John Watson’s struggles began in summer 2014, when a rare and fast-moving skin infection almost killed him.
He underwent multiple surgeries.
With each, doctors cautioned him that he’d likely deal with permanent chronic pain.
Those warnings didn’t alarm Watson, 63, or his wife, Jen, during that harrowing period.
“It was such a traumatic, scary time,” Jen said. “So when we heard them say, ‘John, you are going to have a lot of pain, but you’re going to live,’ we didn’t think much about what they meant by pain.
“We were just so happy he was able to pull through.”
As months of recovery wore on, including skin graft surgeries, he faced the discouraging transition to chronic pain.
The intensity was unrelenting, radiating from his lower back, down his left leg, and up into his abdomen.
Medications offered some help. Sometimes he received nerve-block injections, which provided blissful but short-lived relief.
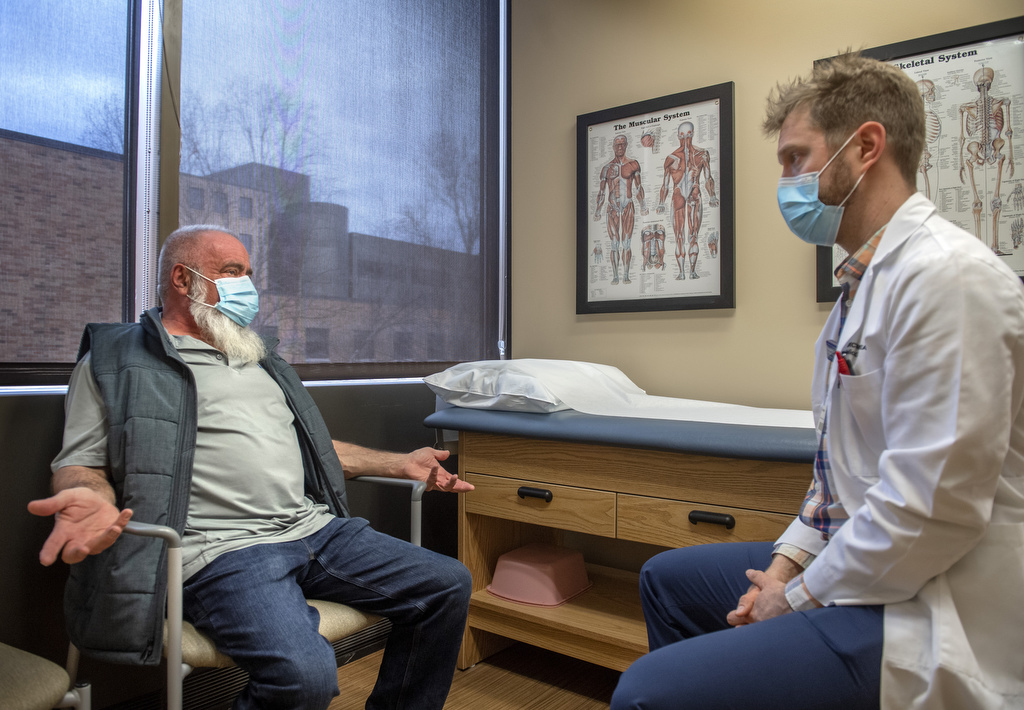
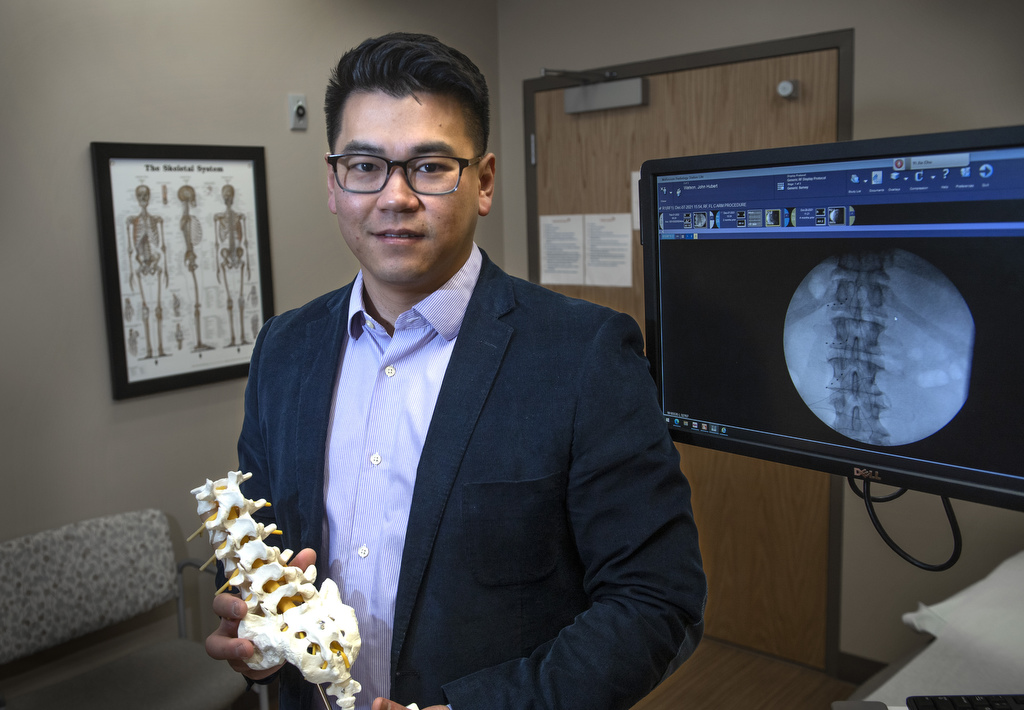
Then, in 2021, he met with Yi Jia Chu, MD, who specializes in interventional spine and chronic pain management at the Spectrum Health Spine and Pain Management Program.
Dr. Chu has had great success implanting a dorsal root ganglion stimulation device in patients battling chronic pain.
The device isn’t for everyone, Dr. Chu said.
But it can be life-changing for patients like Watson, who lives with a type of pain known as complex regional pain syndrome. An estimated 200,000 people are affected by this syndrome each year in the U.S.
Traffic signals
Dorsal root ganglia are structures along the spinal column that are made up of densely populated sensory nerves.
The nerves act kind of like traffic lights, “running interference for and regulating the signals and sensations that travel through nerve fibers,” Dr. Chu said.
After an injury, the light turns green and lets pain signals through.
“That’s good,” Dr. Chu said. “We want to know when we’re injured.”
In most cases, healing begins and the light turns back to yellow, then red.
But in the case of some extreme trauma, like Watson’s, that doesn’t happen.
“It’s as if the traffic signals stay green all the time, allowing all the pain signals to get through, even when there is no longer a painful stimulus occurring,” Dr. Chu said. “These cells misbehave, even though the trauma is now gone.”
The pain then persists, becoming so intense it causes the skin to discolor, creating swelling and temperature changes under the skin. It can even affect the growth of hair and nails.
“In these cases, people can be debilitated,” he said. “Sometimes their limb or extremity becomes completely nonfunctional.”
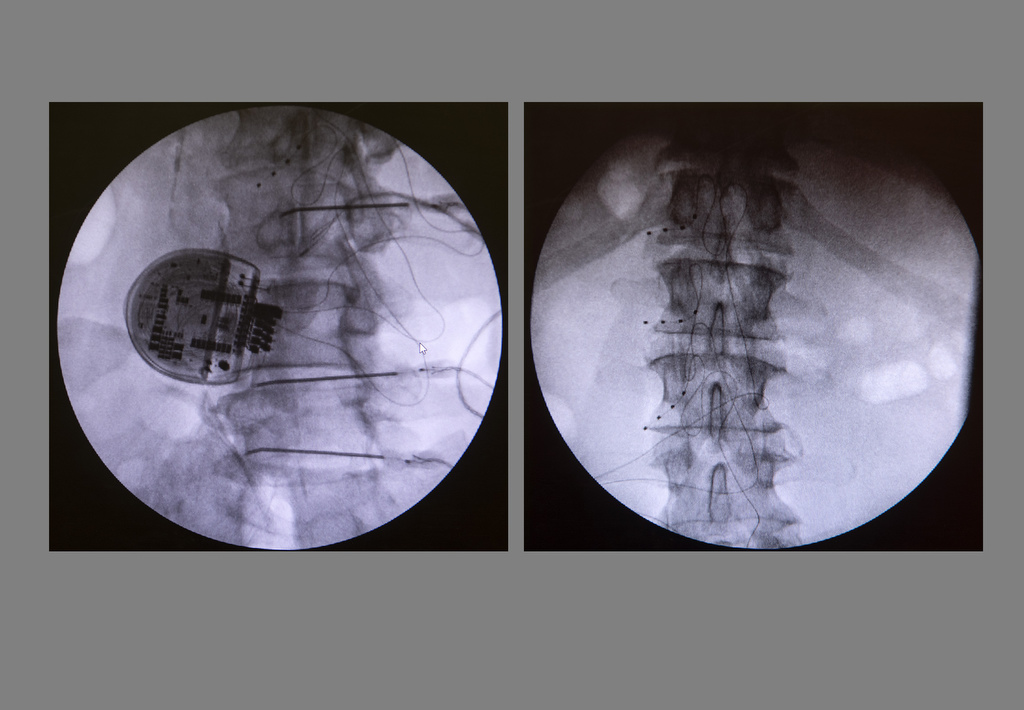
The dorsal root ganglion stimulation device, approved by the FDA in 2016, is similar to a spinal cord stimulator. It disrupts that flawed signal system, sending low doses of electrical impulses directly to the dorsal root ganglia.
The device is a bit like “a pacemaker for the spinal cord,” Dr. Chu said. “It causes the root ganglia to fire at appropriate physiologic levels, rather than in that hyper-excitable pain state.”
Finding relief
The first step involves a trial run.
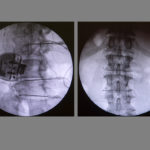
In this procedure, the electrical leads are inserted along the spinal column using a needle, positioning them near the painful places. In Watson’s case, that meant the lower lumbar spine.
But rather than surgically implanting the generator and battery, an external device is used. It’s practically invisible under clothing and it operates with no external cables.
Patients control the tiny generator using an app-based, wireless system connected to an Apple device.
That seven-day period gives patients a chance to see how their body reacts to neuromodulation. They can decide if and how much it helps to improve function and reduce pain.
“I tell patients, ‘It’s my job to convince you to at least do the trial, because I believe you are a good candidate.’ But it’s their job to convince me afterward if they want to go ahead with the implant,” Dr. Chu said.
The treatment is not for everybody.
“It is a risk-benefit analysis every patient has to make on their own,” he said.
Watson experienced some discomfort with the test period, which Dr. Chu said is not typical. But he also felt enough pain relief that he decided to go ahead with the surgical implantation.
Dr. Chu inserted the leads and battery at about the waistband level. The batteries typically need to be changed every six years or so.
Just a few months after surgery, Watson could resume some work at his small agricultural business in Wayland, Michigan. He can sit still again, staying in a pew for a full church service, or on the couch to watch an entire movie with his family.
The list of pain medications he requires keeps shrinking.
And he can’t stop feeling grateful for the vast relief from this tiny device.
“Dr. Chu told me that if the procedure cut my pain levels by 50%, we’d be able to cut back on my pain medications and the procedure would be considered 100% successful,” Watson said.
So far, results have exceeded those expectations.
“It’s reduced my pain by about 98%,” Watson said. “Most of the time, I am almost 100% free from pain.”
After years of pain that hovered around seven on a 10-point scale, his pain is now consistently between zero and one.
“I consider myself a poster child for this technology,” he said.
Watson said he felt relief almost immediately.
There are short-term limitations while the incisions heal, such as not lifting anything heavier than 5 pounds.
His family noticed dramatic improvements, too.
“You can see how much better he is just in the way he moves,” Jen said.
John is delighted to get back to his old self. He’s back to helping more, caring for his 96-year-old mother, who lives with him and his family.
He has an 18-year-old son, and they have a family dog.
Dr. Chu is thrilled to offer a modern solution to an old problem.
“Doctors have described this kind of complex regional pain syndrome as long ago as the Civil War,” he said.
“It’s so debilitating.”
Living with that level of chronic pain means many have to take pain medication, which can present problems.
“And it often leads to anxiety and depression, as people struggle with a diminished quality of life,” he said. With the dorsal root ganglion stimulation device, “patients are finally getting significant long-term benefit.”


















 /a>
/a>
 /a>
/a>
 /a>
/a>
Amazing story! Never even heard of this therapy. More people need to know about it.