Nothing could have prepared Heather David, 28, for the highs and lows she’s faced over the past five years.
The emotional roller-coaster began in the summer of 2017, when she and her husband, Zack, unexpectedly lost a child to stillbirth at 35 weeks gestation.
The couple, from North Muskegon, Michigan, hadn’t fully processed their grief and trauma when Heather became pregnant again in early 2018.
Because of her previous loss, likely linked to a clotting disorder she has, Heather’s local OB-GYN referred her to the Spectrum Health Maternal Fetal Medicine team, which manages high-risk pregnancies.
“We’re here to guide patients through,” said Lisa Thiel, DO, a maternal fetal medicine specialist. “We are on the same team with them … and we very much value our relationships with our patients.”
Ovarian tumor
Things progressed smoothly for Heather until 18 weeks into her new pregnancy, when she noticed something didn’t feel right. The maternal fetal medicine team brought her in for an ultrasound.
The scan showed something alarming: a 10-centimeter ovarian mass on her right side.
Ultrasound images from six weeks earlier had shown no sign of the mass. And by the time Heather had an MRI a week later, the fast-growing tumor—which turned out to be a rare, aggressive form of ovarian cancer—had already moved out of her pelvis and into her abdomen.
The 18-week ultrasound had come at just the right time.
“Ovarian masses grow quickly. If the mass had developed before or after pregnancy, we may not have had the same outcome,” Dr. Thiel said.
“The pregnancy itself helped us to identify the change on the ovary. So the timing and the pregnancy, in my mind, saved her life.”
Suspecting cancer from the start, the maternal fetal medicine team introduced Heather to the team members in gynecologic oncology at the Spectrum Health Lemmen-Holton Cancer Pavilion.
Confident they could remove the mass without harming the developing fetus, doctors performed surgery on Heather in August 2018, removing her right ovary along with the tumor.
The pathology showed a type of small cell carcinoma of the ovary, a rare cancer that carries a high risk of recurrence. Even for those diagnosed in the early stages, as Heather was, long-term survival rates are only 33%.
Treatment would involve an intense chemotherapy regimen—six chemo drugs administered over the course of three days, delivered in six cycles over four months.
“It’s a really tough protocol,” said Leigh Seamon, DO, a gynecologic oncologist. “The general consensus was the regimen would be too toxic to give during pregnancy.”
The couple and their collaborative medical team from maternal fetal medicine and gynecologic oncology faced a wrenching set of decisions about the risks to Heather versus the risks to their baby in utero. How long could she safely wait to deliver before receiving chemotherapy?
“I think fight-or-flight mode initiated right away,” Heather said. “Just like, ‘How can we save myself? How can we save this baby?’”
Together they decided to schedule a cesarean section delivery at 28 weeks—far enough along in the pregnancy to promise the baby a strong future, while hopefully soon enough to keep the cancer from regaining a foothold.
Delivery and treatment
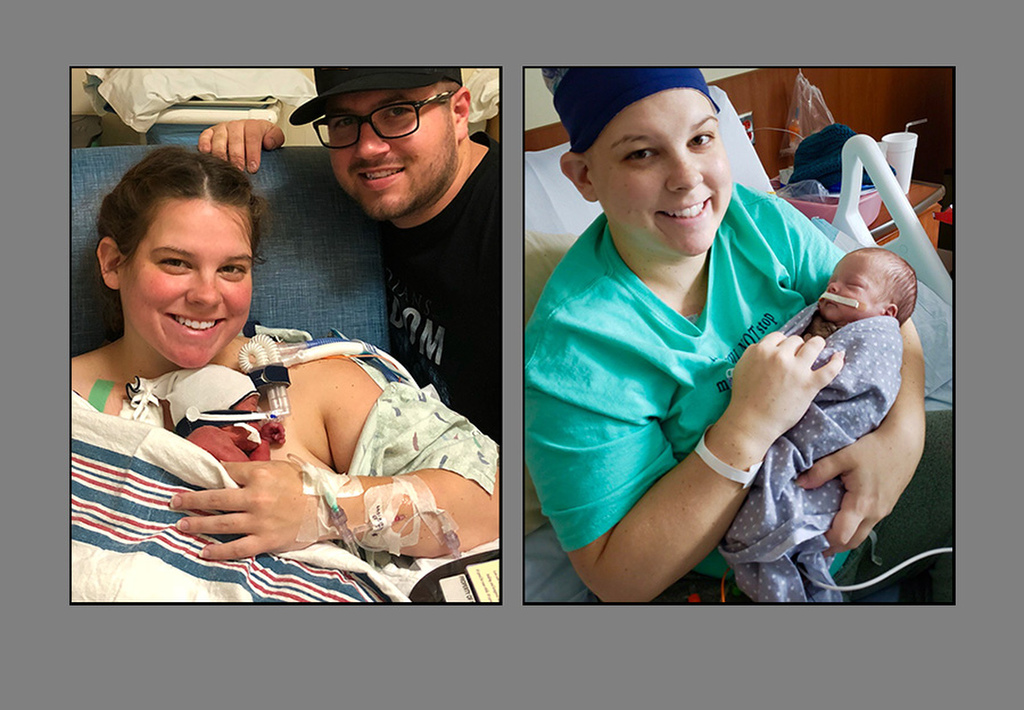
On Oct. 3, 2018, Heather gave birth to Axel, a small but healthy baby who went on to receive 55 days of care in the Gerber Foundation Neonatal Center at Helen DeVos Children’s Hospital.
“We lost our first son, and his due date was Oct. 3—and then we ended up having Axel, the miracle baby, on Oct. 3 of the following year,” Heather said. “So (life) just works in weird ways.”
Following her C-section and abdominal exploration—which thankfully showed no evidence of cancer spread—Heather began her chemo treatments.
As a patient at Spectrum Health Butterworth Hospital, she took every opportunity she could to be with her newborn in the NICU.
“I did treatment at Butterworth as an inpatient for the start of it, so I actually got to be wheeled back and forth to him during treatment,” she said.
“That kind of worked out in my favor and kept me going during the really hard days.”
On the worst days, she experienced a sharp decline in lung function. Her oncologists eliminated the medication they suspected to be the cause, and she underwent pulmonary therapy to regain the lost function.
As her treatments progressed, Heather turned to a life-giving practice: gratitude.
“I started waking up every day and naming three things I was grateful for,” she said. “Some of my days were so dark that one of those grateful things may be that I could step out of bed that morning.”
Heather turned a hopeful corner in February 2019, when her chemo ended. That’s when she and Zack could focus on life as new parents in the aftermath of cancer.
“We just kind of went on to learn a new normal of living life after chemo and trying to hope for remission,” she said. “I was in survival mode.”
Surprise pregnancy
Heather had always known she’d wanted more children.
But with everything her body had endured, doctors weren’t certain whether she could have another pregnancy—and, with her uncertain prognosis, whether they’d even recommend trying.
“It was unknown whether or not she was going to regain ovarian function,” Dr. Seamon said. “Usually that (chemotherapy) regimen does put patients into menopause.”
But despite the odds, Heather did get pregnant again, in late 2020.
The maternal fetal medicine team kept an extra close eye on her throughout this third pregnancy, and she sailed through it without major issues.
“We joke that it was so normal it felt wrong,” Heather said.
Baby Walker made his appearance in June 2021, nearly three years after his big brother.
Today both boys are healthy and growing well, their parents’ two biggest gifts.
Three-year mark
February 2022 marked three years post treatment for Heather, and she remains cancer free.
“Each scan is a landmark. The further out you get, the less likely it is to come back,” Dr. Seamon said. “So we’re feeling really good about it right now. We’re doing what I call ‘ride the wave,’ which is, hey, everything’s looking good, cancer hasn’t returned, we’re watching it very closely.
“I’m hesitant to say that she’s cured … but certainly the highest risk of recurrence is within the first two to three years.”
Drs. Seamon and Thiel both use the words “bravery” and “inspiration” when they reflect on Heather’s journey.
“She was just such a light to everybody else around her. She just kept fighting for her baby and her family, and always was just really positive about her health,” Dr. Thiel said.
“How she’s overcome so much is really, really important, and her joy is really obvious.”
Heather credits the maternal fetal medicine and gynecologic oncology teams with her family’s very existence.
“I would trust them with my life, and I tell anybody that,” she said. “I wouldn’t have my two miracle babies without them.”
She also treasures the support of her husband, who’s been at her side for the past 12 years.
“He was doing double duty for a NICU preemie baby and a sick wife with cancer,” she said.
“Treatment is hard. Babies are hard. But he survived both, and we ended up stronger than ever, so I’m just blessed to have a life partner who never gave in.”
Her friends in the Mona Shores High School community, where she works as a cheer coach, provided an additional source of encouragement.
“They rallied and supported me through the entire thing. They allowed me to coach that entire season on chemo,” she said. They also held a fundraiser for her.
“Having your tribe of people, whether that be one or two people or (an) entire community, if you choose to share your journey—it makes a big difference.”
Heather still shakes her head when she tries to comprehend everything she and Zack have lived through since 2017.
“When I sit back and talk about it sometimes, I’m like, ‘Wow, that really all just happened to us,’” she said.
“We have our very hard days, but we just think back on what we’ve been through and that we’re blessed to have them.”








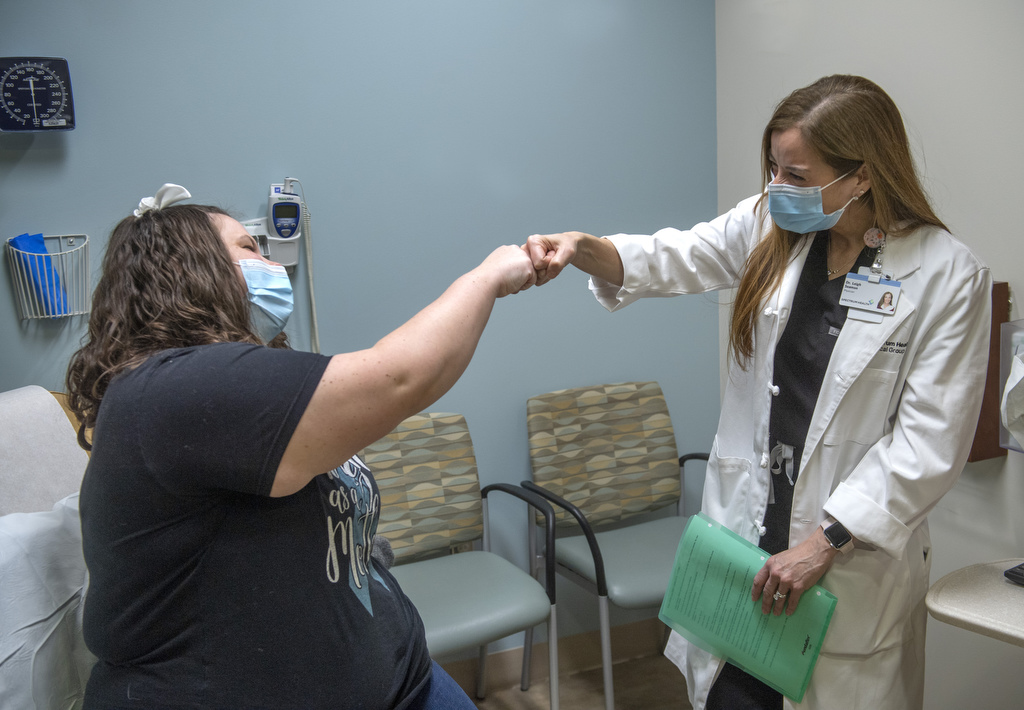














 /a>
/a>
 /a>
/a>
 /a>
/a>
Heather and Zacks story should be shared far and wide. They are a true testiment of love conquering all. Such inspiration and love for life shows us that what we survive makes us stronger and creates a beautiful everlasting bond. This beautiful story gives hope to so many now facing seemingly insurmountable challenges. Thanks for telling Heather and Zacks story in such a beautiful and complete way. I hope this will be published in multiple venues so as many as possible get to share their incredible journey.
Heather is my sister Dianna Supernaw’s granddaughter, and as such there’s little doubt that she inherited the resolve to fight for every breath God has allowed her from her grandmother. Her mother Debbie Norwood has had her own medical struggles ever since I can remember and it has always been her mother, Dianna who was there beside her, supporting her, and reassuring her that she’ll make it through each and every hardship she has faced. Debbie, and Heather have been through a lot, and their fight to live another day, especially in Heather’s case is nothing short of remarkable. Zach was clearly the foundation that afforded Heather hope and together the journey they’ve been on has certainly been a joint effort, but also an effort notwithstanding scores of outside support from family, friends, well wishers, and her cheer team. All those prayers motivated Heather to show the world that she’s not a quitter, another trait inherited from her grandmother Dianna. The story is heartwarming, Hallmark noteworthy, and should be an inspiration to all who are struggling with the many twists and turns of life’s folly. God Bless the David, Norwood, and Supernaw family’s and May Axle and his little brother inherit their mother’s strength to survive and personality and determination to succeed.
Your story is a true inspiration for all and shows that how true love helps to face the innumerable challenges thrown upon by life. Thanks for sharing.