Fall of 2010. Lou Coleman, now 71, sat in the bleachers at the Broncos football game on the Western Michigan University campus in Kalamazoo.
His wife, Helen, sat by his side.
Life seemed good for this parts manager and longtime football fan.
Good—until Coleman looked down at his hands in his lap. He could see a slight tremor in his left hand. He tried to still it but could not.
“I went to see a neurologist in Kalamazoo,” Coleman said. “At first, he didn’t think it was Parkinson’s disease. He thought maybe it was an issue with a blockage in a vein in my neck.”
It wasn’t the vein.
He remembers the moment his doctor delivered the diagnosis: Parkinson’s.
“I was devastated,” he said. “But he said, it’s not the end of the world.”
Parkinson’s disease is a progressive nervous system disorder that affects movement, often beginning with a slight tremor in one hand and progressing to stiffness and a slowing of movement.
Patients will notice a rigidity in their limbs, a slower gait and lack of balance. They’ll also experience more difficulty with speech and writing.
“When Lou was first diagnosed, we were both in shock,” Helen said. “We both went through a depression.”
Hope—lost and regained
Around that same time, their daughter Mary went on to earn her PhD in neuropsychology.
“She was influenced by what happened to me,” Coleman said. “She encouraged me back then to fight this thing.”
Coleman shook off the depression and began his fight in earnest.
He joined an exercise group specifically for patients battling Parkinson’s. There, he gained support from other members.
“I tried new meds and, for the last three years of my career, I went to part-time,” he said.
He retired in 2014.
“It wasn’t so much about a tremor anymore,” Coleman said. “I was getting stiffer and slower.”
Helen noticed her husband’s strides had grown shorter as he walked.
“He would shuffle with his hands in his pockets or at his sides, so that people wouldn’t see the shaking,” she said. “And his speech got much quieter. He would get upset when he thought I wasn’t listening to him, but I just couldn’t hear what he was saying.”
As Coleman became increasingly frustrated with his worsening symptoms, his neurologist recommended he check out Spectrum Health.
“Our daughter Mary had learned about DBS—deep brain stimulation—and she pushed me to look into it,” Coleman said. “She got me information about it and encouraged me to go to Spectrum Health.”
On the fast track
In January 2021, Coleman followed the advice from his daughter and his neurologist.
He made an appointment with Ashok Sriram, MD, a Spectrum Health neurologist and movement disorders specialist.
“By this time, Lou was experiencing motor fluctuations,” Dr. Sriram said. “His medication took a half hour or more to kick in and it stopped working about an hour before he could take another dose, so he was losing one and a half hours.
“He had dyskinesia—involuntary and dance-like movements—when his dosage was increased, it was a side effect of the medication.”
Coleman’s gait had worsened, at moments freezing him in place so that he would get stuck mid-motion for moments at a time.
Doctors scheduled him for a two-day fast-track evaluation.
“The fast-track process is a unique system to determine if someone is a good candidate for deep brain stimulation surgery,” Spectrum Health neurosurgeon Rushna Ali, MD, said. “The patient meets with seven specialists over two days.”
This multidisciplinary team includes a neurologist, movement disorders neurosurgeon, neuropsychologist, psychiatrist, physical therapist, occupational therapist and speech therapist.”
They tested Coleman with and without medication, Dr. Ali said.
They deemed him a strong candidate for a device the FDA recently approved—the Medtronic SenSight Directional Lead System.
The big day
Doctors scheduled surgery for July 2, 2021.
“SenSight is different in that it can send stimulation currents to a very specific area in the brain,” Dr. Sriram said.
Previous deep brain stimulation had been “more circular, less specific and could cause side effects,” he said.
Spectrum Health is one of the first in the nation to use this technology, he said.
“Sensing technology not only stimulates areas of the brain, but also picks up brain activity through the leads wires,” Dr. Sriram said. “That allows us to pick up local field potentials, or signature patterns, in the patient and can be correlated with certain symptoms of Parkinson’s disease.”
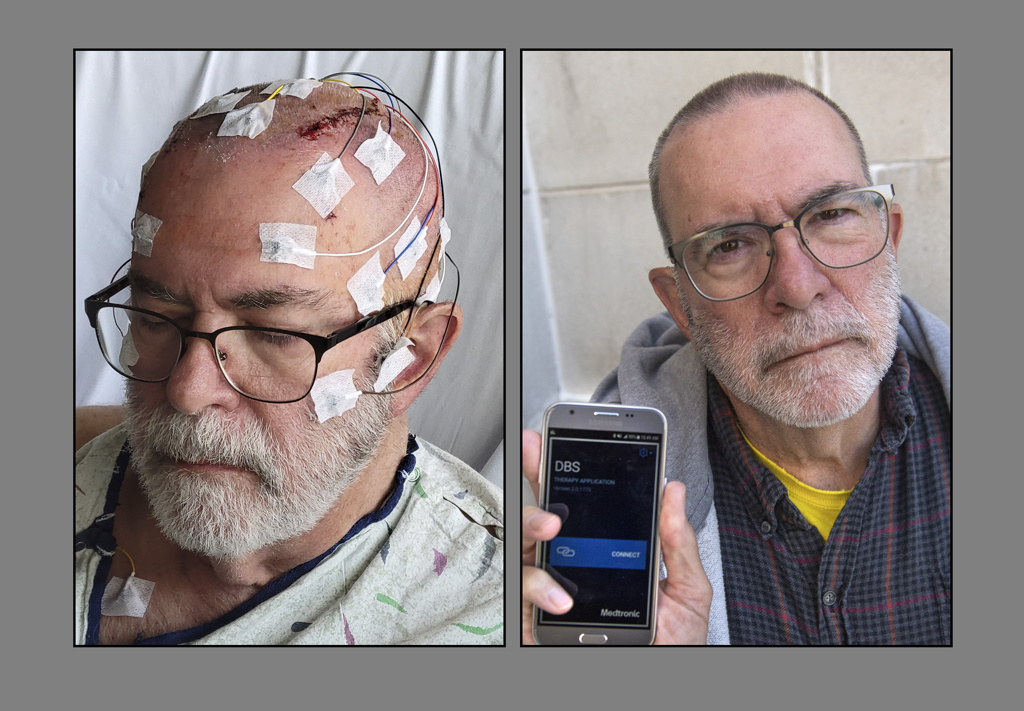
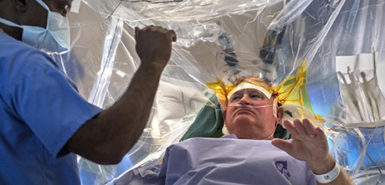
“We do the implantation while the patient is awake,” Dr. Ali said. “We drill two small holes in the top of the head and record brain activity, target areas as small as 5 to 7 millimeters, then insert the lead wire and test response.”
Coleman remembers the surgery quite well.
“Dr. Sriram was on one side, Dr. Ali on my other side,” he said. “It didn’t hurt—the injection before surgery was the most painful. I had to do various movements during the surgery, like make a fist, or say, ‘Today is a sunny day.’”
He said he felt some anxiety, but also excitement at the prospects ahead.
Coleman’s wife and daughter waited in the recovery room, just as excited.
“I was surprised how quickly I saw changes after Lou’s surgery,” Helen said. “Better balance, no more shuffling. Lou could even move his arms freely as he walked. And he had more energy. It’s hard to keep him down now.”
Two days after surgery, Coleman insisted on having friends over to celebrate the Fourth of July holiday.
He enjoyed conversation and playing his favorite game of cribbage with family friends, all of them delighted at seeing their old friend doing so well.
“The future is bright,” Coleman said. “If someone is considering surgery and is a candidate, they would be remiss not to do it. This isn’t kind of like a miracle. This is a miracle.”

















 /a>
/a>
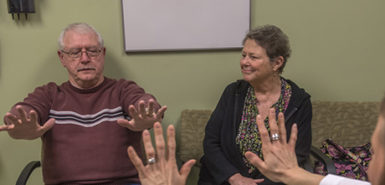 /a>
/a>
 /a>
/a>
Excellent story of hope!