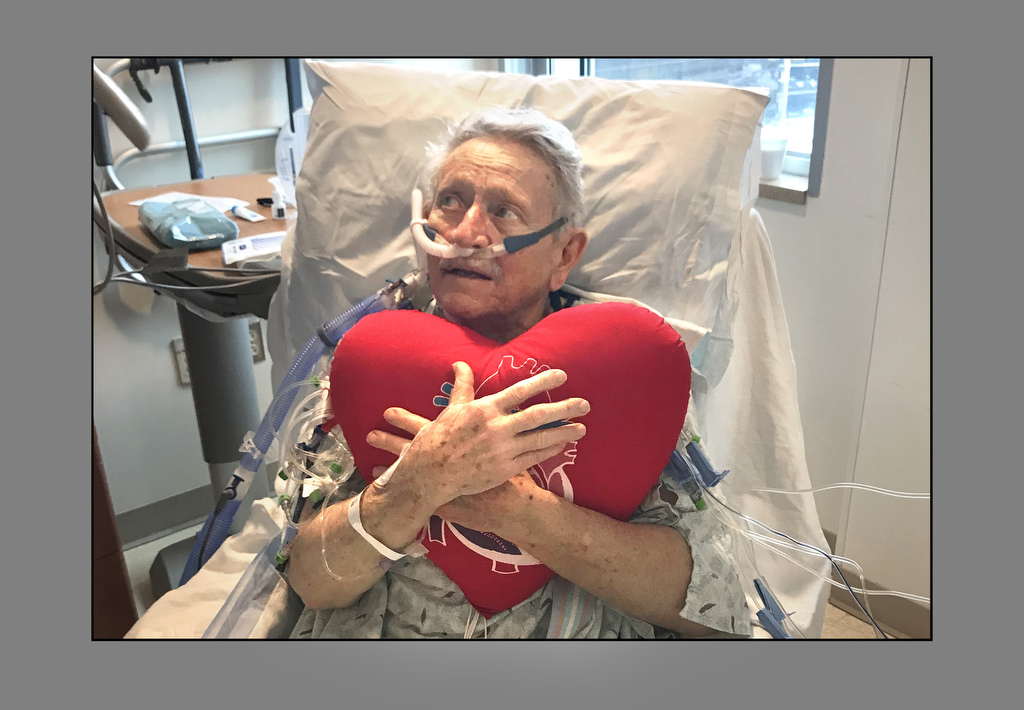
At first, Glen Greta figured it was just a pulled muscle.
He and a friend had just finished loading a trailer chock-full of parts for an antique military vehicle, packed in 100-pound boxes.
It was late December 2017.
Greta had just cleared snow off the deck of his cottage overlooking Big Blue Lake, about 20 miles north of Muskegon.
“After I put the shovel away, I felt this strange sensation of something inside my chest, pushing out,” he said. “I’d read about heart attacks, so I knew that this was a different pain. I figured I’d strained something, so I decided to sleep on it.”
The next day, his chest still hurt.
He called Spectrum Health Integrated Care Campus at North Muskegon and they asked him to come in. He arrived soon and underwent testing.
An electrocardiogram confirmed something was seriously wrong. He wasn’t having a heart attack, but he would need to see a cardiologist as quickly as possible.
Greta went directly to Spectrum Health Butterworth Hospital in Grand Rapids, where the team in the emergency department stood ready and waiting.
They started additional testing to determine the cause of his intense pain.
‘Got to be ready’
A CT scan showed Greta had suffered a hematoma in his ascending aorta, the arch-like portion of the body’s biggest and most vital artery.
By 9 p.m., the surgical team rolled him into the operating room.
Even after doctors briefed him on the procedure, Greta couldn’t quite acknowledge the enormity of the surgery.
“As I was going in, I told Penny, my wife, ‘I’ll see you on the other side,'” he said. “I meant I’d see her when I came out of the operation. She thought I meant on the other side of life. I didn’t realize I’d put her into frantic panic.”
Greta had no idea the extent of his trouble.
Acute aortic syndrome kills an estimated 10,000 people each year, according to the American Heart Association.
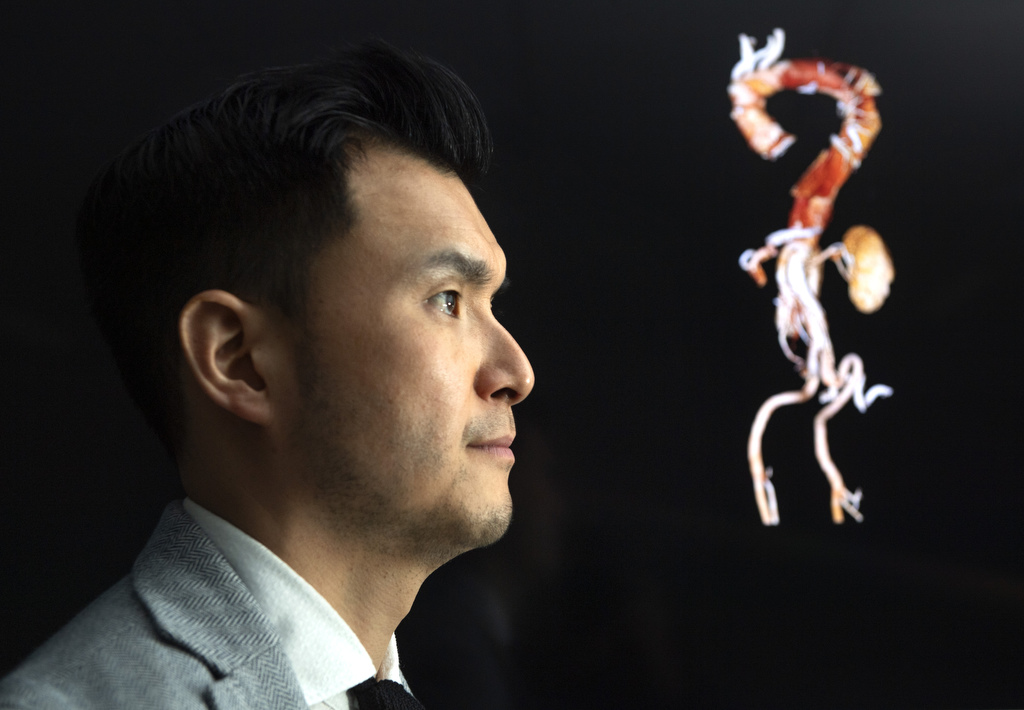
“I usually describe cases like Glen’s as the one true cardiac emergency,” said Stephane Leung, MD, a cardiothoracic surgeon specializing in acute ascending aortic disease. “When it’s not being fixed, it has a mortality rate of about 1% to 2% per hour.”
Greta’s age, then 76, presented an additional risk.
Dr. Leung set about repairing 6 inches of damaged tissue using a graft.
It’s an incredibly intricate and time-consuming surgery.
The aorta, shaped like a candy cane and about a foot long and 1 inch wide with multiple layers, is the largest artery in the body, delivering oxygen-rich blood to the brain and muscles.
Dr. Leung had to cool Greta’s body to about 64 degrees Fahrenheit, protecting his brain from damage.
The aortic repair took about three hours, Dr. Leung said.
But the night was far from finished.
While operating, Dr. Leung quickly determined that in addition to the bulging weak spot in his aorta, Greta also had significant coronary disease and blockages, some of which obstructed as much as 98% of the blood vessels.
“His heart was weak,” Dr. Leung said. “And he needed a triple bypass.”
Bypass surgery is one of the most common procedures in the U.S., but Greta’s case presented additional challenges.
“Because Glen came in as an emergency case, we didn’t know his history,” Dr. Leung said. “We didn’t have a good workup. It’s very much like a box of chocolates, because you never know what you’re going to get.”
Dr. Leung prepared for the work ahead.
“We’ve got to be ready to do anything and everything, from an aortic root repair to replacing the entire arch,” Dr. Leung said.
For the bypass surgery, he used a vein from Greta’s leg. Greta’s heart also wouldn’t resume beating on its own, so Dr. Leung and his team worked to restore his heartbeat.
From the start of the surgery to the moment his heart began pumping again, Greta had spent 10 hours in the operating room.
Staying alert
A retired engineer and lifelong fix-it guy, Greta continues to marvel at the fix-it nature of the surgery that saved his life.
“I asked Dr. Leung why he didn’t just give up,” he said. “Here he is called in at 9 p.m. for emergency surgery, with operations that go on for 10 hours. Why keep going?”
He remembers Dr. Leung’s matter-of-fact answer—it made a lasting impression on him.
“He told me, ‘I never give up. I always have a Plan A and a Plan B. And I think we were down to about Plan E with you.'”
Greta spent the next two days in acute care. He stayed in the hospital 42 days as his care team worked to tame the atrial fibrillation that caused his rapid and irregular heartbeat.
At one point, his heartbeat skyrocketed to 222 beats per minute.
“It set off alarms and people came rushing into the room,” he said.
Then, even as his health improved and he returned home, progress came incrementally.
“I was supposed to start walking, but I could only manage 25 steps at a time,” he said.
He had trouble remembering things, too.
“The most basic things, like how many square inches are in a square foot,” he said.
Psychologically, that period was very difficult. “I don’t know what I would have done without the emotional support I got from Penny, as well as the care team in the cardiology department,” he said.
Greta later returned to the hospital, where the team determined he had no blockages and his heart worked fine mechanically. But he required cardioversion, a procedure that returns the heart to a normal rhythm.
Additional tests revealed significant sleep apnea, associated with a higher risk of cardiac illness.
He now has a pacemaker, which helps control his irregular heartbeat.
“I’m finally beginning to get back to some semblance of normality,” Greta said.
The mental journey, not just the physical recovery, continues to present challenges. This includes acknowledging that some body parts wear out, even with the best of maintenance.
‘Go straight to the hospital’
Greta sees plenty of analogies between the moving parts in his chest and those in the 300 antique military vehicles he’s owned throughout his life.
“Here I was, 76 at the time, enjoying what I consider to be a great life,” he said. “I was able to be very robust in everything I did. I could lift my weight. Heck, I could still even fit in my Vietnam Army uniform.”
These days, he shouldn’t lift more than 50 pounds.
A former runner, he has to content himself with walks around his Grand Rapids condo, the Blue Lake cabin and his elaborate shop.
“It’s taken its toll,” he said. “My brain still thinks I’m 40, but then my body says, ‘Yeah, you’re 80.'”
He remains intensely grateful to his surgical team.
“If it hadn’t been for Spectrum Health and Dr. Leung and his staff, I wouldn’t be here,” he said.
Greta hopes others can learn from his experience.
Dr. Leung, too, urges people to stay alert to symptoms.
“People usually describe it as the worst chest pain they’ve ever had—a tearing, ripping pain,” Dr. Leung said. “It often radiates to the back. And it’s the kind of pain most people just can’t ignore.”
It can even cause a person to lose consciousness. If you see this happen to someone near you, call 911 and head to the nearest emergency room.
Greta’s advice?
“Don’t wait,” he said. “Call right away. I wish I had realized this was an emergency. I’d tell someone else to go straight to the hospital.”
















 /a>
/a>
 /a>
/a>
 /a>
/a>
Thank you so much for your perseverance! Glenn’s wife, Penny, is my cousin! So glad he’s still here!
What a great article. Possibly can save a life.