Fifteen years ago, Phil Simon worked as the sous chef at a restaurant and pub in downtown Grand Rapids, Michigan.
One July morning he awoke to discover he’d lost feeling on one side of his body. His speech slurred. His walk looked more like a stagger.
Phil knew something was wrong—but when you have an intense work ethic and the kitchen staff is counting on you, you show up and get started.
Except he wasn’t the only one who noticed the difference that morning.
“People accused me of being drunk going to work, and I was like, ‘No, I’m not drunk. … I swear to you, I’m sober.’”
Phil went to see his doctor, who referred him to a neurologist, D. Eugene Wiley, MD, who ran some tests and sent him for an MRI.
Soon the diagnosis came: Phil had multiple sclerosis, or MS, an incurable, unpredictable central nervous system disorder that disrupts communication between the brain and other parts of the body.
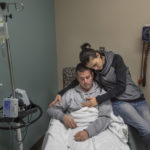
Phil and his wife, Jennifer, then both 23, had a baby at home, their son Cole. The couple, culinary school sweethearts, had their eyes set on career and family.
Phil had no time for this kind of disruption.
Plowing ahead
Phil’s neurologist prescribed Rebif, an injectable drug that can slow the progression of the disease. Phil began giving himself shots three times a week and resumed life as usual.
For the first few years, the medication did its job. Phil tried hard to convince himself his life remained the same.
Though he experienced symptoms—including, at times, mental confusion—he kept these things to himself around his co-workers.
“You’ve got to put your best foot forward,” he said. “They don’t pay me to be weak.”
Then, after seven years of shots—years that included the birth of the couple’s second son, Avery—an injection site on Phil’s upper leg became badly infected, requiring surgery.
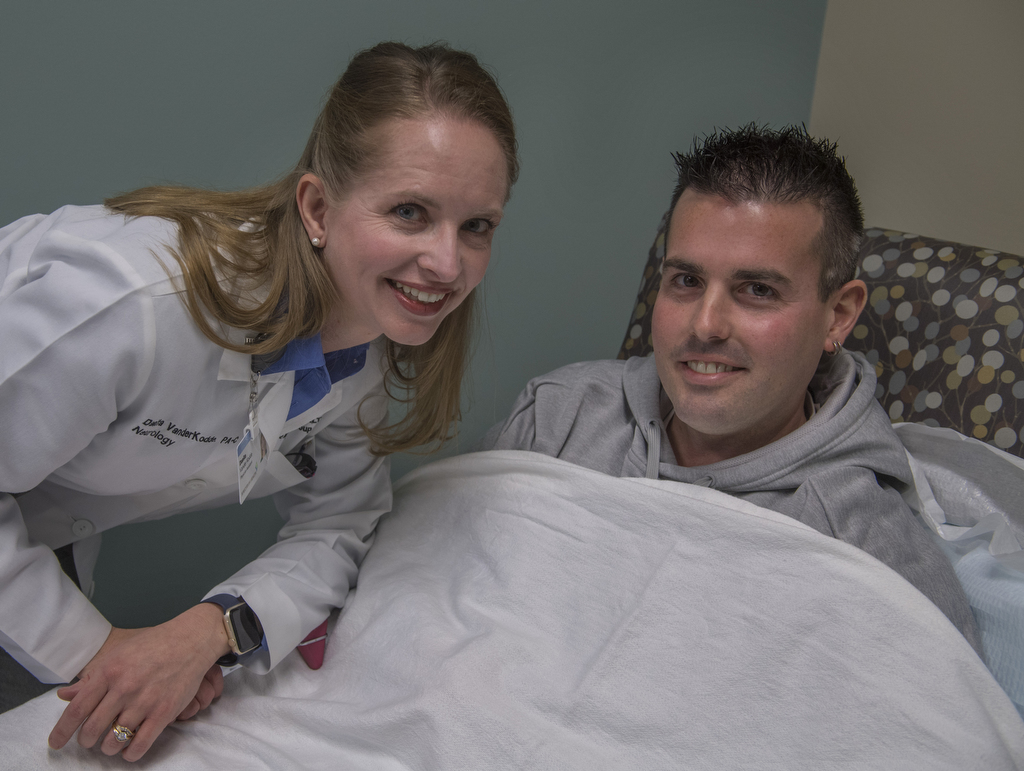
Working with Danita VanderKodde, PA-C, MSCS, a certified MS specialist with Spectrum Health Neurosciences who has helped manage his care for the last 13 years, Phil decided to ditch the needles and move to a daily oral MS medication, Tecfidera.
Serious setback
Three years later, in 2013, another complication surfaced.
VanderKodde discovered a nodule on Phil’s thyroid gland that turned out to be cancerous. It needed to come out. During surgery to remove the thyroid, doctors also removed a tumor wrapped around the front of his neck.
High-dose radiation treatment put the cancer in check, but the whole event threw his body for a loop. He pushed through a rough recovery.
“You didn’t know if it was still him recovering from cancer or if it was his MS going, ‘Wait, hello! I’m here, too,’” Jennifer said.
Phil soon returned to work, although it became clear a chef’s life wouldn’t pair well with the effects of MS.
In 2015 he packed up his knives and left the career he began training for at age 14. He went on disability and became a stay-at-home dad.
“He was a chef working 18 hours a day,” Jennifer said. “He never sat down, he never stopped moving. He was working himself into the ground.”
Today, the two have swapped roles.
Jennifer is working full time as a retail team leader and Phil is home, wishing things were different. It proved to be a big life change for the Hudsonville, Michigan, family—and they’re still adjusting.
“It was a learning experience, for sure,” Jennifer said. “We’re still learning.”
New hope?
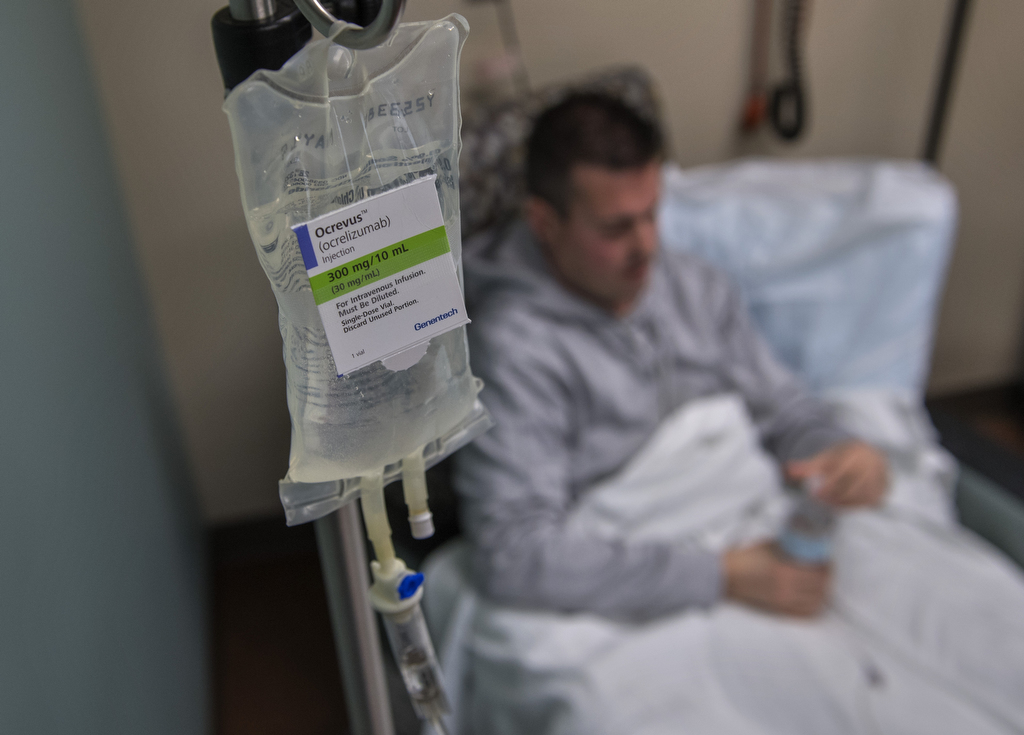
Last year, a new MS medication, Ocrevus, hit the market. It made a huge splash when NBC News featured a clinical trial patient who experienced an incredible turnaround on the drug, getting out of her wheelchair and walking again.
People called it a game-changer, a miracle drug.
And it will be—for some patients.
“This is one of only a couple MS therapies with proof—statistically analyzed proof—that some people got better over time,” VanderKodde said.
The drug is approved for patients with the most common forms of MS, including the relapsing type that Phil has. It’s also the first drug proven effective for primary progressive MS, a less common but more aggressive form of the disease.
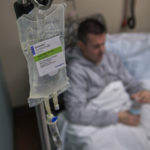
Ocrevus, which is administered by twice-yearly infusion, uses a different mechanism of action than the other 15 or so MS drugs on the market.
“So this is brand-new territory in MS, and that’s the big hope here—that we’re in a whole new level of MS care,” VanderKodde said.
MS is an autoimmune disorder—a disease that causes the body to attack itself—and Ocrevus works to prevent targeted cells from eating away the myelin that protects the nerves of the central nervous system.
By calming down this subtle, ongoing attack, the drug makes way for the body to heal itself.
In clinical trials, Ocrevus was 46 percent more effective at reducing disease relapses than Phil’s first drug, Rebif, which has about a 30 percent relapse reduction rate.
“That’s a pretty good sell, but it’s still not perfect,” VanderKodde said.
She expects patients to see results, but not the dramatic outcomes highlighted in the national news.
“I don’t want to promise anyone, ‘You’re going to get up out of the wheelchair,’ like they showed on TV,” she said. “That was a very special case.”
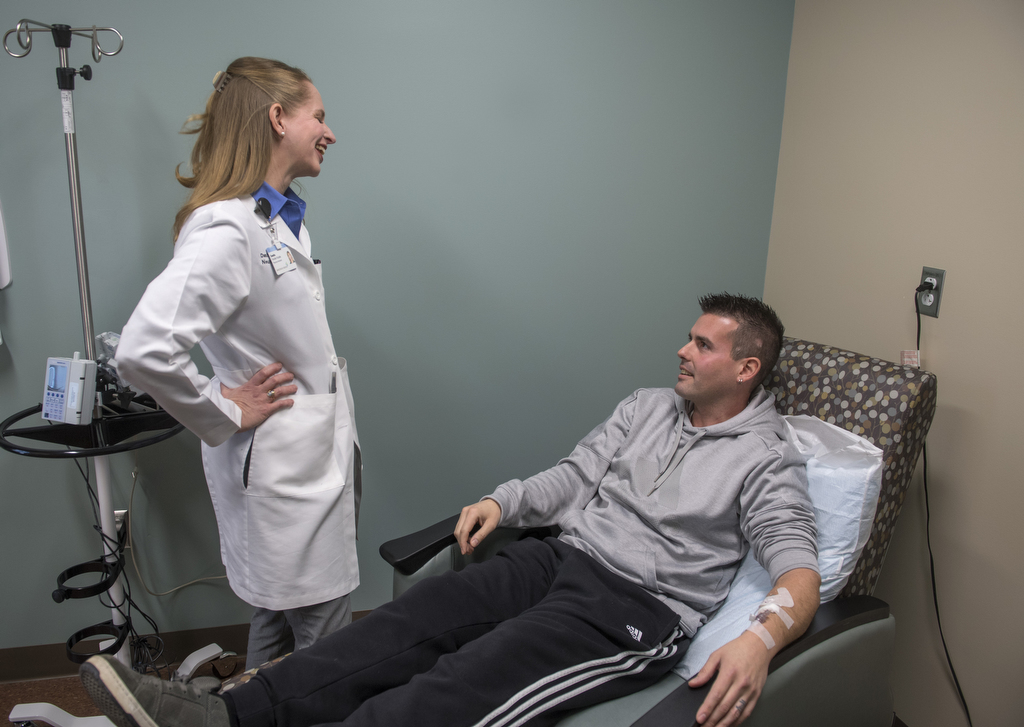
At her office in the Spectrum Health Integrated Care Campus on the East Beltline in Grand Rapids, VanderKodde is part of a collaborative team of neurology providers, including Cynthia Hingtgen, MD, PhD, who together serve more than 1,000 MS patients from across Michigan.
“Unfortunately, it’s really common in our region and we don’t know why,” VanderKodde said. “It’s partly genetic, partly environmental, partly infectious. We don’t know the cause.”
Last May she started her first patient on Ocrevus—a primary progressive MS patient for whom there was no previous therapy.
That patient hasn’t been healed, but she’s at least held steady. That in itself is good news.
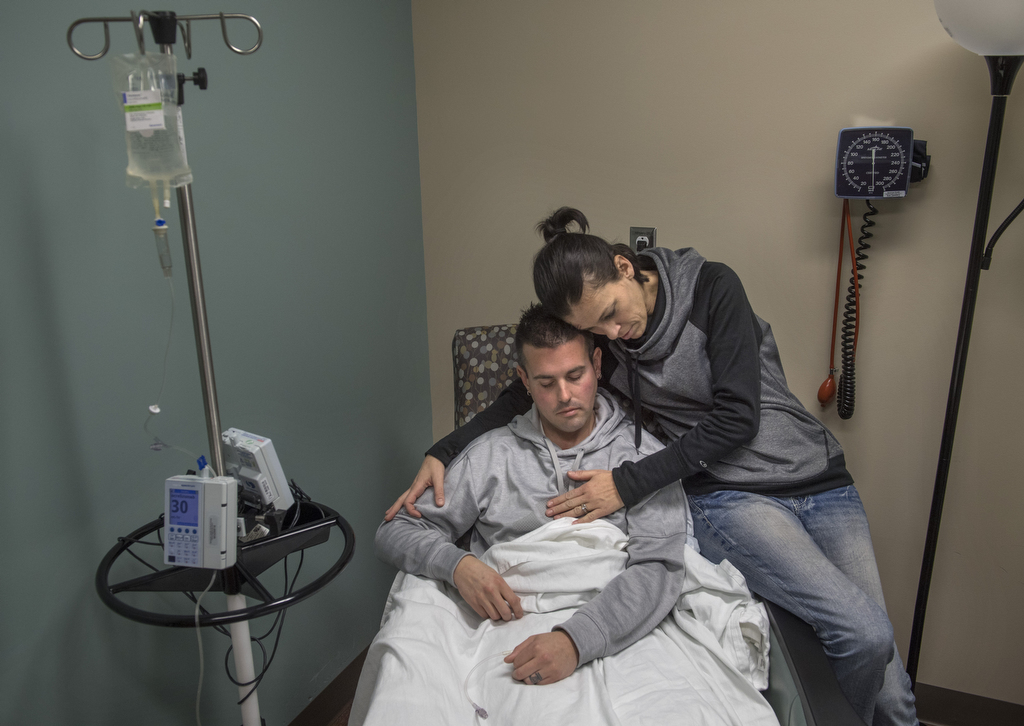
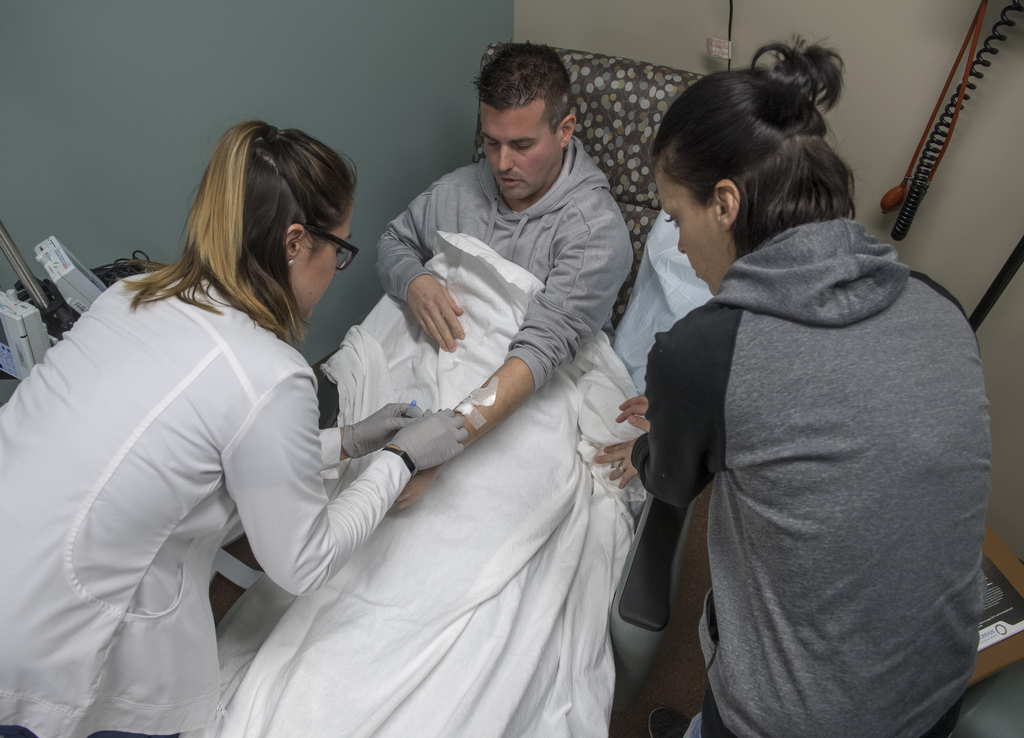
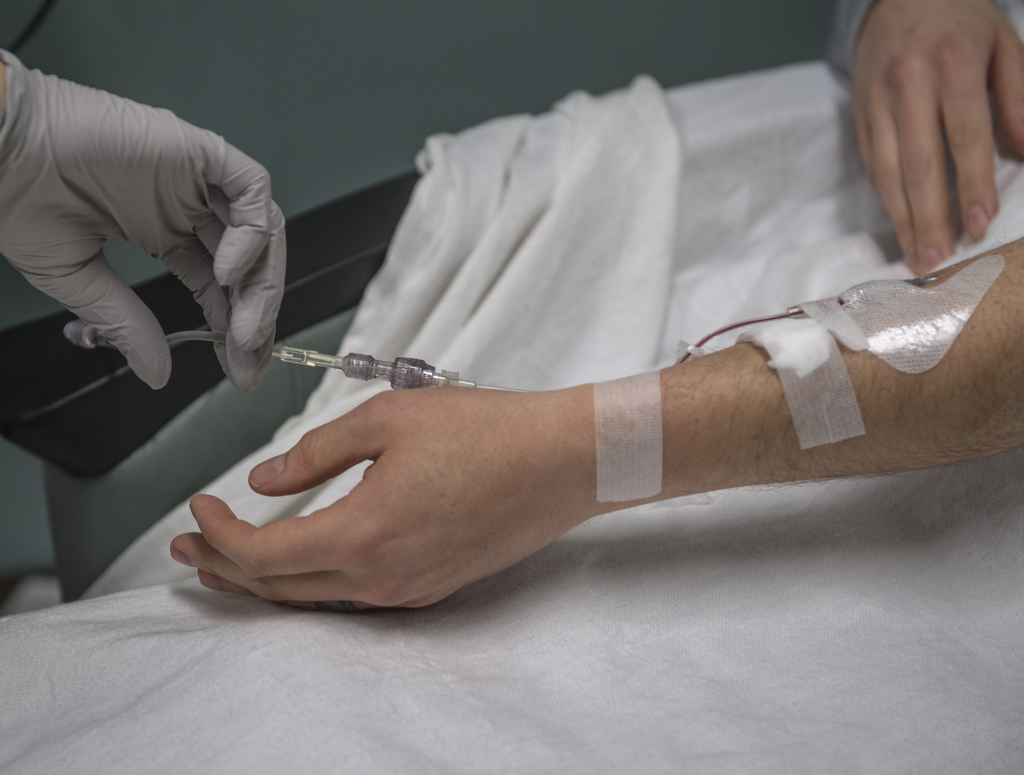
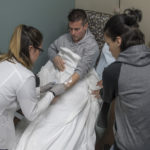
Phil became a new Ocrevus patient on Jan. 17, 2018, when he received his first infusion, at Spectrum Health.
Though not everyone is a good candidate for this new drug, Phil is, VanderKodde said. He’s young (only 38), he’s in decline and he needs a new intervention.
“He’s getting worse and he’s tried what I have,” she said. “Without this medication, he will decline. Without this medication, he’ll be in a scooter or a wheelchair and continue to struggle with relationships and memory and fatigue.”
Fatigue is actually one of the first things that should improve for him on Ocrevus, she said. The other hoped-for effects will take longer to see.
“The people who got better, statistically, got better within a year and a half.”
Daring to dream
Phil knows this is a critical moment in the progression of his disease. He’s pinning his hopes on Ocrevus.
“The drugs I’m on aren’t working,” he said. “I’m confused a lot. My walking isn’t as good. I don’t feel as strong. I don’t feel as confident.”
When he dares to dream about the future, Phil thinks about the family vacations he’d like to take.
“He wants to go back to Disney World and be able to walk it,” Jennifer said. “Because right now that’s not attainable. He would have to be in a scooter.”
VanderKodde didn’t rule out this goal.
“I think it’s possible,” she said. “But it’s not just the drug. It will take the drug and healthy eating and healthy living and physical therapy. But he’s willing to do it, so I think it’s possible.”
Phil wants to give it everything he has.
“I’m never going to be the 19-year-old Phil running around like I used to be, but, you know, anything I can do to get anywhere as close that I can get, I’m going to do,” he said.
It’s about holding onto everyday life as long as he can, as best as he can.
“He wants to be able to go to the boys’ sporting events, be in the bleachers and not stand out,” Jennifer said. “Just be another parent.”


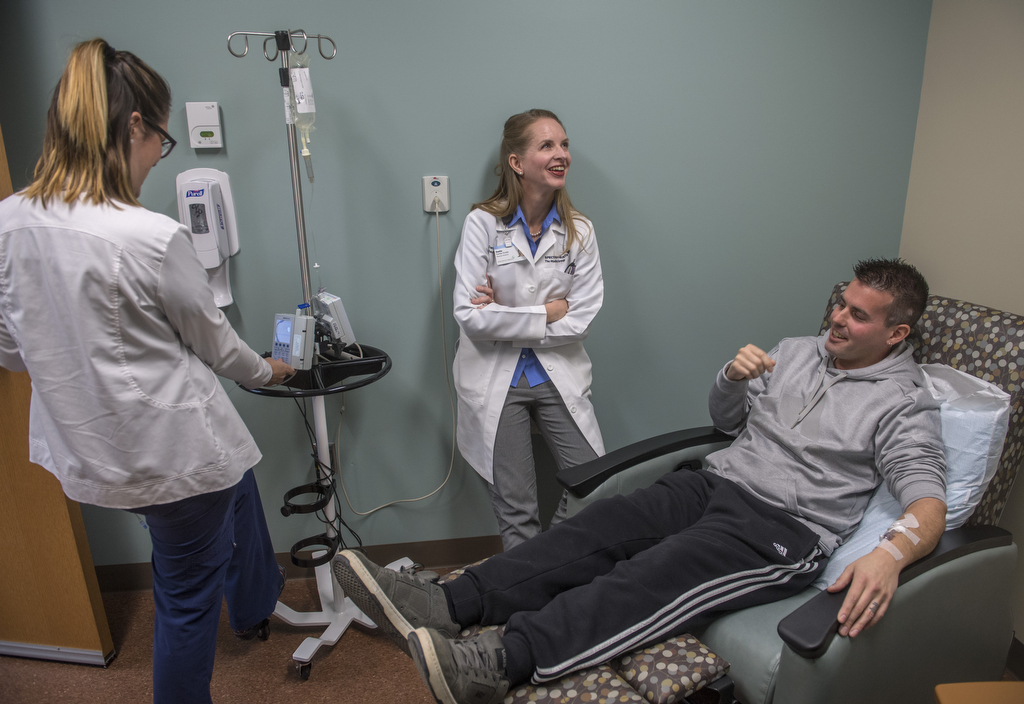















 /a>
/a>
 /a>
/a>
 /a>
/a>
Phillip is my nephew and he has been fighting this disease for years with honor and dignity. He’s an awesome Dad, husband, nephew, son, grandson etc…and we couldn’t be prouder of him in this gallant fight! Love you Phillip..💜
I used to work with Phil and I never knew all of this I was there when they found cancer … but the rest I didn’t know thanks for sharing ur story … I hope and pray this works for you ! Your a hard worker a great person and detergent this ! I hope you get better phil!!
Much love and many prayers to Phil, Jen, Cole and Avery. We love you guys! ❤️
God bless Phil! You Got This!!!
Strength to you Phil and your family❤️. My nephew has MS diagnosed at 24, it’s tough but you have to keep at it!!
Why aren’t more doctors treating MS patients with Low Dose Naltrexone? It has VERY low side effects and can be used along with other treatments. It is successfully used for other autoimmune diseases as well as MS.
Thank you for your comment, Jay. We are fortunate there are many options physicians are able to investigate in treating people with MS and similar conditions. Here’s a recent study on naltrexone that is interesting, if you haven’t seen it before: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3962576/ Best wishes, Cheryl
My daughter with MS just started Ocrevus in November and so far seems to be doing well. I hope you have equally successful results, Phil. MS is so darn complex, with so many unknowns. May you feel strength in the love of family, the prayers of many, and the ever improving drugs to help manage the disease. I wish you all the best.
Thank you, Jan, for your encouraging words. We are so happy your daughter is doing well on Ocrevus. Thank you for being a Health Beat reader and contributor and best wishes to your family!
I am Grandma to Phillip Simon. He is a wonderful young man, deserving of love, healing and prayers. It breaks my heart to know he has this horrible disease, and I pray daily that he can be healed to stay with all of his family for many more years! I love you Phillip! Grandma Simon.
Thank you, Dorothy! Your grandson is special, indeed, and we are so hopeful for him and your family! Best wishes!
I love reading these stories about the strength and determination you all have. I wish pain and suffering didn’t exist…but since it does, our love, hope and prayers go out to all of you. Someday I hope you will be able to travel with your family….but until then, we all admire your courage and pray for strength on this journey.
My husband and I have both been diagnosed with cancer. Although in our 60’s, we share many of the hopes, dreams and concerns. Our advice: keep dreaming! Modern medicine has come a long way. Take a deep breath and the next step. It is a whole new tomorrow.
Thank you, Linda, for your kind words of encouragement. You and your husband are amazing. Best wishes to all.
God bless you. Without God there is no hope. The only hope that you meant is called Jesus our Lord and Saviour. For His blood and wound we were heald and saved. We must claim this promises; that what the bible says. Have faith and read your bible to gain strength.
God is a God of miracles. God of the impossible. When all choices, options and human efforts end at nothing that is when we have to have aside. From there on we have to call up on Jesus. Cast your worries, troubles, needs and your life on His hand and let God start to work to His honor and glory. I will be playing to thank God for this miracle.
You have a beautiful family. Get together to read, study the bible and pray. Give God His honor and glory in Jesus name. The bible says where there are two or more in my name there He is. God bless you all. Keep faith up.