Christopher Cranson sees the scar on his chest daily.
But the 14-year-old Grand Rapids City High School student has no recollection of the worry, pain and medical miracle behind it.
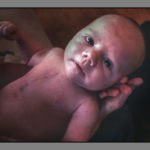
When Christopher entered the world at 4:30 p.m. Oct. 9, 2003, weighing 9 pounds, 6 ounces, all seemed well to his parents, Jeff and Beth Cranson.
“He was big and seemed healthy,” Beth said. “Everything seemed normal.”
Medical staff ran routine tests on baby Christopher.
“They did a test on his foot to determine the level of oxygen in his blood,” Beth said. “The oxygen level was low, but he seemed so big and healthy they thought the machine wasn’t working. They got another machine and determined his oxygen level was still too low.”
The machines were working properly. Unfortunately, Christopher’s heart wasn’t.
“They whisked him away,” Beth recalled. “They knew something was wrong. A couple of hours later, Samuel Lacina, MD, a pediatric cardiologist, showed up and told us he had a congenital heart defect.”
Hard words to hear. This is the same fetal heartbeat Jeff and Beth had listened to in the womb all those months. The same heart they loved unconditionally, before ever having met the baby that contained it. And the heart they hoped would love them in return.
Dr. Lacina recognized the symptoms—large birth weight, blue-tinged skin signifying not enough oxygen—as transposition of the great arteries, which in layperson’s terms, means his heart arteries were the opposite of where they should be.
“Dr. Lacina was on call that evening and diagnosed him immediately, then patiently sat with Jeff and me and drew pictures to help us understand the problem and how it could be repaired,” Beth said.
Beth and Jeff, both long-time journalists, so wished they could edit the words, strike “defect” from the diagnosis. And “fear” too. But, those initial moments proved to be only the beginning of a story seemingly writing itself, the ultimate story of a strong, vibrant and athletic son.
At eight days old, Christopher underwent open heart surgery to transpose his heart arteries. And he’s lived a solid story line since.
‘That scar will always remind me of it’
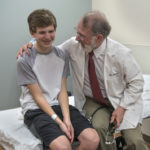
“It’s crazy thinking about what I went through when I was that young,” Christopher said while awaiting a stress test at Helen DeVos Children’s Hospital Congenital Heart Center on a recent weekday. “That scar will always remind me of it.”
Christopher, an avid athlete, loves tennis, baseball and skiing. He’s been advised to stay away from sports that entail a lot of weight lifting, which can cause undue stress on the heart.
As an athlete who likes to push the limits, Christopher recently underwent his first stress test as a precaution, to test his heart function.
Congenital Heart Center technician and exercise specialist Laura Zochowski explained to Christopher that it’s a “maximum effort test,” that he should go as long as he possibly can. Most patients tire and stop in 10 to 12 minutes, she said.
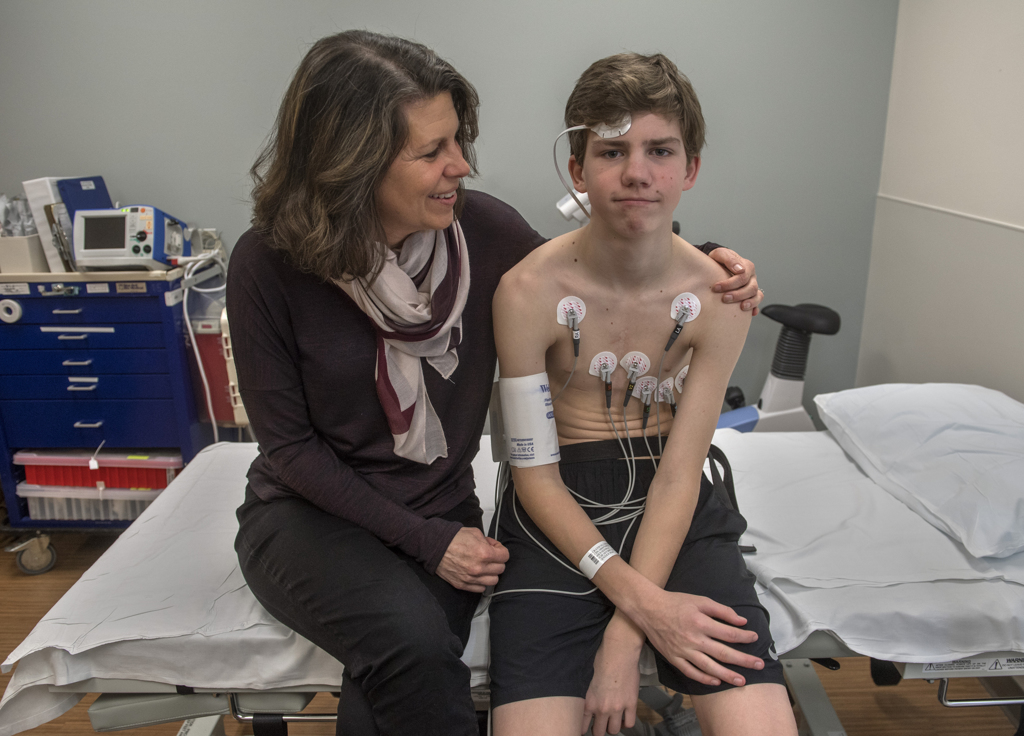
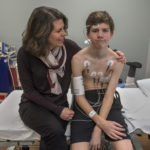
She placed electrode stickers on his chest, checked his sitting and standing blood pressures, then conducted a breathing test.
“A lot of people think this is harder than the actual treadmill,” Zochowski said. “Now, deep breath in and blow. Keep going, keep going, keep going.”
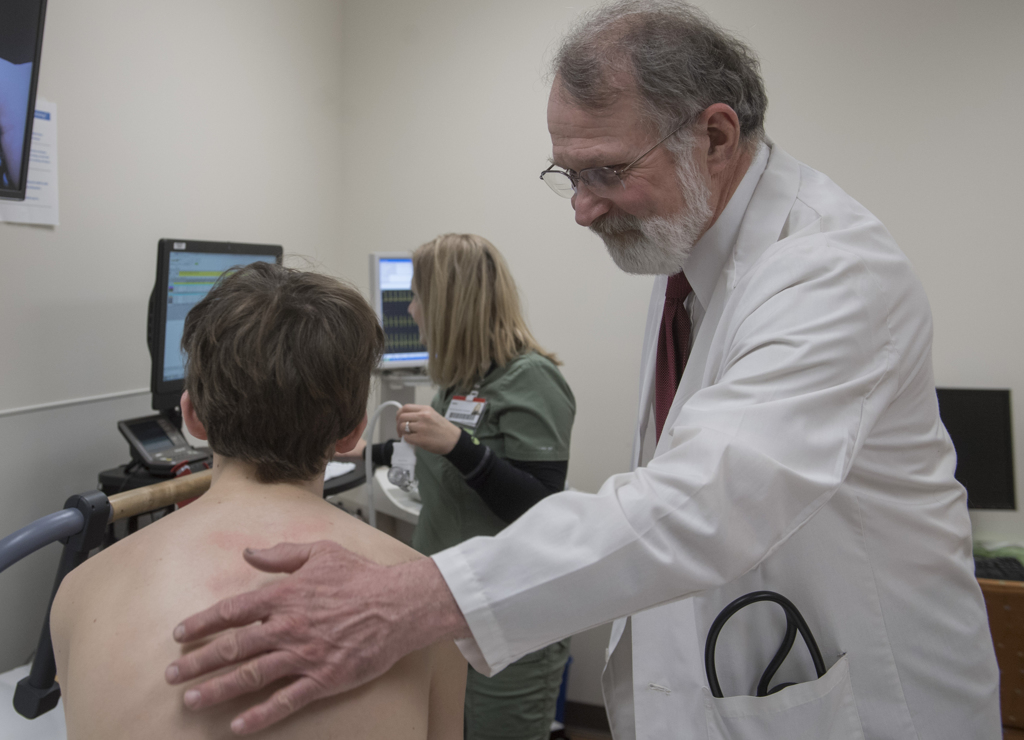
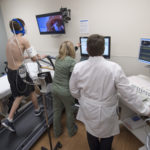
Following the breathing tests, she placed oxygen sensors on his forehead and a breathing mask over his face. Stanley Sedore, MD, pediatric cardiologist, came into the room to help monitor the treadmill test.
“It’s just like gym class,” Dr. Sedore told Christopher. “You watch the Olympics? It’s the same testing that all the Olympic athletes get.”
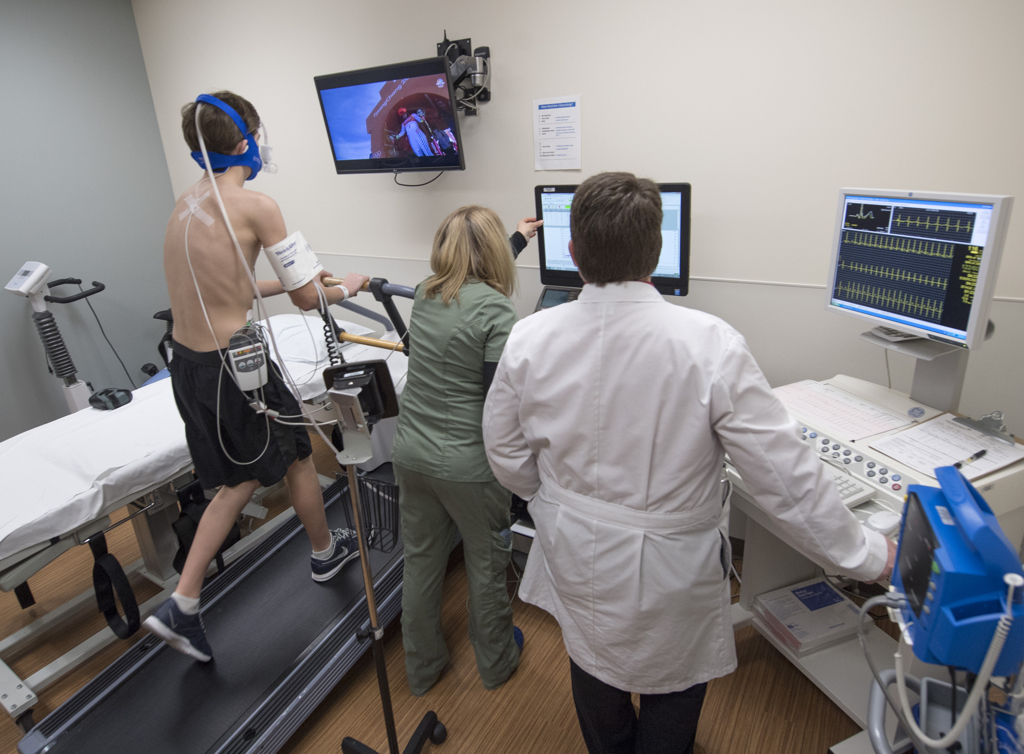
Zochowski fired up the treadmill and Christopher began to walk, slowly at first, but the speed, and simulated incline continued to increase.
“Everything is great, everything looks really good, you’re doing a great job,” Zochowski told him.
Christopher continued walking, then eventually, slow jogging.
He lasted more than 14 minutes on the treadmill.
“We didn’t see any arythymias or anything,” Dr. Sedore said. “We don’t have many kids who don’t have congenital heart disease who can do what you just did.”
Dr. Sedore said congenital heart disease affects 0.8 percent of children born in the United States.
Of children presenting with “blue baby syndrome” like Christopher did, transposition of the great arteries is the most common cause.
These days, most cases are picked up while the baby is still in utero.
“Some babies need a procedure immediately after birth to get blood flowing back to the lungs correctly,” Dr. Sedore said. Christopher was one of those babies, too.
Continuing care
Although technology and pediatric cardiology services have evolved much since Christopher was born 14 years ago, Beth said she’s grateful for the continuity of care.
Dr. Lacina has followed Christopher since birth. And even though Dr. Lacina is retiring May 2, Christopher will still be seen by his co-workers in pediatric cardiology at the congenital heart center.
He’ll eventually transition to the adult congenital heart program in the same space.
“If (Christopher) stays in Michigan, he could be in the same office for years and years,” Beth said. “These specialized doctors could treat him throughout most of his lifetime. I think that’s cool for the sake of research and for consistency. Hopefully what they learn will help other kids, too.”
Doctors perform an electrocardiogram on Christopher every two years to check his heart, valve and vessel functions.
Despite his current heart health, Beth said Christopher’s long-term prognosis is a mystery, and will probably remain that way.
“There’s nobody out there in their 60s, 70s or 80s who has this condition because, back then, they would have died at birth,” Beth said. “We just don’t know.”
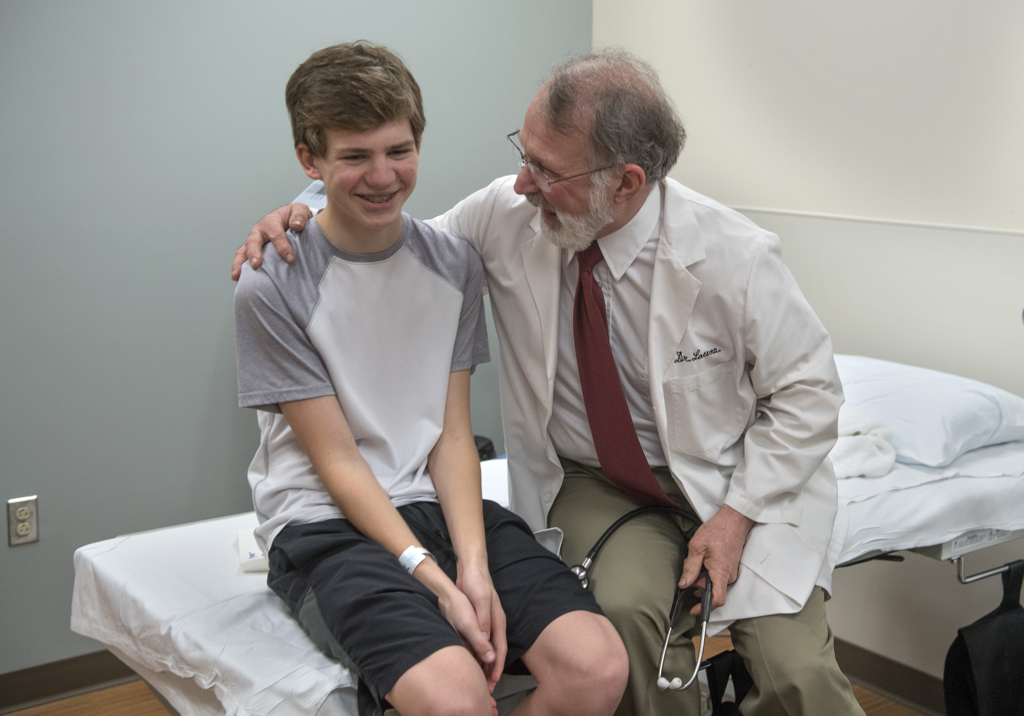
Dr. Lacina entered the room.
“Hi, friend,” he said to Christopher.
Dr. Lacina glanced at the monitors, and smiled at what he saw.
“You don’t go 14 minutes without having really good heart function,” Dr. Lacina said. “He is doing phenomenal.”
Dr. Lacina anticipates that trend will continue, but there is no way of knowing for sure. He said continuity of care with pediatric and adult congenital heart specialists working together is a benefit for both patients and providers.
“I’m so grateful we now have the adult congenital people who have joined our group,” Dr. Lacina said. “In 1968 the first surgeries were done for this condition. We no longer do that original surgery. We started Christopher’s type of surgery in the mid-1980s, so our oldest patients haven’t hit their 40s or 50s. We’re walking together with our patients and they’re teaching us.”
Dr. Lacinia is learning much, including not to underestimate his patients’ abilities and endurance.
“They’ve expanded what we thought was possible,” he said. “We’re being so cautious, but our patients want to do more, like, ‘Let me have a full life.’ We’re walking to the edge with them and these kids are saying, ‘I’m ready to go.’”














 /a>
/a>
 /a>
/a>
 /a>
/a>
Dr Lacina is a wonderful pediatric cardiologist. He can smell congenital heart disease a mile away. He is always very kind and very in tune to all his patients. He has served this community for 39 plus years and has been an excellent asset to congenital heart disease. His wisdom and expertise will be surely missed.
Dr. Lacina is the best. He has seen all three of my children and walked us through some scary times. We are so thankful that we have such amazing doctors in GR and wish him all the best in retirement.
Thank you, Rebecca, for your kind comment. Best wishes to you all. 🙂
There are not enough words to describe Dr. Lacina. November of 1997 my son was diagnosed with Transposition of the Great Vessels and Dr Lacina was part of the team that took care of my son!! Without the passion and genuine care from Dr Lacina I have watched my son drive for the first time, make it to States for high school bowling, graduate high school and work a full time since graduating. So Dr Lacina Thank You for letting me create memories with my heart child!!! Happy Retirement
Thank you for sharing your story and good wishes, Sheila. Your message gladdens our hearts. We are so happy your son is doing so well. Best wishes now and always.