To Randy Remenap, 77, diabetes always seemed like the unavoidable family legacy.
For much of his life, the Grandville, Michigan, resident and retired high school principal watched his mother, who’d been a nurse, struggle with weight problems and diabetes.
Many of his family members struggled with the disease.
“It was one day about 15 years ago that my mom was checking her own blood sugar when she just randomly said, ‘Let me check yours,'” Remenap said. “It was too high, so I went to see my doctor. But it kept getting worse.”
Doctors eventually diagnosed him with Type 2 diabetes.
Like many of his relatives, he struggled to get ahold of the disease.
“My numbers got worse and I was gaining weight,” he said. “I wanted help with food cravings and I wanted to learn how to control these swings in my numbers.”
He reached out to his primary care physician, James Samuelson, MD, an internal medicine and family medicine specialist with Spectrum Health.
Dr. Samuelson knows Remenap’s struggles well—he’s been caring for him for years.
“By September 2018, Randy weighed 228 and he wanted to lose weight,” Dr. Samuelson said. “His sugars at that point weren’t that bad, but he felt he could do better.”
Dr. Samuelson connected him with diabetes educator and dietitian Michelle Telemaque, RD, CDE, a member of the Spectrum Health Diabetes and Endocrinology team.
Coming together
Early on, Telemaque met with Remenap about once a month and Dr. Samuelson would see him every six months.
“We worked together to help Randy,” Telemaque said. “I felt free to make suggestions to Dr. Samuelson and he shared information with me.”
She reviewed Remenap’s medications: Metforim, Trulicity, and Lantus, a long-acting form of insulin.
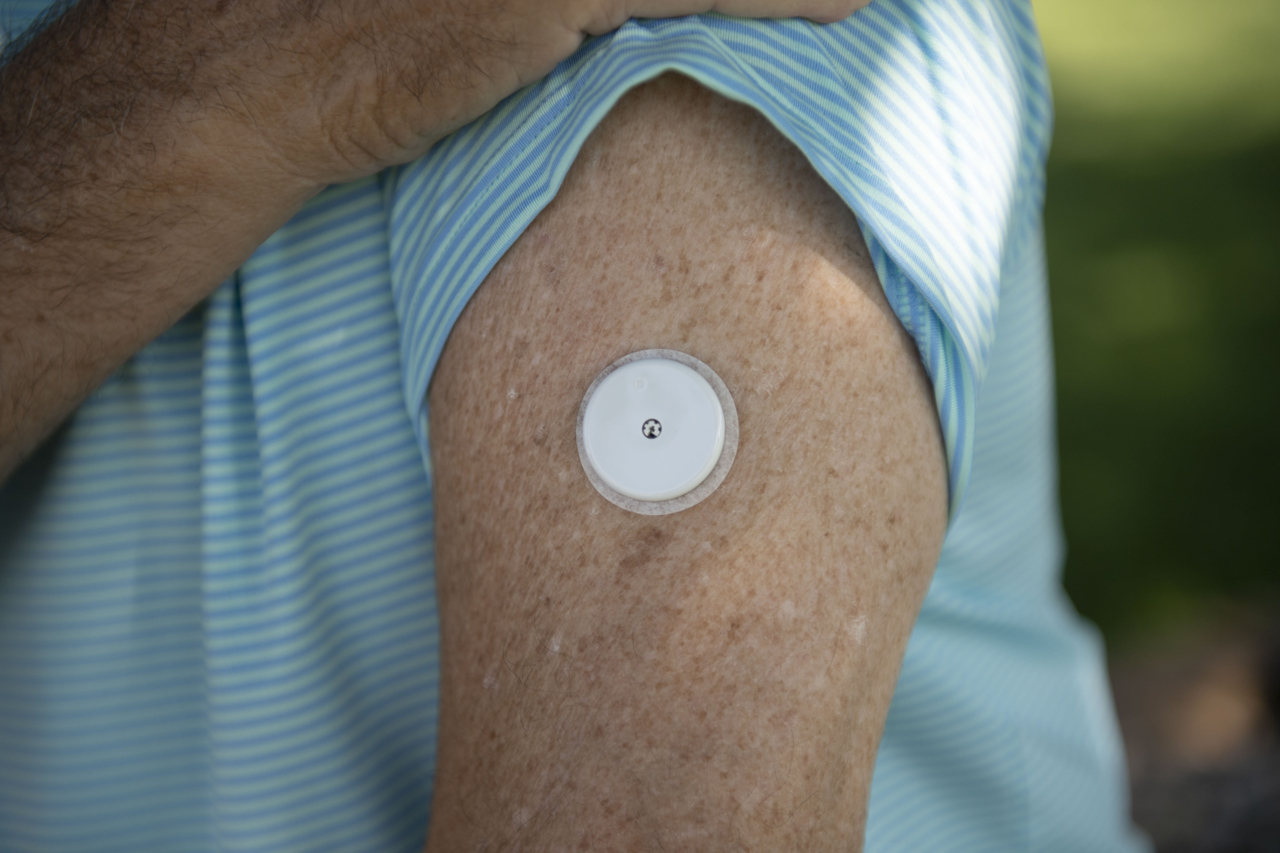
Remenap also started using a device called FreeStyle Libre, a sensor that scans for blood sugar. It replaces the need for a needle prick.
“I checked his doses of Trulicity because Randy had food cravings he wanted to control, something that is common for those with diabetes,” Telemaque said. “I asked Dr. Samuelson to consider increasing dosages.”
Dr. Samuelson agreed.
It helped a little.
“But Randy was still very hungry in the evenings,” Telemaque said. “We switched him to Ozempic and that made a big difference in the cravings.”
Remenap then lost 5 pounds.
“Michelle was unbelievable,” Remenap said. “And the way she and my doctor worked together. They literally surrounded me with the help I needed. I always had the choice to accept or disregard their suggestions.”
He began to absorb new knowledge.
He learned about nutrition and how to eat right. How to control his blood sugar. How to make better decisions about what to eat and when.
When his diabetes got particularly bad, he often found himself craving sugar, sweets and cookies.
He learned, with a sigh, that those bad dessert choices simply aren’t worth the trouble.
“Michelle showed me the research on what that did to my body, so that I could make better decisions,” he said. “Now I choose berries or fruits instead of cookies. And I eat the fruit with a meal and not by itself, so that my blood sugar wouldn’t spike high.”
Turning to tech
The new gadget, FreeStyle Libre, proved invaluable.
Rather than constantly pricking his finger to get a read, Remenap could simply use a device to scan a sensor the size of a quarter, attached to his skin.
“I could instantly know where my blood sugars are, how my body was responding to the food I just ate,” Remenap said. “That thing tells me everything. Every diabetic should have one.”
The downside: “It’s not cheap and insurance doesn’t always cover it,” he said.
Telemaque and Dr. Samuelson used the data from the Libre to adjust Remenap’s medication.
Even as his body still produced some of its own insulin, the proper medication in the right dosages could help his body respond more effectively.
“And so Randy finally was able to lose 5 pounds,” Telemaque smiled. “He was ecstatic at each pound lost. As he continues to lose weight, he will need less insulin—and weight loss then becomes even easier.”
His diabetes could eventually go into remission, she said.
“It takes a motivated person to make these kinds of changes,” Dr. Samuelson said. “And Randy is that. It’s a bit unique to work like this, as a team, and he’s part of this team—the physician, the dietitian, the patient.
“Each team member offers a different perspective,” he said. “And it all comes together to give the patient the best possible care.”
When they learned Remenap had obstructive sleep apnea, they also brought a sleep doctor onto the team. This led to a C-PAP machine at night, which can also affect insulin usage.
What does this all add up to? Randy’s game plan.
“That’s what we call it,” Telemaque said. “We don’t work in a silo, but as a team. And Randy benefits.”
Remenap smiled wide.
He has lost yet another 5 pounds. And he can’t wait to let his teammates know.




 /a>
/a>
 /a>
/a>
 /a>
/a>