With COVID-19 cases on the rise, Ryan Thatcher hopes people take the virus seriously.
He knows firsthand how deadly the virus can be. In April, Ryan cared for patients in New York City, one of the nation’s first coronavirus hot spots.
“It was the scariest thing I’ve ever seen as a nurse,” Ryan said. “It was essentially a war zone. It’s the only way to describe it. Everybody was sick. All the hospitals were at or above capacity— it was crazy.”
A Navy reservist, Ryan was activated to serve for six weeks as a med-surgical nurse at Bellevue Hospital.
The oldest public hospital in the nation, Bellevue Hospital is also one of the largest with more than 800 beds. In April, at the peak of the COVID-19 outbreak in New York City, patients filled its hallways and rooms.
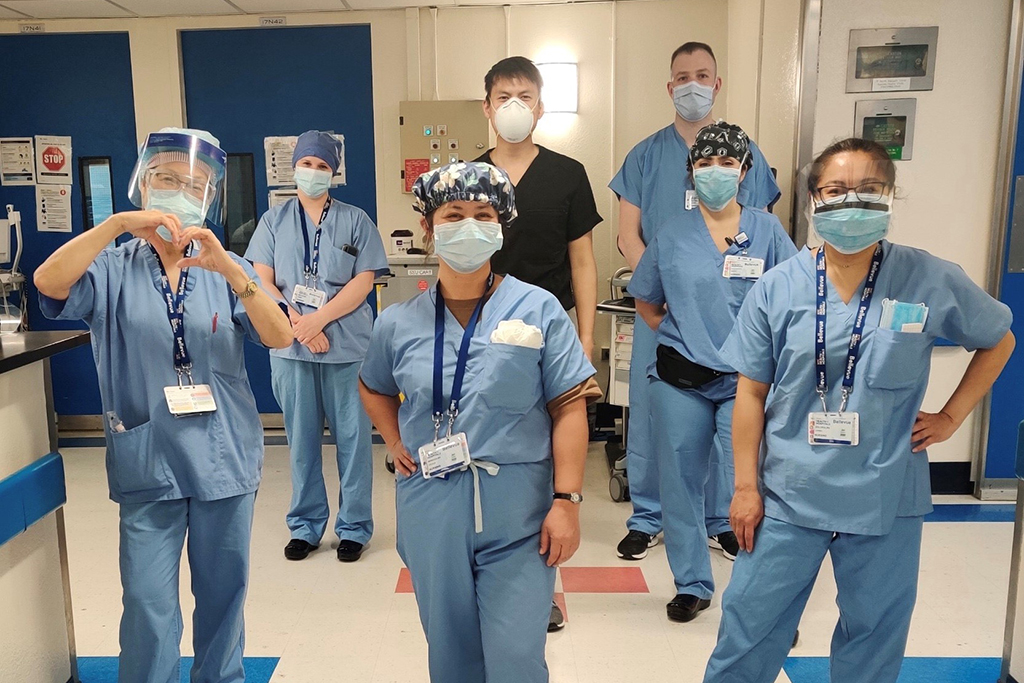
Ryan became one of more than 200 Navy Medical Support Team reservists called upon to care for people in New York City hospitals. About 30 nurses and doctors deployed to Bellevue Hospital.
When he got the call, help was needed immediately, and Ryan had only a day to pack his bags. He learned on Saturday, April 4, he’d be flying out of Detroit the following day.
He needed to inform his employer. Ryan works as a clinical regulatory specialist for Spectrum Health Big Rapids and Reed City Hospitals.
And he had to say goodbye to his husband of six years, Christopher, leaving him to take care of the chores on their busy 40-acre farm in Mecosta County.
‘OK, love you, bye’
Christopher, a nurse at Spectrum Health Kelsey Hospital in Lakeview, grew up in a military family and understood the drill when duty called.
“I know all about the military, so when you have a loved one who is in the military, you’re in the military,” Christopher said. “When the military calls, you’re like ‘OK, love you, bye’ and you just roll with it.”
But he had natural concern that Ryan would be exposed to the virus.
“It worried me, because being a nurse, I knew what the virus could do to people,” Christopher said.
Ryan said by the time he arrived in New York, hospitals had already learned tough lessons regarding the proper use of personal protective equipment, commonly called PPE.
“I was a little worried in the beginning, but by the time we got there, the PPE was in place, and donning and doffing was drilled into our heads before we even touched a patient,” he said.
Ryan worked on 14 North, a 40-bed progressive care unit full of COVID-19 patients.
The unit nurse manager died of the virus the week after he arrived. “From what I understand he was a very, very nice guy.” Ryan said. “They all loved him.”
The loss devastated the unit staff members.
“They were all heartbroken and terrified,” Ryan said.
“Even if you didn’t die, people were so, so sick,” he said. “It was very random. It wasn’t always the unhealthy people. We would have some fairly healthy adults come in and end up on a ventilator for 30 days and then die.”
Because there is no treatment for the virus, Ryan said that made caring for the patients more frustrating. “It was a lot of supportive care; giving oxygen, medicating for pain—those type of things, but there was no treatment.”
Ryan worked 12-hour shifts, two days on, two days off for the six weeks.
‘New York was a ghost town’
When not working, he stayed in his Manhattan hotel room or within a mile radius of the hotel. When he ventured over to the nearby Times Square to check it out, the eerily empty streets chilled him.
“The city was closed; there was nothing to explore,” Ryan said. “New York was a ghost town.”
Ryan received a lot of support from home.
“Tons of people reached out and were worried about my well-being,” he said, noting the level of concern rose far beyond that of his prior deployments. “My husband and my mom worried much, much more … because I was in a hot spot.”
His colleagues back home, led by Big Rapids emergency department nurse Michele Lehman sent some home cooking – more than 200 pounds of cookies for Ryan to enjoy and share with his new team at Bellevue Hospital.
At the same time, he felt frustration with some friends back home because there weren’t many COVID-19 cases in West Michigan, and the threat of COVID-19 did not feel as real to them as it did to him in New York.
“Emotionally, the hardest part was social media back home,” Ryan said. “It’s crazy. The people didn’t think it was real.”
He tried to convince people of the danger of the virus.
“I fought, and I fought, and I fought with people, then I just decided… you can only do so much,” he said. “People don’t believe it because they didn’t see it. I did see it. I know what it’s like. It’s not fear mongering, it’s the truth.”
He continues to educate folks, but only if he’s asked.
I wear a mask to protect you
“If you ask me, I will tell you,” he said. “But I don’t have the energy or willpower to tell people to make the right decision anymore.”
“People need to remember that social distancing is important, masking is important,” he said. “I don’t wear a mask to protect myself, I wear a mask to protect you.”
Ryan completed his assignment in New York on May 14, and then spent 17 days in quarantine at the Virginia naval base before returning home.
Christopher is happy to have him home safe and appreciates sharing the work again on their farm, named Two Men and a Hen.
They have 11 Nigerian dwarf goats, 27 baby goats, more than 300 chickens, 50 head of cattle and 20 pigs.
“It’s definitely not a hobby,” Ryan joked.
In looking back on his experience in New York City, Ryan believes he and members of the Navy Medical Support Team may have been some of the unsung heroes of the COVID-19 response.
While their efforts didn’t get the national media attention like Navy hospital ships Comfort and Mercy or the Javits Convention Center used as a field hospital, they supported 11 hospitals in the city.
“They were very grateful to have us, the staff, the patients, the community were all receptive to us,” he said. “They really needed us.”















 /a>
/a>
 /a>
/a>
 /a>
/a>
Our entire Big Rapids & Reed City teams are so proud of Ryan and his service in NYC. Thank you Ryan and we’re so glad to have you back home!
Our thanks to Ryan and all those who serve as members of our military and as healthcare professionals. Proud of you, indeed!
Beautiful article Ryan!!! Didn’t realize the extent of your services in NY!! Thank you. ..you are a true hero!♥️
Thank you for your service!!! Proud of you! Thank you for sharing the truth!!
Thank you for your service, Ryan. I’m glad you’re on our Spectrum Health team.
Thank you for being an advocate for the health and safety of our community Ryan!
Thank you for your service, Ryan.
Thank you Ryan. And Christopher
This is a truly wonderful story! Thank you, Ryan, for your service in all arenas.
#WearYourMask #RespectOthers #TakeCover
Ryan, your story truly puts this whole Pandemic into perspective. I don’t personally know you but I experience a sense of pride both for you and your while Navy reserve team. When experiencing people not wearing a mask this is my new standard statement to them: “May we think of freedom, not as the right to do as we please, but as the opportunity to do what is right.” – Rev, Peter Marshall, pastor, US Senate chaplain.
Thank you Ryan for your service and doing what I imagine was a very difficult job with grace. Thank you to your family for sharing you with our country and doing what you can to help and educate people during such a difficult time.
Thank you for your service Ryan! Glad to have you back home.
Thanks for sharing your story Ryan and for stepping up! I also want to give a shout out to Christopher – military spouses are often the unsung heroes.
Thank you for your service, Ryan and Christopher.
Thank you for your service!! I enjoyed learning about your farm. You have your hands full
Thank you Ryan for your service! Our daughter works at a hospital in NYC, and she has described the refrigerated trucks of those who passed due to this illness, and many other devastating stories. We all need to do our part by doing what we can to not spread the virus, and your story will hopefully help people to take it more seriously and not to let up being careful!
Thank you for your service! The situation sounds frightening, so glad you’re home again.
We are all proud of you and your family. Thank you for all of your and Christopher’s sacrifice.
thank you for your service and all you do to help others
What an amazing and touching story. It’s great to hear from the frontlines and see how our military is called into action. I cannot imagine what that was like. Thank you.
Thanks for your service and thanks for sharing your story. Hopefully, true experiences like this will spread and people will be more informed and have a better understanding.
Ryan:
Thank you for your service and sacrifice! You are appreciated more than you will ever know!
Ryan, this is such an amazing story. Thank you for sharing your experience and THANK YOU for your service.
Thank you for your service Ryan. You truly are an unsung hero. So glad you made it home safely.
Thank you for sharing this first hand account – and for serving those in such great need regardless of the risk. I wish we could learn from more stories like yours and your fellow servicemen/women….you are all amazing. I’m sure you made a huge difference in more lives than you know!
Thank you Ryan to you and all that serve in this pandemic. We need you and wearing a mask is not that hard to protect each other. God bless.
Thank you Ryan for your service to our country and others in time of need. Very inspirational story. Appreciate all you have done during this pandemic. Thank you. God bless!