A garden grows outside Mary Howell’s front door that blooms from spring to fall, filled with peonies, boomerang lilacs, hydrangeas, wisteria, tiger lilies and lavender.
Keeping the many plants weeded, trimmed and healthy became much easier this year after she received a new left hip joint.
“As soon as I could get in my garden after the surgery, I went out in it,” said Howell, a 74-year-old retired cook who lives in Jenison, Michigan.
Her quick rebound from hip replacement surgery surprised and delighted her. But the therapists who helped her with rehab say she deserves much credit for her recovery.
“She was very motivated,” said Sarah Behrens, PT, a physical therapist who worked with Howell after her operation at Spectrum Health Blodgett Hospital. “It could not have gone any smoother.”
Howell’s experience also shows the value of good preparation for hip replacements, her medical team says.
An increased focus on preparing the patient for the operation has boosted success rates and recovery time in recent years.
At Blodgett, where surgeons perform more than 1,000 hip replacements a year, patients take a class a few weeks before their operation. In the two-hour session, they learn what to expect from the operation.
“We talk a ton about the prevention of complications,” said Lisa McCann-Spry, MSN, who oversees the joint replacement education program. “How do you prevent an infection? How do you prevent a blood clot?”
The class includes practical tips for preparing patients’ homes so they can manage basic tasks and avoid injury in those first days after surgery. Rearranging furniture, removing rugs, placing food on easy-to-reach shelves can improve safety at home. Patients are advised to check out the height of the bed and toilet to see if they need to make adjustments.
Our research has shown with early mobility, there are better outcomes.
McCann-Spry strongly encourages patients to have a helper for the first 48 hours at home. Most people can use a little help with light housework, fixing meals, keeping track of paperwork, remembering when to take their pills and do exercises.
“So many people say, ‘I don’t want to bother my kids,’” she said. “But this is really the time to call on a friend or family member to be your go-to person.”
The class also includes simple exercises patients can do before surgery.
“Your muscles react so much better if they are primed and ready for what they are going to go through,” said Chris Laughhun, a physical therapy assistant who helps teach the class. “I tell them, ‘If you are already doing something―walking, riding bikes, swimming or yoga―continue doing what you are doing.’”
Hip-replacement preparation also includes improving the health of the patient, said Peter Jebson, MD, department chief of orthopedics for Spectrum Health Medical Group.
Surgeons often require patients to lose weight, stop smoking, improve control of diabetes and reduce narcotic use before undergoing the elective surgery. “Pre-surgery optimization” of a patient’s health improves the likelihood of a successful experience, Dr. Jebson said.
“This very purposeful, navigated care prior to surgery, including the joint education classes, has been shown to lower the risk of complications and improve patient satisfaction,” he said.
Scheduling the surgery
Howell said she experienced hip pain and went through therapy for six or seven years before consulting an orthopedist about a hip replacement.
“I had trouble walking,” she said. “I waddled.”
When she moved the wrong way, a jolt of pain stabbed her hips. She remembers one incident when she turned while talking to her granddaughter last fall.
“I let out a yell and I was in instant sobs,” she said. “It was horrible.”
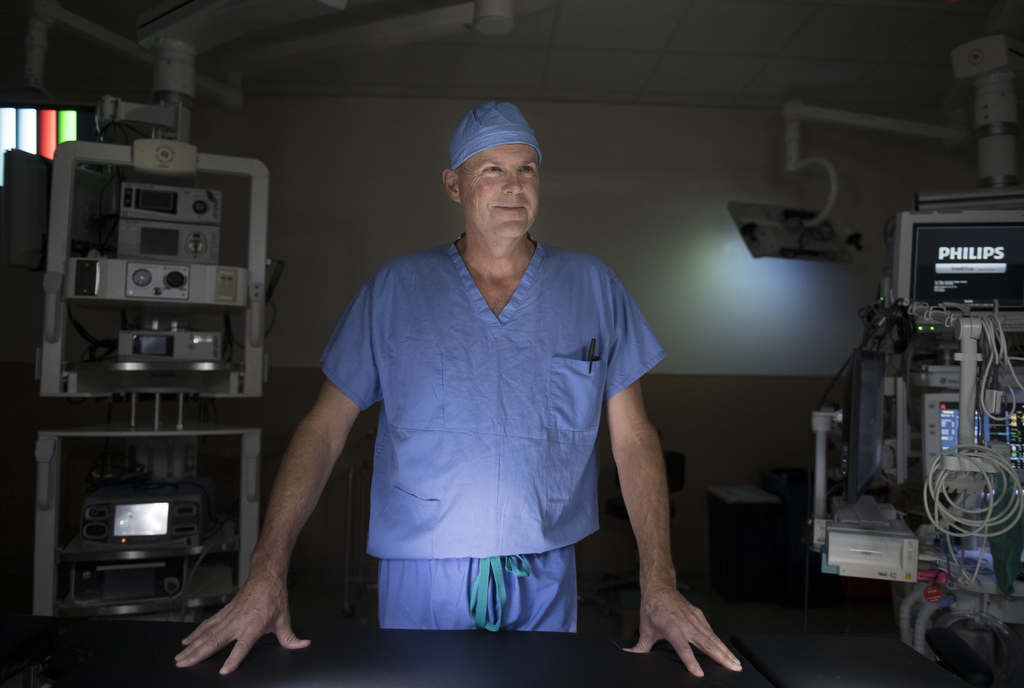
She met with orthopedic surgeon Robert DeMaagd, MD, and scheduled an anterior hip replacement surgery for Aug. 14, 2017―and attended the pre-operation class at Blodgett a couple of weeks before.
The class helps with emotional as well as physical readiness for surgery, Dr. DeMaagd said. For many patients, joint replacement surgery is their first operation—or the first time they spend a night in the hospital.
“A lot of it has to do with expectations. If they aren’t surprised by things, they are more relaxed and things don’t upset them as much,” he said. “That decreases their anxiety about the upcoming surgery.”
On their feet
A few hours after Howell’s operation, Behrens helped her get out of bed for a 75-foot walk down the hall.
“We do short-distance ambulation with a walker that first session,” Behrens said. “Our research has shown with early mobility, there are better outcomes.”
The next morning, an occupational therapist took Howell to a therapy room to see if she could get in and out of a bathtub.
“I got in and out of that tub like it was nothing,” Howell said.
Laughhun helped her walk back to her room with a walker. She managed to go 315 feet without any problems.
“The gait pattern was perfect. Her balance was almost ridiculous to the point where she could probably walk with a cane,” Laughhun said. “It is our job to be motivators and encouragers―and she took it with gusto beyond gusto.”
The quick approach to rehab for hip replacement patients represents a big change. Just five years ago, patients typically stayed three to five days after surgery.
“Five years ago, we didn’t work with patients on the day of surgery,” Behrens said. “And on that next day, they had nerve blocks that caused their knee to buckle.
Now most patients, like Howell, are up walking within hours of surgery. Most go home the next day.
“It’s a dramatic change,” Behrens said. “Therapy has been working with the physicians and care managers to optimize the patient experience and make it more efficient.”
Ready for the second one
Howell now has plans to replace her right hip joint in April. With six children, 13 grandchildren and six great grandchildren, she wants to stay active.
Her positive experience is common for patients who replace painful, poorly working hip joints, research shows.
Hip replacement patients “are my happiest patients,” Dr. DeMaagd said. “They usually go from so bad to so good in a very short period of time.”
“In terms of quality of life, total joint replacement outcome is second only to cardiac bypass,” Dr. Jebson said. “It is a massively impactful surgery in terms of improving patients’ quality of life.”




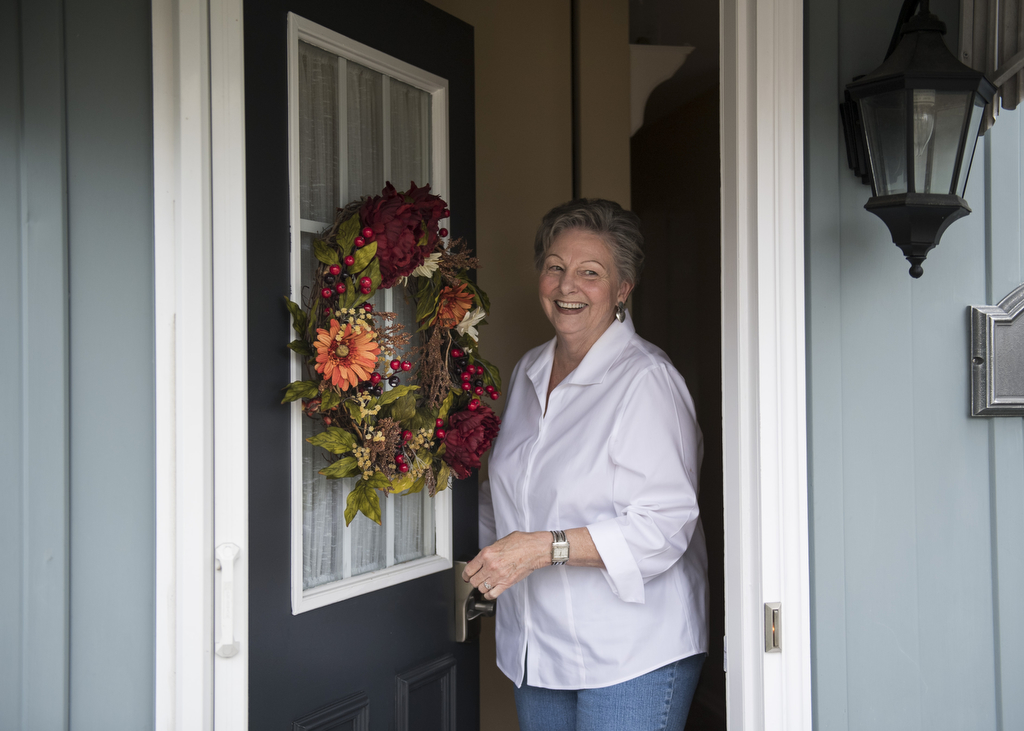




 /a>
/a>
 /a>
/a>
 /a>
/a>
It was very helpful since I’ve a sister ready to get surgery so I share w/her this article since she lives in Colombia SA
Terrific. So glad this article could be helpful to you and your sister, Clara. Best wishes to you both.