Nancy Perry had no idea how close she came to death when her heart valve failed.
Pain shot through her chest. She could barely breathe. She thought she was having a heart attack. Instead, an aortic valve implanted 14 years earlier had suddenly torn.
She needed a new one―and quickly.
“That’s the main valve that exits the heart,” said William Merhi, DO, an interventional cardiologist with Spectrum Health Fred and Lena Meijer Heart Center. “It’s the gateway to the rest of the body from the heart.”
Perry, a 79-year-old Grand Haven, Michigan, woman, arrived by ambulance at Spectrum Health Butterworth Hospital on Aug. 22.
“She was clearly in dire straits,” Dr. Merhi said. “Had she not had some sort of definitive therapy, she would have died.”
Fortunately for Perry, great strides have been made in aortic valve replacement technology since she received her first prosthetic valve in 2002. At that time, her only option was open-heart surgery.
I feel very fortunate that God saved my life.
In recent years, however, researchers have developed a way to implant a valve with a minimally invasive procedure―and that made all the difference for her.
Physicians at Spectrum Health’s Transcatheter Aortic Valve Replacement Clinic have been involved in research that helped develop the TAVR procedure.
The groundbreaking treatment offers hope to patients who are not considered suitable candidates for open-heart surgery or who would face prolonged recovery in an intensive care unit.
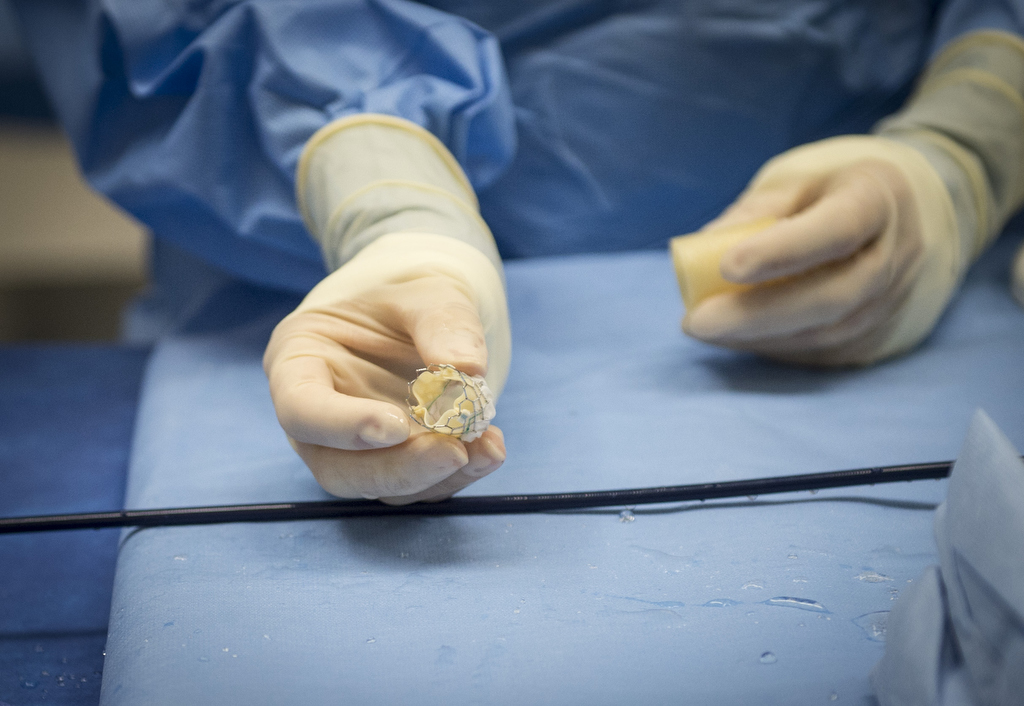
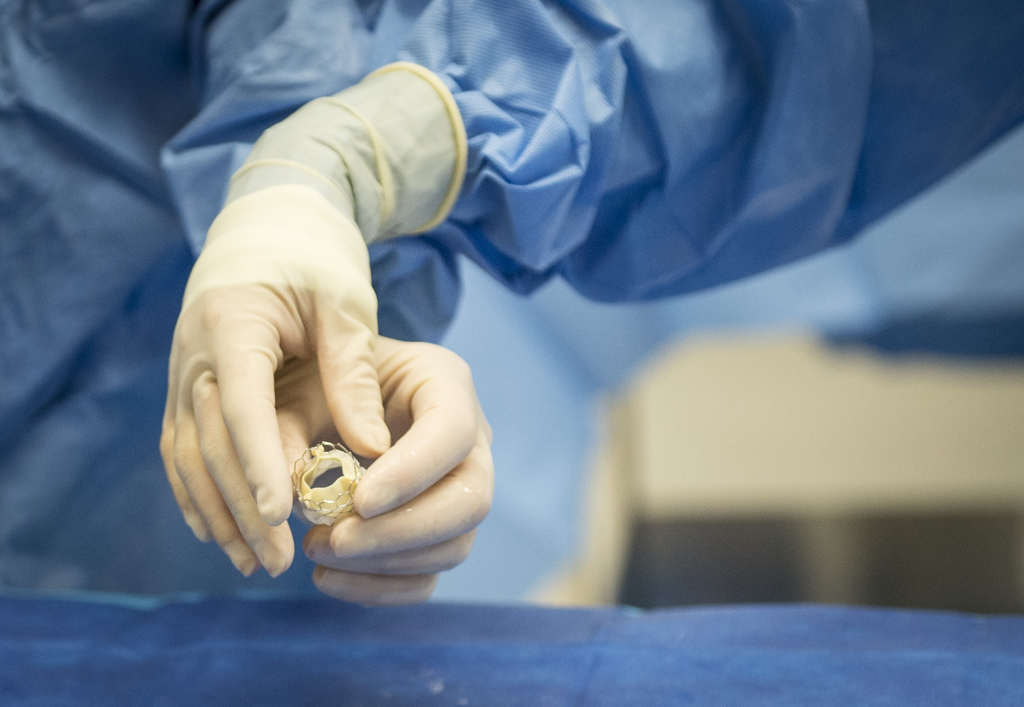
The doctors thread a catheter into an artery in the groin. They feed the replacement valve―collapsed to a small shape―through the catheter to the heart and position it across the aortic valve. This is where the new valve controls the flow of blood from the heart to the body’s main artery. There is no need to remove the old, damaged valve.
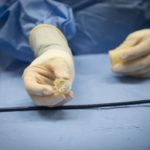
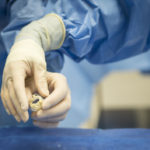
“It’s amazing. It truly is,” Perry said. After her procedure, a nurse showed her a copy of the implanted valve.
“I’m thinking it had to be squished into such a teeny tiny thing and travel up my femoral artery to get into my heart and open up. It just blows your mind.”
‘Call 911’
Perry, a retired legal assistant, leads a busy, full life. She loves to garden. Much of her vegetable garden produce goes into food she cooks for her church. She and her husband, Marvin, married seven years, keep busy with a blended family that includes many grandchildren and great grandchildren.
Problems with her heart first surfaced when she turned 65. She found herself becoming tired or breathless during her usual routines―when she climbed three flights of steps at the office or took her dogs for a long walk.
An echocardiogram revealed her aortic valve had narrowed. She underwent open-heart surgery at Butterworth Hospital to get a replacement valve. The operation, which involved dividing the breastbone, required four to six weeks of recovery time.
She experienced no problems with the valve for the next 14 years―until Aug. 22.
While talking on the phone with a friend from church, she suddenly started sweating profusely. A sharp pain ran through her chest, shoulder and back.
“I walked out of the bedroom and told my husband, ‘I don’t know what’s wrong, but call 911,’” she said.
An artificial valve can become plugged over time and need replacement. But typically, the symptoms are gradual and elective surgery is scheduled to replace them, her doctors said.
She’s enjoying life. It’s really gratifying when you see that.
However, when a valve tears, as it did for Perry, a patient’s condition deteriorates rapidly. Without a functioning aortic valve, blood can leak back into the heart. Thus, the heart can’t pump blood to the rest of the body. It starts to fail, which can lead to respiratory failure, organ failure and ultimately, death.
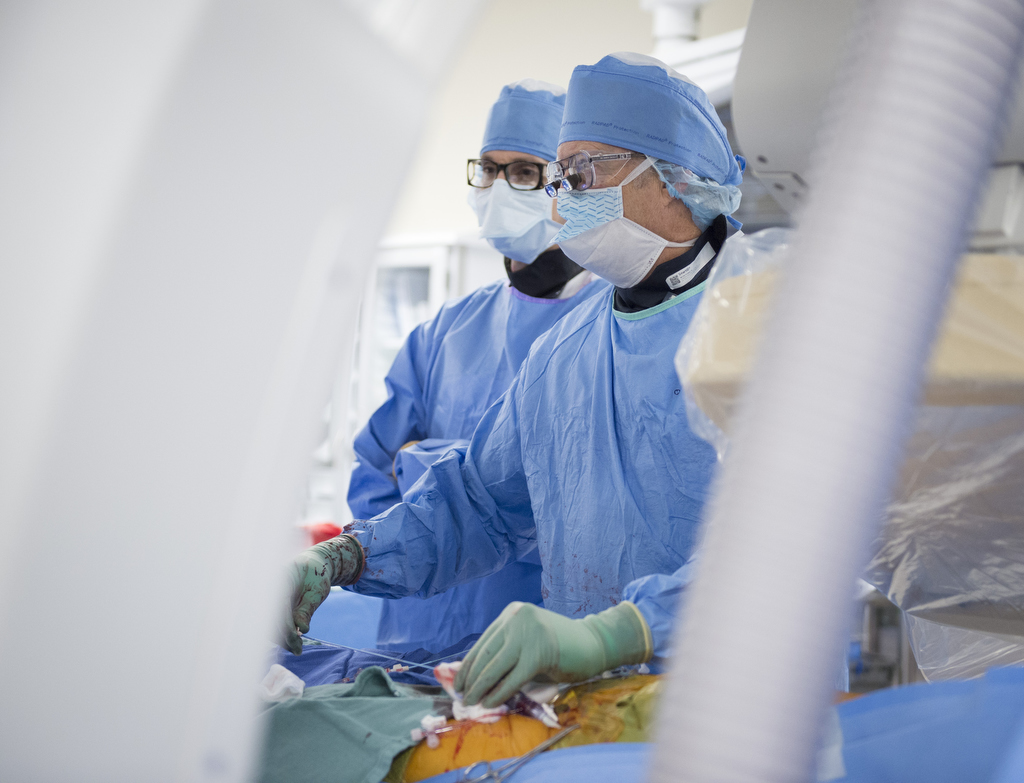
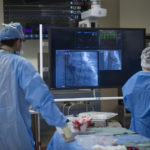
When Perry arrived at the Butterworth emergency department, the cardiothoracic surgical team consulted with the TAVR team, which includes cardiac surgeons as well as interventional radiologists.
The TAVR team “affords the patient the best view from all disciplines,” Dr. Merhi said. “It’s a meeting of the minds.”
The doctors determined open-heart surgery would be risky because she was in shock. And, even in the best of circumstances, recovery from a second open-heart surgery would be more challenging.
Instead, the team opted for the TAVR procedure.
Perry marveled at her quick recovery―a much easier course than with her open-heart surgery. She was up and walking the halls the next day. Three days after the procedure, she returned home and even spent 15 minutes weeding the garden.
“No comparison. This is definitely much easier on the body,” she said.
From research to practice
“This wasn’t available six years ago,” Dr. Merhi said of the TAVR procedure.
The TAVR team at Spectrum Health began using the minimally invasive method to implant aortic valves when the doctors began taking part in clinical trials in 2011.
The U.S. Food and Drug Administration approved TAVR procedures for extreme-risk patients in 2012 and for high-risk patients in 2013.
A trial for middle-risk patients recently closed. Spectrum Health is one of a select few sites in the U.S. enrolling low-risk patients for a clinical trial.
Open-heart surgery remains the gold standard for aortic valve implants, said John Heiser, MD, a cardiothoracic surgeon at the heart center and a member of the TAVR team. But the TAVR approach is becoming more common as more long-term results become available, he said.
At Spectrum Health, physicians have performed more than 600 TAVR valve replacements in the past five years.
“We’ve gained a level of expertise that you just gain with experience,” Dr. Merhi said.
At a checkup a month after Perry got her new valve, her doctors cleared her to return to a full slate of activities.
“I’m able to do everything I need to do―to cook for my husband, to clean house and work outside in the yard,” she said. “I feel very fortunate that God saved my life. I just feel very thankful to be alive.”
“We just told her to live life to the fullest,” Dr. Merhi said. “She’s enjoying life. It’s really gratifying when you see that.”
















 /a>
/a>
 /a>
/a>
 /a>
/a>
I had in or you St. Jude’s mechanical valve installed in 1996 and have been very happy with mine it is encouraging to see that the need for replacement is out there in appears much more simple thank you Dr. Heiser!
Thanks for sharing, Gary! Glad you’re doing so well. 🙂
THANK YOU FOR SHARING, IT IS A GOOD SIGN FOR THOSE US OVER 70. HOPE YOU CONTINUE TO DO WELL.
I I am sure Nancy Perry appreciate your good wishes. Thank you for reading this story and sharing your comment. Wishing you the best of health!