Nothing about Jacquelyn Ritsema’s pre-pregnancy life might have suggested back problems.
The 24-year-old registered nurse worked out regularly and did yoga. In her work at Spectrum Health Blodgett Hospital, she often helped lift patients.
But after she and her husband welcomed their baby, Kinsley, last July via an emergency Cesarean section, that all changed.
“It was the first time I’d ever had surgery,” she said. “So I expected some pain and recovery time.”
But the pain soon became sharp and stabbing. She would feel it whenever she leaned forward or backward—it would take her breath away.
“Even leaning over the baby to change her diaper was painful,” she said.
Initially, her doctor instructed her to try ice, heat and ibuprofen.
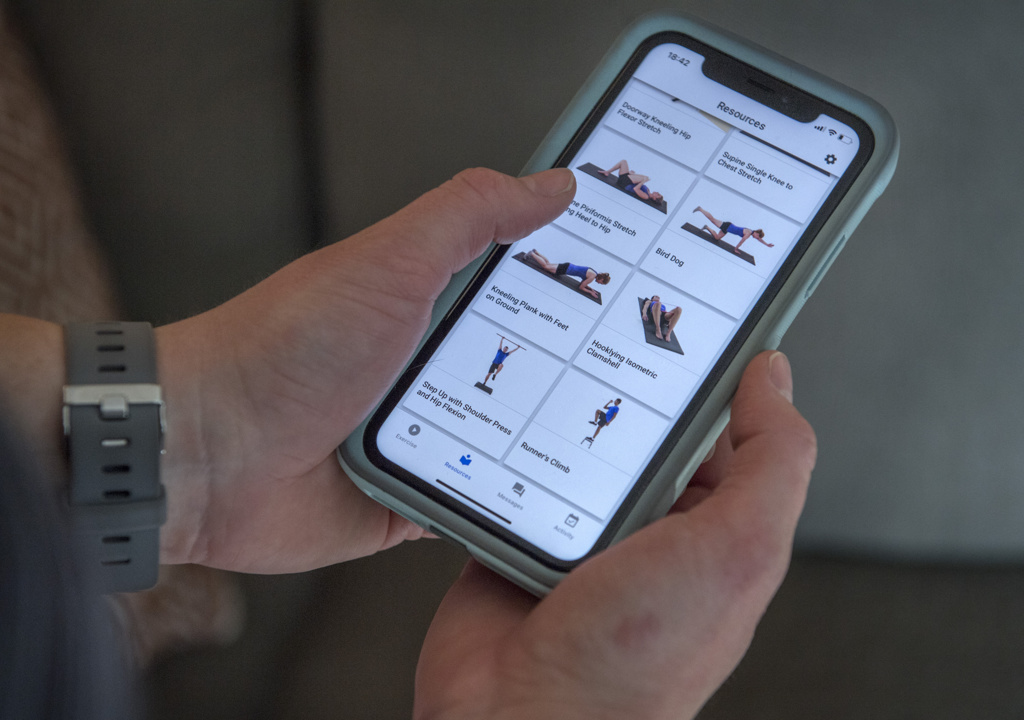
But the pain persisted. By Ritsema’s six-week postpartum checkup, her doctor suggested she see a physical therapist specializing in post-childbirth recovery.
The doctor also told Ritsema the treatment is standard in some countries—and it’s becoming more common in the U.S. as providers aim to improve maternal health care.
“My obstetrician assured me that (physical therapy) could make a big difference,” Ritsema said. “And I was intrigued. And it hurt so much, I figured it couldn’t get worse.”
The unspoken pain
Not everyone is aware that back ailments can be a side effect of pregnancy. Roughly 50% of women suffer back pain during pregnancy, with anywhere between 5% and 40% of those still in pain six months later.
The incidence is even higher in C-section deliveries using epidural anesthesia, like Ritsema’s.
Ritsema met with Elizabeth Harris, PT, a Spectrum Health physical therapist who specializes in pelvic floor rehabilitation.
Harris quickly helped Ritsema understand her back trouble.
“Between the C-section and my abs not working as I recovered from surgery, my vertebrae stopped lining up the way they should,” Ritsema said.
A woman’s body can change dramatically as the baby develops, Harris said.
“We looked at the whole dynamics of her spine and her abdominals, restoring postural integrity so she could go back to work,” Harris said. “An essential part of the job is moving patients.”
By September, Ritsema had begun weekly sessions with Harris.
Over eight meetings, she learned to retrain her core muscles through a new series of stretches and strengthening exercises.
“In the beginning, I could not lay flat on my back, contract my abs and then pick my legs up off the ground one at a time,” said Ritsema, who lives in Marne, Michigan. “Now I can do that, no problem.”
“We started by focusing on the dynamics of her spine,” Harris said. “Nurses move patients and it’s so important that they lift properly. She needed to learn new ways to move.”
Ritsema is now working a normal workload—about 36 hours a week in three 12-hour shifts.
Almost all of it is on her feet.
“My back pain is completely gone, which is fantastic,” she said.
She’s sticking with the 30-minute exercise routine that Harris prescribed.
“I do the full routine on days when I’m not working,” Ritsema said. “And on the days when I work, I at least find time to do the stretches.”
Spreading the news
Both Harris and Ritsema wish providers would let more women know about the benefit of physical therapy. It would spare many women from suffering in silence, thinking back pain is somehow normal.
“Several of my friends had babies around the same time, all struggling with some level of back pain,” Ritsema said. “And none of them knew how much they could benefit from this.”
Harris agrees.
“It’s all too common for new moms to think, ‘It’s just pregnancy—I should be able to bounce back from this, no problem.'” Harris said. “And, of course, some do. But often they don’t—particularly in the case of C-sections or more complicated deliveries.”
Physical therapy should be considered early in the process.
Harris encourages new moms to talk about back pain when they go in for their six-week checkup.
“We are seeing more referrals,” she said. “So when it comes to building better backs, stronger cores and improved pelvic floor health for new moms, we are moving in the right direction.”




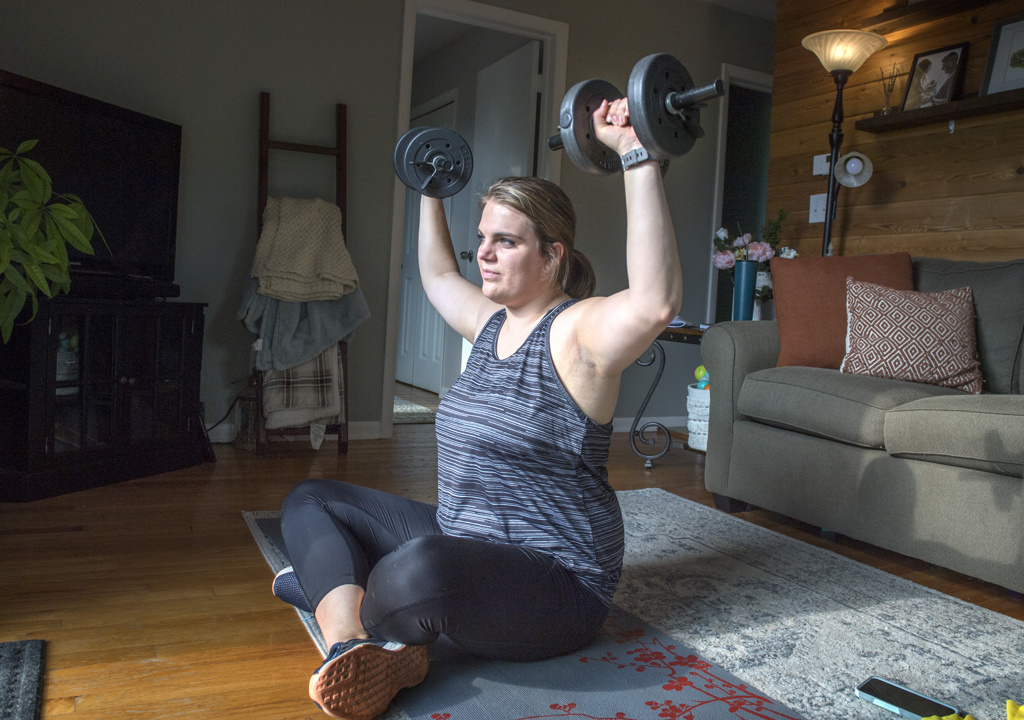










 /a>
/a>
 /a>
/a>
 /a>
/a>