Charlotte Drinkall, 13, always lagged behind on the weight charts.
But being a Highland dancer, performing Scottish routines, and being an overall very active child, her parents, Tanya and Mark Drinkall, didn’t think much of it.
“Her dad is the same way,” Tanya said. “He can eat 5,000 calories a day and not gain weight. We thought she just had an active metabolism.”
In March of 2016, when Charlotte was 10 years old, the family took a road trip to Florida to visit family.
“We get in the car to go and she is like having to pee all the time,” Tanya said. “We thought ‘she just wants to get out of the car.’ We had never done a long road trip before.”
As the miles piled on, the time between Charlotte’s bathroom break requests became more compressed.
“It was the first time in her little life she had been stationary for so long,” Tanya said.
What the family didn’t realize at the time, was Charlotte had entered a danger zone.
“She was slowly going into diabetic ketoacidosis,” Tanya said. “She was headed for a diabetic coma and we didn’t know it. We thought it was car sickness. When I’d look at her in the back seat, I’m like, “I swear she’s losing weight.’ She was getting skinnier and skinnier. What was happening is she was dehydrating.”
When the family arrived at Tanya’s parents house in Bonita Springs, Florida, and Charlotte was able to resume her active lifestyle, symptoms subsided.
Charlotte was running, swimming, playing and eating fruit.
“That probably brought her sugar levels back down. Her sugar levels were building sitting stationary in the car,” Tanya said. “With Grandma and Grandpa, she was running around on the beach.”
Fun family time, for sure. But then the car trip home almost cost one family member her life.
‘Everything clicked’
“She looked like she was near death,” Tanya said. “All of a sudden everything clicked. I asked her to read the sign on the back of the seat in front of her. She said, ‘I can’t. It’s all blurry.’ I’ve been a nurse for 15 years. It all hit. I thought ‘impossible, she can’t have diabetes. We eat a plant-based diet. She’s active. She can’t have diabetes.'”
Tanya told her husband to head to the hospital.
“All of a sudden, Tanya yelled, ‘give her water,'” Mark said. “That’s when we realized she was in a real serious health condition.”
Tanya, who is studying to be a nurse practitioner, said when she made the connection, they were two minutes from a children’s hospital in Chattanooga.
“They drew her blood. Her blood sugar level was so high it didn’t even register. They said she had diabetes.”
The reality of the future didn’t quite sink in for Tanya.
“What’s going through my head is we’re going to have to watch her sugars,” she said. “The whole weight of Type 1 diabetes didn’t hit me. You can eat an apple and you’re screwed. She was minutes away from a coma. Once they hit that coma, it’s hard to get them back out of it.”
Staff took Charlotte immediately to the ICU, where she required close monitoring.
“We knew life would be totally different from now on,” Tanya said. “There’s no doing anything the same anymore. When the doctor told me she was diagnosed with Type 1 diabetes, I remembered from nursing school it’s something that’s not curable. It didn’t occur to me she would need injections every time she eats.”
Heading home for help
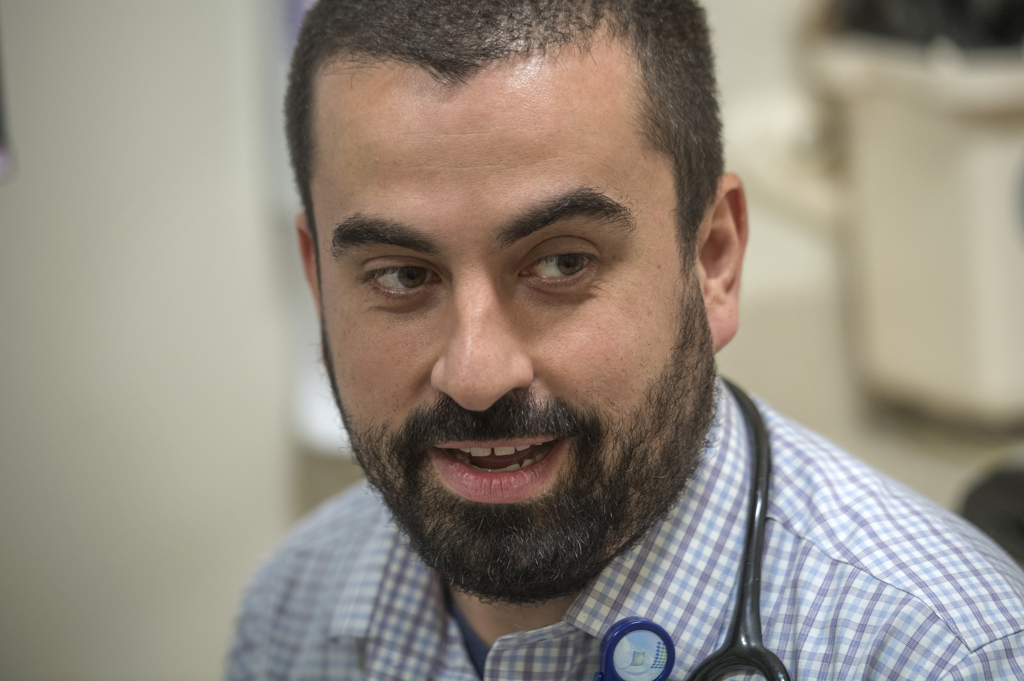
After two days in the ICU, Charlotte spent another week in the hospital before heading home to Petoskey, Michigan. Enroute home, they stopped in Grand Rapids for a scheduled appointment with Jose Jimenez Vega, MD, a pediatric endocrinologist with Spectrum Health Helen DeVos Children’s Hospital.
“The big difference is the doctor in Grand Rapids,” Tanya said. “That’s where everything changed. Everything changed in his office. He asked us how it was going. I said, ‘Her blood sugar is 400, you tell me how it’s going.’ He completely understood. He told us what to do from there.”
After meeting with Dr. Jimenez Vega, they followed up with Amy Martinez, a nurse and certified diabetes educator who works with Dr. Jimenez Vega.
“They want a hemoglobin A1C (average blood sugars over a three-month period) of 7.5 percent or less,” Tanya said. “With all the hard work we do, she has always stayed around 6.”
Tanya said the family has to be ever mindful of the disease, 24 hours a day, 365 days of the year.
“Simply grabbing an apple and reading a book—an apple is 15 carbs and inactivity for two hours is not cool,” Tanya said. “She was starving all the time that first month. Her body got so used to high blood sugar that normal blood sugar felt like she was dying of starvation.”
Charlotte needs an insulin injection before eating.
“That’s eight or nine shots a day, every day,” Tanya said. “There are foods she can eat that she doesn’t need insulin for. Fat. She can do cheese and meat and not get a shot. But if you’re filling up on cheese and meat, imagine what that does for your cholesterol levels. People with diabetes are prone to high cholesterol levels. Charlotte is quite the trouper.”
Helping others as a way to help herself
Charlotte decided to take action and try to help other adolescents with Type 1 diabetes—so she started a blog.
Her first entry? Her account of the day of her diagnosis.
“She’s got around 600 followers,” Tanya said. “One day, she was having a really hard day. She was eating salad and cheese and her blood sugar was like 200. …She started making up her own memes and posting them on social media.”
She heard back from a reader who wrote: “I am sitting in the hospital. I was just diagnosed yesterday and I’m just sitting on my bed laughing at your memes with my mom.”
Here’s an excerpt from Charlotte’s blog, which can be found at type1diabetes.blog:
Well, March 3rd or 4th, 2016, we found out that my pancreas died. My body killed it. I no longer have the organ that eats the sugar in my body. Crazy, right? So let’s go back.
I don’t remember much about diagnosis because a lot of my memory was wiped. But I do remember this: March 3rd, technically the 4th, because it was past midnight, was the day I was diagnosed with Type 1 Diabetes. We were on a trip to see some family about 13 hours away. Did you know that, when you are diagnosed with T1D, (Type 1 Diabetes) you usually have ketones. So your body needs to flush them out. Let’s stop right there.
You get T1D because your pancreas no longer makes insulin. Insulin eats the sugar in your body. So if you eat literally anything, your pancreas, an organ, will release this ‘insulin’ to use the sugar. If your body uses sugar, you don’t get many ketones.
So you can’t have a lot of ketones in your body. That’s not good. Too many ketones can kill you. So now at this point of the story, I have many ketones in my body because my pancreas is now dead. My body is flushing them out. I know what you’re thinking, “Flushing, like flushing the toilet? Haha!” Yes, like flushing the toilet. I did that about every 5 minutes. Now remember, this is a 13ish hour trip. Every 5 minutes stopping to go flush my ketones. Yeah. Now it’s like a 38 hour trip. But, whenever you pee, you get thirsty. I was really thirsty. Worst. Family. Vacation. EVER.
Tanya said she’s proud of her daughter for wanting to give back.
“At first you think it’s a terrible thing,” she said. “How can I survive? She’s learning how to help others survive.”
‘She’s the life of every party’
The exposure has helped Charlotte leave her shell.
Charlotte said many young people recently diagnosed with Type 1 diabetes reach out to her after reading her Instagram page or blog.
“They’re stressing out,” Charlotte said. “They go on Instagram and find my page and reach out.”
Charlotte also attends a diabetes camp every summer, with about 500 fellow campers.
“There’s a lot of kids with it,” she said.
Tanya said Charlotte, who entered eighth grade this year, isn’t letting anything hold her back.
“She’s the life of every party,” Tanya said. “She never was before. She was always the kid that clung to my leg. We homeschooled her entire life. This year she’s going to school. She’s like Miss Popularity. She’s very funny. People really just love her.”
Dr. Jimenez Vega said about 1.25 million Americans live with Type 1 diabetes, including 200,000 younger than 20 years old.
“In our center, we see more than 1,500 patients ages 2 to 18 with Type 1 diabetes,” Dr. Jimenez Vega said. “Last year, 200 patients with new onset Type 1 diabetes were diagnosed or referred to our center.”
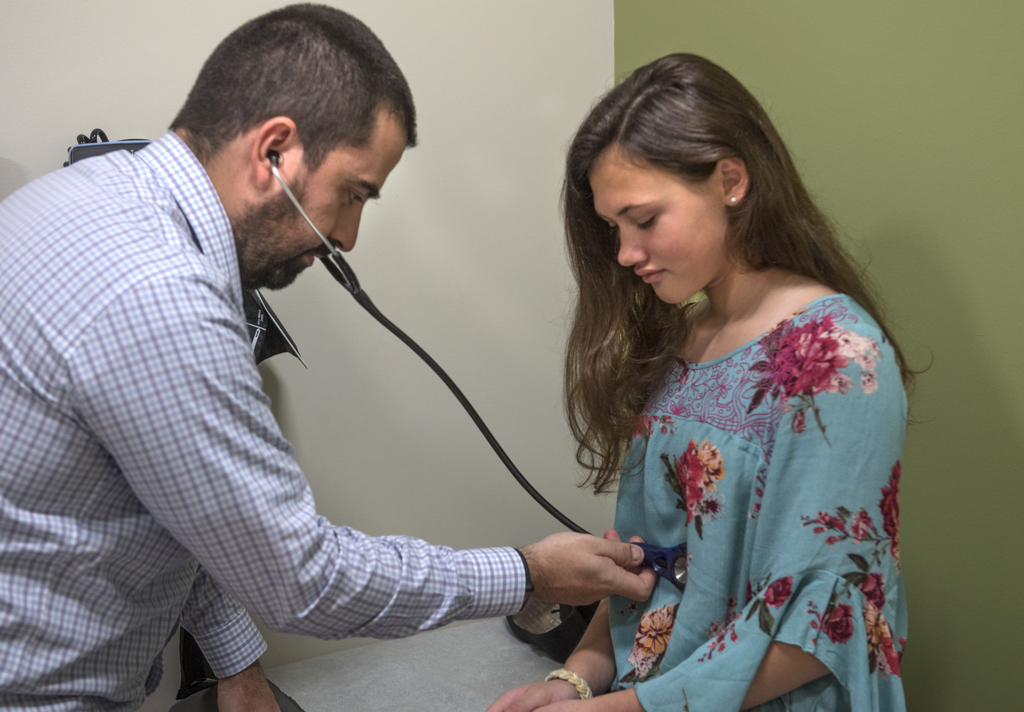
In early October, the family drove down from Petoskey for a three-month checkup with Dr. Jimenez Vega.
They laughed and joked with the doctor, and rejoiced about her good results.
Charlotte said she’s learning to live with the disease. She is using an insulin pump, which delivers small amounts of insulin per hour, as well as allows her to give insulin for her meals and snacks without having to give herself a shot every time. She also uses a continuous glucose monitor, a device that can check her sugar levels every five minutes and give her a trend of where her sugar levels will be heading.
“It’s more normal than it was when I was first diagnosed,” she said. “It’s the simple things, like when someone would hand me an apple, I would need a shot. Now, I check my pump and punch in a couple of numbers. It is more normal with the pump. The pump has made things easier.”
Through this technology, Mark and Tanya can monitor Charlotte’s blood sugar levels while she is at school.
“If she has a math test, we know what class she’s in depending on her blood sugar,” said Mark. “If you’re stressed, your blood sugar goes up. If you’re exercising, it goes down. Most people don’t realize your whole life is affected. You never have a day off unless there’s a miracle healing.”
Dr. Jimenez Vega checked the computer monitor and reviewed the insulin pump and and monitor information for the past two weeks. He said he’s impressed with the way the family is helping Charlotte successfully handle the disease.
“She is doing really well,” he said. “They have been able to deal with this in a jovial, fun way with a sarcastic sense of humor. In the context of a really scary life-threatening situation, they try to laugh.”
Dr. Jimenez Vega said he’s pleased with Charlotte’s perseverance.
“She is a very smart adolescent who continues to learn and understand what diabetes is and what it entails,” he said. “Even with the stress of a life-threatening disease like Type 1 diabetes, the need for 24/7 monitoring and the trials and tribulations of adolescence and high school, Charlotte uses social media and blogs as a way to vent and show the good and not so good things about Type 1 diabetes.”




















 /a>
/a>
 /a>
/a>
 /a>
/a>
You go, girl! What a horrific discovery. Now you (along with your parents) are adjusting to a new life. Keep smiling. Keep joking. Keep living.
Great story. My son, Brooken, is 15. He was diagnosed at the age of 7. It has been a journey. He controls his sugars very well. He has taken command of the disease and does not let it control him. Good luck to you young lady. We will be in your corner.
I must say, not only are you an inspiration to many young people out there that are new to having type 1 diabetes but you are also an inspiration to people who don’t have it. I commend you for taking your disease and turning it into something good. You have definitely touched my life and im greatful to you for that. Thank you for sharing your story with the world, and with me. I believe you will grow up to be a great advocate for finding a cure for diabetes. May the Great Spirit always watch over you and protect you from this day forward. ( Written by a Native American elder who lost many loved ones to diabetes as it is a very common disease to the Native American people.)