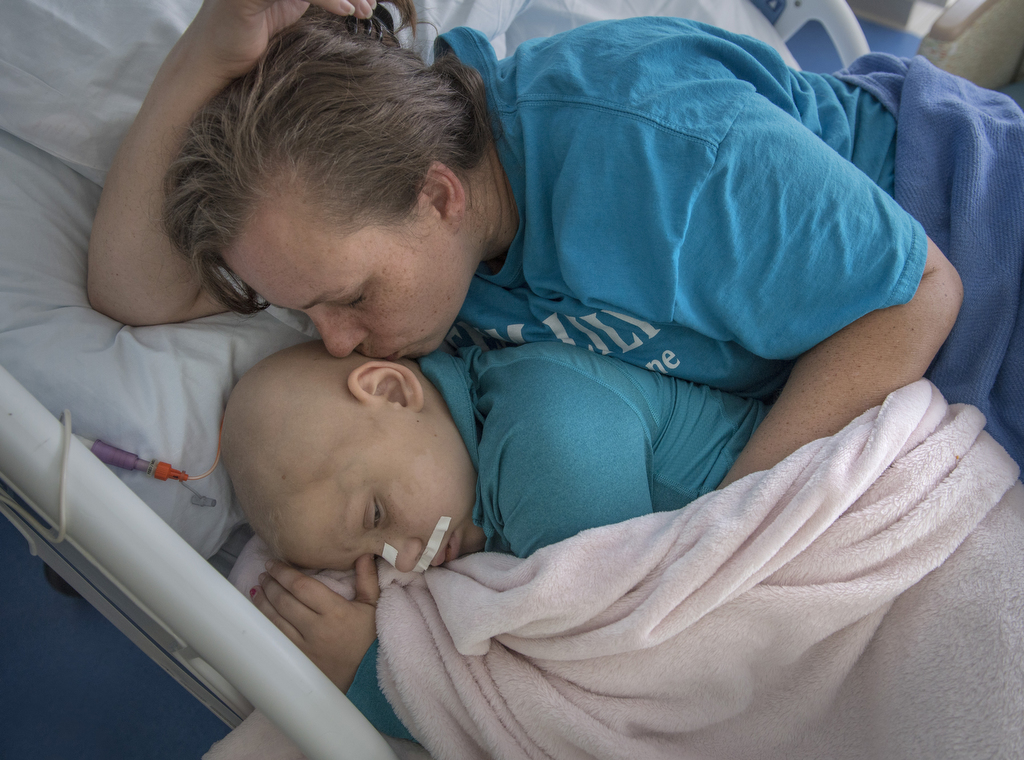
This positive stance is Lily’s mom in a nutshell, according to Dr. Mitchell.
“Her mom is a hero,” Dr. Mitchell said. “She’s going to find the good while there’s good to be found, and I think she does that heroically—and not in a dishonest way. She’s never dishonest with Lily. But it’s not time to mourn, and she takes that approach.”
Despite the uncertainties of Lily’s future, Dr. Mitchell remains hopeful. A wall full of photographs behind her desk testifies to the countless young patients she’s seen beat the odds.
“I have tremendous hope, partly because I go to (former patients’) weddings and see people grow up,” she said. “But also, I see basic science and molecular biology translating to better therapies—better therapies for a cure and less toxic therapies.”
She sums up Lily’s case with thoughtful honesty: “I think we’re persevering with hope but no guarantees, with a very beloved child.”
No matter what happens, Girlie has the comfort of knowing that Lily isn’t afraid. When things were looking bleak last summer, Lily sat with her mom and talked about death.
“She said, ‘Mom, it’s OK if I die because then I won’t have to be here anymore and I can be there with God and he’s gonna make it OK. If he feels it’s time for me to go be with him, then I’m OK with that, Mom, and I’ll be able to watch over you guys and you’re not gonna be alone.’
“To hear your child say that, it breaks your heart,” Girlie said, “but I’m also glad that she’s not afraid because we don’t know, and I don’t want her to be scared.
“But,” she said, “I don’t want her to quit fighting either.”
So today Lily, the mature-beyond-her-years fourth grader, fights on.








 /a>
/a>
 /a>
/a>
 /a>
/a>
Our daughter was in DeVos Children’s hospital before the new one was built. Dr Mitchell is a wonderful Dr. Elizabeth is no longer a pediatric patient because she is now an adult she really misses Dr. Mitchel and the whole team at DeVoss. Lizzie suffered from Setemic Lupus and many other disorders like kidney failure. My heart goes out to this young lady, Lily and her family . Hoping and praying that this bone marrow transplant is successful. And that she is on an upward swing with this battle.