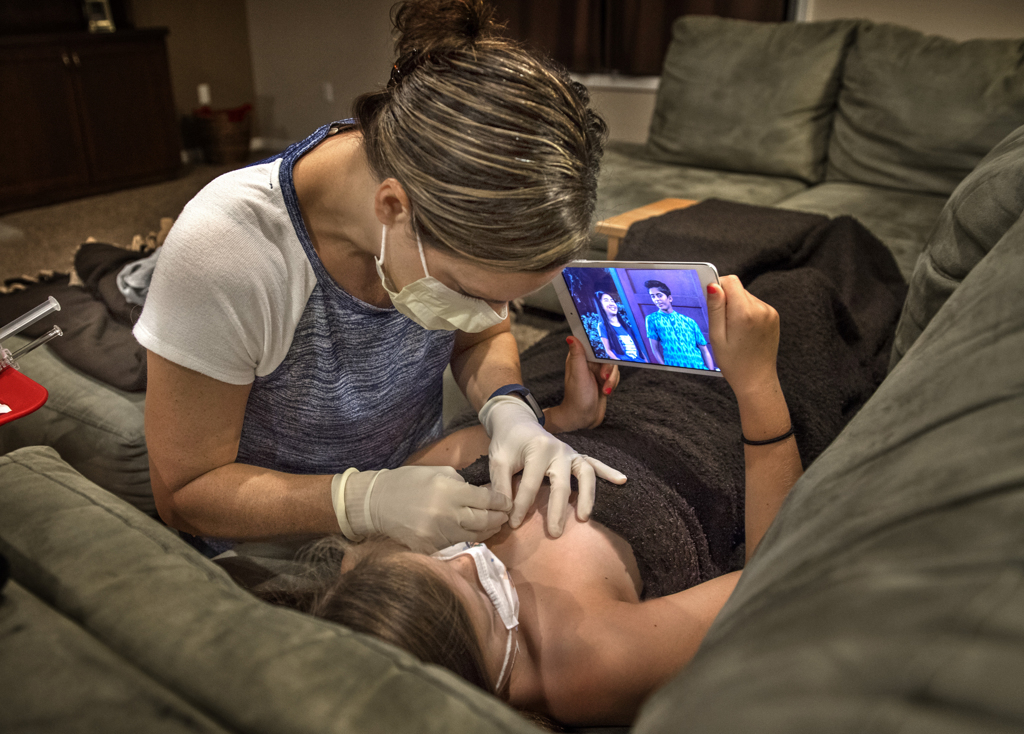
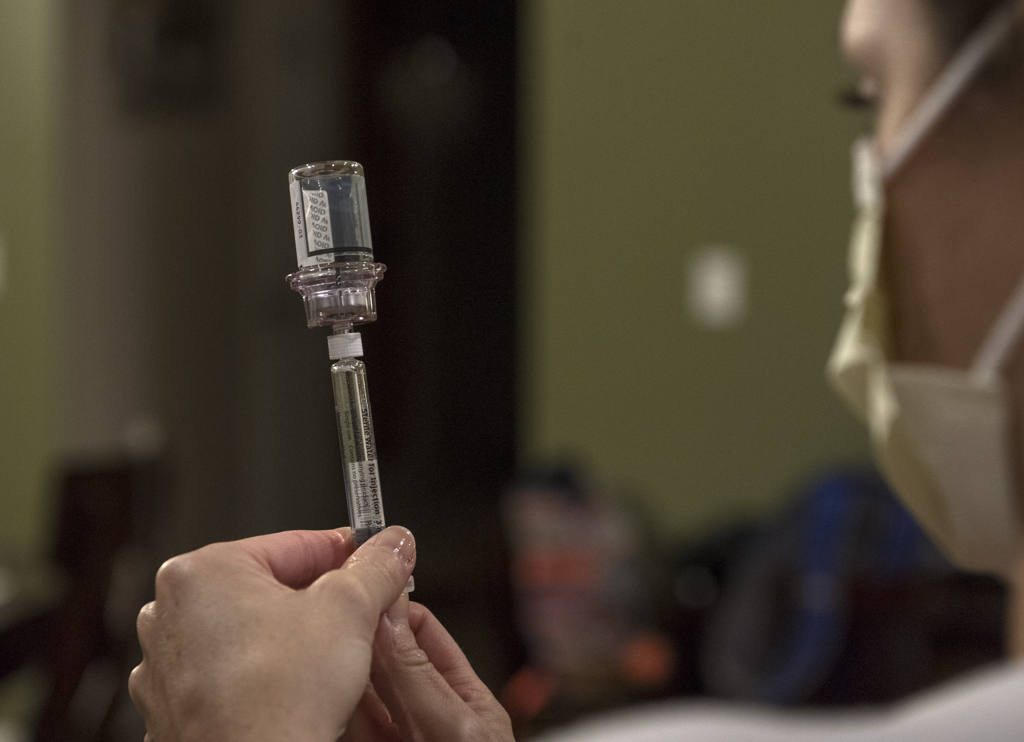
Emma Warner lay on the couch, sleepily watching a TV show on a tablet as her mom mixed water into a small vial of powder.
A tray appeared beside the couch, spread with syringes and a pair of gloves. Nine-year-old Emma didn’t even look up.
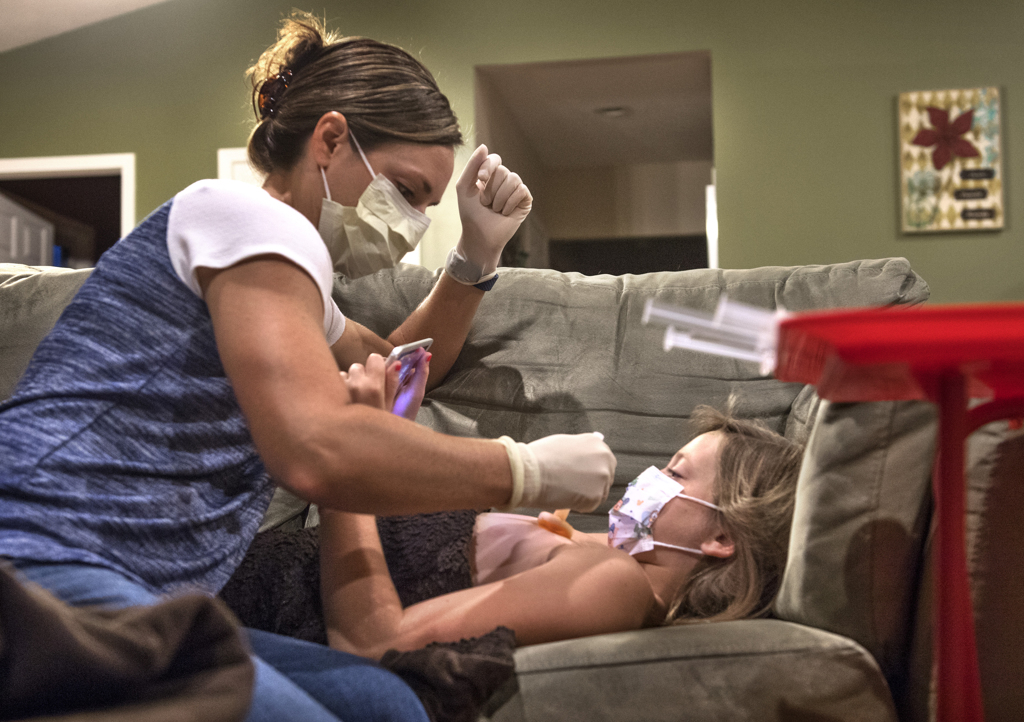
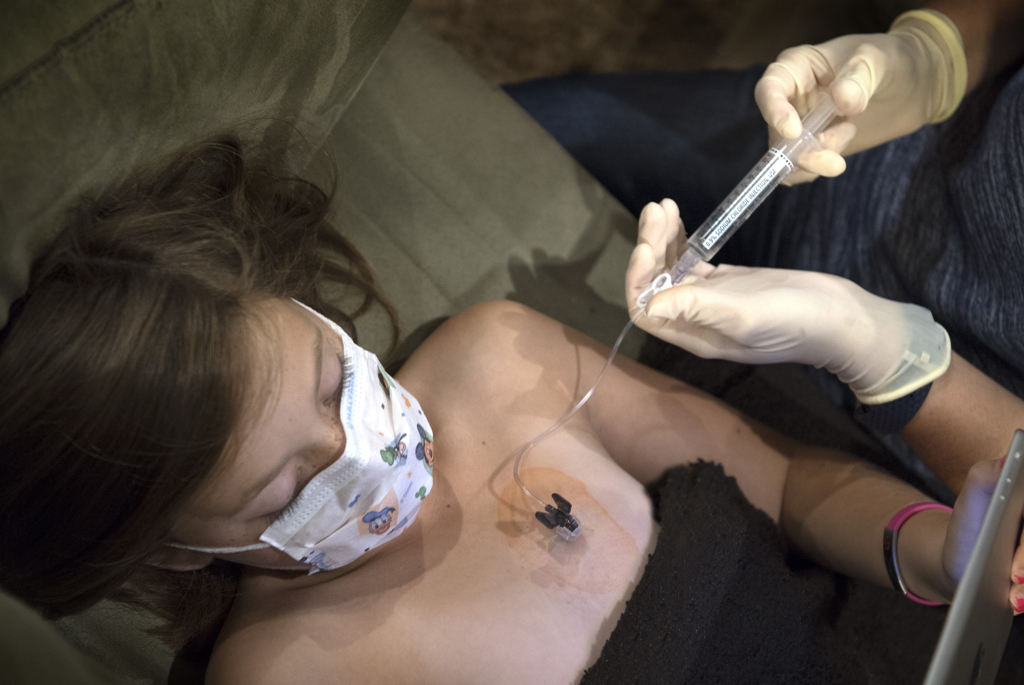
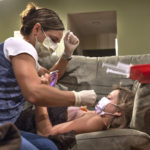
Her mom, Becky Warner, applied an orange antiseptic solution to the spot on Emma’s chest where a port lay beneath the skin. Into the port, she poked a needle connected to an intravenous line.
With a syringe, she injected saline into the line. Then came the medicine for hemophilia.
“This is the good stuff,” Becky said, as she slowly pressed the plunger on the syringe.
That good stuff—clotting factor—prevents uncontrolled bleeding that could damage Emma’s joints and cause other injuries.
Another shot of saline, followed by heparin to prevent clots, and the treatment was done.
Emma set down the tablet, yawned, and headed to the kitchen to eat breakfast with her 7-year-old brother, Gage.
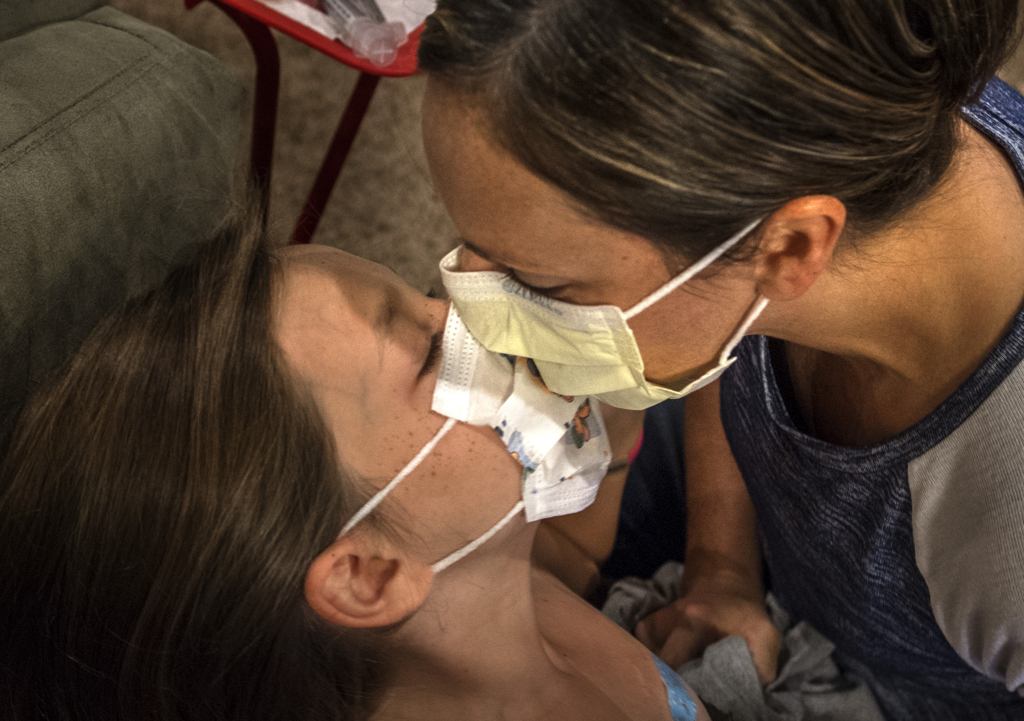
She has a quick smile and charm. She is so easy to treasure.
The school-day routine, performed with a calm, antiseptic precision born of years of practice, gave no hint of the extraordinary nature of these treatments, of Emma herself.
To be born with severe hemophilia A puts her in a select group. And to be a girl with hemophilia is rarer still, said Deanna Mitchell, MD, a pediatric hematologist-oncologist at Spectrum Health Helen DeVos Children’s Hospital who sees children with hemophilia at the coagulation disorders clinic.
“We follow about 100 boys and young men with hemophilia, and she is my only female (patient),” she said.
Emma, a sandy-haired girl with a spray of freckles across her face, has made an impression, and not just because she’s the only girl in a group of boys. Her calm, easygoing nature wins over her medical team.
“She has a quick smile and charm,” Dr. Mitchell said. “She is so easy to treasure.”
The chronic condition requires vigilance and monitoring by specialists, parents and the children themselves. But research has led to improved treatments, and there is hope on the horizon, as researchers test a gene therapy for hemophilia.
Shock and fear
For Emma’s parents, Becky and Luke Warner, the diagnosis of hemophilia came without warning. They have no family history of the disorder.
Their first hint of a problem arose when Emma, at 13 months old, started to crawl. Large, dark bruises covered both knees, extending down into her lower leg.
“We knew something was not right,” Becky said.
Their family doctor ran blood work and Becky learned the diagnosis in a phone call: hemophilia A, or classic hemophilia.
Their reactions?
“Shock,” Luke said.
“Fear,” said Becky. “We didn’t know a lot about hemophilia.”
Meeting with Dr. Mitchell, they learned the disease puts a child at risk of prolonged bleeding after a cut or injury. A blow to the head could cause bleeding.
And often, children with hemophilia experience spontaneous bleeding in their joints, even when there is no noticeable injury. If not treated, it could cause irreversible damage to the joints over time.
“At 1, Emma couldn’t tell us what was happening,” Becky said. “So that part was scary.”
In years past, children with hemophilia often suffered such damage to their joints that, by adulthood, they needed a wheelchair or a pair of crutches for mobility. But improvements in treatments have made it possible to minimize the impact on the joints.
“Emma was born at a time when she has safe factor available that is completely synthetically made,” Dr. Mitchell said.
For Emma, a fourth-grader at Northeastern Elementary School in Hastings, Michigan, hemophilia means avoiding contact sports and activities that might lead to injury.
“I cannot go on trampolines,” she said. “I cannot go on snowmobiles.”
“She can’t do gymnastics or cheerleading,” Becky said. “At a young age certain sports are fine, like soccer. But if they become competitive when she gets older, that’s when the danger kicks in.”
Even with those activities off the table, Emma does plenty.
She golfs, swims and shoots hoops on the driveway with her brother and parents. She plays piano and recently started guitar lessons.
At school, she likes music class best.
“This year in fourth grade, we get to play recorders,” she said.
The genetic mystery
Through genetic testing, the Warners learned how Emma became one of the few girls with the disease.
About 1 in 5,000 newborn boys have hemophilia A, which is caused by a defect in a gene that codes for a protein needed for blood clotting, called factor 8.
The gene is carried on the X chromosome. Because girls have two X chromosomes, a girl with the genetic mutation on one chromosome usually does not have the disease. A functioning backup gene on the other X chromosome allows her to create factor 8.
A girl with the genetic defect is a carrier, and may pass the disease on to her sons. That’s how most cases occur.
But with Emma—and 30 percent of people with hemophilia—a spontaneous mutation caused the disease.
And in her case, the backup gene on her other X chromosome is inactive. Although rare, this issue occurs occasionally in X-linked genetic conditions, Dr. Mitchell said.
Kids with mild or moderate hemophilia A have low levels of factor 8. But Emma’s blood test showed no detectable amount of the protein, which means she has a severe form of the disease.
Getting used to pokes
For the first few years, Emma received infusions of clotting factor only when needed. Her parents watched for signs of bleeding in her joints.
Her mom recalled an incident when Emma was a toddler. She slept on a mattress on the floor, with a railing, to minimize risk of falls.
One morning, she woke up excited about going to day care. She jumped up eagerly, and then suddenly dropped back to the floor.
Worried she had a bleed in her ankle, the Warners took her to Helen DeVos Children’s Hospital. Emma got an infusion.
Once, when she was 3, Emma got a bump on her cheek. It swelled to the size of a tennis ball.
How did she handle the pokes as a small child? A shy smile spread across Emma’s face.
“The first couple of times, I was scared. Once I tried to bite someone,” she said. “But I got used to it.”
The bleeds happened more frequently as Emma grew and became more mobile. At 5, when she started kindergarten, she began to get infusions regularly, as a preventive treatment.
“I feel better sending her to school knowing she has protection,” Becky said.
She and Luke give the infusions to Emma every Monday, Wednesday and Friday mornings.
“Parents are just heroes in the world of hemophilia,” Dr. Mitchell said. “They have made it so children don’t have joint disability. They can grow up to be strong and healthy.”
The Helen DeVos Children’s Hospital clinic treats kids who have a variety of bleeding disorders. In addition to hemophilia A, they see children with hemophilia B, which affects 1 in 30,000 boys, and von Willebrand disease, which occurs in both genders and affects 1 percent of the population.
To help combat complications of the disease, the team hosts comprehensive coagulation clinics every month that allow children to see a number of providers in one visit.
The kids come in once a year and meet with a hematologist and review their medication doses and adjust if needed. They also see nurses, research coordinators, a psychologist, a physical therapist who measures joint mobility, and a dental hygienist who addresses ways to prevent bleeding gums.
Eventually, kids like Emma learn to give intravenous infusions to themselves.
Treatment options may change dramatically in Emma’s future, Dr. Mitchell added. Researchers are developing new medications and holding clinical trials to test a gene therapy treatment.
Because hemophilia often affects multiple family members, the clinical team forms ties with multiple generations of extended families.
“That’s very gratifying to follow families for many years and to see the progress being made,” Dr. Mitchell said.
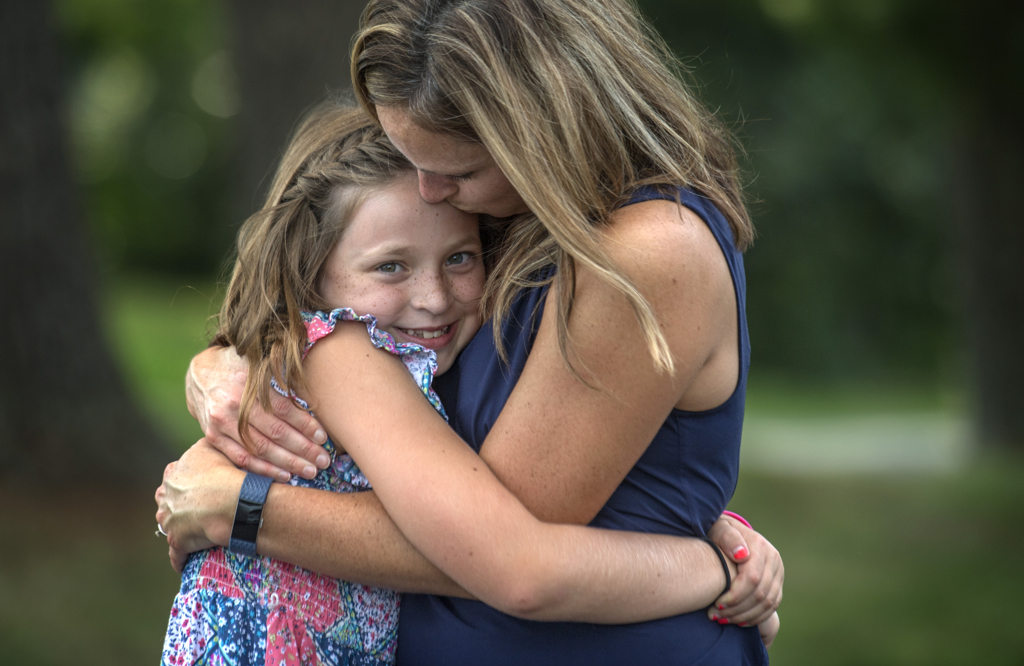


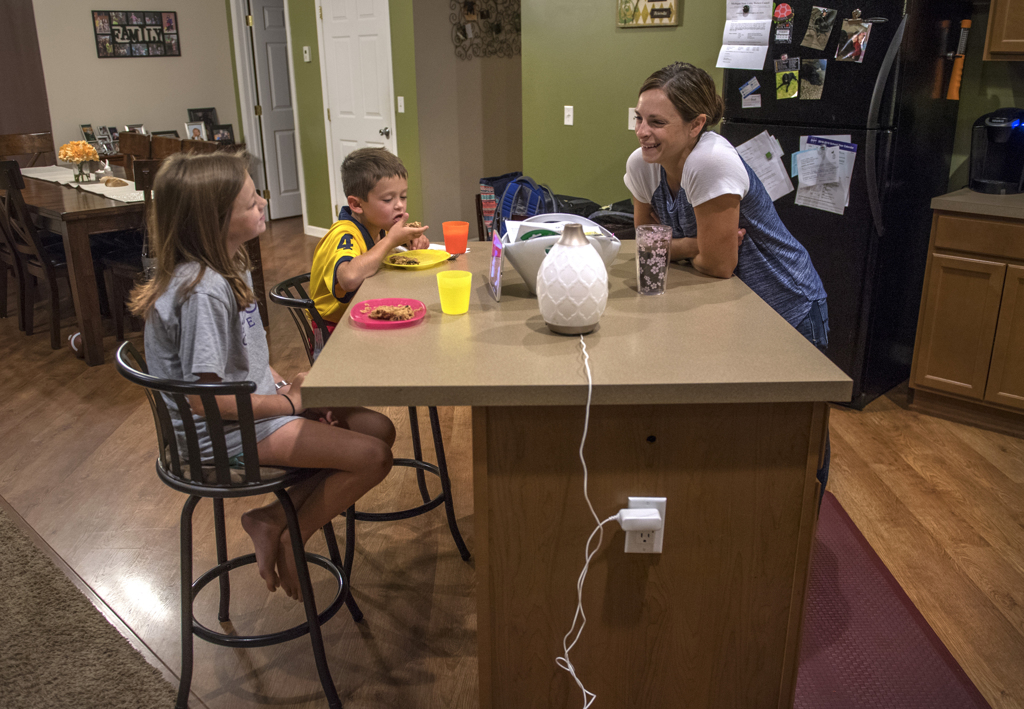














 /a>
/a>
 /a>
/a>
 /a>
/a>
My dear friend Jan Warner is the grandmother of little Emma. She has been telling me about her for years, and she is every bit as amazing as Jan says she is. Also every bit as cute! Her parents,Luke, who is Jan’s son, and Becky are obviously amazing people too. Dealing with so much for all these years, and doing it so well can’t be easy. I admire them all, including Tom, Jan’s husband and Emma’s grandfather, who I did not mean to leave out. We live in PA, while the Warners live in MI, but I hope to some day meet Emma, Luke and Becky, and give them all the hugs they deserve.
Thank you, Gail! Appreciate your kind comments and for sending virtual hugs. Hope you have a wonderful day! Cheers, Cheryl
I have known Emma’s family for a long time and have been in awe of how they have handled this with Emma, family, friends, and her school. They are amazing and have made life as normal as they possibly can for Emma. I know they think the world of Emma’s doctors and all they have done through the years to help her through some scary times. I hope more people become aware of this disease. Becky, Luke, and their families have been incredible through this journey!
Thank you, Ann, for your lovely comment. Emma and her family are amazing. 🙂 Cheers, Cheryl