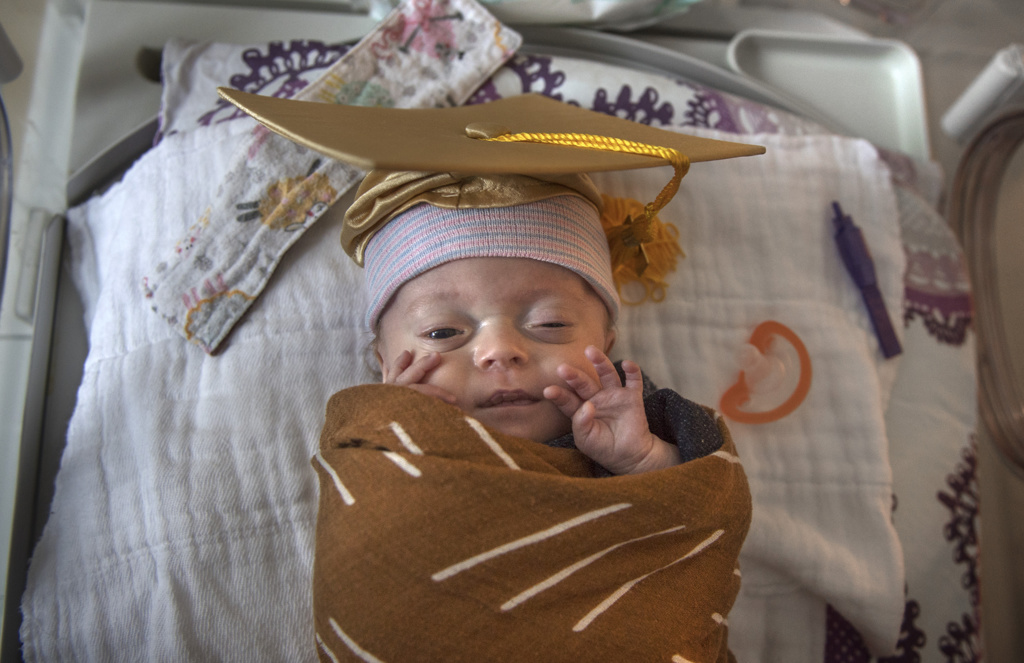
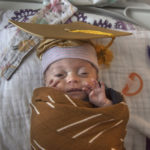
Brooke and Randy Sherrell cried upon seeing their daughter in a graduation cap.
But this precious moment had nothing to do with pomp. It’s about circumstance.
Little Lexanne, their precious newborn, had just graduated from the NICU in the Gerber Foundation Neonatal Center at Helen DeVos Children’s Hospital in Grand Rapids, Michigan.
“Oh, baby, you’re doing it,” Brooke said, as she and her family prepared to go home after 124 days in the hospital. “She’s like ‘I have earned this.’ She has earned every second of that cap. Soak it up. Look at you, big girl. You did it! You graduated!”
Moments weren’t so celebratory when Lexanne arrived on Sept. 24 during an emergency C-section. She made it to life. Her twin sister did not.
“I was pregnant with twins,” Brooke said. “In August, we got the diagnosis of twin-to-twin transfusion syndrome.”
Blood vessels in the placenta didn’t develop properly, causing one twin to give a majority of nutrients and blood flow to the other twin. Lexanne was on the receiving end; her placenta partner, the giver.
“The biggest risk was losing the twin that was giving all the nutrients,” Brooke said. “She was giving nutrients and she also had a very poor percentage of the placenta she was connected to. It was awful. Every single appointment we went to, we never knew if that was going to be the one where they’d say, ‘We’re sorry, she’s gone.’ Or, ‘They’re both gone.’”
A tense transition
Doctors put Brooke on bed rest, to preserve blood flow for the babies.
“In September, I had to have surgical intervention or we could have lost both of them,” Brooke said of her experience at a medical facility on the east side of Michigan. “It looked like everything went well, but following up just before discharge, we found out we had lost the smaller twin. The ultrasound technician did all the studies on the surviving twin first. She scrolled Eliza. She said that Eliza had passed. It was really hard, a terrible, terrible day. I was at 22 weeks.”
The following week, Brooke made an appointment with the Spectrum Health maternal fetal medicine team for Lexanne, the daughter still growing within her womb.
Then, another unexpected twist—she experienced early labor, likely due to stress.
While still on the other side of the state, she delivered, via emergency C-section.
“My husband walked in 30 seconds before my daughter came out,” Brooke said. “They delivered (Lexanne) at 1 pound, 5 ounces. She was tiny. They also were able to deliver Eliza. Randy and I got to hold her and say our goodbyes.”
Lexanne spent a month in the hospital there, then transferred to Spectrum Health Helen DeVos Children’s Hospital via ambulance on Oct. 24.
“She’s had seven surgeries,” Brooke said of her baby girl. “She had two bowel ruptures that required drain placements. Then, she developed a gut infection. They did a surgery to fix scar tissue inside her intestines and place a feeding tube. She also had a hole in her heart.”
While this is common in premature babies and normally closes by itself, hers was so large it caused her lungs to bleed internally. She also suffered bleeding in her brain at birth because her blood vessels were so fragile.
That’s not the end of the medical trauma. Lexanne experienced hydrocephalus, fluid buildup in the brain that required a drain in her head.
“Twice a week they had to go in with a needle and pull fluid off her brain,” Brooke said. “We will do that until she’s like 6 months old. She has bleeding in her eyes that can cause scar tissue. If it’s not treated with laser surgery, it will cause blindness.”
A strong little girl
Despite the obstacles, little Lexanne is going strong.
“She has passed through it all with flying colors,” Brooke said. “I don’t know if there will ever be a stronger girl. We have a really unbelievable supportive community through our church and friends. There were lots of people praying for us and digging really deep into their own faith.”
And on this day, graduation day from Helen DeVos Children’s Hospital, it all came together. Pomp, despite the circumstance.
A graduation ceremony from Child Life staff, for a child whose life hung in the balance for so many months. A metaphorical journey down an aisle; a road that leads from hospital to home.
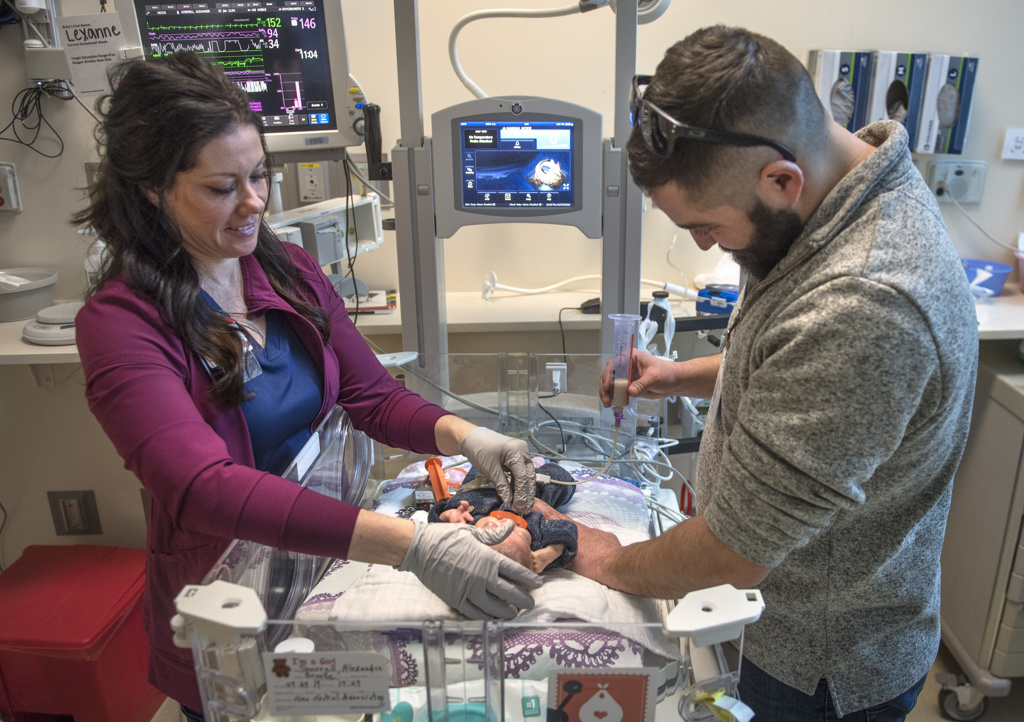
Brooke and Randy received lessons on how to feed their precious daughter through her feeding tube. Brooke spoke with a dietitian on the phone about ordering supplies.
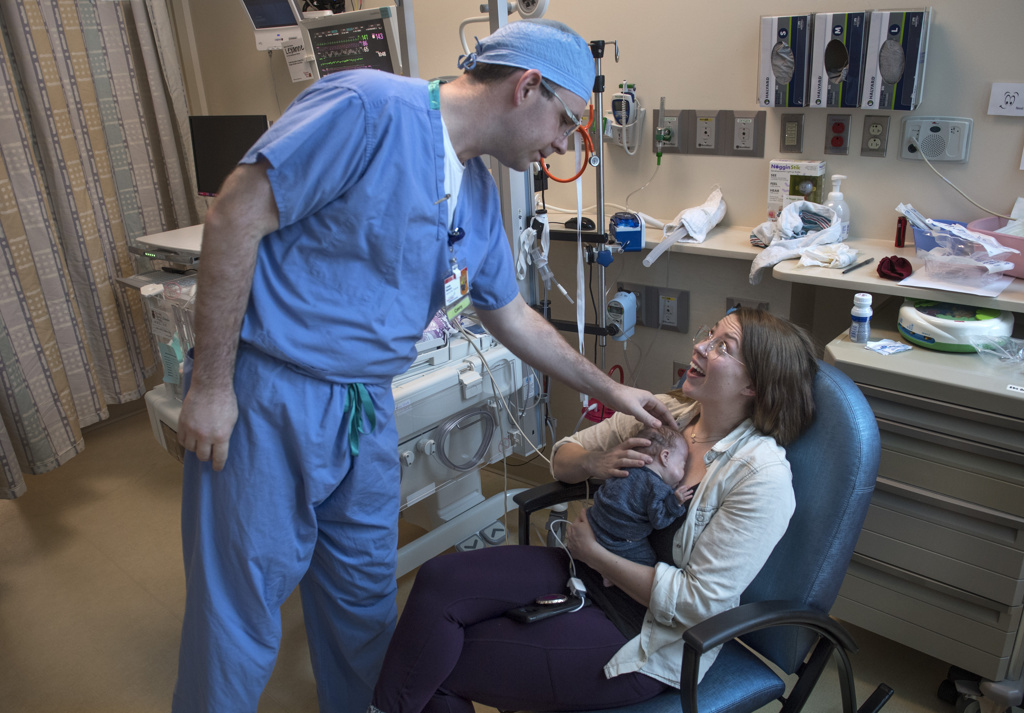
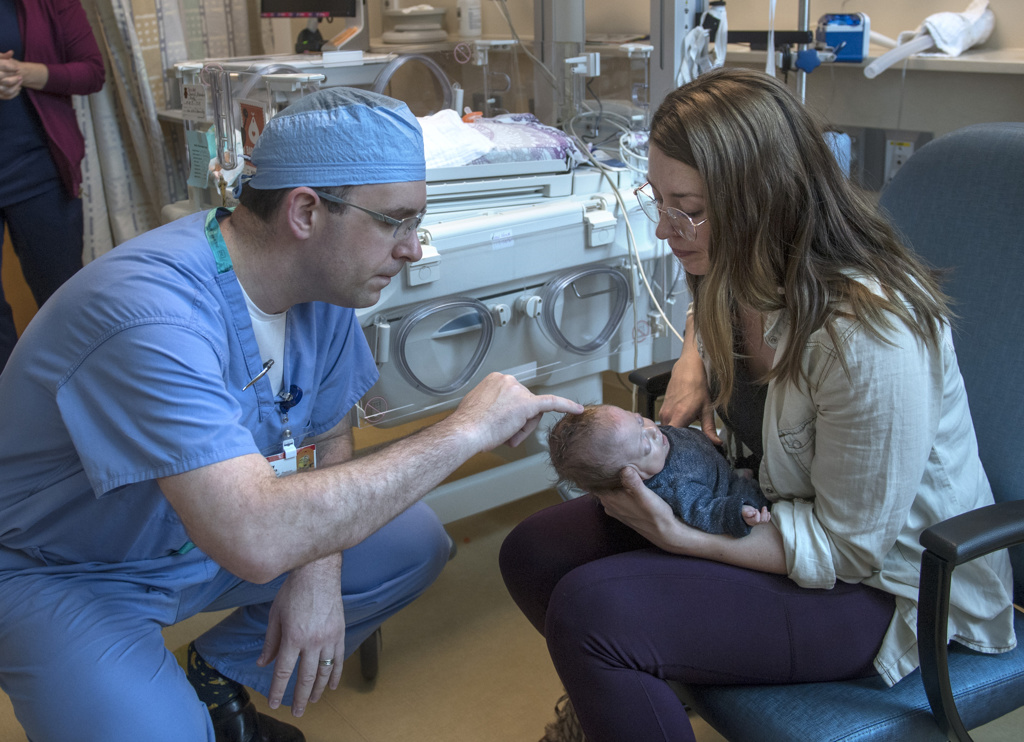
Casey Madura, MD, a Helen DeVos Children’s Hospital pediatric neurosurgeon, visited with the family shortly before she left the hospital.
“You’re going home today,” Dr. Madura told Brooke and Randy. “Does that feel great? We’re going to see you a bunch, but it’s going well.”
When Brooke and Randy asked what they should be aware of, Dr. Madura instructed the family on symptoms to watch for.
“The real answer is, just be her parents and pay attention to her,” he said. “If you don’t like what’s going on, call us. She’s done really well in the last couple weeks. She’s clearly made progress. Now, she gets to go home.”






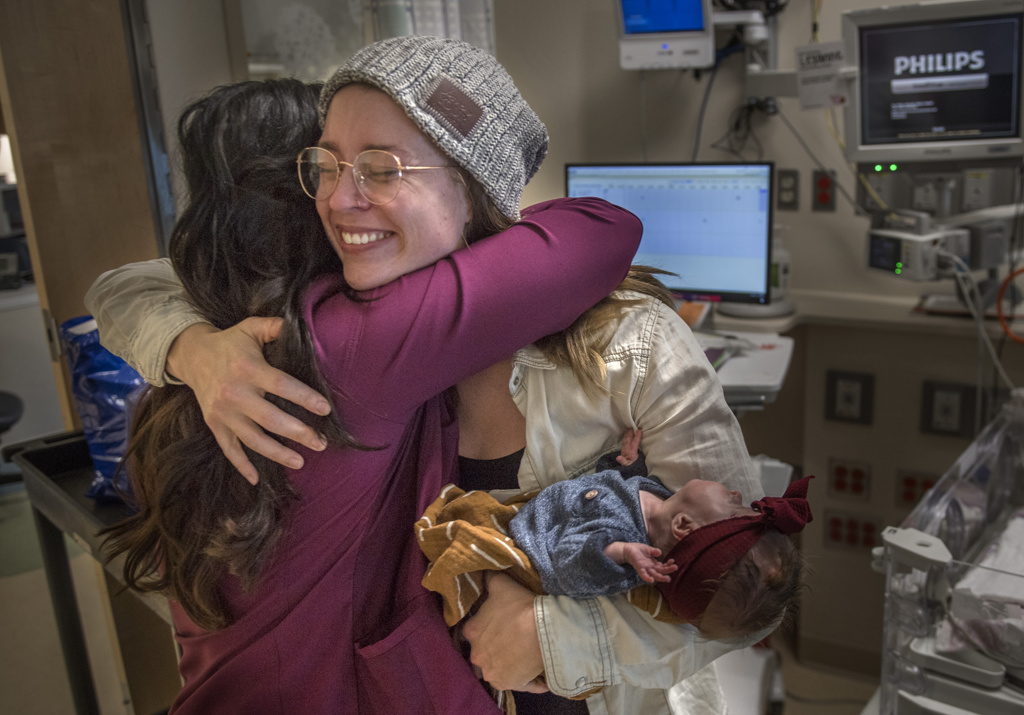


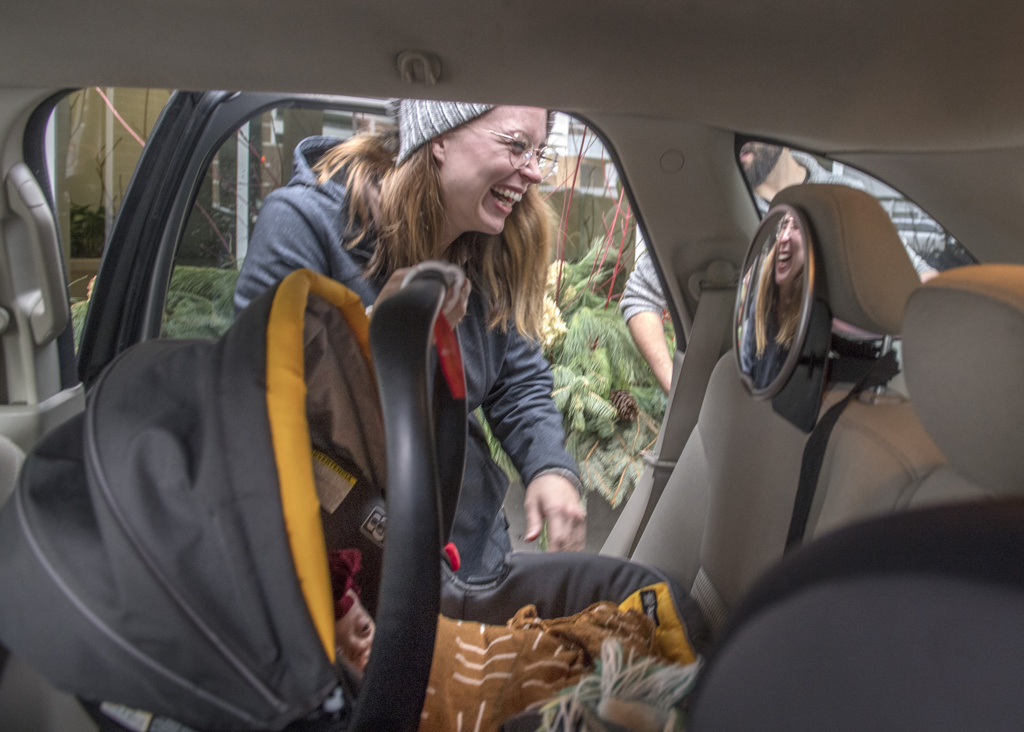












 /a>
/a>
 /a>
/a>
 /a>
/a>
What a wonderful story with a happy ending. I’ll be praying for little Lexanne and partners. God bless you all!
Parents*
What a sweet little peanut.